- Submissions

Full Text
Investigations in Gynecology Research & Womens Health
Intestinal Function after Surgical Treatment of Deep Endometriosis: A Comparative Cohort Study
Ricardo de Almeida Quintairos1*, Paulo Augusto Ayroza Galvão Ribeiro2, Maurício Simões Abrão3 and Helizabet Salomão Abdalla Ayroza Ribeiro2
1 Center of Endometriosis Porto Dias Hospital Belem, Brazil
2 Division of Gynecology Endoscopy and Endometriosis, Department of Obstetrics and Gynecology, Santa Casa de São Paulo School of Medical Sciences, São Paulo, Brazil
3 Endometriosis Section, Gynecologic Division. Hospital of the Clinics HCFMUSP, Faculty of Medicine, University of São Paulo, SP, Brazil; Gynecologic Division, BP-The Portuguese Beneficent Society of Sao Paulo, SP, Brazil
*Corresponding author:Ricardo de Almeida Quintairos, Center of Endometriosis Porto Dias Hospital Belem, Brazil
Submission:February 04, 2026;Published: March 03, 2026

ISSN: 2577-2015 Volume6 Issue1
Abstract
Study objective: To compare clinical outcomes in women undergoing Segmental Resection (SR) or Linear Excision (LE) of intestinal Deep Infiltrating Endometriosis (DIE) lesions.
Design: Prospective, non-randomized, comparative cohort study.
Setting: Three tertiary referral centers for endometriosis surgery.
Participants: Fifty-six women with DIE lesions located in rectosigmoid undergoing surgical treatment.
Interventions: Surgical treatment of intestinal endometriosis with two techniques: SR (n=28) or LE (n=28); treatment choice was performed according to lesion characteristics by a shared decision-making process with standardized protocols in all hospitals. Measurements and Main
Results: Functional outcomes were assessed using the Knowles-Eccersley-Scott Symptom Questionnaire (KESS) and the Low Anterior Resection Syndrome (LARS) score preoperatively and at 3 and 6 months postoperatively. The SR group had significantly higher LARS scores in 3 months, meaning poorer intestinal functioning compared to LR, however both groups showed improvement over time. At 6 months, no significant difference was observed between groups in KESS scores.
Conclusion: Although SR may be associated with transient poorer bowel function, both techniques demonstrate functional recovery over time.
Keywords:Prospective studies; Postoperative complications; Constipation; Fecal incontinence; Endometriosis; Minimally invasive surgical procedures
Introduction
Deep Infiltrating Endometriosis (DIE) involving the bowel affects up to 12% of patients with endometriosis and is considered the most severe manifestation of the disease [1]. When the rectosigmoid is affected, symptoms can range from cyclic pain to significant gastrointestinal dysfunction, especially in the presence of full-thickness infiltration [2]. When untreated, these cases often result in a marked decrease in quality of
life, impacting nutritional habits, emotional wellbeing, and sexual health [3,4]. The clinical presentation of bowel endometriosis is heterogeneous and often overlaps with other gastrointestinal disorders such as Irritable Bowel Syndrome (IBS) or Inflammatory Bowel Disease (IBD). Patients may present with dyschezia, tenesmus, bloating, alternating bowel habits, constipation, or diarrhea. In more advanced cases, partial bowel obstruction or sub occlusive episodes can occur, especially during menstruation [1,5,6]. Surgical management is indicated in cases of severe, refractory symptoms or anatomical alteration of the intestine leading to impaired transit [7-9]. The primary approaches are Segmental Bowel Resection (SR) [10-12] and nodulectomy. The latter includes techniques such as Linear Excision (LE) [10-12] and Discoid Resection (DR) [13], tailored according to lesion size, depth, and location. SR involves removing an entire segment of the bowel and performing an anastomosis, while nodulectomy aims to excise the nodule while preserving the bowel’s integrity [8].
Recent studies have attempted to refine the criteria for surgical decision making and propose algorithms based on lesion morphology and preoperative imaging [7]. However, an ongoing debate about whether “less is more” is still present. Given that, we aimed to evaluate and compare the functional outcomes of SR and LE in patients with bowel endometriosis, by applying validated tools for postoperative bowel function evaluation.
Materials and Methods
Study design and participants
This is a prospective, non-randomized comparative study. The study population consists of women aged 18 to 45 with a clinical and imaging diagnosis of deep infiltrating endometriosis involving the rectosigmoid. Patients were recruited consecutively from three tertiary referral centers between 2021 and 2024.
Ethics
This study was approved by the Institutional Review Board (IRB) of the Faculty of Medical Sciences of Santa Casa de São Paulo (Decision Number: 6.927.353); Porto Dias Hospital (Decision Number: 7.015.883); and Beneficência Portuguesa de São Paulo Hospital (Decision number: 7.235.312). All participants provided written informed consent before enrolment. The study protocol is registered in the Brazilian Registry of Clinical Trials (ReBEC-Clinical Trials) under the identification RBR-7zrm8fd. The study follows the STROBE Statement [14].
Sample size
We estimated the sample size based on a size effect (Cohen’s d) of 0,4; significance level (α): 0.05 (Zα = 1.645); Type II error (β): 0.20; Statistical power (1-β): 80% (Zβ=0.84) for a paired t test, resulting in 55 participants.
Eligibility criteria
All patients attending the outpatient endometriosis clinic of the three centers were consecutively included in accordance with the eligibility criteria: clinical signs of DIE with intestinal involvement, with at least one of the following symptoms: dysmenorrhea, deep dyspareunia, chronic pelvic pain, infertility, dyschezia, hematochezia, and dysuria [15]; with confirmation by imaging (transvaginal ultrasound with bowel preparation (TVUw/ BP) for endometriosis mapping or Magnetic Resonance Imaging (MRI) of the pelvis [16]; with histopathological confirmation of endometriosis in a surgical specimen. Women with DIE who did not wish or were not eligible for surgical treatment, those unable to complete the questionnaires within the expected deadlines, with a diagnosis of cancer, patients in whom protective ileostomy was performed after surgery, and those who developed rectovaginal fistula in the postoperative period were excluded from the study.
Interventions
The decision of the surgical technique to be used was based on preoperative imaging and agreement of the patient after counselling of the surgeons’ team. Patients with nodules smaller than 3cm, affecting less than 30% of the bowel circumference and less than 15cm of the anal verge were eligible for LE, but this was not always performed. The others necessarily underwent intestinal SR, according to the protocol conducted at the institutions [7]. A team of experienced gynaecologist surgeons performed surgical procedures via video laparoscopic approach following the techniques for intestinal endometriosis previously described by Matuoka et al. [17], Redwine et al. [18] and Ribeiro et al. [8]. Additional interventions have been performed in cases of endometriotic lesions in ovaries, uterosacral ligaments, or other pelvic viscera. In the postoperative period, GnRH analog was prescribed for 3 months for patients who underwent concomitant removal of the endometrioma, and dienogest for those without endometrioma. Women who wanted to become pregnant were instructed to wait three months after surgery.
Instruments
The Knowles-Eccersley-Scott Symptom Questionnaire (KESS) instrument [19] was developed to standardize the chronic obstipation diagnosis, is based on seven multiple choice questions and the score ranges from 0 to 30, the diagnosis is determined with scores of 15 or higher. The Low Anterior Resection Syndrome Score (LARS) questionnaire is a score system based on patient report symptoms related to disfunction caused by rectum anterior wall resection. No LARS: 0-20 points; LARS minor: 21-29 points; LARS major: 30-42 points. Both tools were administered preoperatively and at 3 and 6 months, postoperatively. For the comparative analysis between preoperative, 3 and 6 months postoperatively, it was considered appropriate to use only data from women who had a diagnosis of intestinal constipation, defined by a score of 21 or higher on the LARS questionnaire before surgery. This subgroup was called LARS+.
Statistical analysis
The descriptive statistics include: mean, standard deviation, percentiles, minimum and maximum values for numerical variables; number and proportion for categorical variables. To compare the scores of functional variables (such as LARS and KESS) between different assessment times (preoperative, 3 months, and 6 months postoperative) and between intervention groups (linear and segmental resection), Analysis of variance for repeated measures (ANOVA) was used. Before applying ANOVA, the data were subjected to normality tests (Shapiro-Wilk, asymmetry, and kurtosis) and, when necessary, transformations were performed to ensure the adequacy of the test assumptions. Mauchly’s sphericity test was used to verify the validity of repeated measures ANOVA; in case of violation, appropriate adjustments were applied. After identifying significant differences using ANOVA, post-hoc tests with Bonferroni correction for multiple comparisons were performed to identify the pairs of times at which the differences occurred. The effect size was calculated using partial eta squared for the overall ANOVA and Cohen’s d for paired comparisons. When the ANOVA residuals did not show a normal distribution, the bootstrapping method was used to estimate the distribution of the F statistic and p-values, increasing the robustness of the results.
Results
Figure 1 shows the study participants’ flowchart. Of 101 patients assessed for eligibility, 56 were suitable for allocation, 28 for each group, and all of them received the intended intervention, follow up and had their data analyzed. The baseline characteristics of the sample are presented in Table 1. An analysis of the KESS questionnaire revealed that the total sample had a mean of 10.04 points and a Standard Deviation (SD) of 5.52 in the preoperative period. In the 3-month postoperative period, the mean was 7.82, and the SD was 5.39. Finally, the mean was 6.75, and the SD was 5.05 in 6 months postoperatively. Of the participants, 25% in the SR group and 10% in the LE group achieved 15 points or more, which defines the diagnosis of chronic constipation according to this instrument. Analysis of the LARS questionnaire showed that the total sample had a mean of 19.54, SD=12.02 in the preoperative period, a mean of 17.82, SD=11.40 in 3 months, and a mean of 15.54, SD=10.98 at 6 months postoperatively. The LARS+ subgroup comprised 26 women, 13 of whom were assigned to the LE group and 13 to the SR group. The mean age of the participants was 42 years, with a minimum age of 27 years and a maximum age of 55 years.
Figure 1:Participants’ flow diagram.
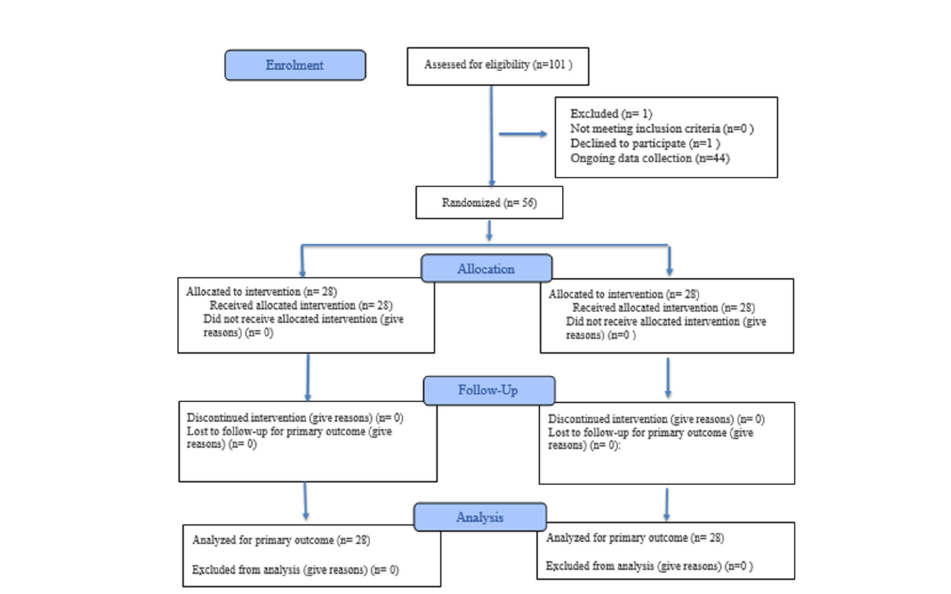
Table 1:Sample baseline characteristics (TOTAL SAMPLE).
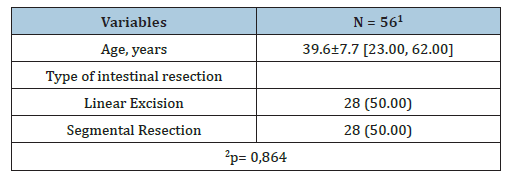
1 Median [Min, Max]; n (%); 2t-test for equality of means.
In the KESS analysis of the LARS+ group, no statistically significant difference was identified between the SR and LE groups (p=0.240). Conversely, statistically significant variations were identified across the evaluated time points (p=0.001). No statistically significant differences were observed for the interaction between group and time (p=0.679). A subsequent analysis of the follow-up times revealed a statistically significant discrepancy between the initial interview and the subsequent interviews conducted after three months (p=0.022) and after six months (p=0.008). The study revealed no statistically significant difference between the 3-month and 6-month groups (p=0.917). (Refer to Table 2 and Figures 2a&2b for further details.)
Figure 2a:Chronic constipation - KESS score and time (LARS +Subgroup).
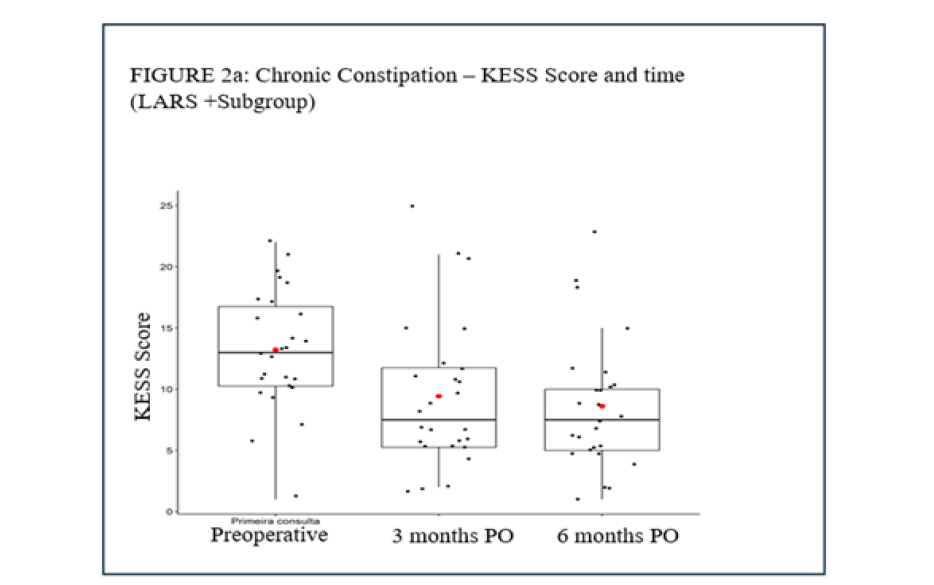
Figure 2b:Chronic constipation - KESS score and time of evaluation (LARS+Subgroup) according to intervention.
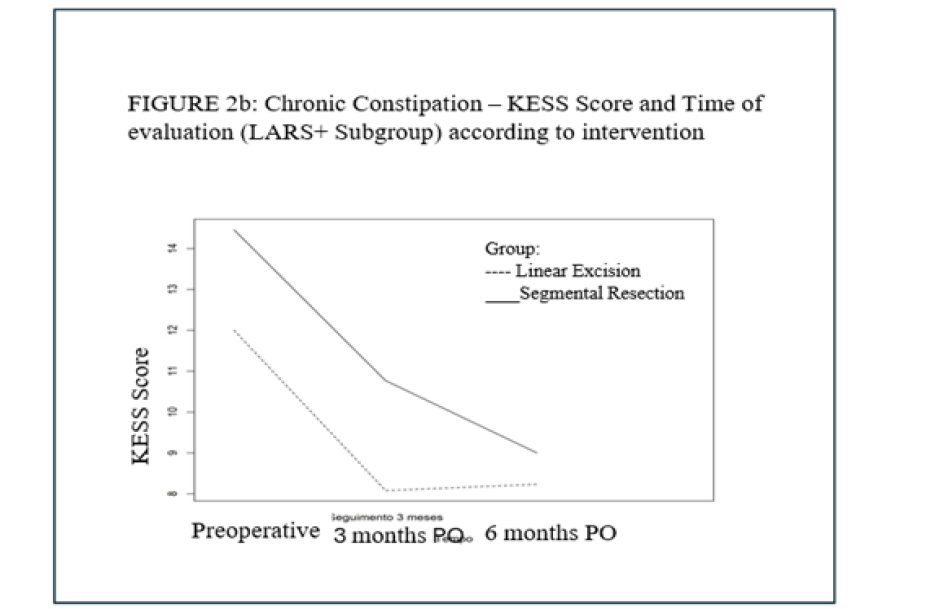
Table 2:Chronic Constipation - KESS scores (LARS+Subgroup).
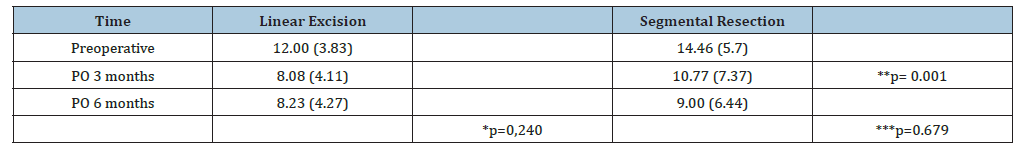

Note: Mean (Standard deviation); *ANOVA comparison between groups; **ANOVA comparison between times; ***ANOVA group: time interaction.
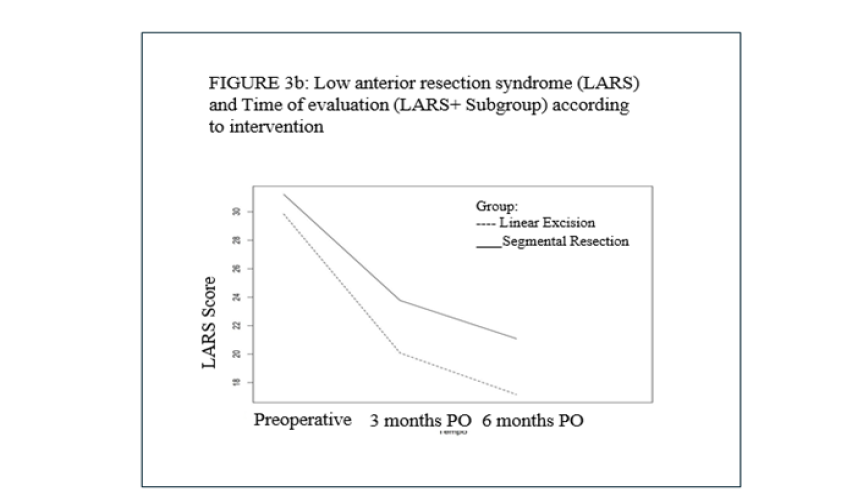
In the LARS analysis, similarly, we did not identify a statistically significant difference between the SR and LE groups (p=0.359). There was a significant difference between the times evaluated (p<0.0001). No significant difference was observed for the interaction between group and time (p=0.960). Exploring the follow-up times, we found significant difference between the first visit and 3 months of follow-up (p=0.001), as well as between the first visit and 6 months of follow-up (p=0.000). There was no difference between the 3rd and 6th months of follow-up (p=0.095) (Table 3) (Figures 3a&3b).
Table 3:Low Anterior Resection Syndrome-LARS Scores (LARS+Subgroup).
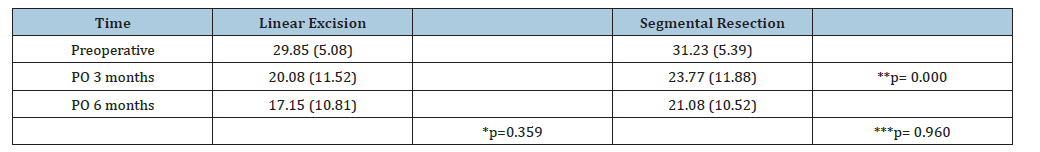
Note: Mean (Standard deviation); *ANOVA comparison between groups; **ANOVA comparison between times; ***ANOVA group: time interaction.
Figure 3a:Boxplot of Low Anterior Resection Syndrome (LARS) and Time of evaluation (LARS+Subgroup).
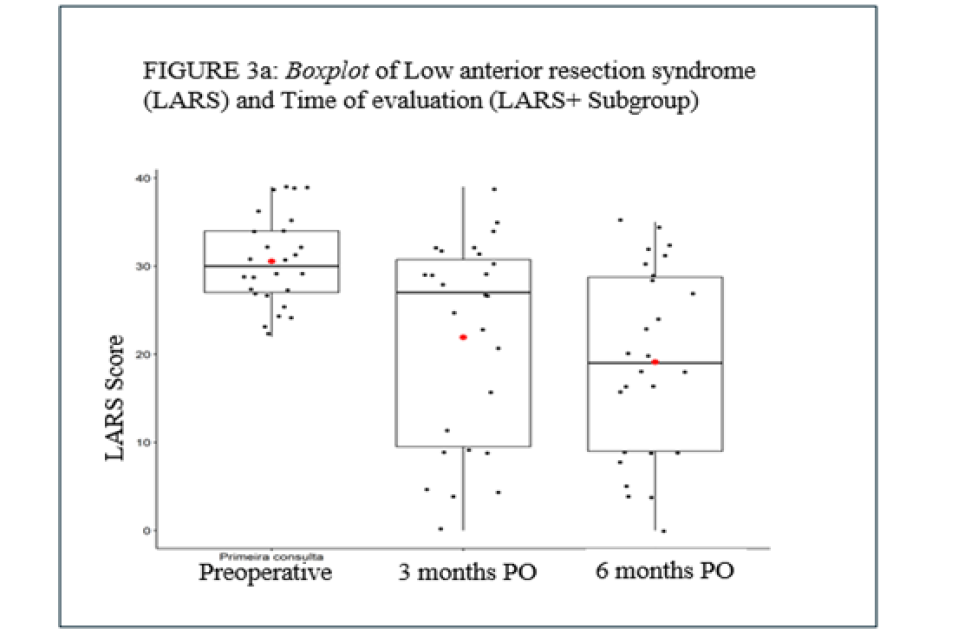
Figure 3b:Low Anterior Resection Syndrome (LARS) and Time of evaluation (LARS+Subgroup) according to intervention.
Discussion
This study demonstrated a significant improvement in functional outcomes during the follow-up period with both surgical approaches (SR and LE). These findings support the notion that surgical management of bowel endometriosis contributes to symptom relief in patients with DIE, either through direct excision of the lesions or by restoring pelvic anatomy via the release of adhesions caused by the disease. Recent years have witnessed a change in the paradigm of the surgical management of bowel endometriosis, with a growing preference for conservative techniques over extensive SR. Numerous studies have shown that function-preserving approaches, such as linear or discoid excision, can offer symptom relief comparable to SR, with a lower incidence of postoperative bowel dysfunction, including rectal urgency, incontinence, and Low Anterior Resection Syndrome (LARS) [19]. A systematic review in 2021 [20] highlighted that patients undergoing conservative excision had significantly lower rates of major complications and better functional outcomes at long-term follow-up. Additionally, shorter operative time and reduced hospital stay were observed in the conservative groups, which is particularly relevant in the context of minimally invasive gynecology and valuebased surgical care.
Another relevant point is the concept of ‘function-first’ surgery, where lesion removal is tailored to preserve pelvic organ function whenever possible. Studies have demonstrated that in selected cases, particularly with lesions <3cm and limited bowel circumference involvement, linear or discoid resection is sufficient to alleviate symptoms without compromising oncologic or anatomic safety [21,22].
On the other hand, SR tends to produce functional results comparable to other more conservative techniques, it is associated with a higher risk of complications, notably rectovaginal fistula [23]. Therefore, it should be indicated only for cases with extensive visceral involvement [23]. Thus, the absence of significant differences between the groups in our study reinforces the idea that the choice of technique can, in many cases, be guided by anatomical criteria and the experience of the surgical team, without compromising the functional outcome.
Among the positive aspects of the study, the rigorous methodology with a prospective design and the application of robust statistical reinforce the reliability of the results. Another key point is the use of validated instruments, KESS and LARS, both translated and validated for the Brazilian context, which allows a standardized and objective assessment of intestinal symptoms.
The study’s limitations consist in small sample size, with 56 participants (28 per group), that may have limited the statistical power needed to detect subtle differences between surgical techniques. Despite the absence of randomization in the allocation of procedures may introduce biases, decision-making process in complex gynecological surgery follows individualized care. The 6-month follow-up period may not be sufficient to capture the longterm evolution of symptoms and their recurrence, longer followups in future studies are in our planning.
Conclusion
This study shows that even though segmental resection showed less pronounced improvement in the early postoperative period compared to linear excision, both techniques resulted in substantial and sustained functional gains over six months. These findings indicate that the choice between segmental resection and linear excision can be guided by lesion characteristics and surgical expertise, as both approaches are effective in restoring bowel function and improving patient outcomes.
Statements and Declarations
Ethics
This study has received approval from the Human Research Ethics Committee of Santa Casa de São Paulo, Decision No. 6.927.353; the Ethics Committee of Porto Dias Hospital, Belém, PA, Decision No. 7.015.883; and the Ethics Committee of Beneficência Portuguesa Hospital, São Paulo, SP, Decision No. 7.235.312. The study is registered in the Brazilian Clinical Trials Registry (REBEC), that is part of the International Clinical Trials Registry Platform (ICTRP) Network, under the identification RBR-7zrm8fd.
References
- Chapron C, Fauconnier A, Vieira M, Barakat H, Dousset B, et al. (2003) Anatomical distribution of deeply infiltrating endometriosis: Surgical implications and proposition for a classification. Human Reproduction 18(1): 157-161.
- Fauconnier A, Chapron C (2005) Endometriosis and pelvic pain: Epidemiological evidence of the relationship and implications. Hum Reprod Update 11(6): 595-606.
- Nnoaham KE, Hummelshoj L, Webster P, D’ Hooghe T, Nardone FD, et al. (2011) Impact of endometriosis on quality of life and work productivity: A multicenter study across ten countries. Fertil Steril 96(2): 366-373.
- Simoens S, Dunselman G, Dirksen C, Bokor A, Brandes I, et al. (2012) The burden of endometriosis: Costs and quality of life of women with endometriosis and treated in referral centres-of-illness/quality of life/international/multi-centre. Human Reproduction 27(5): 1292-1299.
- Koninckx PR, Martin DC (1992) Deep endometriosis: A consequence of infiltration or retraction or possibly adenomyosis externa? Fertil Steril 58(5): 924-928.
- Ballweg ML (2024) Impact of endometriosis on women’s health: Comparative historical data show that the earlier the onset, the more severe the disease. Best Pract Res Clin Obstet Gynaecol 18(2): 201-218.
- Abdalla-Ribeiro H, Maekawa MM, Lima RF, De Nicola ALA, Rodrigues FCM, et al. (2021) Intestinal endometriotic nodules with a length greater than 2.25cm and affecting more than 27% of the circumference are more likely to undergo segmental resection, rather than linear nodulectomy. PLoS One 16(4): e0247654.
- Ribeiro PAA, Rodrigues FC, Kehdi IPA, Rossini L, Abdalla HS, et al. (2006) Laparoscopic resection of intestinal endometriosis: A 5-year experience. J Minim Invasive Gynecol 13(5): 442-446.
- Abrão MS, Bassi MA, Podgaec S, Júnior JAD, Sobrado CW, et al. (2009) Bowel endometriosis: A benign disease? Review Article Rev Assoc Med Bras 55(5): 611-617.
- Roman H, Vassilieff M, Gourcerol G, Savoye G, Leroi AM, et al. (2024) Surgical management of deep infiltrating endometriosis of the rectum: Pleading for a symptom-guided approach. Hum Reprod 26(2): 274-281.
- Abrão MS, Podgaec S, Dias JA, Averbach M, Silva LFF, et al. (2008) Endometriosis lesions that compromise the rectum deeper than the inner muscularis layer have more than 40% of the circumference of the rectum affected by the disease. J Minim Invasive Gynecol 15(3): 280-285.
- Panebianco V, Poli A, Blandino R, Pistritto A, Puzzo L, et al. (1994) Low anterior resection of the rectum using mechanical anastomosis in intestinal endometriosis. Minerva Chir 49(3): 215-217.
- Landi S, Pontrelli G, Surico D, Ruffo G, Benini M, et al. (2008) Laparoscopic disk resection for bowel endometriosis using a circular stapler and a new endoscopic method to control postoperative bleeding from the stapler line. J Am Coll Surg 207(2): 205-209.
- Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, et al. (2008) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: Guidelines for reporting observational studies. J Clin Epidemiol 61(4): 344-349.
- Bellelis P, Dias JA, Podgaec S, Gonzales M, Baracat EC, et al. (1992) Epidemiological and clinical aspects of pelvic endometriosis–a case series. Rev Assoc Med Bras 56(4): 467-471.
- Reid S, Lu C, Condous G (2015) Can we improve the prediction of pouch of douglas obliteration in women with suspected endometriosis using ultrasound-based models? A multicenter prospective observational study. Acta Obstet Gynecol Scand 94(12): 1297-1306.
- Matuoka M, Abdalla-Ribeiro H, Ferruzzi C, Costa A, Ohara F, et al. (2015) Laparoscopic resection of intestinal endometriosis: The linear nodulectomy. J Minim Invasive Gynecol 22(6S): S133.
- Redwine DB, Sharpe DR (1991) Laparoscopic segmental resection of the sigmoid colon for endometriosis. J Laparoendosc Surg 1(4): 217-220.
- Quintairos RA, Brito LGO, Farah D, Ribeiro HSAA, Ribeiro PAAG (2022) Conservative versus radical surgery for women with deep infiltrating endometriosis: Systematic Review and meta-analysis of bowel function. J Minim Invasive Gynecol 29(11): 1231-1240.
- Bendifallah S, Puchar A, Vesale E, Moawad G, Daraï E, et al. (2024) Surgical outcomes after colorectal surgery for endometriosis: A systematic review and meta-analysis. J Minim Invasive Gynecol [28(3): 453-466.
- Kho RM, Andres MP, Borrelli GM, Neto JS, Zanluchi A, et al. (2021) Surgical treatment of different types of endometriosis: Comparison of major society guidelines and preferred clinical algorithms. Best Pract Res Clin Obstet Gynaecol 51: 102-510.
- Jayot A, Bendifallah S, Abo C, Arfi A, Owen C, et al. (2025) Feasibility, complications, and recurrence after discoid resection for colorectal endometriosis: A series of 93 cases. J Minim Invasive Gynecol 27(1): 212-219.
- Donnez O, Roman H (2017) Choosing the right surgical technique for deep endometriosis: Shaving, disc excision, or bowel resection? Fertil Steril 108(6): 931-942.
© 2026 Ricardo de Almeida Quintairos. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






