- Submissions

Full Text
Trends in Telemedicine & E-health
Value of Telemedicine for Care of Patients with Diabetes Delivered by Retired Endocrinologists
Richard J Santen MD*
Emeritus Professor of Medicine, University of Virginia Health System, USA
*Corresponding author:Richard J Santen MD, Emeritus Professor of Medicine, University of Virginia Health System, 450 Ray Hunt Drive, Charlottesville Virginia, USA
Submission: January 26, 2026;Published: February 04, 2026

ISSN: 2689-2707 Volume 6 Issue 3
Introduction
The provision of health care in rural, underserved areas in the United States primarily involves nurse practitioners, physician assistants, and primary care physicians but not specialists [1-4]. When patients in rural areas have complicated medical problems requiring a specialist, arrangements are usually made for referrals, often to hospitals or clinics far distant and with long waiting times. For reasons such as lack of transportation, financial limitations, distance, timeliness and other reasons, evaluation by specialists often does not take place. Accordingly, the level of care can be compromised [5].
Specialists tend to live in urban and not rural areas and work in hospital systems or large private clinics [2]. Waiting times for new patients to see Endocrinologists or Diabetologists is usually prolonged and often quite expensive, particularly for patients with limited or nonexistent insurance coverage. As these issues affect a large number of patients with diabetes mellitus or other endocrine disorders, resolution of the problem of access to specialists is a very important issue and requires innovative thinking. One practical solution is to develop procedures that allow the patient to be evaluated and managed by a specialist at a distance using telemedicine [6]. This opinion piece suggests that telemedicine and the efforts of retired endocrinologists can serve to ameliorate this problem and the overall methods described have substantial value.
The Federal government in the United States has established a program called the Federally Qualified Health Centers (FQHCs) which provide care for patients in rural, underserved areas [7]. Currently, approximately 1400 of these clinics exist. They are partially supported by the Federal government which provided roughly 4.5 billion dollars in support in 2025 with 8.1 billion in the 2026 proposed budget. The clinics possess a comprehensive range of facilities which generally include: areas to draw and send out blood samples for laboratory testing; retinal cameras for evaluation of diabetic retinopathy; ultrasound for bone density assessment; and telemedicine capabilities. In addition to providers, personnel available include nutritionists, nurse educators, case managers, social workers, and administrators for scheduling and electronic medical record maintenance.
A solution to the problem of lack of endocrinologists or diabetologists is to utilize telemedicine for new patient evaluations and follow-up care of patients with diabetes who require specialty care [6,8]. In general, patients with diabetes mellitus with Haemoglobin A1c levels above 10% generally require specialty care. In addition, patients with a range of other endocrine disorders also can benefit from this level of expertise. My experience over an 8-year period provides evidence of the feasibility of this approach. In this opinion piece, I will describe my experience with such a program and discuss the various aspects which relate to the organization and implementing of a six-month, intensive consultation and management program for poorly controlled patients with diabetes. Also discussed is the feasibility of consultations for general endocrine clinical problems.
Initial steps
In order to set up a telemedicine program, several steps were required in my experience [6,8]. I first contacted several FQHC administrators to ascertain their willingness to collaborate on a program designed for intensive diabetes management over a sixmonth period. The rationale was to utilize specialty level expertise to educate patients and initiate new therapies with a goal of achieving reasonable diabetes control. An active medical license in the state of the FQCHC was required. I had an existing license but most states have programs targeted toward retired practitioners that allow them to re-instate lapsed licenses under non-stringent conditions. I obtained malpractice insurance with the stipulation that my practice would be part time with a limited number of hours. Later I learned that the FQHC system had instituted a legal tort agreement with the government that covered malpractice. Accordingly, retired physicians would not need to obtain their own malpractice insurance. As expenses for me included malpractice insurance, internet access, telephone access, a computer, printer, Dragon One MedicalR dictation software and various supplies, I negotiated a $500 a month stipend from the FQHC to cover these expenses.
Several components were key to the success of this program. A dedicated nurse educator formally certified in diabetes education is critical. Recently the training for this position has undergone substantial enhancement and this position is now called Certified Diabetes Care and Education Specialist (CDCES). Such individuals communicate with the patients to address their education and communication needs and serve as liaisons with the providers at the clinic. A nutritionist is essential but not all clinics have one available. The CDCES serves this role if a nutritionist is not available. Clinic notes, laboratory data and all medical reports are shared by HIPPA compliant e-mails. I do not utilize the electronic medical record of the clinic myself but all of my notes are sent by HIPPA secure e-mail and entered into the EMR of the clinic by staff. When I need data from the patient’s chart, scanned documents are sent to me by e-mail.
Implementation
The providers at the FQHC identify patients under poor control (i.e. generally with a HbA1C>10%) and arrange new patient appointments via telemedicine [6]. All prior data are then sent to me by scanned PDFs via HIPPA secure e-mail. When the patient arrives in clinic for the telemedicine visit, the CDCES takes vital signs and explains to the patient the procedures. The CDCES and I then take a detailed history from a standard diabetes history form. The CDCES obtains demographic data, a nutrition and exercise history, a smoking, alcohol and recreational drug history, and information about exercise. I then obtain information about medications, take a standard medical history, and am told the vital signs. I have found that the physical exams taken by the providers previously are generally very comprehensive and accurate and I review these data. Occasionally the CDCES is asked to observe patients for tremor, pallor, visible goiter or other findings. I then review the laboratory data which has been sent to me. At this point, I recommend the additional laboratory testing needed and any changes in medications. I ask the patient whether or not they are willing to call me weekly with a report of their glucose levels or continuous glucose monitoring results.
The next step is to use Dragon One MedicalR software to dictate a full history and re-iterate the physical exam from the chart. I dictate an assessment and recommendations and then review the dictation for errors. This entire evaluation process takes approximately one hour and allows sufficient time for questions and an in-depth discussion of the patient’s lifestyle. This document is then converted to a PDF and e-mailed to the CDCES who then shares with the provider and inserts in to the EMR. The CDCES communicates with the patient’s provider and arranges the blood tests and prescriptions needed. This frees me up from the process of ordering laboratory tests and prescribing medicine and having to obtain pre-authorizations as the clinic staff take care of these steps.
Each week the patient calls me at a specified time and date and reads the blood sugar log or allows me to review the CGM, DEXCOM or Libre. Generally, phone calls do not exceed five minutes. I usually make a change in the regimen weekly so as to allow improvement in glucose parameters quickly. As needed, log sheets are scanned and faxed to the provider for their information and to scan into EMRs. The patient is discharged when the goal of therapy is achieved or if the patient misses three weekly appointments. They are told up front, “three strikes and you are out.” I explain to them that this method lets me know if patients are not motivated for this management program and therefore will not benefit from my time and effort. When discharged, the patient is told that I will be available at any time later if they need advice or assistance.
Table 1:Area and number of patients with other endocrine problems identified.
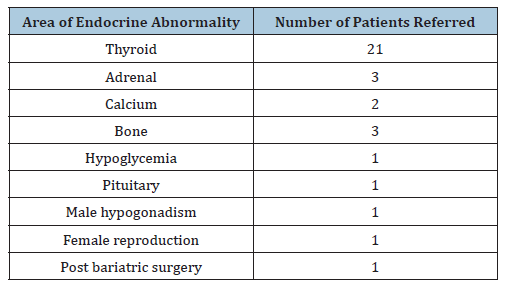
As I have expertise in most areas of endocrinology, patients with thyroid, adrenal, bone, reproductive or calcium problems are referred to me as well (Table 1). For these patients, I also take an extensive history and rely on the physical exam obtained by the clinic provider. For patients with thyroid disorders, I order thyroid ultrasounds at a local facility. For patients with osteopenia or osteoporosis, a DEXA bone density analysis is obtained, usually at a regional hospital. For patients with incidfental adrenal nodules, the patients go to a regional hospital for a CT scan.
Experience
I have been providing this telemedicine specialty management for the past 8 years and have now evaluated 264 new patients with diabetes mellitus and 34 new patients with other endocrine problems (Table 1. of the patients with diabetes mellitus, 96% had type 2 diabetes and 4% type one. I refer the type one patients to a distant University Hospital comprehensive diabetes program. Approximately 80% of the patients with diabetes follow the full six-month program and 20% appear to be insufficiently motivated and drop out, or miss more than three telephone call appointments without a reasonable excuse. Several years ago, I conducted a full evaluation of the results in a serial cohort of patients and am planning to update again in the future [6]. Forty % of patients were men and 60 % women; 81% Caucasian, 12% African American and 7% Hispanic. The average age was 55.9±12.2 (SD) years; weight 220±61.8 (SD); and 84% required insulin [6].
Baseline HbA1c at the start of therapy was 10.3±1.94% and at the time of discharge 7.78±1.51%. At that time, 14% of patients had a HBA1C of <6.5%; 18% 6.6 -7.0%; 27% 7.1-7.5%; 9% 7.6-8.0% and 32%>8.1%. Body weight did not change with an initial weight of 226±60 pounds and at the time of discharge, 225±58 pounds. Various regimens were used including: (1) basal/bolus with correction factor 62%, (2) GLP-1 agonist 48%; (3) basal insulin without bolus 32%, (4) sulfonurea 30%, (5) DPPS inhibitor 1%, (6) U 500 insulin 10% and (7) SGTL2 inhibitor 10%. The largest number of patients used 2 different modalities followed by those using respectively: 3, 1, 4 and 5 modalities.
Figure 1:Left panel, individual HbA1C levels over the period of telemedicine management and after the follow up of the program. Right panel mean HbA1c levels and SEM variations. Figure modified from [6].
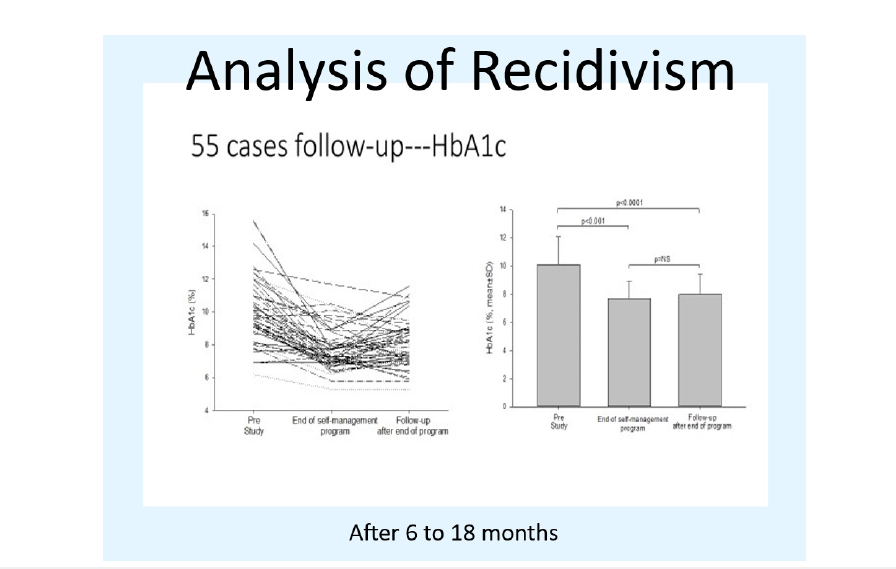
We were concerned whether a patient after discharge would experience a deterioration of control after discharge and for that reason, followed patients for a mean of 16 months [6]. In these patients, the mean HbA1C levels at the time of discharge and during follow up did not change. As shown in the Figure 1, some patients improved and others deteriorated slightly, but not to baseline, over the period of follow up. During the program, the average number of telephone calls per 6 months was 20. The number of new referrals ranged from a maximum of three per week to none and the average number approximately one per week. An estimated amount of my time spent per week averaged about 5 hours.
We were concerned that there was no decrease in average weight inpatients even though they had received nutritional advice. We decided to conduct a pilot study using meal replacements to see if this resulted in weight loss [1,9,10]. The meal replacement provided 1450 to 1500 calories daily for men and 1200 to 1250 in women. The diet consisted of 45-55% carbohydrate, 20-30% protein and ≤30% fat. On these diets, body weight dropped by 7.1% from 271±16 to 252±11 pounds (SEM) p=0.009) and insulin levels decreased by 50%. HA1c levels at baseline were 9.85±0.33% (SEM) at baseline and 7.77±0.47% at the end of the protocol. Compliance on the diet was assessed on a 0-10 scale and the average was highly variable but during weeks 1-4, 5-12, 14-20 and 21-24 were 8.85, 8.61, 7.66, and 8.0. No patient developed hypoglycemia while on meal replacements. Continuous glucose monitoring was utilized at the start of the meal replacement in order to detect hypoglycemia at that time. This occurred in the first patient and thereafter insulin doses were decreased by 50% upon start of the meal replacement.
For the patients with other endocrine disorders, I took over the primary care and management until the patients were treated and placed on stable long-term management. As an example, patients with hyperthyroidism were treated either with surgery, radioactive iodine, or anti-thyroid therapy and followed by telephone or telemedicine visits. Communication with the CDCES facilitated ordering of laboratory tests or scheduling of ultrasounds and nuclear medicine testing. For the patients with other endocrine disorders, long term follow-up included routine three-month review of all records and telephone and telemedicine visits as appropriate.
Discussion
My personal experience supports the value of telemedicine to consult and manage patients with diabetes mellitus living in rural, underserved areas. As a retired endocrinologist, this represents a way to benefit patients and to give back to the profession on a “pro bono” basis. As I have been serving as a telemedicine consult for 8 years, I have been able to judge the pros and cons of such programs. The time commitment is about five hours per week and the specific appointment times for the initial visit and for the telephone calls are completely flexible. The contact with patients and the observations that they are improving with respect to glucose control are quite rewording. As a physician continuing to practice at the University of Virginia Endocrine Clinic, I have time limits of 45 minutes for new patients and 20 minutes for follow ups. This time constraint limits the ability to get to know patients and causes anxiety about keeping to schedule. With telemedicine, my schedule is not time constrained and I feel comfortable asking about lifestyle, hobbies, and other patient activities and family issues. Most importantly, I find that participating in the care of these patients is very rewording for me and has markedly benefited the patients. With the collaboration with a CDCES, this type of consultation practice is “practicing medicine without the hassles”. The cons are that this activity is neutral with respect to financial earnings and involves a number of steps to initiate the program. For those physicians whose medical licenses have lapsed during retirement, reinstatement is required. However, most states have plans to make this fairly straightforward. One needs excellent internet and computer facilities. On balance, the benefits clearly outweigh the problematic issues.
For retired endocrinologists to initiate their own telemedicine programs in the United States, this manuscript provides a step-bystep method to make this possible. The FQHCs have the greatest unmet need for consultant endocrinologists. A state-by-state list of all of these FQCHCs is available on line. Connection with the CEOs of these Centers provides a means of determining their willingness and need for Endocrine Specialty services. My experience can provide a template for anyone interested in setting up this program. I am willing to assist and can be reached through my e-mail, rjs5y@ uvahealth.org. In summary, use of telemedicine for the specialty care of patients with diabetes and other endocrine disorders is valuable and provides a means for retired endocrinologists to continue to practice their specialty in a system without the hassles associated with working in a large bureaucratic organization or small private practice. The expertise gained over several years of practice can be utilized to markedly benefit patients.
References
- Santen RJ CC, Horton C, Nass R, Yue W (2023) Meal replacements in conjunction with an integrated technology-drive strategy for treament pf patoients with diabetes in rural, underserved areas: A pilot study. Trends Telemed & E-Health 4(1): 1-8.
- Ross S, Benavides VS, Schumann L, Haberman M (2015) Issues that impact type-2 diabetes self-management in rural communities. J Am Assoc Nurse Pract 27(11): 653-660.
- Myers CA, Slack T, Broyles ST, Heymsfield SB, Church TS, et al. (2017) Diabetes prevalence is associated with different community factors in the diabetes belt versus the rest of the United States. Obesity 25(2): 452-459.
- Marsh Z, Teegala Y, Cotter V (2022) Improving diabetes care of community-dwelling underserved older adults. J Am Assoc Nurse Pract 34(10): 1156-1166.
- Klonoff DC (2016) Telemedicine for diabetes: Economic considerations. J Diabetes Sci Technol 10(2): 251-253.
- Santen RJ, Nass R, Cunningham C, Horton C, Yue W (2023) Intensive, telemedicine-based, self-management program for rural, underserved patients with diabetes mellitus: Re-entry of retired endocrinologists into practice. J Telemed Telecare 29(2): 153-161.
- Lee EK, Donley G, Ciesielski TH, Freedman DA, Cole MB (2023) Spatial availability of federally qualified health centers and disparities in health services utilization in medically underserved areas. Soc Sci Med 328: 116009.
- Santen RJ (2020) Re-booting after retirement: Novel approach using telemedicine to solve the work-force gap in diabetes management. Maturitas 133: 68-69.
- Kempf K, Rohling M, Niedermeier K, Gartner B, Martin S (2018) Individualized meal replacement therapy improves clinically relevant long-term glycaemic control in poorly controlled type 2 diabetes patients. Nutrients 10(8): 1022.
- Cheskin LJ, Mitchell AM, Jhaveri AD, Mitola AH, Davis LM, et al. (2008) Efficacy of meal replacements versus a standard food-based diet for weight loss in type 2 diabetes: A controlled clinical trial. Diabetes Educ 34(1): 118-127.
© 2026 Richard J Santen MD. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






