- Submissions

Full Text
Modern Research in Dentistry
Odontogenic Keratocyst: Accidental Findings And Imaging Features Of A Benign Lesion With An Aggressive Behaviour - Treatment And Follow-Up Done At Tertiary Center In Kathmandu
Bikash Desar1* and Rajani Shakya2
1Chief of Department of Oral and Maxillofacial Surgery, Patan Academy of Health Sciences- Dental Department, Lagankhel, Nepal
2Registrar Community Medicine Dhulikhel Hospital, Kathmandu University, Nepal
*Corresponding author: Bikash Desar, Assistant Professor, Chief of Department of Oral and Maxillofacial Surgery, Patan Academy of Health Sciences - Dental Department, Nepal
Submission: November 25, 2025;Published: April 06, 2026

ISSN:2637-7764Volume8 Issue5
Abstract
Introduction: The 4th edition of the World Health Organization (WHO) classification of head and neck tumors, released in January 2017, re-designated the keratocystic odontogenic tumor as the Odontogenic Kerato-Cyst (OKC). The subsequent 5th edition published in 2022 maintains essentially the same conceptual framework for odontogenic lesions. OKCs are now regarded as benign odontogenic cysts and represent approximately 10% of all odontogenic cysts. They originate from remnants of the dental lamina and are characterised by a cystic cavity containing desquamated keratin, lined by a thin, parakeratinised squamous epithelium. OKCs can occur across a wide age range but most frequently present in the third decade of life, with a slight predominance in males. Although they may arise in any tooth-bearing area, the mandible is affected more often than the maxilla, particularly the posterior body, angle and ramus. In our series, a few cases involved the anterior mandible and were detected incidentally on panoramic radiographs. Subsequent CBCT imaging clarified the extent of cortical involvement and internal architecture. In contrast, maxillary OKCs most frequently originate in the anterior region and third molar area. OKCs are notable for their locally aggressive behavior and relatively high recurrence rate, especially in syndromic cases. Multiple OKCs are a hallmark feature of Nevoid Basal Cell Carcinoma Syndrome (NBCCS), an autosomal dominant multisystem disorder. Radiological evaluation-particularly Computed Tomography (CT)-plays a central role in the diagnosis, characterization and management of OKCs. This pictorial review aims to illustrate the imaging characteristics of OKCs across different modalities and highlight key radiologic findings that aid in distinguishing them from other cystic and neoplastic odontogenic lesions.
Key points:a. Panoramic radiography is valuable for the initial evaluation of suspected OKCs.
b. CBCT is the preferred imaging modality for detailed assessment of OKCs.
c. The differential diagnosis should include ameloblastoma, dentigerous cysts and radicular
cysts.
d. The presence of multiple OKCs is a major diagnostic criterion for NBCCS.
Keywords:Odontogenic keratocysts; Panoramic radiography; Computed tomography; Magnetic resonance imaging; Basal cell nevus syndrome
Introduction
Odontogenic Kerato-Cysts (OKCs), first described by Philipsen in 1956 [1], are benign intraosseous cystic lesions of odontogenic origin that account for roughly 10% of jaw cysts. They display locally aggressive behavior and are associated with a relatively high recurrence rate [2]. Histologically, OKCs arise from the dental lamina and consist of a keratin-filled cavity lined by a uniform parakeratinised squamous epithelium, typically 5-10 cell layers thick. The basal layer is composed of palisaded columnar or cuboidal cells with vertically oriented nuclei. The interface with adjacent connective tissue is usually flat, although budding of the basal layer and formation of satellite cysts may occur [3]. Mitotic activity is generally higher than that of other odontogenic cysts [4]. In the 3rd edition of the WHO classification of head and neck tumors, these characteristics-combined with their aggressive behavior and frequent association with mutations or inactivation of the tumor suppressor PTCH gene-led to their classification as Kerato-Cystic Odontogenic Tumors (KCOTs) [5]. However, in the 4th edition published in 2017 [6], the consensus panel concluded that current evidence does not sufficiently support a neoplastic nature for this lesion and further investigation is required [7]. Accordingly, the term “odontogenic keratocyte” was reinstated, replacing KCOT.
Accurate preoperative imaging is crucial for treatment planning, as OKCs often require more aggressive management than other radiolucent jaw lesions with similar imaging appearances. The purpose of this pictorial review is to describe the imaging presentation of OKCs, emphasizing characteristic findings across modalities and highlighting features that help differentiate them from other odontogenic cysts and tumors.
a. Panoramic radiography is helpful in the preliminary
assessment of OKCs.
b. CBCT is considered the tool of choice in the evaluation of
OKCs.
c. Ameloblastoma, dentigerous and radicular cysts should be
considered in the differential diagnosis.
d. The presence of multiple OKCs is one of the major criteria
for the diagnosis of NBCCS.
Incidence, Clinical Presentation and Natural History
Odontogenic Kerato-Cysts (OKCs) account for roughly 10% of all odontogenic cysts. They may occur across a broad age range-from approximately 8 to 82 years-with the highest incidence observed during the third decade of life [3,8,9]. Most epidemiological studies report a slight male predominance [10]. Multiple OKCs, which may arise synchronously or metachronous throughout a patient’s lifetime, are strongly associated with Nevoid Basal Cell Carcinoma Syndrome (NBCCS), also known as Gorlin-Goltz syndrome. This autosomal dominant multisystem disorder is linked to a younger mean age of presentation, typically around 25 years [11-13]. In line with other odontogenic lesions, OKCs develop in tooth-bearing areas. They occur approximately twice as often in the mandible as in the maxilla [14]. Within the mandible, they most frequently involve the posterior body, angle and ramus [15,16]. In contrast, maxillary OKCs most commonly arise in the anterior sextant-particularly between the canine and lateral incisor-or in the third molar region [17,18]. Larger lesions are especially common at the mandibular angle and ramus [19]. OKCs may present in periapical, pericoronal or lateral root positions, although around 30% demonstrate no association with adjacent teeth [10,17]. Despite their aggressive biological behavior, OKCs often cause minimal buccolingual expansion because they tend to extend along the cancellous bone spaces, effectively “growing in the length of the bone” [20]. Even extensive lesions capable of significant cortical erosion or involvement of neighboring structures may remain asymptomatic [21]. For this reason, particularly in Western populations, OKCs are frequently detected incidentally during routine imaging.
A 2011 systematic review by Mac Donald-Jankowski noted differences in symptomatology among populations: Patients of East Asian origin often present earlier with swelling and pain, while Latin American patients more commonly report discharge or inferior alveolar nerve paranesthesia [22]. Unlike Amel blastomas and other aggressive odontogenic lesions, OKCs only rarely produce resorption of adjacent tooth roots [10]. Reported postsurgical recurrence rates vary widely, reaching up to 30%, with the highest rates observed following conservative treatments such as simple enucleation [2,19]. Recurrence is more frequent in NBCCSassociated cases and in multilocular lesions. Several mechanisms have been proposed, including incomplete removal of the active basal epithelial layer, persistence or regrowth of small satellite cysts and the development of new lesions in adjacent jaw regions [13,19]. Surgical approach alone may not fully explain recurrence, and some authors suggest a role for inherent biological factors such as elevated expression of proliferative markers like Ki-67.
Imaging techniques
The primary imaging methods used to evaluate Odontogenic Kerato-Cysts (OKCs) include conventional radiography-particularly panoramic radiographs-along with Computed Tomography (CT) and Magnetic Resonance Imaging (MRI). Each modality offers distinct technical features, acquisition protocols and diagnostic capabilities, providing complementary information that supports accurate assessment and management of these lesions.
Panoramic radiography
Panoramic radiography provides a two-dimensional depiction of the curved maxillary and mandibular dental arches and serves as a valuable initial tool for evaluating odontogenic lesions, including OKCs. It assists in assessing lesion location, size, morphology, margins and overall extent. However, its diagnostic capability is limited by inherent drawbacks such as magnification, geometric distortion and superimposition of anatomical structures. Consequently, three-dimensional imaging is often requiredparticularly for larger lesions-to obtain more accurate preoperative information. On panoramic images, OKCs typically present as welldefined unilocular or multilocular radiolucent lesions bordered by a corticated rim (Figure 1). The unilocular pattern is more frequently observed, whereas multilocular lesions occur in roughly 30% of cases and are more common in the mandible [9]. In mandibular unilocular OKCs, a few thin or incomplete internal septa may be visible, a feature more commonly associated with larger lesions.
Figure 1:
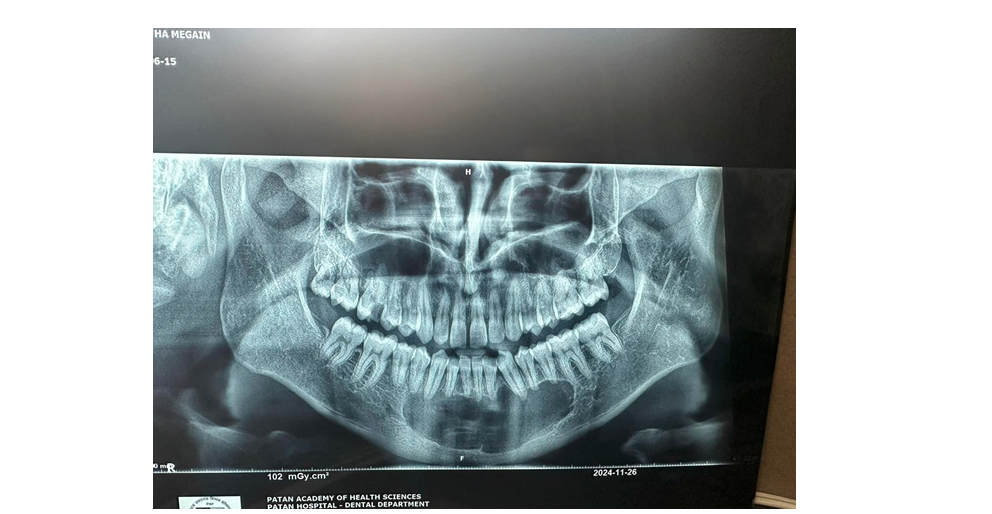
Mandibular odontogenic kerato-cysts (Okc’s)
a. Cropped panoramic radiograph illustrating a unilocular
lesion in the posterior mandible and ramus, causing mesial
displacement of the impacted third molar (curved arrow).
b. Cropped panoramic radiograph showing a multilocular
lesion involving the posterior mandible and ramus, exhibiting
a characteristic soap-bubble appearance.
A cropped panoramic radiograph reveals a large OKC with well-defined, lobulated borders (arrowheads) occupying the mandibular body. An incomplete internal septum is also visible within the lesion (opposing arrows). Approximately 30% of OKCs are associated with at least one unerupted tooth-most commonly the third molars [9]. This association is observed more frequently in younger patients [15]. The radiographic characteristics of OKCs are not pathognomonic, especially in small unilocular lesions [15]. When a small unilocular OKC appears in the anterior maxillary sextant, it may mimic other odontogenic or non-odontogenic cysts, such as radicular cysts (Figure 1), lateral periodontal cysts or nasopalatine duct cysts [17]. Histologically confirmed OKCs. Cropped panoramic radiographs (a and b) demonstrate two unilocular radiolucent lesions (asterisks) with well-defined, corticated borders (arrowheads) located in the anterior maxilla between the roots of adjacent teeth. The radiographic appearance of these radiolucencies may mimic a radicular cyst. Large mandibular OKCs characteristically grow along the length of the mandible, showing minimal Bucco-lingual expansion, particularly within the mandibular body [15]. On panoramic radiography, this growth pattern typically presents as an extensive radiolucent lesion with significant mesiodistal extension and little or no cortical expansion (Figure 1 & 2). In contrast, large maxillary OKCs often produce marked expansion of the alveolar bone and may involve adjacent anatomical structures. Notably, when a maxillary OKC originates in the molar region, extension into the maxillary sinus is commonly observed (Figure 2) [22].
Figure 2:
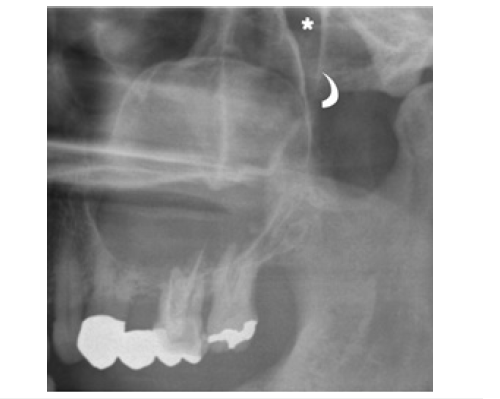
A cropped panoramic radiograph of the posterior left maxilla shows a large OKC extending into the maxillary sinus (arrows). The posterior wall of the maxillary sinus (curved arrow) and the pterygopalatine fossa (asterisk) are also visible. Radiographically, OKCs may cause tooth displacement and, less commonly, root resorption. Root resorption is considered an uncommon feature, with reported incidences ranging from 1.3% to 11% [9]. The literature indicates that cortical bone perforation is not unusual in OKCs, with intraoperative reports ranging from 39% to 51% [9]. However, this feature is rarely detectable on panoramic radiography and when present, is generally confined to the alveolar crest.
Cone beam and multidetector computed tomography
In clinical practice, two CT techniques are primarily used to evaluate maxillofacial disorders: Cone Beam CT (CBCT) and Multi- Detector CT (MDCT). Both modalities are suitable for diagnosing OKCs and for preoperative planning, as they provide high-quality Multi-Planar Reconstruction (MPR) images in various planes. Using dedicated dental arch reconstruction software (Denta Scan), the three-dimensional datasets from either modality can be reformatted into panoramic and cross-sectional MPR images aligned with the curvature of the alveolar bones. These highresolution images offer three-dimensional visualization of the jaws and deliver detailed information about the OKC and its relationship to surrounding structures, including teeth, sinonasal cavities, canals, foramina and adjacent soft tissues. The major advantage of CBCT in evaluating maxillary and mandibular lesions is its superior spatial resolution compared with MDCT. However, CBCT has limited contrast resolution, making it unsuitable for differentiating soft tissues and preventing assessment of soft tissue extension or the use of contrast media. Consequently, CBCT is most effective for demonstrating bony alterations of the cortical plates (buccal, palatal or lingual), whereas MDCT is more effective for evaluating internal density and soft tissue involvement.
Figure 3:a) Panoramic radiograph • Shows a large radiolucent area in the maxilla. • The lesion has a well-defined, corticated rim, which typically indicates a slow-growing process. • The white arrows (in the original figure) point to the margins of the cystic lesion. b) Axial MDCT - bone window This view highlights bony structures. • Shows hydraulic (balloon-like) expansion of the maxillary alveolar bone. • Black arrows originally indicate the direction of this expansion. • Wavy arrows show thinning of the buccal cortical plate. • Curved arrows identify focal perforation of the buccal cortex.
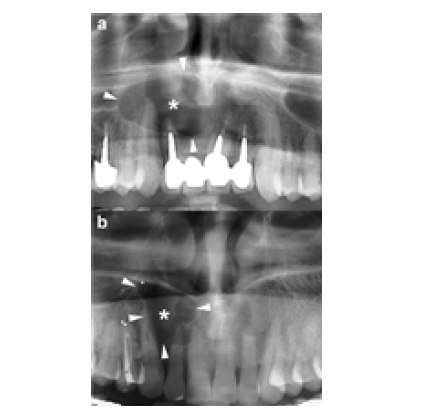
Similar to panoramic radiography, CT scan depicts the main radiological characteristics of OKCs, including size, shape (hydraulic or scalloped), margins (well-defined and corticated), internal configuration (uni- or multilocular) and effects on adjacent structures such as displacement of teeth, root resorption, elevation of the maxillary sinus floor or inferior displacement of the mandibular canal. Additionally, CT provides valuable information on other features of OKCs, including buccolingual or palatal expansion, cortical erosion, internal density and soft tissue extension (Figure 3a & 3b).
a. Panoramic radiograph
• Shows a large radiolucent area in the maxilla.
• The lesion has a well-defined, corticated rim, which
typically indicates a slow-growing process.
• The white arrows (in the original figure) point to the
margins of the cystic lesion.
b. Axial MDCT - bone window
This view highlights bony structures.
• Shows hydraulic (balloon-like) expansion of the maxillary
alveolar bone.
• Black arrows originally indicate the direction of this
expansion.
• Wavy arrows show thinning of the buccal cortical plate.
• Curved arrows identify focal perforation of the buccal
cortex.
These features are common with OKCs due to their tendency to grow anteroposteriorly and expand bone with minimal buccolingual widening-though expansion can still occur in maxillary lesions.
c. Axial MDCT - soft tissue window
Highlights soft tissue differences.
• Shows posterior bowing of the maxillary sinus floor, often
caused by mass effect from the lesion (arrowheads).
• Asterisks denote inflammatory contents within the left
maxillary sinus, which may occur secondarily from obstruction or
irritation caused by the lesion.
Therefore, CT is considered superior to conventional radiography for differentiating OKCs from other unilocular or multilocular osteolytic lesions and for providing essential information during preoperative assessment (Figure 4). In the mandible, OKCs typically exhibit mesiodistal growth along the length of the bone, resulting in minimal buccal or lingual cortical expansion. However, in some cases, OKCs may produce appreciable expansion and even erosion of the cortical plates (Figure 4).
Figure 4:
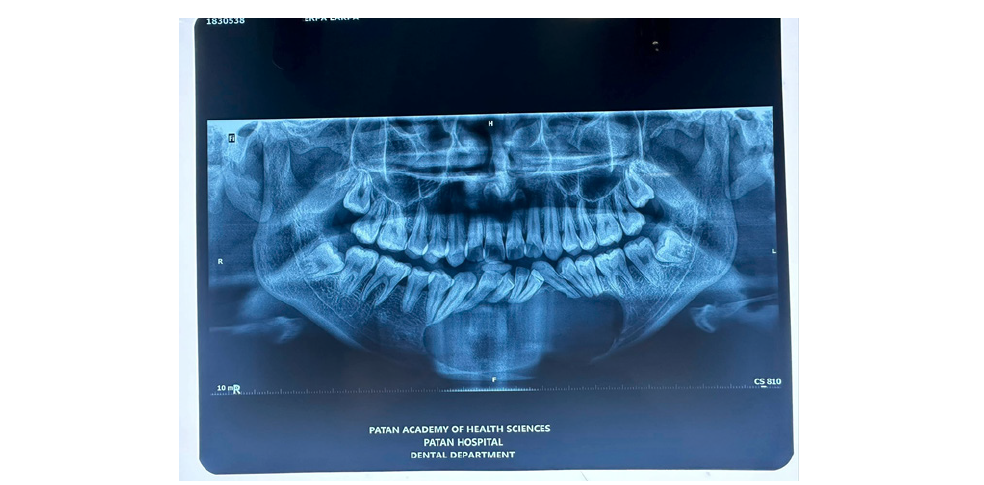
Mandibular OKC
Panoramic (a) and cross-sectional (b) Cone Beam Computed Tomography (CBCT) images show an osteolytic odontogenic lesion in the posterior left mandible and ramus, demonstrating growth primarily along the length of the bone (double-headed arrow) with only minimal expansion of the buccal and lingual cortical plates (curved arrows) (Figure 5a). Mesial displacement of the impacted third molar and inferior displacement of the mandibular canal (arrowheads and dots) are evident. A small, incomplete internal septum (small black arrows), reflecting endosteal scalloping of the cortical plate, is also visible. The wavy arrow indicates the mandibular foramen. Panoramic CBCT imaging with a 20-mm slice thickness (a) shows a mandibular OKC containing a septum (opposing arrows) that appears to divide the lesion into two major loculations. Displacement of adjacent teeth is evident (Figure 5b). However, panoramic (b) and axial (c) CBCT images reconstructed at 0.5-mm and 0.2-mm slice thicknesses, respectively, demonstrate that the septum is actually incomplete (arrows). Perforation of the buccal cortex in the anterior portion of the lesion is also visible (curved arrows).
Figure 5:
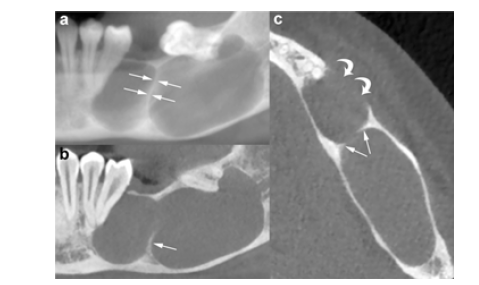
Figure 6:
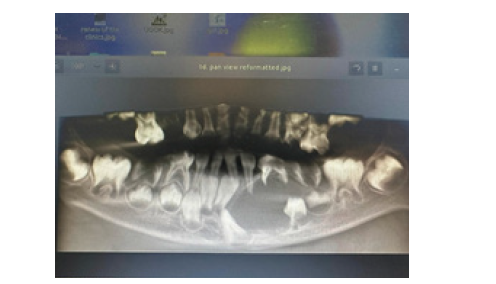
Figure 7:
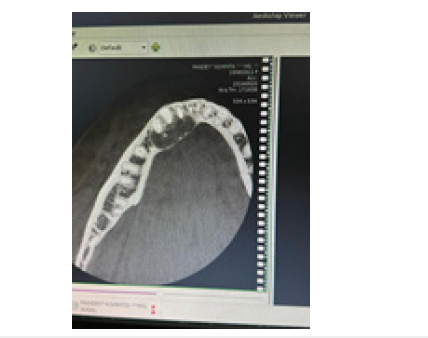
Panoramic (a) and cross-sectional (b) CBCT images show an OKC with well-defined, lobulated margins located in the interforaminal region of the mandible (asterisk). The lesion exhibits mesial growth, crossing the midline (white arrows). Root resorption is evident (arrowheads), along with perforation of the cortical plates (curved arrows). Scalloping of the endosteal surface of the cortices (small black arrows) and a small internal septum (wavy arrow) are also demonstrated (Figure 5c). Large black arrow indicates the left mental foramen; 33, left canine; 34, left first premolar; 35, left second premolar; 36, left first molar. In contrast, large OKCs in the maxilla more commonly exhibit a hydraulic expansion of the alveolar bone, characterized by remodeling, thinning, scalloping and perforation of the cortical plates. Additionally, when OKCs arise from the alveolar bone subjacent to the maxillary sinus, the sinus floor becomes elevated, and the sinus lumen is reduced (Figure 6). Panoramic CBCT images of a maxillary OKC (asterisks) originating from the molar region distally to the second molar tooth. The OKC causes significant sinus floor elevation (arrowheads). Curved arrows, posterior wall of the maxillary sinus; arrows, lateral pterygoid lamina (Figure 7). The difference between the growth pattern of mandibular and maxillary OKCs may be partly due to the higher cortical thickness of the mandible compared to that of the maxilla [15]. On CT images, OKCs typically manifest as osteolytic lesions that exhibit a unilocular or a predominantly unilocular morphology with few and incomplete septa. The multilocular presentation with adjacent satellite cysts (daughter cysts) is possible, particularly in large lesions. In these cases, loculations are usually large and few (soap-bubble appearance). Panoramic CBCT images with 20-mm (a) and 0.5-mm (b) slice thickness of an OKC demonstrate a unilocular lesion with well-defined, corticated margins located in the posterior sextant and ramus of the right mandible (arrows), adjacent to the distal root of the second molar (arrowheads). An interruption of the superior border of the retromolar region is visible (curved arrow), along with inferior displacement of the mandibular canal (opposing arrows and dots).
c Histological section shows the characteristic parakeratinised stratified squamous epithelial lining with a corrugated surface pattern (H&E, 10×). Panoramic CBCT imaging with a 20-mm slice thickness (a) reveals a multilocular OKC. On this reconstruction, septa appear to subdivide the lesion into multiple locules. Crosssectional CBCT images reconstructed at 0.5-mm thickness (b) demonstrate that several of these septa are complete (arrowheads), while others are incomplete (wavy arrows). Some of the small loculations observed on the panoramic reconstruction (black asterisk, white and black stars) actually represent a single, larger loculation with scalloped inner borders (Figure 8a). Compression and lingual displacement of the mandibular canal beneath the root of the third molar are also evident (opposing arrows). Curved arrow identifies the mandibular foramen; arrows indicate the mandibular canal. OKCs may be associated with an impacted tooth, a feature resembling that of a dentigerous cyst and observed more frequently in younger patients [14,15]. Internal highdensity foci are commonly present and correspond to keratinized material within the cystic cavity [14]. This characteristic internal appearance is more effectively demonstrated on MDCT because of its superior soft tissue contrast resolution compared with CBCT. Although uncommon, calcifications can occur within OKCs and are most often identified on histological evaluation (Figure 8b). On MDCT, OKCs typically show no appreciable enhancement following contrast administration.
Figure 8:Axial MDCT image with bone window (a) shows an OKC in the posterior region of the right mandible (asterisk). Axial MDCT image with soft tissue window (b) clearly demonstrates a high-density area within the lesion (elliptical ROI), with a mean attenuation value of 80 HU.
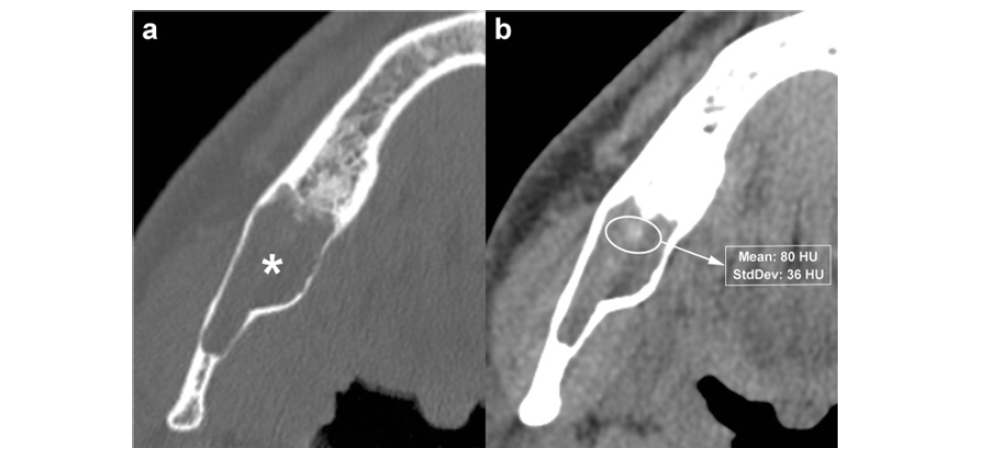
Panoramic (a) and axial (b) MDCT images depict an osteolytic lesion in the interforaminal region of the mandible, histologically confirmed as an OKC. The lesion causes expansion and thinning of the buccal cortex (arrowheads). Multiple punctate high-density foci consistent with calcifications are visible within the lesion (arrows), and one of these foci extends into the adjacent soft tissue (curved arrow). Dots indicate the mesial portion of the mandibular canal. (c) Histological images show the characteristic epithelial lining and calcifications (large black arrows) within the underlying connective tissue (H-E 10×).
Magnetic resonance imaging
MRI is primarily used as a complementary imaging modality to CT (either CBCT or MDCT) in the evaluation of cystic lesions of the jaws. In selected cases, it provides superior characterization of internal contents and soft tissue involvement (Figure 8a & 8b).
Unilocular OKC in the left maxillary tuberosity
a. Axial MDCT image with bone window demonstrates
remodeling and thinning of the adjacent cortical plates
(arrows).
b. Enhanced T1-weighted fat-saturated MRI sequence
shows a thin rim of peripheral enhancement surrounding the
lesion (arrowheads).
Axial MRI images illustrate the typical signal characteristics of
an OKC. The lesion, located in the posterior left mandible (arrows),
demonstrates:
a. Intermediate-to-high signal intensity on T1-weighted
imaging.
b. Heterogeneous high signal intensity on T2-weighted
imaging.
c. No internal enhancement on contrast-enhanced T1-
weighted fat-saturated sequence.
d. Restricted diffusion with high signal intensity on both b0
and b1000 images.
e. Corresponding low signal intensity on the Apparent
Diffusion Coefficient (ADC) map.
OKCs typically exhibit variable signal intensities on MRI, reflecting the nature of their internal contents. These lesions usually contain abundant keratin, sometimes accompanied by hyaline bodies when inflammation is present.
Several authors have reported that most OKCs demonstrate intermediate to high signal intensity on T1-weighted images and heterogeneous signal intensity-ranging from low to high-on T2- weighted images [20]. These MRI signal characteristics have been shown to aid in differentiating OKCs from ameloblastomas. In a retrospective study of 19 ameloblastomas and 14 OKCs, we compared the uniformity values of signal intensity within the cystic components of these lesions. Consistent with previous findings, the authors observed significant differences between the two lesion types across all MRI sequences. Specifically, both unicystic and multicystic ameloblastomas tend to exhibit more homogeneous internal signal, which appear low on T1-weighted images and high on T2-weighted images. Additionally, cystic ameloblastomas often feature a thick, irregular enhancing wall, sometimes accompanied by papillary projections or intralesional nodules.
In contrast, OKCs are characteristically associated with a thin, smooth rim of enhancement on contrast-enhanced T1-weighted images [10,16]. MRI with Diffusion-Weighted Imaging (DWI) and Apparent Diffusion Coefficient (ADC) mapping are sensitive to physiological characteristics such as tissue cellularity, the nucleusto- cytoplasm ratio and the integrity of cell membranes. These parameters allow MRI to provide insight into the microstructural composition of living tissues [18]. As an adjunct to conventional MRI sequences, DWI can aid in distinguishing OKCs from other odontogenic tumors that may present with similar imaging features. First demonstrated that OKCs typically exhibit significantly lower ADC values than cystic or predominantly cystic ameloblastomas. In a study by Srinivasan et al., the mean ADC value of OKCs was reported as 1.019 ± 0.07 × 10-3mm²/s, with an optimal cut-off point of 2.013 × 10-3mm²/s for differentiating them from predominantly cystic ameloblastomas. These results reflect the higher viscosity of OKC contents, attributed to the presence of desquamated keratin, whereas the cystic spaces of ameloblastomas generally contain mildly proteinaceous fluid, sometimes mixed with colloid material. Conversely, benign odontogenic cysts may show a broad range of ADC values due to varying degrees of inflammatory cell infiltration.
Sakamoto et al., in a retrospective analysis of 35 odontogenic cystic lesions, reported that Diffusion Kurtosis Imaging (DKI) may serve as a valuable quantitative technique for distinguishing OKCs from other cystic entities. DKI offers more detailed insight into the microstructural complexity of tissues, and the combined assessment of its parameters appears capable of differentiating between simple fluid viscosity and the restricted diffusion produced by suspended keratinous material. Consequently, DKI may enhance diagnostic accuracy in separating OKCs from other odontogenic cysts when compared with conventional ADC measurements. Radiological imaging-primarily CT (CBCT or MDCT) and, in selected circumstances, MRI-plays a key role in assessing Odontogenic Kerato-Cysts (OKCs). Nevertheless, especially in smaller lesions, OKCs may present radiographic features that closely resemble those of other osteolytic jaw pathologies. Therefore, a definitive diagnosis ultimately relies on histopathological evaluation [14]. From this perspective, imaging is generally more valuable for determining lesion extent and its relationship with adjacent structures than for establishing a specific diagnosis.
In some cases, however, the combination of clinical information
and imaging characteristics can help narrow the differential
diagnosis and may even support a correct provisional diagnosis of
OKC [18]. The imaging features most suggestive of an OKC include:
i. A well-circumscribed unilocular osteolytic lesion in the
posterior jaw region.
ii. A large mandibular osteolytic lesion with sparse
septations and limited buccolingual expansion.
Despite these clues, OKCs can resemble other odontogenic lesions depending on their presentation. When associated with an impacted tooth, they may mimic a dentigerous cyst (Figure 9a). Multilocular OKCs located in the posterior mandible or ramus can resemble an ameloblastoma, while those in a periapical position or an edentulous area may simulate a radicular cyst. Consequently, dentigerous cysts, ameloblastomas, and radicular cysts remain the most frequent entities considered in the differential diagnosis of OKCs.
Figure 9:
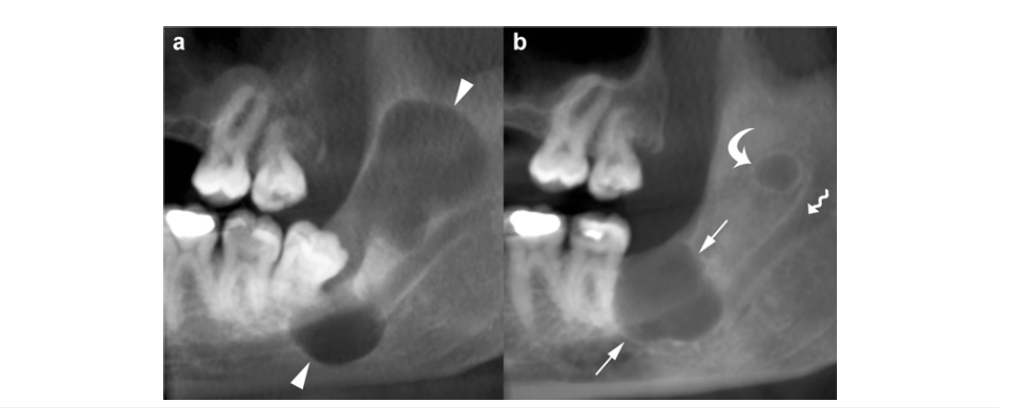
The imaging characteristics that more strongly indicate a
dentigerous cyst rather than an OKC include the following [14]:
i. An unilocular osteolytic lesion enveloping the crown of an
impacted tooth
ii. Absence of internal septa or loculations
iii. Greater buccolingual expansion in the mandible
iv. A more homogeneous and higher T2-weighted signal on
MRI
Conversely, the imaging features that are more suggestive of an
ameloblastoma rather than an OKC are [14]:
a. A multilocular osteolytic lesion containing multiple
internal septa
b. Marked buccolingual expansion in the mandible
c. More pronounced displacement of adjacent teeth and
root resorption
d. Post-contrast enhancement of internal septa or mural
nodules, which is more readily identified on MRI than on MDCT.
e. Mean ADC values greater than 2.013 × 10⁻³mm²/s on
diffusion-weighted imaging, a finding that favors ameloblastoma
over OKC.
Finally, the imaging characteristics that more strongly suggest a
radicular cyst rather than an OKC include [14,15]:
i. A round or pear-shaped unilocular radiolucency
ii. A lesion whose epicenter lies at the apex of a non-vital
tooth
iii. The presence of iron-like high-density material within the
cystic cavity, typically reflecting endodontic overfilling
The typical features of OKCs, dentigerous cysts, radicular cysts
and ameloblastomas are summarized in Table 1.
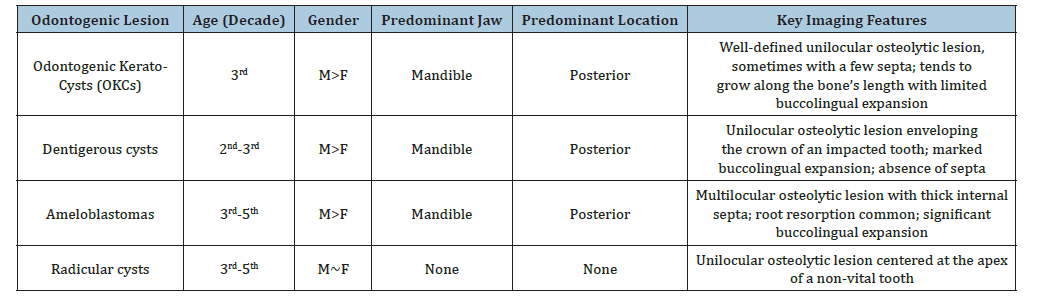
Table 1:Overview of typical characteristics of Odontogenic Kerato-Cysts (OKCs), dentigerous cysts, ameloblastomas and radicular cysts.
Syndromic and non-syndromic multiple OKCs
The presence of multiple Odontogenic Kerato-Cysts (OKCs) is considered one of the major diagnostic criteria for Nevoid Basal Cell Carcinoma Syndrome (NBCCS), and their appearance may represent the earliest manifestation of the condition. NBCCSalso known as Gorlin-Goltz syndrome-is an autosomal dominant multisystem disorder characterised by multiple nevoid basal cell carcinomas, numerous OKCs, palmar or plantar pits, calcification of the falx cerebri and various skeletal abnormalities, including bifid, fused, or splayed ribs. Additional features of NBCCS may involve craniofacial, neurological, sexual, ophthalmic and cardiac systems. The syndrome is associated with mutations in the PTCH tumor suppressor gene, and similar PTCH alterations have been identified in certain non-syndromic OKCs. Consequently, several authors propose that PTCH gene abnormalities play a key role in the pathogenesis of OKCs.
Multiple OKCs may also occur in other syndromes, such as Noonan syndrome, Ehlers-Danlos syndrome and oral-facial-digital syndrome. In syndromic cases, OKCs typically appear at an earlier age (first or second decade), tend to arise more frequently in the posterior maxillary regions (Figure 9a), exhibit more aggressive behavior, and demonstrate a higher recurrence rate compared with non-syndromic OKCs [18]. A panoramic CBCT slice (1mm thickness) demonstrates two unilocular OKCs in the right and left maxilla (asterisks) in a young male diagnosed with Nevoid Basal Cell Carcinoma Syndrome (NBCCS). Both cystic lesions arise in the posterior maxillary segments and extend into the Maxillary Sinuses (MS). Although uncommon, multiple OKCs may occasionally be found in patients without any identifiable systemic condition. Nevertheless, when multiple OKCs are present, a syndromic association should be strongly considered until excluded. Individuals with multiple OKCs require ongoing clinical followup to monitor for the potential development of other systemic manifestations.
Treatment and follow-up
Management of OKCs focuses on lowering the risk of recurrence while simultaneously limiting patient morbidity. Currently, no single therapeutic approach is universally accepted as the standard of care. The selection of the most suitable treatment depends on several factors, including the size and anatomical position of the cyst, whether it is unilocular or multilocular, the presence of cortical perforation or involvement of adjacent soft tissues, and the age of the patient (Figure 9b). A variety of surgical strategies have been described. These include simple enucleation or enucleation combined with adjunctive procedures such as peripheral ostectomy, application of Carnoy’s solution, or cryotherapy. Other options, such as marsupialization and decompression, may be used in selected cases. More aggressive techniques, including marginal or segmental resection, are reserved for extensive or recurrent lesions [19].
In a systematic literature review, Johnson et al. [13] reported that simple enucleation is associated with the highest recurrence rate, approximately 30%. Marsupialization alone shows a lower recurrence rate of around 18%. When enucleation is combined with an adjunctive technique such as chemical cauterization using Carnoy’s solution-a mixture of chloroform, absolute ethanol, glacial acetic acid and ferric chloride-the recurrence rate is significantly reduced to roughly 8% [22]. Although marginal and segmental resections demonstrate the lowest recurrence rates, their considerable morbidity makes them unsuitable as firstline treatments. These more aggressive surgical approaches are generally reserved for cases requiring retreatment, particularly in patients with multiple recurrent lesions [22]. The literature indicates that most recurrences of OKCs develop within the first 5-7 years following therapy [13]. In contrast, a study by Apajalahti et al. [19] reported a shorter average time to recurrence, approximately 2 years. This reduced interval likely reflects the routine use of CT during the follow-up of large OKCs (Figure 10a), which enables earlier detection of very small, clinically silent lesions.
Figure 10:Serial follow-up images of the same NBCCS patient shown in Figure. a) An axial CBCT scan reveals the development of a new lesion in the right mandibular third-molar region (arrows), which was subsequently removed surgically. b) A postoperative axial CBCT scan obtained one year later shows a very small recurrence at the previous surgical site (arrowheads).
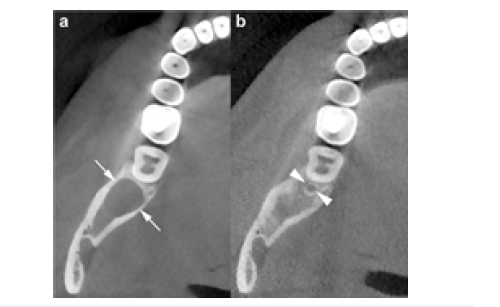
Panoramic CBCT images (20mm thickness) obtained at baseline (a) and at the first follow-up (b) illustrate the evolution of the lesion. At baseline (a), a large unilocular OKC is visible in the posterior mandible and ramus (arrowheads). At the first followup (b), performed two years after surgery, the CBCT scan reveals two recurrent lesions-one in the third molar region (arrows) and another within the mandibular ramus (curved arrow). The wavy arrow indicates the mandibular foramen. These findings highlight the importance of periodic radiographic surveillance following surgical management of OKCs. Annual imaging is recommended during the first five years after treatment, followed by examinations every two to three years thereafter. Patients diagnosed with NBCCS have an even higher propensity for developing new cysts, both at previous surgical sites and in other areas of the jaws (Figure 10b). Therefore, these individuals require a rigorous, long-term radiological follow-up protocol to enable early detection and appropriate management of new or recurrent lesions [22].
Conclusion
Odontogenic Kerato-Cysts (OKCs) are benign odontogenic lesions that represent roughly 10% of all odontogenic cysts and are notable for their locally aggressive behavior. Imaging-primarily Computed Tomography (CT) and, when indicated, Magnetic Resonance Imaging (MRI)-plays a key role in both diagnosing and managing these lesions. Although imaging alone may not always yield a definitive diagnosis, familiarity with the characteristic and variant radiological appearances of OKCs is fundamental for accurate assessment and appropriate treatment planning. In particular, correlating clinical findings with imaging features helps determine lesion extent and its effects on surrounding anatomical structures. Given the relatively high recurrence rate, especially following more conservative treatment approaches, regular radiographic surveillance is essential. Follow-up should be maintained for at least the first five years after surgery to ensure early detection of recurrent disease.
References
- Jordi BF, Alba ST, Javier AN, José-Manuel AU, Cosme GE, et al. (2020) Therapeutic management of the odontogenic keratocyst. An energetic approach with a conservative perspective and review of the current therapeutic options. J Clin Exp Dent 12(8): e794-e799.
- Santosh ABR (2020) Odontogenic cysts. Dent Clin North Am 64(1): 105-119.
- Borrás-Ferreres J, Sánchez-Torres A, Gay-Escoda C (2016) Malignant changes developing from odontogenic cysts: A systematic review. J Clin Exp Dent 8(5):
- Fidele NB, Yueyu Z, Tianfu W, Sun Y, Liu B, et al. (2019) Recurrence of odontogenic keratocysts and possible prognostic factors: Review of 455 patients. Med Oral Patol Oral Cir Bucal 24(4): e491-e501.
- Myoung H, Lee JI, Hong SP, Choi JY, Hong SD, et al. (2001) Odontogenic keratocyst: Review of 256 cases for recurrence and clinicopathologic parameters. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 91(3): 328-333.
- Rojas LV, Claudio CA, Huamán CJV, Rojas GV (2022) Diagnosis and conservative treatment of odontogenic keratocyst. Odontoestomatologia 24(39): 1-9.
- Vitali KP, Mello FW, Riet CER (2020) Comparative analysis between developmental and inflammatory odontogenic cysts: Retrospective study and literature review. Oral Maxillofac Surg 24(1): 73-84.
- Tarakji B, Salah H, Kusai B, Nazer AS, Zakaria NM (2013) Possible recurrence of keratocyst in nevoid basal cell carcinoma syndrome: A review of literature. Eur J Dent 7(Suppl 1): S126-S134.
- Winters R, Garip M, Coropciuc R, Meeus J, Politis C (2023) Safety and efficacy of adjunctive therapy in the treatment of odontogenic keratocyst: A systematic review. Br J Oral Maxillofac Surg 61(5): 331-336.
- Borghesi A, Nardi C, Giannitto C, Tironi A, Preda L, et al. (2018) Odontogenic keratocyst: Imaging features of a benign lesion with an aggressive behaviour. Insights Imaging 9(5): 883-897.
- Dias G, Marques T, Coelho P (2017) Treatment options for keratocyst odontogenic tumour (KCOT): A systematic review. Oral Surgery 10(4): 193-209.
- Mendes RA, João FCC, Isaac W (2010) Characterization and management of the keratocystic odontogenic tumor in relation to its histopathological and biological features. Oral Oncol 46(4): 219-225.
- Johnson NR, Martin DB, Neli WS (2013) Management and recurrence of keratocystic odontogenic tumor: A systematic review. Oral Surg Oral Med Oral Pathol Oral Radiol 116(4): E271-E276.
- Stoelinga PJW (2005) The treatment of odontogenic keratocysts by excision of the overlying, attached mucosa, enucleation and treatment of the bony defect with carnoy solution. J Oral Maxillofac Surg 63(11): 1662-1666.
- Cunha JF, Gomes CC, Alves MR, Eugênio MAG, Gomez RS, et al. (2016) Clinicopathologic features associated with recurrence of the odontogenic keratocyst: A cohort retrospective analysis. Oral Surg Oral Med Oral Pathol Oral Radiol 121(6): 629-635.
- Naruse T, Kentaro Y, Tohru I, Yuki S, Umeda M, et al. (2017) Histopathological and immunohistochemical study in keratocystic odontogenic tumors: Predictive factors of recurrence. Oncology Letters 13(5): 3487-3493.
- Noy D, Rachmiel A, Zar K, Emodi O, Nagler RM (2017) Sporadic versus syndromic keratocysts-can we predict treatment outcome? A review of 102 cysts. Oral Dis 23(8): 1058-1065.
- Blanas N, Freund B, Schwartz M, Furst IM (2009) Systematic review of the treatment and prognosis of the odontogenic keratocyst. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 90(5): 553-558.
- Apajalahti S, Hagström J, Lindqvist C, Anni S (2011) Computerized tomography findings and recurrence of keratocystic odontogenic tumor of the mandible and maxillofacial region in a series of 46 patients. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 111(3): e29-e37.
- Swinson B, Jerjes W, Thomas GJ (2005) Squamous cell carcinoma arising in a residual odontogenic cyst: Case report. J Oral Maxillofac Surg 63(8): 1231-1233.
- Waldron CA, Mustoe TA (1989) Primary interosseous carcinoma of the mandible with probable origin in an odontogenic cyst. Oral Surg Oral Med Oral Pathol 67(6): 716-724.
- Al-Moraissi EA, Kaur A, Gomez RS, Ellis E (2023) Effectiveness of different treatments for odontogenic keratocyst: a network meta-analysis. Int J Oral Maxillofac Surg 52(1): 32-43.
© 2026 Bikash Desar. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






