- Submissions

Full Text
Researches in Arthritis & Bone Study
Shoulder Dislocation & Rotator Cuff Tears a Challenging Combo!!
Suresh Kishanrao*
Department of Family Physician & Public Health Consultant, India/p>
*Corresponding author:Suresh Kishanrao, Family Physician & Public Health Consultant, Bengaluru, Karnataka, India
Submission: January 05, 2026;Published: February 11, 2026
Volume2 Issue3February 11, 2026
Abstract
Introduction: The shoulder is one of the most mobile and unstable joints of the human body. When the
head of the humerus pops out of the shoulder blade’s socket called the glenoid it is called dislocation.
Shoulder Dislocation (SD) is primarily caused by traumatic injuries especially among elderly falling in
bathroom, and among youth by direct blows in sports or vehicle accidents, or extreme rotation, forcing
the humerus head out of the socket, often with the arm raised or twisted. Other causes include underlying
ligament laxity, electric shocks and seizures, which can cause muscles to contract violently and pull the
joint out of place. The powerful force causing a dislocation can easily tear one or more tendons stabilizing
the humerus especially the rotator cuff, making them a frequent combination, particularly in older
individuals.
Materials & methods: This article aims to report in all five cases shoulder dislocation. Two cases of
primary dislocation, one case each of accidental dislocation, chronic dislocation and bilateral dislocation
and their management. It shows that in the elderly shoulder dislocation is often associated with a rotator
cuff tear and becomes a challenge for rehabilitation.
Outcome: The elderly patient had to undergo arthroscopy, for a trivial injury due to a fall, The young
football player needed the labral tear repair arthroscopically followed by mini-open rotator cuff repair
and took almost a year to resume his sports. The chronic shoulder dislocation case had temporary relief
with cortisone injection but had to undergo rotator cuff repair surgery followed by physiotherapy a year
later after three injections, bicycle accident patient had to undergo surgical intervention, physiotherapy
to recover complete range of movements in about 16 weeks. Other elderly with bilateral dislocation were
treated with closed reduction under procedural sedation, put in sling for immobilization for 6 weeks to
allow healing.
Keywords:Shoulder; Head of humerus; Glenoid; Luxation; Sub-luxation; Arthroscopy; Physiotherapy; Xray; MRI; CT scan
Abbreviations: RCT: Rotator Cuff Tear; ROM: Range of Motions
Introduction
The shoulder is one of the most mobile and unstable joints of the human body. When the head of the humerus pops out of the shoulder blade’s socket called the glenoid it is called dislocation. Shoulder Dislocation (SD) is primarily caused by traumatic injuries, especially among elderly falling in bathroom, and among youth by direct blows or collusions in sports or vehicle accidents, or extreme rotation, forcing the humerus head out of the socket, often with the arm raised or twisted. The impact /injury can also damage the tissue around the shoulder joint, like tendons, muscles, nerves ligaments and blood vessels. Sometimes extreme rotation, when the arm is raised or twisted can force the humerus head out of the socket. Other rare causes include ligament laxity, electric shocks and seizures, that cause muscles to contract violently and pull the joint out of place [1].
Two types of SD are described in literature
i) Complete dislocations known as luxation, in which the bones in the shoulder joint
are totally separated and pushed out of place
ii) Subluxation -a partial dislocation. A powerful force causing a dislocation sometimes
tears one or more tendons stabilizing the humerus, common being the rotator cuff,
making them a frequent combination, particularly in elderly people [2].
Among youth and middle-aged shoulders injuries are common in contact sports, such as football, hockey, volleyball, tennis or sports that involve falls, or collusions like downhill skiing, gymnastics, swimming, football, Volleyball, hocky or weightlifting. A hard blow to the shoulder during a motor vehicle accident or landing awkwardly after a fall, after a 2-wheeler accident or a fall from a ladder or from tripping on a loose rug, or slippery bathroom also dislocate a shoulder [3]. Patients present with gradual or sudden pain, weakness, reduced Range of Motions (ROM), difficulty with overhead activities. Management depends on type of dislocation, additional injuries like tear size, patient age, activity level and concomitant injuries. Non-surgical approaches are immobilization of the shoulder using string around the neck, analgesics, initially complete rest, followed by physiotherapy, to rehabilitate over few weeks or months. Chronic and long-term SD pain are managed by intra-articular Cortisone injections for partial tears. Surgical approaches include tendon repairs tendon transfers and reverse shoulder arthroplasty for massive or full thickness rotator cuff tears. The outcomes are measured by pain relief, improved Rotator Cuff Tears (RCT), strength, and final recovery to pre-injury levels. Physiotherapy is essential for both pre- and post-operative recovery, focusing on pain, Range of Motions (ROM) and strength. Many patients, even with significant tears, achieve functional recovery with appropriate treatment. Patients who sustain shoulder dislocation should be evaluated for a rotator cuff tear, particularly if older than 40. Reverse total shoulder arthroplasty is a treatment of choice for elderly with irreparable cuff tears and post-instability arthropathy [3]. This article is prompted by a shoulder dislocation case following a trivial injury in elderly person recently and four other cases in last 5 years, attended by the author with orthopedic surgeons.
Case Reports
Case report 1: Rotator cuff Injury in elderly
An elderly male aged 93 years, presented with symptoms of instability, pain, and restricted shoulder movement after tripped and fell in the bathroom, directly injuring his left shoulder. Despite the seemingly minor nature of the fall, he sustained tears of her supraspinatus and subscapularis tendons. On examinations we found synovitis around the rotator interval, long head of the bicep’s tendinitis, and tears of the subscapularis tendon, supraspinatus tendon and subacromial bursitis. The anterior labrum was normal. As primary traumatic shoulder dislocation in the elderly is often associated with rotator cuff injury, a detailed evaluation and management of the rotator cuff injury was done. Arthroscopy was performed in this patient.
Case report 2: Direct strike related shoulder dislocation in a young football player
An 18-year-old football player presented to my clinic for five days following an initial left anterior shoulder dislocation in January 2025. He recovered from a fumbled ball when he was struck by two other players and felt his left shoulder dislocated. As on-the-field reduction was unsuccessful; he was taken to a private orthopedics who did a reduction under sedation. My examination, at presentation there was occasional paraesthesia’s in the left ring & little finger. He was a muscular, 90kg, collegiate football player with minimal left shoulder swelling. His range of motion on the left was significantly decreased, particularly to abduction and external rotation. His supraspinatus was also weak and very painful to strength testing but both anterior and posterior portions of the deltoid were intact. No Neurovascular deficits were there. Preliminary x-rays showed an anterior shoulder dislocation without bony Bankart lesion. An MRI showed an anterior labral tear, a supraspinatus tendon tear, and a possible posterior labral tear. He was referred to as an orthopedic surgeon, whose examination under general anaesthesia revealed no shoulder instability, but some crepitus with range of motion. Arthroscopic evaluation showed an extensive detachment of the anterior labarum and a 2cm full thickness supraspinatus rotator cuff tear, but no evidence of a posterior labral tear or Hill- Sachs lesion. The heavy size of the patient and the nature of the combined injury necessitate an extensive incision for repair of both lesions on an open basis.
The labral tear was repaired arthroscopically followed by miniopen rotator cuff repair. His range of motion continued to improve without apprehension, but his shoulder girdle muscles did undergo noticeable atrophy. At 12 weeks, the patient progressed through physical therapy from passive to active exercises. At seven months post-op, the patient was back to full strength with a full range of motion except for a mild decrease in external rotation and some residual weakness without pain in his supraspinatus. At about a year post-op, follow-up the patient showed no instability, 90-95% supraspinatus strength, full range of motion and no pain.
Case report 3: A middle-aged woman with chronic shoulder pain
A 46-year-old woman presented with chronic shoulder pain persisting for 8 months after a minor injury. More pain in the night, incidental pain during internal rotation & shoulder abduction were main complaints. The pain primarily centered around the supraspinous fossa. The patient had no significant comorbidities or medical conditions. Physical examination revealed Painful arc, Positive Neer’s test, Severe pain in the anteromedial shoulder on internal rotation.
Ultrasound findings: Cortical irregularity at the level of insertion of the supraspinatus tendon synovial thickening and fluid collection in the subacromial bursa. The patient was diagnosed with a rotator cuff tear. She was treated with anti-inflammatory medicine (cortisone)injection to reduce pain and swelling in the shoulder. It resulted in effective for short-term pain relief for months, allowing better participation in physical therapy. But it did not heal the tear. Same injections were repeated thrice over one year period which weakened tendons. After a year rotator cuff repair surgery was done followed by physiotherapy.
Case report 4: Massive rotator cuff tear in a young male
A 34-year-old male cyclist moving at a low speed (10-20mph) sustained a massive rotator cuff tear and long head of biceps tendon tear after falling on an outstretched Right hand due to a light touch from a city bus coming from behind. He was unable to lift his bicycle and was suffering severe pain. Patient Presented with sudden, severe pain, inability to move arm, history of trauma. On examination there was guarding, limited range of motion abduction/external rotation and feeling of instability, loss of normal shoulder contour, prominent humeral head anteriorly with squared shoulder appearance. On palpation there was tenderness, humeral head palpable in unusual position and Range of Motion (ROM) severely limited and painful. No axillary nerve palsy (loss of sensation/weakness on lateral shoulder), pulses and capillary refill.
Investigations: Radiographs (X-ray) confirmed anterior dislocation and no fractures (Hill-Sachs, Bankart lesions, greater tuberosity fractures). He underwent surgical intervention, physiotherapy and recovered complete range of movements in about 16 weeks.
Case report 5: Bilateral shoulder dislocation after a fall while trying to sit down on a chair
An elderly female aged 75 years experienced bilateral inferior shoulder dislocation (luxatio erecta) after a “trivial fall forwards with arms outstretched while trying to sit on a chair”. Clinical exam indicated humeral head in axilla, which was confirmed by X-ray and CT scan ruled out any associated fractures (tuberosity, glenoid, acromion).
Treatment: Closed reduction under procedural sedation (traction-counter-traction) was done and Sling/brace for Immobilization was advised for 6 weeks to allow healing. He was put on analgesics, muscle relaxants and rehabilitated with physical therapy to restore range of motion and strength.
Discussion
Shoulder Dislocation (SD) is a significant problem as pathological damage that occurs is high and contributes up to 60% of all major joint dislocations [2-4] and a costly and long drawn treatment in India. The incidence of shoulder dislocation is around 23 per 100.000 person per year [5]. Acute shoulder dislocation in youth and people below 40 years is usually caused by an accident or in traumatic sports events as was in our second and fourth cases [3,4]. Dislocations occur most frequently (96%) occasionally posteriorly, and rarely inferiorly [6]. The anteroinferior shoulder dislocation consists of four types, denoted by the humeral head position: sub-coracoid (70%), sub-glenoid (25%), sub-clavicular (4%) and intrathoracic (1%). The sub-glenoid subtype is a type of shoulder dislocation located beneath the inferior rim of the glenoid which is associated with potential axillary artery injury, brachial nerve plexus complications and Rotator Cuff Tears (RCT) (Figure 1) [7]. Anteroinferior dislocation occurs with the combination of abduction, external rotation, and extension [3,5]. Rapid hyperabduction of the arm at the shoulder, with extension at the elbow and pronated arm, usually results in sub-glenoid dislocation [3,4,6]. In India among SD cases Rotator cuff injuries are around half of cases, fractures in one third and neurological damage in 5% of cases. Anterior shoulder dislocation & concurrent rotator cuff tears are common in older individuals, possibly due to the weakening of posterior structures and among younger patient’s rotator cuff tears are rare due to stronger posterior shoulder structures [8].
Figure 1:
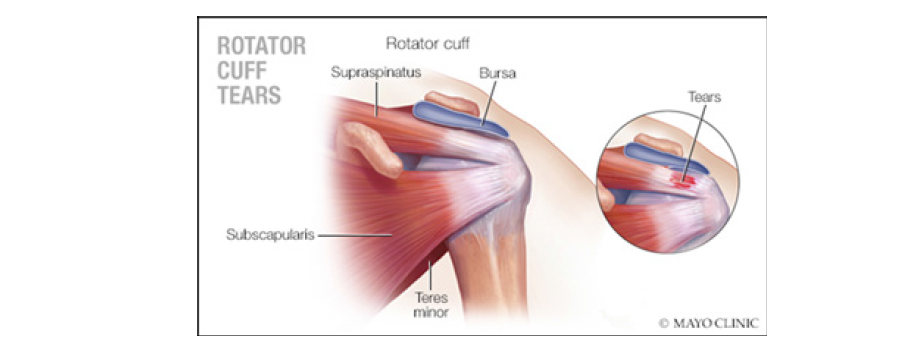
Diagnosis
Shoulder dislocation diagnosis involves
i) observing visible deformity, swelling, and pain,
ii) confirming with an X-ray to see the bone’s position and
check for fractures
iii) A physical examination assesses nerve function
(numbness/tingling) and range of motion,
iv) MRI or CT scans are used to check for soft tissue damage
like torn ligaments or rotator cuff injuries
v) Magnetic resonance imaging and arthroscopy are used to
confirm diagnosis.
Anteroposterior, lateral scapular, and axillary views of the plain X-rays are sufficient to diagnose anterior dislocations. CT scans are used to better identify bony lesions. As MRI may not differentiate between partial and full-thick rotator cuff tears; arthroscopy will be required for confirmatory diagnosis.
Key causes of rotator tears and shoulder dislocation
The key reasons for combined SD & Rotator cuff tears in India include age, mechanism of the injury and associated injuries (Figure 2). As rotator cuff tendons have degenerative changes due to natural aging, decreased blood supply, and micro-trauma over time, among elderly aged over 60 years, even a simple fall causes an acute, complete tear, whereas in a young, healthy person, a higher-energy impact is needed to cause similar injury. A common mechanism is a sudden eccentric loading of the contracting muscletendon unit, occurring when a person attempts to brace oneself with an outstretched arm. The resulting stress can exceed the tensile strength of the already weakened tendons. Trivial injuries are associated with other pathologies like Bankart or Hill-Sachs lesions, fractures, and nerve injuries (Figure 3). A Bankart lesion is a tear of the labarum of the glenoid from the bone. A Hill-Sachs lesion is a compression fracture or dent on the back of the humeral head. Both often happen during an anterior shoulder dislocation, as the humeral head slams into the glenoid rim [9]. These injuries are missed if clinicians do not suspect, due to minor trauma. Persistent severe pain or weakness after a shoulder reduction is a red flag for a potential rotator cuff tear, necessitating an MRI. Rotator cuff injuries cause loss of dynamic stabilization of the shoulder, leading to recurrent shoulder dislocation or chronic instability.
Figure 2:
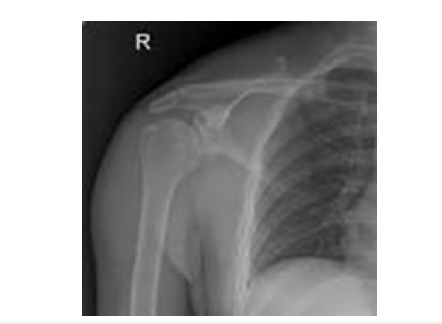
Figure 3:

Management & recovery timeline
Mild strain is managed with rest, ice pack & physiotherapy, recovering within 4 to 6 weeks. Partial tears are managed with Physical therapy & gradual strengthening which takes 2 to 3 months to recover. Full-thickness tears require surgical repair, followed by 4 to 6 months of structured rehab to return to full activity.
Chronic shoulder dislocation
Larger Hill-Sachs, due to more contracted capsule and rotator
cuff, as time progresses the problem becomes big and chronic in
nature as
i) The head becomes softer because there is no head-glenoid
contact,
ii) Increased bone loss of anterior glenoid,
iii) Internal adhesions between deltoid, cuff, and neo-capsule
strengthening the patho-anatomy,
iv) Shortening of the posterior cuff occurs,
v) The supraspinatus becomes adherent to the coracoid and
sits in a precarious surgical position for the naïve surgeon,
vi) The posterior deltoid moves anteriorly and scars in place,
vii) Heterotopic ossification occurs to make a new glenoid on
the anterior surface of the scapular neck,
viii) Subscapularis is locked in place with adhesions to the
coracoid, HO and neo-capsule.
Treatment involves physical therapy, bracing, pain management (ice/NSAIDs), Intra-joint Cortisone injections as non-surgical options. Most often chronic shoulder dislocation if frequent or interferes with daily life, requires arthroscopic stabilization, bone grafting, or shoulder replacement to repair damaged ligaments/ bone & restore stability, to rebuild strength, range of motion & prevent recurrence [8].
Bilateral shoulder dislocation
Bilateral shoulder dislocation is rare, but occurs due to severe trauma like two-wheeler accidents, diving, weightlifting, swimming, accidental drop on an armed chair or involuntary muscle contractions due to seizures or electrocution. While Posterior dislocations are more common bilaterally, anterior bilateral dislocations are very rare and often linked to specific trauma, with associated fractures [10]. Epileptic Involuntary Muscle Contractions (IMC), or electrocution also cause bilateral dislocations. Mechanism involves the shoulder in abduction and external rotation, or traction in forward flexion, causing the humeral head to come out of the socket. Severe pain, inability to move the arm, numbness, tingling, and potential muscle spasms are common symptoms. Diagnosis requires imaging (X-rays, CT scans) to confirm the dislocation and check for associated fractures (e.g., greater tuberosity). Bilateral inferior shoulder dislocations) in the elderly are extremely rare, but caused due to osteoporosis or comorbidities, leading to the humeral head going below the glenoid, not above.
Diagnosis & Management
Diagnosis: Clinical exam (humeral head in axilla) confirmed by X-ray and CT scan to check for associated fractures (tuberosity, glenoid, acromion).
Treatment: Closed reduction under procedural sedation (traction-counter-traction) is common. Followed by Immobilization using sling/brace for several weeks (4-6) to allow healing.
Medication: Pain relievers, muscle relaxants. Rehabilitation through physical therapy to restore range of motion and strength, often challenging in the elderly [11].
Associated Injuries: Rotator cuff tears, brachial plexus injury, or fractures (greater tuberosity, glenoid) are frequent associated injuries leading to complications like recurrent dislocation, instability, stiffness (periarthritis) and functional decline.
Preventing recurrent shoulder dislocations: Once there is a dislocation chances of recurrence is common, to prevent or minimize such risk patient must
i) Focus on the rotator cuff and shoulder stabilizer exercises
to support the joint.
ii) Maintain shoulder mobility without overstretching the
ligaments.
iii) Athletes must follow correct posture and movement
patterns during sports or gym activities.
iv) Practice protective measures like avoiding sudden jerks,
heavy overhead lifts or repetitive overhead motion immediately
after injury.
Conclusion
The shoulder is one of the most vulnerable joints of the human body for dislocations and is usually associated with rotator cuff tears among elderly people. The management of the rotator cuff tears in primary traumatic shoulder dislocation can prevent further shoulder instability events. Prompt assessment by an orthopedic specialist and Imaging, MRI or CT Scan help in diagnosis of tears and ensure a personalized recovery plan. Early rehab and adherence to prevention strategies significantly reduce the risk of recurrent dislocations, allowing athletes to return to their normal activities.
References
- (2023) Dislocated shoulder.
- (2022) Dislocated-shoulder/symptoms-causes.
- (2020) Surgical management of complex shoulder injuries. Indian Orthopaedic Association.
- (2024) Shoulder-dislocation treatment in Delhi.
- Renaldi P, Hans KH, Wendy YR, Adrian FI, Petrasama, et al. (2022) Primary traumatic shoulder dislocation associated with rotator cuff tears in the elderly. International Journal of Surgery Case Reports 95(1): 107200.
- Natalie KK, Jamie EC, Brian F, Michael RD (2025) Evaluation & management of rotator cuff tears following shoulder dislocation. Curr Rev Musculoskelet Med 18(9): 323-330.
- Thomas T, John A (2001) Concurrent anterior shoulder dislocation & rotator cuff tear in a young athlete. Iowa Orthop J 21: 76-79.
- (2015) Rotator-cuff-tear-injection.
- Alabd M (2024) Hill-sachs lesion with bony bankart lesion. Radiopaedia.
- Sanjay M, Pramod S, Vivek S, Ramakant K, Vivek T (2013) Bilateral anterior shoulder dislocation. Nat Sci Biol Med 4(2): 499-501.
- (2015) An evidence-based assessment & management of rotator cuff injury case. Physiopedia.
© 2026 Suresh Kishanrao. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






