- Submissions

Full Text
Significances of Bioengineering & Biosciences
Smart Prosthetics: A Systematic Review of 3D-Printed Myoelectric Limbs with Integrated Sensory Feedback
Ameh Benson Agi1, Micheal Abimbola Oladosu2*, Moses Adondua Abah3, Dominic Agida Ochuele3, Abimbola Mary Oluwajembola2, Olaide Ayokunmi Oladosu4, Bukola Oluwaseyi Olufosoye5 and Olamide Yosola Falana6
1Department of Chemistry, College of Science, University of Siegen, Germany
2Department of Chemical Sciences, Faculty of Science, Anchor University, Nigeria
3Department of Biochemistry, Faculty of Pure and Applied Sciences, Federal University of Wukari, Nigeria
4Department of Computer Science, Faculty of Science and Technology, Babcock University, Nigeria
5Department of Medical Microbiology, Faculty of Medical Laboratory Sciences, Ambrose Alli University, Nigeria
6Department of Public Health, Teesside University, United Kingdom
*Corresponding author:Micheal Abimbola Oladosu, Department of Chemical Sciences, Faculty of Science, Anchor University, Ayobo, Ipaja, Lagos, Nigeria
Submission: November 19, 2025; Published: March 11, 2026

ISSN 2637-8078Volume7 Issue 5
Abstract
The advancement of prosthetic technology has undergone a significant transformation with the incorporation of 3D printing, myoelectric control, and integrated sensory feedback systems. This systematic study analyses the contemporary field of smart prosthetics, emphasizing 3D-printed upper-limb prosthesis augmented with myoelectric data acquisition and tactile feedback systems. The paper examines advancements in materials and fabrication methods, namely the application of biocompatible polymers and soft robotics, alongside control schemes that encompass signal processing and actuation. It also assesses sensor integration, such as touch and pressure sensors, and the consequent enhancements in clinical and functional outcomes, including dexterity, user comfort, and cost-effectiveness. Significant limitations, including power supply issues and user adaptability, are thoroughly examined, with recommendations for enhancing usability and accessibility presented. This analysis underscores the transdisciplinary advancements influencing next-generation prosthetics and stresses the necessity for scalable, user-centric solutions to improve limb replacement technologies.
Keywords: Intelligent prosthetics; Additive manufacturing; Myoelectric control; Sensory feedback; Biocompatible materials; Signal processing
Introduction
Limb loss resulting from accident, congenital anomalies, or disease profoundly affects an individual’s quality of life, mobility, and autonomy [1]. In recent decades, the domain of prosthetics has experienced significant developments, especially with the incorporation of myoelectric control systems and additive manufacturing (3D printing) technology [2,3]. These developments have led to the emergence of a new generation of smart prosthetics, intelligent, adaptable devices that can not only replicate limb movement but also deliver sensory feedback, thereby restoring a measure of tactile perception to the user [4,5]. Myoelectric prostheses operate by sensing electrical impulses from the remaining muscles in the severed limb and converting them into controlled movements of an artificial limb [2]. This control mechanism provides more intuitive and natural movement than standard mechanical prosthetics; yet, it has previously been deficient in sensory feedback, which is essential for executing delicate or precise tasks [4]. Recent research has concentrated on incorporating sensory systems, such as pressure, temperature, and proprioceptive sensors, into prosthetic design to facilitate closed-loop communication between the device and the user’s nervous system, thereby addressing this constraint [5]. The emergence of 3D printing has transformed prosthesis production by facilitating affordable, customized, and lightweight designs [3,6]. This technique facilitates swift prototyping and customized fitting, rendering advanced prosthetic options more attainable, particularly in resource-limited environments. The merger of 3D printing, myoelectric control, and sensory integration has facilitated the creation of advanced prosthetic limbs that are both functionally advanced and economically accessible, prioritizing user needs [3,6]. This systematic review seeks to rigorously evaluate the existing research and development in smart prostheses, emphasizing 3D-printed myoelectric limbs with embedded sensory feedback. The review examines design techniques, control algorithms, sensor technologies, user experiences, and clinical outcomes. The study synthesizes recent findings to identify gaps, challenges, and future directions essential for improving the functionality, usability, and accessibility of intelligent prosthetic systems.
Evolution of prosthetics
The history of prosthetics is a testament to human ingenuity in the face of physical adversity. Early prosthetic devices, dating as far back as ancient Egypt and Rome, were rudimentary and primarily cosmetic or functional substitutes for lost limbs, typically constructed from materials like wood, leather, and metal [1]. These devices lacked articulation and were largely non-functional, often serving more as symbolic replacements than true mobility aids. Significant advancements emerged in the post-World War eras, driven by the increased number of amputees and the demand for improved rehabilitation tools [1]. The mid-20th century witnessed the introduction of body-powered prostheses, which used harnesses and cables to transfer motion from the user’s body to the prosthetic limb [1]. While functionally superior to their predecessors, these devices were often bulky, uncomfortable, and limited in their range of motion. The next major leap occurred with the advent of myoelectric prosthetics in the 1960s, pioneered by Soviet researchers [2].
These devices harnessed electrical signals generated by residual muscles in the amputated limb to control motorized prosthetic components. Myoelectric systems offered more intuitive control and eliminated the need for mechanical harnesses, marking a paradigm shift in prosthetic technology. Over time, advancements in signal processing and microcontroller technology further refined the accuracy, responsiveness, and versatility of these devices [2]. In the 21st century, the field has been revolutionized by the integration of biomechanics, robotics, and neuroscience, paving the way for smart prosthetics, devices that incorporate machine learning, wireless communication, and sensory feedback systems [4,5]. Moreover, the use of 3D printing has democratized prosthetic production by enabling low-cost, customizable, and lightweight solutions tailored to individual users [3]. Simultaneously, researchers have made strides in restoring sensory perception through neural interfaces and tactile feedback systems [4,5]. These advances aim to close the feedback loop, allowing users not only to control prosthetic limbs with greater precision but also to “feel” through them, thereby improving functionality, embodiment, and user satisfaction. Thus, the evolution of prosthetics reflects a shift from static mechanical devices to intelligent, adaptive systems that enhance both motor and sensory integration [1-5]. This progression continues to be propelled by interdisciplinary innovations in biomedical engineering, materials science, and artificial intelligence.
Role of 3D printing and embedded sensors
The amalgamation of 3D printing technology and embedded sensor systems has profoundly altered the design, functionality, and accessibility of contemporary prosthetic limbs [3,6,7]. These two technologies are essential to the development of smart prostheses, providing innovative answers to enduring issues related to cost, customization, usability, and sensory integration.
Three-Dimensional printing in prosthetic design
3D printing, or additive manufacturing, facilitates the swift production of intricate and tailored prosthetic parts through Computer-Aided Design (CAD) [3]. This technology has revolutionized prosthetics by facilitating the creation of lightweight, anatomically precise, and individualized devices at a significantly reduced cost compared to conventionally produced prosthetics [3]. In contrast to traditional techniques that necessitate specialized labor and costly molds, 3D printing enables local and decentralized manufacturing of prosthetic limbs, which is especially advantageous in resourcelimited or post-disaster environments [6,8]. Additionally, it fosters user-centered design, facilitating iterative prototyping and realtime adjustments to enhance fit, comfort, and visual appeal [6]. The incorporation of biocompatible and resilient materials, including Polylactic Acid (PLA), Thermoplastic Polyurethane (TPU), and Acrylonitrile Butadiene Styrene (ABS), significantly improves the structural integrity of 3D-printed prosthetic devices, rendering them appropriate for prolonged utilization [3,9].
Integrated sensors and sensory feedback mechanisms
3D printing enhances the physical design and accessibility of prosthetics, while embedded sensors furnish the functional intelligence necessary for responsive and interactive control of prosthetics [7]. The sensors, including Electromyography (EMG), Force-Sensitive Resistors (FSRs), Inertial Measurement Units (IMUs), temperature sensors, and pressure sensors, facilitate the prosthetic limb’s ability to discern the user’s intentions and engage with the environment [7]. Myoelectric control systems employ surface EMG sensors to capture muscle impulses from the residual limb, enabling users to manipulate prosthetic movements in a more natural and intuitive way [2]. Simultaneously, pressure and tactile sensors included in the prosthetic hand or fingers can transmit feedback to the user via haptic actuators, vibrotactile systems, or neural interfaces, thus completing the sensorimotor loop [4- 5]. This integration boosts both dexterity and precision in task execution, as well as embodiment, the psychological perception that the prosthetic limb is an integral part of the user’s body [5]. This facilitates enhanced device acceptability and diminishes cognitive load during operation.
Collaborative advantages
The amalgamation of 3D printing with sensor integration establishes a versatile, scalable, and economical foundation for the advancement of smart prosthetics [3,7,10]. Sensors may be integrated directly during the printing process or affixed to modular components after production, facilitating seamless mechanical and electrical integration [10]. This convergence facilitates prosthetics that are both customized in design and responsive in function, adapting dynamically to human intent and environmental stimuli [3,7].
Materials and Fabrication
The advancement of intelligent prosthetics, specifically 3D-printed myoelectric limbs with embedded sensory feedback, depends significantly on progress in material science and digital manufacturing technology [3,11,12]. This breakthrough is fundamentally based on three essential components: soft robotics, printable electronics, and biocompatible polymers. These materials and fabrication techniques facilitate the creation of prostheses that are lightweight, adaptable, user-friendly, and functionally integrated with embedded sensors and actuators.
Compliant robotics
Soft robotics has incorporated compliant, deformable materials into prosthesis design, emulating the flexibility and dexterity of organic tissues [11]. In contrast to conventional rigid prosthetics, soft robotic actuators utilize elastomeric materials and pneumatic or hydraulic systems to facilitate fluid, multi-Degree-of-Freedom (DoF) movements [11]. These solutions augment comfort, mitigate injury risk, and enhance the natural relationship between the prosthetic limb and the user’s residual limb or adjacent surroundings. Recent advancements include the 3D printing of silicone-based actuators and the integration of fluidic networks within soft prosthetic fingers, facilitating adaptive gripping and enhancing safety in human-prosthesis interactions [11]. Soft robotic systems enable the integration of sensor arrays for pressure and strain feedback, enhancing closed-loop control methods.
Printable electronics
Printable electronics facilitate the incorporation of flexible circuits, sensors, and conductive paths directly onto prosthetic elements [10]. These circuits are produced utilizing conductive inks, such as silver nanoparticle inks, graphene-based materials, or carbon nanotube composites, via methods including inkjet printing, aerosol jet printing, and screen printing [12]. This technique facilitates the seamless integration of EMG sensors, temperature and pressure sensors, strain gauges, and wireless communication modules onto the inner or exterior surfaces of the prosthetic shell [12-13]. Consequently, real-time data collecting and signal processing can transpire without the need for cumbersome, discrete hardware. The downsizing and adaptability of printable electronics improve the cosmetic and ergonomic attributes of the prosthesis, hence fostering user acceptability and extended wearability [12].
Biocompatible polymers
Biocompatibility is essential for all wearable medical devices [11,14]. Prosthetics that sustain skin contact or interact with neurological or muscle tissues must be constructed from nontoxic, hypoallergenic materials that do not induce discomfort or inflammation after prolonged use.
Frequently utilized biocompatible materials in 3D-printed
prosthesis comprise:
Polylactic Acid (PLA): A biodegradable and dermally safe
polymer generated from renewable materials [3,9].
a) Thermoplastic Polyurethane (TPU): Esteemed for its
flexibility, durability, and comfort in dynamic joints and socket
linings [9].
b) Polycaprolactone (PCL): A gradually disintegrating
polymer frequently utilized in bespoke orthopedic and
prosthetic applications [9].
c) Silicone elastomers are utilized for soft liners, finger pads,
and flexible joints in prosthetics that incorporate soft robotic
mechanics [9,11].
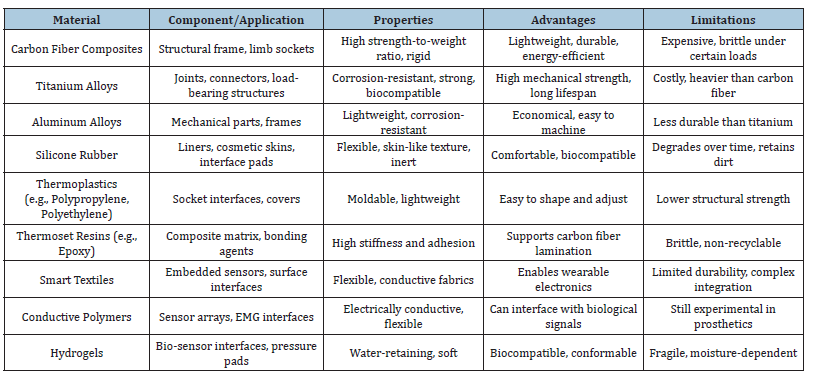
These materials are suitable for several additive manufacturing methods, including Fused Deposition Modelling (FDM), Stereolithography (SLA), and Selective Laser Sintering (SLS) [3,9]. Besides mechanical integrity and biocompatibility, numerous polymers provide post-processing methods for surface modification or sensor integration. The integration of soft robotics, printable electronics, and biocompatible polymers has advanced the domain of smart prosthetics, resulting in more adaptable, functional, and cost-effective solutions [3,9,11,12]. These material advancements not only diminish manufacturing complexity and expenses but also facilitate the seamless integration of sensing and actuation systems vital for responsive and intuitive prosthetic limbs. Table 1 presents the materials used in Smart Prosthetic Fabrication.
Table 1:Materials used in smart prosthetic fabrication [3,9,11,12].
Control Strategies
The efficacy of smart prosthetics is primarily contingent upon sophisticated control algorithms that decode user intent and convert it into accurate and lifelike prosthetic motion [2,15]. Myoelectric control, together with real-time data processing and actuation, constitutes the foundation of contemporary upper-limb prostheses. These solutions facilitate intuitive control, enhance motion precision, and allow for the possibility of closed-loop feedback systems [2,5,15].
Myoelectric signal acquisition
Myoelectric control utilizes surface Electromyography (sEMG)
to identify the electrical activity produced by muscle contractions
in the residual limb [2]. These signals are obtained using surface
electrodes positioned across designated muscle groups, usually
the flexor and extensor muscles in the forearm or upper arm [2].
Essential elements of myoelectric acquisition comprise:
a. Electrodes: Dry or moist surface electrodes non-invasively
acquire EMG signals [2].
b. Amplifiers: Low-amplitude EMG signals are augmented to
guarantee precision in detection [2].
c. Band-pass filters (often 10-500 Hz) are utilized to remove
noise and motion distortions [2].
d. Analog-to-Digital Conversion: Signals are digitized for
processing by internal microcontrollers or external processors
[2]. The acquisition procedure is acutely dependent on
electrode positioning, skin impedance, and individual muscle
physiology, requiring calibration and frequently personalized
adjustment of the prosthetic system [2,16].
Signal processing and actuation
Upon acquisition of the EMG signals, they undergo a sequence of computer processes for analysis and activation [2,15].
Signal processing pipeline: Preprocessing encompasses
filtering, normalizing, and signal rectification [15].
a. Feature Extraction: Time-domain features, such as mean
absolute value and waveform length, together with frequencydomain
features, including median frequency and zero
crossings, are calculated [15].
b. Classification Algorithms: Machine learning algorithms,
including Support Vector Machines (SVM), Artificial Neural
Networks (ANN), K-Nearest Neighbors (KNN), and Linear
Discriminant Analysis (LDA), are utilized to categorize signal
patterns into designated motions or movements [15].
c. Regression Models: In proportional control, regression
models predict force or velocity of movement based on EMG
amplitude [15].
Actuation mechanism: Subsequent to signal classification
or regression, control commands are transmitted to actuators,
typically DC motors, servo motors, or pneumatic actuators,
integrated into the prosthetic device [10]. Actuation methods may
include:
a) Position-oriented: The actuator adjusts the prosthetic
joint to a specified angle [10].
b) Velocity-based: The actuator modulates joint velocity in
accordance with the intensity of the EMG signal [10].
c) Force-based: The actuator provides grip force
commensurate with muscle activation [10].
These actuators are generally synchronized through microcontrollers (e.g., Arduino, STM32, or Raspberry Pi) that oversee motor control, power management, and sensor integration [10].
Integration of sensory feedback (towards closed-loop control)
Advanced control strategies seek to provide bidirectional
prosthetics through the use of sensory feedback mechanisms,
including [4-5]:
i. Tactile sensors (force, pressure, or deformation) [7,13].
ii. Vibrotactile and electro tactile feedback mechanisms [4].
iii. Peripheral nerve stimulation or transcutaneous electrical
nerve stimulation (TENS) [5].
This allows the prosthetic system to deliver instantaneous input about contact, grip strength, and object texture, hence enhancing fine motor control and embodiment [5]. Myoelectric control methodologies enhanced by advanced signal processing and actuation systems have transformed prosthesis technology. They provide amputees with enhanced control precision, natural movement dynamics, and, progressively, a level of sensory perception [2,5,15]. The integration of bio-signal acquisition, machine learning, and soft actuation represents a crucial advancement towards fully autonomous, user-adaptive, and intelligent prosthetic limbs. Table 2 shows the summary of control methods and performance while Figure 1 illustrates the Myoelectric Control Workflow.
Table 2:Summary of control methods and performance [2,10,15].
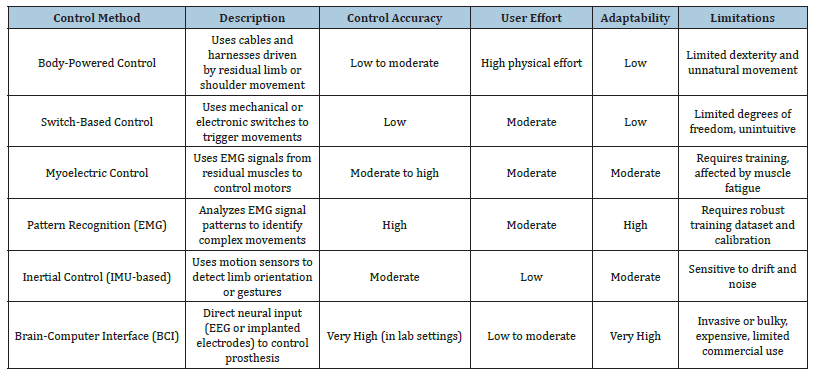
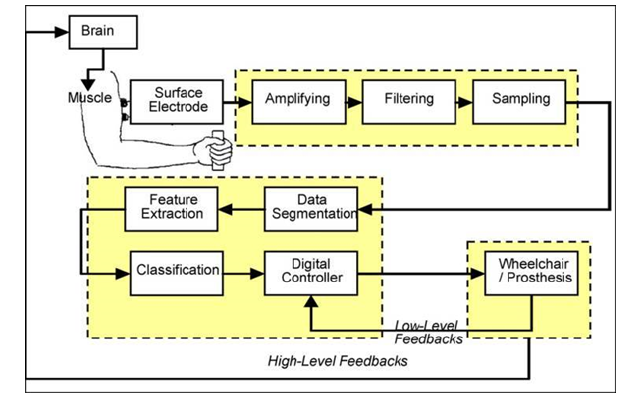
Figure 1:Myoelectric control workflow [17].
Sensor Integration
The incorporation of touch and pressure sensors with haptic feedback systems is crucial for converting passive prosthetic limbs into intelligent, user-responsive devices [4,7,13]. These components facilitate closed-loop control by enabling the prosthetic to detect interactions with the external world and transmit sensory information to the user, thereby improving precision, embodiment, and user confidence [4-5].
Tactile and pressure sensors in advanced prosthetics
Tactile and pressure sensors function as the principal sensory interfaces in intelligent prosthetic systems, facilitating the detection of physical interactions including grip force, object texture, slippage, and surface compliance [7,13]. These sensors are essential for mimicking normal hand function and responsiveness. Diverse sorts of touch sensors are utilized according to their operational principles. Piezoresistive sensors, which modify electrical resistance in response to pressure, are frequently utilized for their simplicity and cost-efficiency, especially in fingertip applications [13]. Capacitive sensors, recognized for their enhanced sensitivity, identify variations in capacitance resulting from surface contact or deformation [13]. Piezoelectric sensors produce voltage when subjected to mechanical stress and are especially adept at detecting dynamic touch and vibrations [13]. Furthermore, optical and magnetic sensors are employed for the detection of surface deformation and proximity. To facilitate seamless incorporation into prosthetic designs, these sensors are typically manufactured on flexible substrates by printed electronics, enabling adaptation to curved surfaces like fingertips, palms, and wrist joints [13]. The positioning of sensors is intentionally optimized throughout the prosthetic limb [7]. Fingertips facilitate precise tactile perception and force application; the palmar and phalangeal areas analyses load distribution; whilst the wrist and forearm regions aid in evaluating force vectors and adaptive grip modifications. The acquired sensory data is processed by embedded microcontrollers or onboard computing systems, where algorithms evaluate the inputs to produce suitable actuation responses or deliver real-time user feedback [7,15].
Haptic feedback systems
Haptic feedback is an essential element that finalizes the sensorimotor loop in smart prosthetics, allowing the prosthetic to convey sensory information to the user [4-5]. This functionality is crucial for reinstating tactile sensation and proprioception, enabling amputees to proficiently manage grip strength, discern object properties, and react to environmental stimuli with diminished reliance on visual cues [4]. Multiple haptic feedback modalities are frequently employed. Vibrotactile feedback employs vibrating motors positioned on the residual limb or other skin-contact areas to provide stimuli, with variations in vibration frequency or amplitude signifying grip intensity or contact location [4]. Electro tactile stimulation utilizes regulated electrical impulses transmitted via surface electrodes to stimulate underlying nerves; although technique provides excellent precision, user acclimation may be necessary to mitigate discomfort [4]. Mechan tactile feedback utilizes actuators to exert mechanical pressure or deformation on the skin, thereby emulating a more immediate tactile experience or force feedback [4]. Innovative techniques encompass temperaturebased feedback, which conveys information via thermal fluctuations to signify item temperature or interaction context [4].
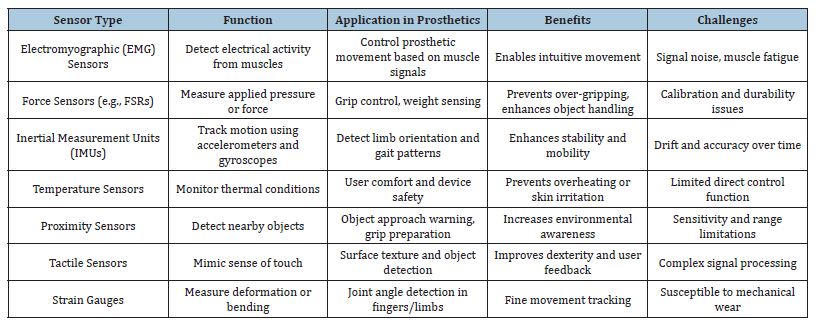
Feedback can be categorized into various strategies: eventcentric feedback is triggered solely by specific occurrences, such as object contact or slippage; continuous feedback is delivered in accordance with real-time sensor inputs, such as grip strength; and location-specific feedback correlates sensor data to particular regions of the skin to improve spatial awareness [4]. Feedback is normally supplied to the residual limb, but alternate places such as the contralateral limb, chest, or back are also examined for more effective sensory mapping [4]. The incorporation of these haptic feedback systems provides several advantages, such as improved grip force management, enhanced item manipulation, heightened spatial and kinetic awareness, and alleviation of phantom limb pain [4-5]. Moreover, it fosters an enhanced sense of embodiment and psychological comfort for users. The integration of touch sensors and sophisticated haptic feedback systems signifies a pivotal transition from passive prosthetic devices to dynamic, responsive smart prosthetics, greatly improving their functionality and user acceptance [4,5,7,13]. Table 3 highlights the Types and Roles of Embedded Sensors.
Table 3:Types and roles of embedded sensors [2,7,13]..
Clinical and Functional Outcomes
The efficacy of smart prosthetics, particularly those utilizing 3D printing, myoelectric control, and sensory input, is ultimately assessed by their clinical and functional results [4,6,14]. These outcomes influence the practical effects on users’ quality of life, daily functioning, and acceptance of the prosthetic device. The principal domains evaluated encompass dexterity, comfort, and cost-effectiveness.
Agility
Dexterity denotes the prosthesis user’s capacity to execute intricate and accurate hand and finger movements, essential for activities spanning from gross motor functions to fine manipulation [4,6]. The influence of myoelectric control and sensory feedback: Research consistently indicates that myoelectric prostheses equipped with sensory feedback systems enhance dexterity in comparison to body-powered or passive devices [4]. The closedloop control enabled by tactile and haptic feedback permits users to adjust grip force, minimise item slippage, and execute intricate operations such as buttoning or typing [4-5]. 3D-Printed Prosthetics and Dexterity: Customizable 3D-printed designs provide optimum articulation of finger joints and tailored mechanical properties, hence enhancing functional hand movements [6]. Nonetheless, constraints in actuator strength and sensor resolution may occasionally diminish precision in challenging jobs [6]. Assessment Instruments: Standard clinical evaluations for dexterity are the Box and Block Test (BBT), Nine-Hole Peg Test (NHPT), and Southampton Hand Assessment Procedure (SHAP) [4].
Comfort
Comfort is a crucial determinant affecting prosthesis usage duration and user contentment, including socket fit, weight, material biocompatibility, and ergonomic design of the user interface [14]. Socket and Interface Design: Innovations in 3D scanning and printing permit custom sockets that precisely match the contours of the residual limb, hence minimizing pressure points and skin discomfort [14]. The utilization of soft biocompatible polymers and flexible liners improves comfort [9,14]. The lightweight characteristics of 3D-printed polymers, in contrast to conventional prosthetic materials, mitigate fatigue over extended usage [9]. Research indicates that sensory feedback systems enhance users’ psychological comfort by augmenting limb embodiment and alleviating phantom limb pain [5].
Economic efficiency
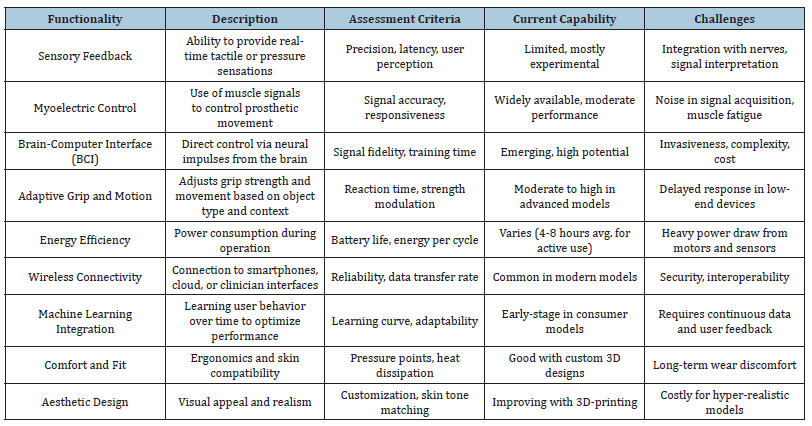
Cost-effectiveness pertains to the financial accessibility of the prosthetic as well as the enduring value provided in terms of functionality and durability [3,6,8]. 3D Printing and Cost- Effectiveness: 3D printing markedly decreases production expenses by minimizing material waste, facilitating quick prototyping, and permitting local fabrication without the need for costly tooling or assembly lines [8]. This is especially significant in resource-limited environments [17]. Maintenance and Repair: Modular designs and the capacity to swiftly fabricate replacement components diminish downtime and repair expenses in comparison to conventional prosthetics [8]. Notwithstanding cost benefits, the requirement for sophisticated electronics, sensors, and actuators in smart prostheses may elevate total expenditures [10]. Nonetheless, continuous advancements in affordable sensors and open-source control systems seek to close this gap [6,8]. The clinical and practical results of smart prostheses demonstrate significant enhancements in dexterity and comfort due to advanced materials and sensing technologies, while cost-effectiveness is progressively being tackled through additive manufacturing [3,4,6,8,9,14]. Nonetheless, ongoing advancement is essential to reconcile intricate control and feedback systems with cost-effectiveness and enduring usability. Table 4 presents Functional Assessment of Smart Prosthetics.
Table 4:Functional assessment of smart prosthetics [4,5,10,14,15].
Limitations and Future Directions
Smart prostheses signify a significant advancement in prosthetic technology, integrating 3D printing, myoelectric control, and sensory feedback, yet they encounter numerous technological, physiological, and practical constraints that hinder general adoption [8,16,18]. Primary areas of concern encompass power supply issues, user flexibility, and comprehensive integration into healthcare systems.
Challenges in power supply
A significant obstacle to the functionality and usability of smart prostheses is a dependable and efficient power source. Battery Life Constraints: The incorporation of sensors, actuators, microcontrollers, and wireless feedback systems markedly elevates power consumption. Most myoelectric prosthetics depend on lithium-ion batteries, which generally offer restricted operational duration (usually 6-12 hours) before requiring recharging. Bulky Battery Packs: Achieving longer battery life sometimes comes at the cost of greater bulk and weight, compromising comfort and prosthetic aesthetics. Energy Efficiency: Current actuators and sensor systems are not optimized for low-energy operation, and energy regeneration technologies (e.g., from limb motion) are currently under development. Prospective Trajectories: Advancement of lightweight, high-capacity energy storage solutions (e.g., graphene batteries, flexible supercapacitors). Integration of energy-harvesting systems (e.g., piezoelectric generators or thermoelectric materials). Utilization of lowpower microcontrollers and signal processors to enhance energy efficiency [10].
User flexibility
Despite advanced technology, user adaptability continues to be a crucial limiting factor affecting the long-term success and acceptance of smart prosthetics [16,18]. Training and Learning Curve: Operating myoelectric limbs with integrated feedback necessitates neuromuscular training to interpret signals and haptic feedback [16]. Numerous users, particularly elderly individuals or those with extended limb loss, encounter challenges in mastering these systems [16]. Cognitive Load: The continuous influx of sensory information and control impulses may result in cognitive fatigue, especially with intricate multi-degree-of-freedom prosthetics [16]. Psychological Factors: Embodiment, perceived usefulness, and device aesthetics all influence user satisfaction [18]. Some users endure dissatisfaction or abandonment due to device complexity or social stigma [18]. Prospective Trajectories: Creation of adaptive machine learning algorithms that tailor control systems to the user’s EMG patterns and preferences [15-16]. Improved user interface designs to facilitate feedback analysis [4,16]. Extended rehabilitation programs and virtual training settings to enhance adaption and confidence [16].
Supplementary challenges and prospects
Sensor Resilience and Longevity: Numerous implanted sensors
deteriorate due to perspiration, particulate matter, or continuous
mechanical strain [7,13]. Integration with Neural Interfaces:
Although promising, direct interaction with peripheral nerves
or cerebral signals remains predominantly experimental [5].
Affordability and Accessibility: Although smart prosthetics are
more economical through 3D printing, they remain excessively
costly in low-income environments due to component expenses
and insufficient clinical infrastructure [3,6,8].
Future research opportunities: Standardization
of manufacturing and evaluation methods [19]. Greater
interdisciplinary collaboration among materials scientists,
neuroscientists, and rehabilitation specialists [19-20]. Expansion
of open-source hardware and software platforms to democratize
innovation [6,8].
Final assessment
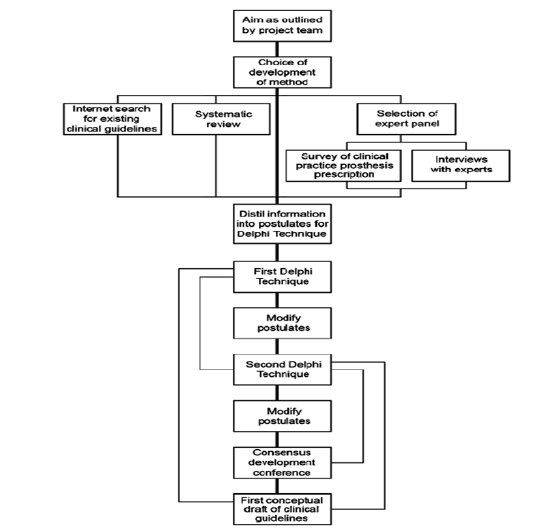
Although intelligent prosthetics are initiating a novel epoch of user-interactive, anatomically adaptive mechanical limbs, significant issues in power efficiency, user training, and technological resilience require resolution [10,16,18,19]. Addressing these disparities necessitates ongoing research, user-centric design, and scalable manufacturing technologies to completely actualize the promise of prosthetics that restore both functionality and feeling. Recent comprehensive reviews have systematically examined the manufacturing challenges associated with 3D-printed robotic prostheses [19]. These challenges encompass material limitations, precision requirements in additive manufacturing, integration of electronic components, and quality control protocols [19]. Addressing these technical barriers is essential for advancing the reliability, durability, and accessibility of next-generation prosthetic devices. Future innovations must focus on developing standardized manufacturing protocols, improving material properties for long-term biocompatibility, and establishing rigorous testing frameworks to ensure consistent performance across diverse manufacturing platforms [19]. Table 5 shows the Key Gaps and Innovation Opportunities while Figure 2 presents the Design Roadmap for Future Prosthetics.
Table 5:Functional assessment of smart prosthetics [4,5,10,14,15].
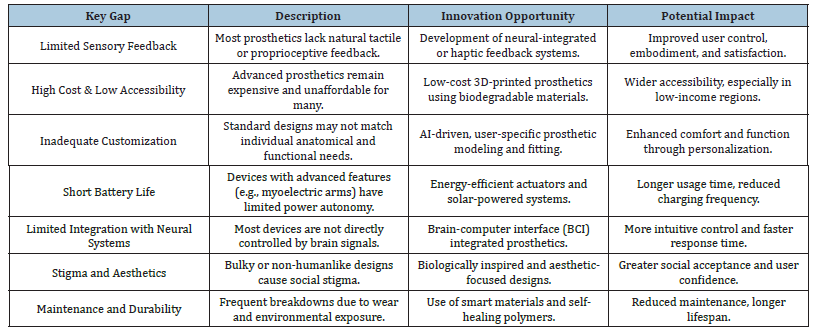
Figure 2:Design roadmap for future prosthetics [20].
Conclusion
Intelligent prosthetics are transforming the realm of assistive technology by integrating 3D printing, myoelectric control, and embedded sensory input into practical, user-centric artificial limbs. These innovations are augmenting the dexterity, comfort, and customization of upper-limb prostheses, providing users with more control and a heightened sensation of embodiment. 3D printing has transformed prosthetic design and production, facilitating rapid prototyping, reducing costs, and allowing for customization that meets the specific anatomical and functional requirements of everyone. Incorporating inbuilt touch and pressure sensors, smart limbs now provide haptic feedback, enabling users to execute delicate motor tasks with enhanced confidence and precision. Notwithstanding these advancements, the domain encounters significant restrictions, such as power supply constraints, sensor durability issues, and obstacles in user adaptability. Resolving these issues necessitates additional interdisciplinary research, especially in energy-efficient components, adaptive machine learning methods, and cost-effective open-source solutions. The integration of soft robotics, biocompatible materials, and intelligent control systems is advancing prosthetic technology towards a future in which artificial limbs serve as both functional replacements and responsive extensions of the human body. Future technologies must stress usability, clinical efficacy, and global accessibility to promote equitable and sustainable deployment.
Acknowledgment
The authors acknowledge all the researchers whose work serve as reference material for the writing of this review work.
References
- Klein C (1979) The history of prosthetics. Orthotics and Prosthetics 33(3): 17-23.
- Farina D, Jiang N, Rehbaum H, Holobar A, Graimann B, et al. (2014) The extraction of neural information from the surface EMG for the control of upper-limb prostheses: Emerging avenues and challenges. IEEE Trans Neural Syst Rehabil Eng 22(4): 797-809.
- Ten Kate J, Smit G, Breedveld P (2017) 3D-printed upper limb prostheses: A review. Disabil Rehabil Assist Technol 12(3): 300-314.
- Antfolk C, D'Alonzo M, Rosén B, Lundborg G, Sebelius F, et al. (2013) Sensory feedback in upper limb prosthetics. Expert Rev Med Devices 10(1): 45-54.
- Raspopovic S, Capogrosso M, Petrini FM, Bonizzato M, Rigosa J, et al. (2014) Restoring natural sensory feedback in real-time bidirectional hand prostheses. Sci Transl Med 6(222): 222ra19.
- Zuniga JM, Katsavelis D, Peck J, Stollberg J, Petrykowski M, et al. (2015) Cyborg beast: A low-cost 3D-printed prosthetic hand for children with upper-limb differences. BMC Res Notes 8: 10.
- Dosen S, Popović D (2011) Accelerometers and force sensors for evaluating voluntary grasp force control in myoelectric prostheses. Med Eng Phys 33(7): 867-875.
- Mavroidis C, Sivak ML, Cha K, Patritti BL, Lavalle C, et al. (2017) The role of 3D printing in the design of prosthetic limbs. Int J Adv Manuf Technol 91: 2231-2241.
- Hussain T, Malik MH, Iqbal J, Ansari MS (2020) Additive manufacturing of personalized prosthetics: A review of current approaches. Adv Eng Mater 22(6): 1901302.
- Pylatiuk C, Schulz S, Doderlein L (2007) Results of an internet survey of myoelectric prosthetic hand users. Prosthet Orthot Int 31(4): 362-370.
- Ilievski F, Mazzeo AD, Shepherd RF, Chen X, Whitesides GM (2011) Soft robotics for chemists. Angew Chem Int Ed 50(8): 1890-1895.
- Sekitani T, Noguchi Y, Hata K, Fukushima T, Aida T, et al. (2008) A rubberlike stretchable active matrix using elastic conductors. Science 321(5895): 1468-1472.
- Kim DH, Lu N, Ma R, Kim YS, Kim RH, et al. (2011) Epidermal electronics. Science 333(6044): 838-843.
- Pezzin LE, Dillingham TR, MacKenzie EJ, Ephraim P, Rossbach P (2004) Use and satisfaction with prosthetic limb devices among persons with trauma-related amputations. Arch Phys Med Rehabil 85(5): 723-729.
- Oskoei MA, Hu H (2008) Support vector machine-based classification scheme for myoelectric control applied to upper limb. IEEE Trans Biomed Eng 55(8): 1956-1965.
- Castellini C, Gruppioni E, Davalli A, Sandini G (2014) Real-time myoelectric control of a multi-fingered hand prosthesis using principal components analysis. J NeuroEngineering Rehabil 11(1): 1-15.
- Alshamsi H, Jaffar S, Li M (2016) Development of a local prosthetic limb using artificial intelligence. Int J Innov Res Comput Commun Eng 4(9):
- Biddiss E, Chau T (2007) Upper-limb prosthetics: Critical factors in device abandonment. Am J Phys Med Rehabil 86(12): 977-987.
- salazar m, portero p, zambrano m, rosero r (2025) Review of robotic prostheses manufactured with 3D printing: Advances, challenges, and future perspectives. Appl Sci 15(3): 1350.
- Van der Linde H, Hofstad CJ, Van Limbeek J, Postema K, Geertzen JH (2005) Use of the delphi technique for developing national clinical guidelines for prescription of lower-limb prostheses. J Rehabil Res Dev 42(5): 693-704.
© 2026 Micheal Abimbola Oladosu, This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






