- Submissions

Full Text
Orthopedic Research Online Journal
Hand Blast Injuries During a Mass-Casualty Incident: Patterns, Acute Management Strategy, and Lessons learned from the 2024 Lebanon Pagers Explosion
Jad Zalaket1, Andrea Achkouty1, Sami Kais1, Marven Aoun1, Toni Mansour1,2, Sami Roukoz1,2 and Rami El Abiad1,2*
1Department of Orthopedic Surgery, Hotel Dieu de France Hospital, Lebanon
2Saint Joseph University, Faculty of medicine, Lebanon
*Corresponding author:Rami El Abiad, Department of Orthopedic Surgery, Hotel Dieu de France Hospital, Beirut, Lebanon
Submission: April 10, 2026;Published: April 21, 2026

ISSN: 2576-8875 Volume12 Issue 1
Abstract
Introduction: On September 17, 2024, a coordinated detonation of hundreds of pagers across multiple regions in Lebanon caused a devastating mass-casualty incident with high concentration of complex hand injuries. This study aims to describe the musculoskeletal injuries, outline the acute response management protocol in a resource-challenged setting and identify lessons to improve future disaster preparedness.
Methods: This retrospective case-series was conducted including all patients admitted to our hospital suffering from musculoskeletal injuries directly related to the incident. Demographic characteristics, injury patterns, operative management, missed diagnoses, and need for secondary intervention were recorded. Associated injuries with other systems were also analyzed.
Results: A total of 45 patients [43 males] were included. Age ranged from 4 to 59 years (mean of 34 +/- 9.7 years). Hand trauma was the most frequent injury, affecting 42 out of 45 patients, with 25 cases involving bilateral damage, Totaling 67 injured hands. Additional musculoskeletal injuries included 10 lower-limb deep lacerations, 2 iliac bones fractures and 3 forearm penetrating wounds. Concomitant injuries were common, particularly ocular trauma in 38 patients. Initial surgery focused on debridement, fracture stabilization, foreign body removal and soft-tissue coverage. K wires were applied in 10 hands. Postoperative radiographs identified 15 missed injuries, of which six required revision surgery.
Conclusion: This incident was a significant and unique challenge for healthcare workers, particularly in the field of orthopedic surgery. Rapid triage, early debridement, prioritization of thumb and digit preservation and parallel multi-team workflow proved effective in managing the surge of patients. Lessons learned from such events highlight the need for disaster protocols in order to improve preparedness and optimize patient care in future mass-casualty encounters.
Keywords: Mass-casualty incident; Mangled hands; Digit amputation; Polytrauma
Introduction
On the 17th of September 2024, a synchronous detonation of numerous pagers occurred across several regions in Lebanon, resulting in a Mass-Casualty Incident (MCI) with over 2800 wounded and 9 fatalities [1]. A Mass-Casualty incident is characterized by an overwhelming influx of patients towards healthcare centers and hospitals demanding substantial resources and personnel [2]. Hotel-Dieu de France (HDF), a university hospital in Beirut, admitted approximately 70 patients, Most presenting severe hand and eye injuries. An effective management plan was quickly implemented, leveraging HDF’s experience from the Beirut port blast on August 4, 2020, during which the hospital treated over 700 injuries [3,4]. Fortunately, life-threatening injuries were minimal, but a significant number of patients sustained mangled hands and ocular globe injuries. A mangled hand injury is a severe and complex injury characterized by multi-tissue involvement including communitive open fractures, extensive soft tissue damage, and neurovascular compromise. Such injuries predominantly arise from high-energy trauma (e.g., blasts or fireworks) in young populations [5] and can profoundly impact patient’s quality of life and their future prospects [6,7]. This study aims to describe the hand and other Musculo skeletal injuries patterns managed by the orthopedic department at HDF hospital, to outline the acute response protocol adopted under crisis conditions and identify lessons for future disaster preparedness.
Material and Methods
Study design and ethical approval
A retrospective case-series was conducted. Institutional review board approval was obtained (IRB #CEHDF 2517).
Patient selection
All patients admitted to Emergency Rooms (ER) of HDF hospital with musculoskeletal injuries directly caused by the pager explosions were included. Those with superficial wounds treated and discharged from the emergency department were excluded from the cohort.
Data collection
Demographic data, including age and gender, were collected. Specific factors related to musculoskeletal injuries such as hand dominance, unilateral or bilateral involvement, injury severity, characteristics patterns of hand injuries, number of affected digits, fractures, foreign bodies, use of K wires, missed injuries and secondary surgeries were recorded.
Data collection additionally encompassed other associated injuries including penetrating eye injuries, ears-drum perforation, brain contusion or intracranial hemorrhage, face fractures and lower limbs involvement (Table 1).
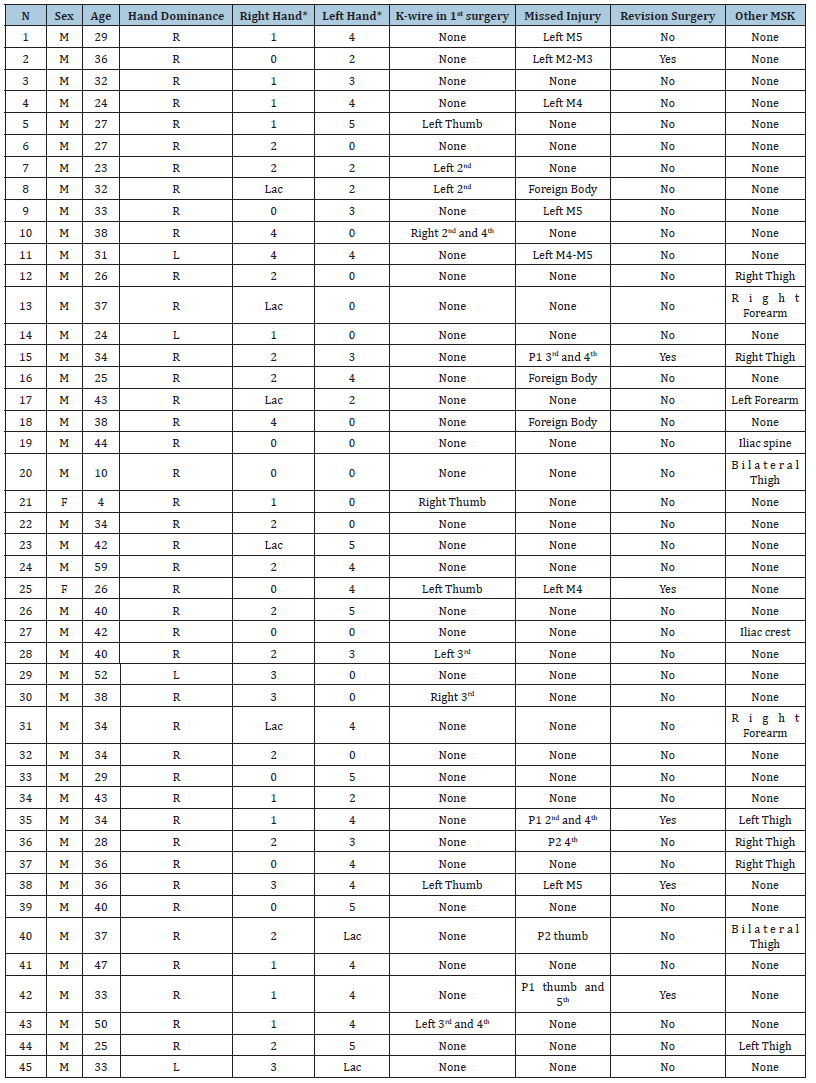
Table 1:Descriptive Table of Musculoskeletal injuries. (*) Number of affected digits, Lac (Lacerations), M(metacarpal), P1(proximal Phalange), P2(middle Phalange).
Acute response protocol
A disaster plan was activated upon the arrival of the first patient in the ER at 3:40PM. A junior orthopedic resident was responsible for patient triage in the ER, along with a group of general surgery residents. Upon admission, all patients received analgesics, tetanus antitoxin injection and intravenous antibiotics (Amoxicillin/Clavulanic acid 1.2g) after confirmation of no known allergies. Alternatively, Clindamycin 600mg was administered, with doses adjusted for patients under 18 years old. Dressings were applied following copious irrigation with normal saline. Rings were removed using a ring cutter and a tourniquet was applied if active bleeding was present.
Internal communications were facilitated via hospital’s platform providing all the active orthopedic surgeons and residents with handover notes, including images of musculoskeletal and associated injuries (eyes, face, thigh, and abdominal wall) to aid in the triage process. Most patients presented severe hand injuries with signs of burns and multiple foreign bodies embedded in the soft tissues.
Following initial evaluation, patients with moderate and minor injuries were transferred to regular floor rooms in the orthopedic surgery department to clear more space in the ER for other incoming patients. Unstable patients were intubated in the ER by the resuscitation team and immediately transferred to the Operating Rooms (OR) or the Intensive Care Unit (ICU). All other patients underwent surgery overnight, prioritizing those with bilateral and unilateral eye injuries associated with hand injuries, followed by those with isolated hand or limb injuries within the subsequent 24 hours.
The OR operated at full capacity (10 rooms) with simultaneous operations performed by orthopedic, ophthalmology and plastic surgery teams to expedite the process. A single dose of Gentamicin 180mg IV was administered in the OR for patients over 18 years old with severe mangled hand injuries. Amoxicillin/Clavulanic acid (1.2g IV q 8 hours) was continued for 24 hours postoperatively, followed by an oral regimen with adjusted doses for children, for a total period of five days [8].
From an orthopedic perspective, debridement of the hand injuries prioritized thumb preservation [9]. Mangled fingers underwent amputation, foreign bodies were thoroughly removed, and tension free closure of the wounds was performed whenever possible.
Pedicled local skin flaps were used to cover soft tissue defects (Figure 1). Well vascularized fingers with unstable fractures were fixed using Kirschner wires (K-wires). In some cases, interphalangeal or metacarpo-phalangeal fusion was performed by resecting the smashed articular cartilaginous surface prior to reduction and fixation. Dressings included fusidic acid, sterile paraffin tulle gras, and gauze. The next dressing change was scheduled 24 to 48 hours later.
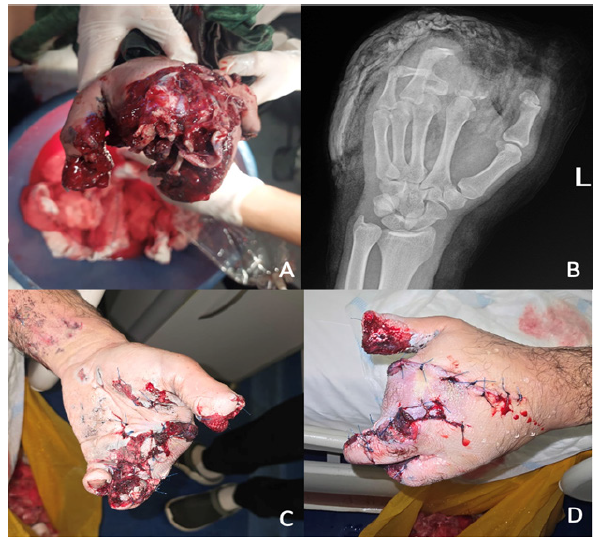
Figure 1:Patient who had a local skin flap to cover the defect. A: Preoperative status. B, C, D: Post operative result.
Postoperative X-rays were conducted the following day enabling the triage of patients requiring further revision surgeries, mainly for missed metacarpal fractures, as we haven’t done either preoperative or intra operative X-rays.
Results and Statistical Analysis
A total of 45 patients (43 males and 2 females) with musculoskeletal injuries were included in this study. Patient age ranged from 4 to 59 years with a mean of 34 +/- 9.7 years. Among the 45 individuals, 41 were right-hand dominant and 4 were lefthand dominant.
The most common musculoskeletal trauma was hand injury with 42 out of 45 patients, with 25 cases involving bilateral hand injuries, accounting for a total of 67 injured hands. Other musculoskeletal injuries included 10 deep lower limb wounds, 2 iliac fractures and 3 forearm penetrating wounds, one of which causes an ulnar nerve palsy.
Concomitant injuries were common, with ocular trauma being the most prevalent, affecting 28 patients bilaterally and 10 unilaterally. Additionally, 13 patients sustained facial bones fractures and 8 had ear-drum perforations. The facial fractures were minor and did not require surgical intervention after assessment by maxillofacial surgeons; and ear-drum perforations were managed with topical antibiotics. Lastly, 10 patients were unstable at presentation and required intubation in the ER.
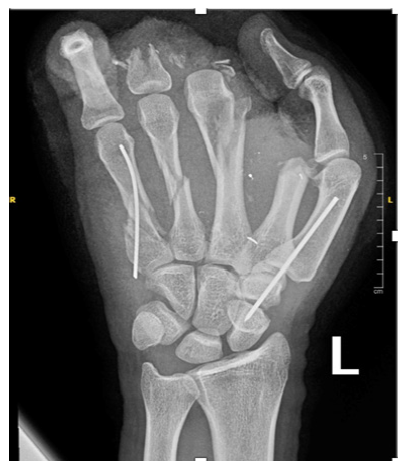
Regarding orthopedic surgical management, K-wires were initially used in 10 hands. Post operative X-Rays revealed 15 previously missed injuries (comprising 7 metacarpal fractures, 5 phalangeal fractures and 3 missed metallic foreign bodies). Of these 6 patients underwent secondary surgeries the following day, primarily for intramedullary pinning in case of metacarpal fractures (Figure 2), or standard pinning for phalangeal fractures while foreign bodies were removed at the bedside under local anesthesia.
Figure 2:Patient who presented with a severe injury and required revision surgery. A, B: Clinical status upon arrival. C, D, E: Post debridement and partial amputation. F: Post revision surgery the following day.
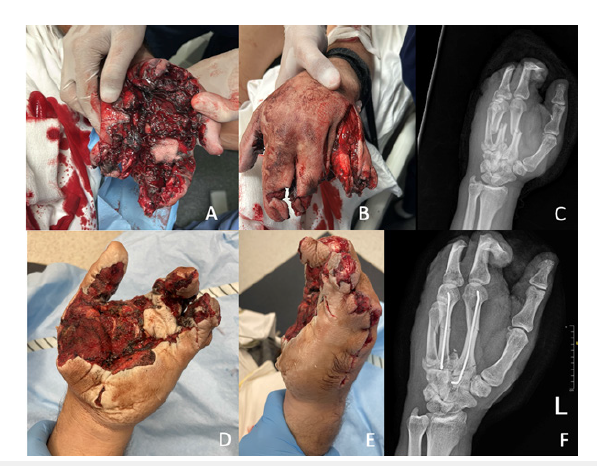
Figure 3:Preoperative and postoperative status of a patient who had a displaced iliac crest fracture.
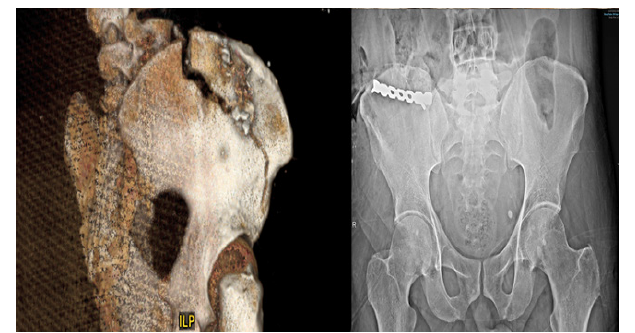
Out of 45 included patients, only 3 had intact eyes and hands. The first one had the device in his pocket which only caused a wound to the abdominal wall with avulsion fracture of the anterior superior iliac spine. The second one was driving when the pager exploded on his lap which caused a deep wound to the right thigh associated with an iliac crest fracture requiring open reduction and internal fixation (Figure 3). The last individual sustained bilateral lower limbs injuries from projectile small fragments due to his relative proximity to the explosion.
Discussion
The global prevalence of conflicts and wars is escalating worldwide, particularly in the Middle East, often overwhelming the medical facilities and leading to Mass-Casualty Incidents (MCI) [10]. Rapid and effective response is essential to managing injuries and providing optimal care for the wounded person. The pager incident in Lebanon represents an unprecedented global event, and to our knowledge this study is among the first one to describe the pattern and management of musculoskeletal injuries within such an MCI.
The synchronous nature of the explosions, triggered by a message sent to the pagers, accounts for the extensive eye and hand injuries observed. To date, there is no universally optimal management protocol for these type of hand injuries [11], especially when associated with extensive burns and penetrating foreign bodies. The orthopedic surgery team at our institution set a goal to preserve all viable digits and as many functional digits as possible with a high priority given to the thumb in addition to at least another finger for opposition (Figure 4). Indeed, in cases of mutilating long fingers trauma, a preserved thumb contributes to over 50% of overall hand function, as stated by Moran and Berger [9]. Furthermore, our objective was to achieve what Del Pinal described as an ‘acceptable hand’ which, in addition to a functioning thumb, comprises a hand with three fingers of near normal length with good PIP joint motion and good sensibility [12].
Figure 4:Example of a patient where effort was made to preserve at least a long digit in addition to the thumb for opposition.
Surgical treatment had to be performed within the first 24 hours to carry out a rapid surgical debridement and achieve good soft tissue coverage. Aggressive and prompt debridement is recommended in similar settings to reduce the risk of infections [13]. Consequently, pre or post debridement cultures weren’t routinely taken as they do not appear to be predictive of infections in combat related extremity injuries [13]. Moreover, due to the chaotic environment caused by a significant influx of patients, preoperative X-rays and intra operative fluoroscopies were not performed. This is attributed to various factors including understaffing, a limited number of portable X-ray machines, and the need for rapid patient turnover. Furthermore, it is worth noting that mangled hand X-rays would be difficult to interpret, and intra-operative fluoroscopies were difficult to perform due to the overcrowded operating rooms where multiple surgical teams were working simultaneously. Despite these limitations, our retrospective analysis showed that only 9% (6 out of 67 hands) required a secondary surgery due to missed displaced fractures, validating further our attitude.
Despite causing a mutilating injury to the hands and eyes, the pagers explosions in Lebanon didn’t account for a high number of deaths. In our emergency department, 11 patients were unstable due to brain contusions, intra-cranial hemorrhage, or extensive facial burns, and all of them recovered well by the end of the week without requiring any neurosurgical invasive intervention.
Finally, it is worth mentioning that none of the existing classifications in the literature could thoroughly describe the hand injuries observed in our cohort and guide their specific management [14,15]. The surgical treatment of complex cases was performed under the direct supervision of hand surgeons to optimize outcomes and preserve the maximum of the hand function. Consequently, our team is working on developing a specific classification or a scoring system, based on this experience, to establish guidelines for the targeted management of mangled hand injuries.
This incident highlighted several critical and important lessons that can improve future responses to similar disastrous events.
Firstly, we noticed a shortage in sterilized surgical kits and drills by midnight, attributed to the use of multiple kits per patient (multiple teams and a variety of needed instruments) in addition to the slow sterilization process. We, therefore, suggest the establishment of multidisciplinary surgical boxes containing essential tools to be used by multiple teams for this kind of emergencies, as well as increasing the number of drills in our stock. Secondly, we believe that the preop or intra operative X-Rays would not have significantly changed our attitude since preoperative imaging would have delayed surgery and overwhelmed the radiology department which was focused on conducting cerebral and abdominal CT scans for unstable patients. On the other hand, intra operative x-rays were difficult to perform as stated due to the overcrowding of the operating rooms. Thirdly, we suggest that, in similar settings, medical and paramedical teams should be organized into shifts, as we observed fatigue and decreased efficiency after 8 to 10 hours of intense effort following a regular workday. Lastly, this event underscored the importance of continuous training and drills for healthcare professionals to maintain readiness for any mass casualty.
Limitations
This study, however, has several limitations. The most significant being the lack of long-term follow-up to assess eventual complications, mainly the infection, nonunion and wound dehiscence rate and functional results. In fact, many patients were lost to follow-up after initial management, making it hard to assess postoperative complication rate and outcomes. Moreover, without extended monitoring it would be impossible to evaluate the long-term impact of a mangled hand on the patient’s quality of life along with the effectiveness of management strategies. Finally, the reliance on data from a single institution account for another limitation of this study, as it restricts the possibility to compare acute responses, surgical treatments, and eventual outcomes with other centers.
Conclusion
In conclusion, despite all the challenges, the medical staff in our institution effectively managed the massive inflow of patients from the pager explosions, mainly owing this to previous disaster experiences in Lebanon. This event also highlighted some flaws that may require improvements. Mass casualty incidents are a significant and unique challenge for healthcare workers particularly in the field of orthopedic surgery. It is crucial to learn from these experiences to strengthen the response and deliver optimal patient management.
References
- CNN (2024) Lebanon pager attack explosions: what we know so far.
- Harper K, Rehman S (2016) Orthopedic disaster management in the 2015 Amtrak derailment. J Trauma Acute Care Surg 80: 1032-1038.
- Daher M, Ghoul A, Salameh BL, Youssef B, Sabbagh J, et al. (2023) Management of the 4th of August explosion in an orthopedics department. Egypt Orthop J 58(2): 83-88.
- Kerbage A, Haddad SF, Zoghbi M, Souaid T, Haroun E, et al. (2021) Beirut blast 2020: cries and bloodshed at the busiest hospital. Disaster Med Public Health Prep 17: e80.
- Tintle SM, Baechler MF, Nanos GP, Forsberg JA, Potter BK (2010) Traumatic and trauma-related amputations: part II: upper extremity and future directions. J Bone Joint Surg Am 92: 2934-2945.
- Gustafsson M, Amilon A, Ahlström G (2003) Trauma-related distress and mood disorders in the early stage of an acute traumatic hand injury. J Hand Surg Br 28: 332-338.
- Meyer TM (2003) Psychological aspects of mutilating hand injuries. Hand Clin 19: 41-49.
- Redfern J, Wasilko SM, Groth ME, McMillian WD, Bartlett CS (2016) Surgical site infections in patients with type III open fractures: comparing antibiotic prophylaxis with cefazolin plus gentamicin versus piperacillin/tazobactam. J Orthop Trauma 30: 415-419.
- Moran SL, Berger RA (2003) Biomechanics and hand trauma: what you need. Hand Clin 19: 17-31.
- Al-Hajj S, Ghamlouche L, Nasser AlDeen K, El Sayed M (2023) Beirut blast: the experiences of acute care hospitals. Disaster Med Public Health Prep 17: e318.
- Agarwal R, Agarwal D, Agarwal M (2019) Approach to mutilating hand injuries. J Clin Orthop Trauma 10(5): 849-852.
- del Piñal F (2007) Severe mutilating injuries to the hand: guidelines for organizing the chaos. J Plast Reconstr Aesthet Surg 60: 816-827.
- Murray CK, Hsu JR, Solomkin JS, Keeling JJ, Andersen RC, et al. (2008) Prevention and management of infections associated with combat-related extremity injuries. J Trauma 64(Suppl 3): S239-S251.
- Abdo EM, Farouk N, Elimam SE, Elshinawy WE, Abdelhafez AA, et al. (2023) Mangled extremity severity score in the assessment of extremity injuries: is it reliable? Vasc Endovascular Surg 57: 445-450.
- Sharma A, Sankhe M (2022) A proposed classification for sugarcane crusher injuries of the hand and its correlation with patient-rated outcome scores at 6 months. J Hand Surg Asian Pac 27: 267-275.
© 2026 Rami El Abiad*. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






