- Submissions

Full Text
Investigations in Gynecology Research & Womens Health
Immediate Postpartum Hemorrhage in an Arcuate Uterus: A Case Report of Asymmetric Uterine Atony
Amina El Alami¹*, Othmane Echarfaoui², Oumaima Fakir1, Aziz Slaoui1, Aziz Baidada1 and Jaouad Kouach²
1Gynaecology-Obstetrics and Endocrinology Department, Maternity Souissi, Ibn Sina University Hospital Center, Mohammed V University, Morocco
2Department of Gynecology-Obstetrics, Mohammed V Military University Hospital, Faculty of Medicine and Pharmacy, Mohammed V University, Morocco
*Corresponding author:Amina El Alami, Gynaecology-Obstetrics and Endocrinology Department, Maternity Souissi, Ibn Sina University Hospital Center, Mohammed V University, Rabat, Morocco
Submission:January 19, 2026;Published: March 09, 2026

ISSN: 2577-2015 Volume6 Issue1
Abstract
Background: An arcuate uterus is a minor congenital uterine anomaly that is often considered clinically insignificant. However, non‑uniform myometrial contractility may occasionally predispose to obstetric complications, including postpartum hemorrhage (PPH).
Case presentation: A 26‑year‑old primiparous woman had an arcuate uterus incidentally identified on fetal MRI. She delivered vaginally at 39+2 weeks. Immediately after placental delivery, she developed heavy bleeding (~1200mL) despite an apparently satisfactory uterine tone on abdominal palpation (uterine globe). Bedside ultrasound excluded retained products and suggested asymmetric fundal hypocontractility at the site of the fundal indentation. After initial medical management (uterine massage, uterotonics, tranexamic acid) and mechanical measures, bleeding persisted and she was transferred to the operating room. Uterus‑sparing surgery with stepwise uterine devascularization (Tsirulnikov ligatures) combined with a B‑Lynch compression suture achieved hemostasis.
Conclusion: A clinically “good” uterine globe can be misleading in PPH. When examination findings and bleeding are discordant, a structured 4Ts assessment and bedside ultrasound may expedite diagnosis of segmental/asymmetric atony and guide timely escalation to conservative interventions.
Keywords:Arcuate uterus; Postpartum hemorrhage; Uterine globe; Asymmetric uterine atony; Uterotonic agents; Bakri balloon; B-Lynch; Tsirulnikov; Bedside ultrasound
Abbreviations: ASRM: American Society for Reproductive Medicine; EBL: Estimated Blood Loss; ESGE: European Society for Gynaecological Endoscopy; ESHRE: European Society of Human Reproduction and Embryology; MRI: Magnetic Resonance Imaging; NB: Newborn; PROM: Prelabor Rupture of Membranes; GA: Gestational Age; HR: Heart Rate; PPH: Postpartum Hemorrhage; TXA: Tranexamic Acid; 4Ts: Tone, Trauma, Tissue, Thrombin
Introduction
Müllerian anomalies (congenital anomalies of the female genital tract) are classified by several systems, including the ASRM Müllerian Anomalies Classification 2021 (MAC2021) and the ESHRE/ESGE classification [1,2]. An arcuate uterus corresponds to a mild fundal indentation of the uterine cavity without a significant septum and is generally considered a minor anomaly/anatomic variant [1,3]. Available data suggest a possible increased risk of certain complications (malpresentation, preterm birth, cesarean delivery, and possibly postpartum hemorrhage), but findings remain heterogeneous depending on the definitions used [4,5]. Postpartum hemorrhage in an arcuate uterus is rarely described; a plausible pathophysiologic mechanism is non-uniform myometrial contractility leading to segmental/asymmetric uterine atony at placental delivery.
Case Presentation
Maternal characteristics
Ms B., 26 years old, primigravida (G1P0), with no notable gynecologic history, regular cycles, and a desired, well-followed pregnancy. The routine antenatal work-up was unremarkable.
Antenatal assessment
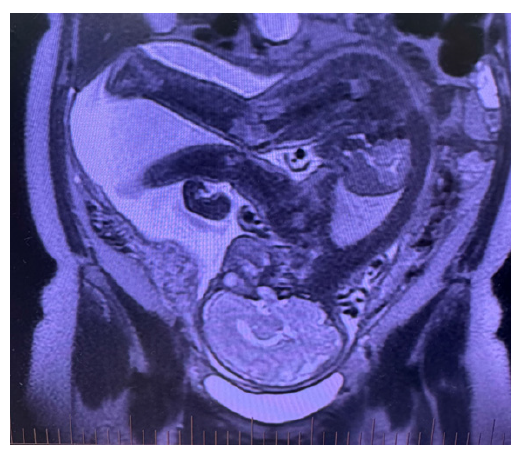
On the second-trimester anatomic ultrasound, suspected partial agenesis of the corpus callosum was raised, prompting fetal MRI at 28 weeks’ gestation. MRI found no fetal abnormality and revealed an arcuate uterus. Fetal biometry was appropriate for gestational age (~22nd percentile) (Figure 1).
Figure 1:A coronal T2-weighted Foetal MRI sequence of the pelvis showing an arcuate uterus.
Labor and delivery
At 37 weeks + 5 days’ gestation, the patient presented with prelabor rupture of membranes and early labor. Labor progressed uneventfully with timely cervical dilation and fetal descent. She delivered vaginally a eutrophic newborn with no immediate clinical abnormality.
Postpartum hemorrhage and clinical peculiarity
Immediately after placental delivery, postpartum hemorrhage occurred with an estimated blood loss of 1200mL; the patient remained hemodynamically stable (BP 112/75mmHg, HR 87bpm). The placenta was complete on inspection. A well-contracted uterine fundus (uterine globe) was palpated; despite this, bleeding persisted, emphasizing that satisfactory palpatory tone does not rule out postpartum hemorrhage and should not delay systematic etiologic evaluation [6-10].
Management and decision to proceed to the operating room
a) Immediate measures: Call for help, monitoring, two IV
lines, labs (CBC, coagulation) and blood preparation as needed
[6-10].
b) First-line maneuvers: Uterine massage±bimanual
compression, bladder emptying [6-10].
c) Etiologic approach using the 4Ts: Cervico-vaginal/
perineal inspection (Trauma), assessment for retained tissue
(Tissue), tone assessment (Tone), and coagulation testing
(Thrombin) [6-10].
d) Medical management per protocol: Uterotonics (first-line
oxytocin) plus early TXA administration [6,8,9,11].
e) Bedside ultrasound when examination is discordant
(uterine globe but persistent bleeding) to rule out retained
products of conception and guide escalation [12,13].
f) Mechanical measure: Intrauterine balloon tamponade
(Bakri-type) when available [8,10].
g) Ongoing bleeding despite these measures led to transfer
to the operating room for examination under anesthesia and
uterus-sparing hemostasis [6-10].
Uterus-sparing surgical hemostasis
After failure of initial measures, conservative surgery was
performed, combining:
a) Progressive uterine devascularization using Tsirulnikov
triple ligation [14,15].
b) B-Lynch uterine compression suture [16,17].
Hemostasis was achieved, avoiding hysterectomy. The postpartum course was uncomplicated.
Discussion
Types of uterine malformations and physiology of the arcuate uterus
The arcuate uterus is classified differently across systems (ASRM vs ESHRE/ESGE), which partly explains divergent findings in the literature [1,2]. Anatomically, it consists of a moderate fundal indentation without a significant septum [1,3]. In rare cases, nonuniform myometrial contractility may result in localized/segmental atony at placental delivery.
Complications of the arcuate uterus
Reported complications mainly include malpresentation, some dystocia, and adverse outcomes such as preterm birth or cesarean delivery, with results varying by study design and diagnostic criteria [4,5]. Postpartum hemorrhage appears possible but remains poorly documented and may relate to atypical uterine retraction dynamics.
Rapid management and special considerations
International and national guidelines emphasize immediate, structured, and stepwise management of postpartum hemorrhage with frequent reassessment [6-10]. The key message of this case is to avoid false reassurance from a firm uterine globe and to apply the 4Ts approach systematically.
Role of bedside ultrasound in the delivery room
With persistent bleeding or a discordant clinical exam, bedside pelvic ultrasound can help exclude retained products of conception, guide management, and accelerate therapeutic decisions [12,13].
Conclusion
Pregnancy in an arcuate uterus can progress to term with a healthy newborn. However, non-uniform uterine retraction may exceptionally be associated with postpartum hemorrhage. Vigilance at placental delivery, the 4Ts approach, and bedside ultrasound when the clinical exam is discordant are key elements [6-10,12,13].
Key Points/Learning Messages
a) A firm uterine globe does not exclude postpartum
hemorrhage.
b) In postpartum hemorrhage, promptly apply a structured
etiologic approach (4Ts) and reassess frequently.
c) Bedside ultrasound is useful when the clinical examination
is discordant.
d) If initial measures fail, escalation to mechanical and then
uterus-sparing surgical techniques should be rapid.
Highlights
a) An arcuate uterus may rarely be associated with
segmental/asymmetric uterine atony and immediate PPH.
b) A palpably “good” uterine globe does not exclude
significant bleeding—avoid false reassurance.
c) Bedside ultrasound can rapidly exclude retained tissue
and support early escalation to uterus‑sparing interventions.
References
- Pfeifer SM, Attaran M, Goldstein J, Lindheim SR, Petrozza JC, et al. (2021) The American Society for reproductive medicine Müllerian anomalies classification 2021. Fertil Steril 116(5): 1238-1252.
- Grimbizis GF, Gordts S, Sardo AS, Brucker S, Angelis CD, et al. (2013) The ESHRE/ESGE consensus on the classification of female genital tract congenital anomalies. Hum Reprod 28(8): 2032-2044.
- Dixit R, Duggireddy CS, Pradhan GS (2025) Müllerian anomalies: Revisiting imaging and classification. Insights Imaging 16(1): 40.
- Kugelman N, Gangbe EM, Badeghiesh A, Baghlaf H, Dahan MH (2025) Pregnancy and neonatal outcomes in women with arcuate uterus: A population-based cohort study of over 3.8 million women. BMC Pregnancy Childbirth 25(1): 1143.
- Connolly CT, Hill MB, Klahr RA, Zafman KB, Rebarber A, et al. (2024) Arcuate uterus as an independent risk factor for adverse pregnancy outcomes. Am J Perinatol 41(2): 167-173.
- Escobar MF, Nassar AH, Theron G, Barnea ER, Nicholson W, et al. (2022) FIGO recommendations on the management of postpartum hemorrhage 2022. Int J Gynaecol Obstet 157(1): 3-50.
- Royal College of Obstetricians and Gynaecologists (RCOG) (2017) Prevention and management of postpartum haemorrhage: Green-top guideline no. 52. BJOG 124(5): e106-e149.
- Basso M, Robinson D, Chan C, Duckitt K, Lett R, et al. (2022) Guideline No. 431: Postpartum hemorrhage and hemorrhagic shock. J Obstet Gynaecol Can 44(12): 1293-1310.e1.
- World Health Organization (2012) WHO recommendations for the prevention and treatment of postpartum haemorrhage.
- Queensland Health (2024) Primary Postpartum Haemorrhage (PPH): Queensland clinical guideline. pp: 1-46.
- WOMAN Trial Collaborators (2017) Effect of early tranexamic acid administration on mortality, hysterectomy, and other morbidities in women with postpartum haemorrhage (WOMAN) an international, randomised, double-blind, placebo-controlled trial. Lancet 389(10084): 2105-2116.
- Vardar Z, Dupuis CS, Goldstein AJ, Siddiqui E, Vardar BU, et al. (2022) Pelvic ultrasonography of the postpartum uterus in patients presenting to the emergency room with vaginal bleeding and pelvic pain. Ultrasonography 41(4): 782-795.
- Yagur Y, Jurman L, Weitzner O, Arbib N, Markovitch O, et al. (2023) Ultrasound for diagnosis of postpartum retained products of conception-how accurate we are? BMC Pregnancy Childbirth 23(1): 572.
- Morel O, Malartic C, Muhlstein J, Gayat E, Judlin P, et al. (2011) Pelvic arterial ligations for severe post-partum hemorrhage: Indications and techniques. J Visc Surg 148(2): e95-e102.
- Bouchghoul H, Madar H, Resch B, Pineles BL, Mattuizzi A, et al. (2024) Uterine-sparing surgical procedures to control postpartum hemorrhage. Am J Obstet Gynecol 230(3 Suppl): S1066-S1075.
- B-Lynch C, Coker A, Lawal AH, Abu J, Cowen MJ (1997) The B-Lynch surgical technique for the control of massive postpartum haemorrhage: An alternative to hysterectomy? BJOG 104(3): 372-375.
- Matsubara S, Hitoshi Yano, Akihide Ohkuchi, Tomoyuki Kuwata, Rie Usui, et al. (2013) Uterine compression sutures for postpartum hemorrhage: An overview. Acta Obstet Gynecol Scand 92(4): 378-385.
© 2026 Amina El Alami. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






