- Submissions

Full Text
Investigations in Gynecology Research & Womens Health
The Role of Immunological and Genetic Factors in Neonatal Lupus
Shiva Ghayur, Sima Koohestani, Aezo Zare And Shahin Asadi*
Department of Obstetrics and Gynecology, School of Medicine, Urmia University of Medical Sciences, Urmia, Iran
*Corresponding author:Shiva Ghayur, Department of Obstetrics and Gynecology, School of Medicine, Urmia University of Medical Sciences, Urmia, Iran
Submission:February 13, 2026;Published: February 20, 2026

ISSN: 2577-2015 Volume5 Issue5
Abstract
Neonatal lupus is a rare acquired autoimmune disorder that is present at birth (congenital). Affected infants often develop a distinctive red rash or skin eruptions. The most important potential complication is a heart condition known as congenital heart block. Congenital heart block does not resolve in the first few months of life, and infants may eventually need a pacemaker. Some infants have only skin symptoms, some infants have only heart symptoms, and in rare cases, some infants develop both. The most common symptom associated with neonatal lupus is a skin rash consisting of reddish, ring-shaped skin lesions that resemble the rash associated with systemic lupus erythematosus. The rash is temporary (transient), usually appearing in the first few weeks of life and disappearing at some point in the next few months. In rare cases, the skin lesions may persist into childhood. The face and scalp are most commonly affected. The raccoon eye patch, if present, is a big clue to the diagnosis. Neonatal lupus is a rare acquired disorder that occurs when specific antibodies are transferred across the placenta from a pregnant woman to the developing fetus. In most cases, it is an anti-Ro/SSA antibody, an anti-La/SSB antibody, or both. In rare cases, the skin rash associated with neonatal lupus has been associated with another autoantibody that reacts against a different type of ribonucleoprotein (called an anti-RNP test). Other symptoms, such as congenital heart block, are not thought to occur with anti-RNP, but a few isolated cases have been reported recently, the significance of which is not yet clear.
Keywords:Neonatal lupus; Autoimmune disorder; Erythematosus; Anti-La/SSB antibody
Introduction
Neonatal lupus is a rare acquired autoimmune disorder that is present at birth (congenital). Affected infants often develop a distinctive red rash or skin eruptions. The most important potential complication is a heart condition known as congenital heart block. Congenital heart block does not resolve in the first few months of life, and infants may eventually need a pacemaker. Some infants have only skin symptoms, some infants have only heart symptoms, and in rare cases, some infants develop both. Less common findings include liver disease, an abnormally large head circumference (macrocephaly), or low numbers of circulating platelets that help with blood clotting (thrombocytopenia), white blood cells that help fight infection (neutropenia), and red blood cells that help carry oxygen to the body (anemia). Neonatal lupus is caused by specific autoantibodies that are passed across the placenta from a pregnant woman to her developing fetus. These autoantibodies damage specific tissues in the fetus through a process that is not fully understood [1]. Neonatal lupus is not the neonatal form of lupus (systemic lupus erythematosus). The disorder is so named because the skin rash resembles the rash associated with lupus. The affected infant or child does not have systemic lupus erythematosus, and the mother often does not have the disease either (this is often passed on to the mother by mistake, but she has a 20% risk of developing lupus later). Neonatal lupus is a separate disorder [1].
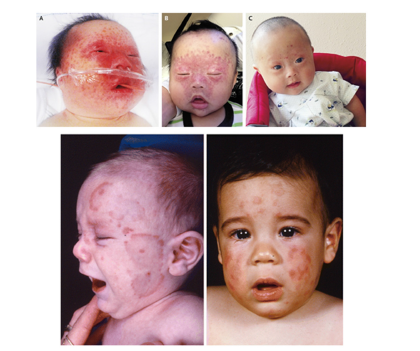
The most common symptom associated with neonatal lupus is a skin rash consisting of reddish, ring-shaped skin lesions that resemble the rash associated with systemic lupus erythematosus. The rash is temporary (transient), usually appearing in the first few weeks of life and disappearing at some point in the next few months. In rare cases, the skin lesions may persist into childhood. The face and scalp are most commonly affected. The raccoon eye patch, if present, is a big clue to the diagnosis. Rarely, the rash may appear on the trunk, arms, and legs. Some affected infants may also show an abnormal sensitivity to sunlight (photosensitivity), which may initially cause the rash. Although the most common time for the rash to appear is about 6 weeks after birth, sometimes the rash may not appear until 2 to 3 months later. It is important to note that breastfeeding is not associated with an increased risk of the rash (Figure 1) [1,2].
Figure 1:Images of infants and children with neonatal lupus disorder [1].
The most serious complication of neonatal lupus is a heart condition known as congenital heart block. The incidence of congenital heart block in newborns may be as common as skin rashes, but it is not known. This is the most serious complication, and once the block is complete, it is a permanent condition and can be potentially life-threatening. Congenital heart block is characterized by interference with the transmission of the heart’s impulses from the top to the middle (conduction system) that controls the heart rate. The severity of such conduction abnormalities may vary among affected infants, meaning that there can be first, second-, or third-degree blocks, the latter being the most serious (Figure 2) [1,2].
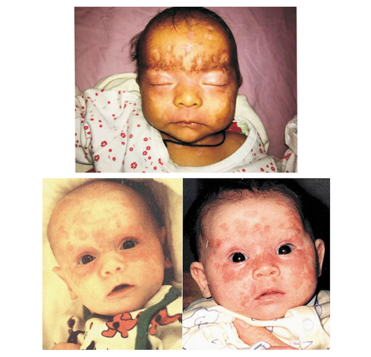
Figure 2:Other images of infants with neonatal lupus with skin disorder [1].
The normal heart has four chambers. The two upper chambers, known as the atria, are separated from each other by a fibrous partition called the atrial septum. The two lower chambers, known as the ventricles, are separated from each other by the ventricular septum. Valves connect the atria (left and right) to their respective ventricles. In the mild form of heart block, the two upper chambers of the heart (the atria) beat normally and there is little time for the lower chambers (the ventricles) to be stimulated, but this is of no clinical significance. In more moderate forms, some beats are missed (second-degree block, which slows the heart rate slightly) and in the most severe form, there are no beats missed at all. This is the severe form of complete heart block, in which the atria beat at a normal rate but the ventricles beat slowly. In some cases, heart block may lead to fainting (syncope), shortness of breath, or irregular heartbeats (arrhythmias). Some babies may also develop a heart muscle disease (cardiomyopathy), which can occur with thickening of the muscle lining of the heart chambers due to an increase in the amount of supporting connective tissue and elastic fibers (endocardial fibroelastosis). In rare cases, additional heart abnormalities have been reported, including inflammation of the myocardium, which is the middle layer of the heart wall, a condition known as myocarditis. In severe cases, potentially lifethreatening complications such as heart failure or sudden cardiac arrest can develop. There may also be abnormalities of the mitral and tricuspid valves [1,2].
Infants with neonatal lupus may also have low numbers of certain red blood cells (platelets) that help blood clot (thrombocytopenia), low levels of other circulating red blood cells (anemia), low levels of certain white blood cells (neutropenia), and an abnormally large spleen (splenomegaly), an abnormally large liver (hepatomegaly), and a type of liver disease known as cholestatic hepatitis. Cholestatic hepatitis is a rare condition characterized by blocked or reduced bile flow from the liver (cholestasis), inflammation of the liver (hepatitis), and yellowing of the skin, mucous membranes, and the whites of the eyes (jaundice). Fortunately, anything more than a transient increase in liver enzymes without associated symptoms is the most common liver abnormality. Again, most of these noncardiac abnormalities resolve within the first six months of an affected baby’s life, when maternal antibodies are cleared from the baby’s circulation. Although very rare, some babies with neonatal lupus may have an abnormally large head (macrocephaly). Macrocephaly is defined as a condition in which the head circumference is larger than expected for the child’s age and sex. Some of these babies and children may develop hydrocephalus, a condition characterized by an excessive buildup of cerebrospinal fluid in the skull, which can put pressure on brain tissues (Figure 3) [1,2].
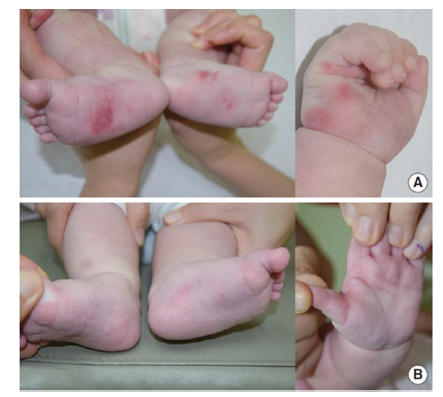
Figure 3:Images of skin disorder in neonatal lupus [1].
Neonatal lupus is a rare acquired disorder that occurs when specific antibodies are transferred across the placenta from a pregnant woman to the developing fetus. In most cases, it is an anti-Ro/SSA antibody, an anti-La/SSB antibody, or both. In rare cases, the skin rash associated with neonatal lupus has been associated with another autoantibody that reacts against a different type of ribonucleoprotein (called an anti-RNP test). Other symptoms, such as congenital heart block, are not thought to occur with anti-RNP, but a few isolated cases have been reported recently, the significance of which is not yet clear. Antibodies are produced by the immune system to fight foreign substances, known as antigens, in the body. Antigens include microorganisms that have the potential to cause disease, toxins, and other such substances. During pregnancy, antibodies pass from the mother across the placenta into the bloodstream of the developing fetus. This is a normal and important process because the fetus cannot make antibodies on its own. In neonatal lupus, certain antibodies called autoantibodies also cross the placenta. Autoantibodies are antibodies that mistakenly damage healthy tissue (autoantigens). Autoantibodies are produced in people with autoimmune disorders such as lupus, Sjögren’s syndrome, and other disorders. These autoantibodies attack healthy tissue in the fetus, causing the various symptoms associated with neonatal lupus. The exact underlying process by which maternal autoantibodies affect the fetus is not fully understood. Mothers of infants with neonatal lupus do not necessarily have lupus themselves. Women who have anti-Ro or anti-La antibodies may have a different rheumatic disorder, such as Sjögren’s syndrome or rheumatoid arthritis. In many cases, women with these antibodies may have no symptoms of rheumatic disease (asymptomatic) or only vague symptoms such as sensitivity to light or discoloration of the fingers in cold weather (Raynaud’s) suggestive of rheumatic disease, or they may only be diagnosed with an autoimmune disorder after their baby is diagnosed with neonatal lupus. Again, it is important to remember that many mothers are clinically healthy and have no disease, just the autoantibodies [1,3].
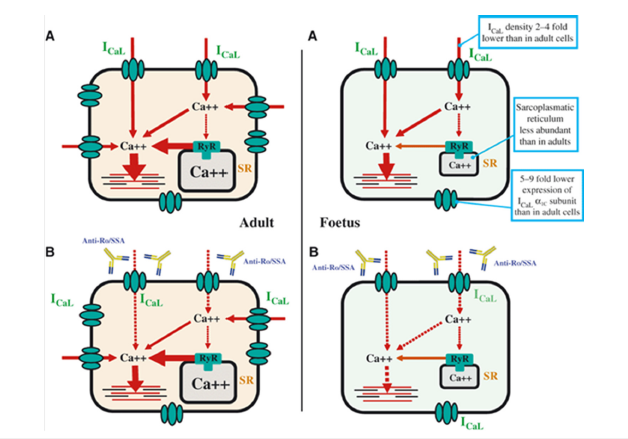
Regarding the risk of congenital heart block, this is not related to lupus or SS, but rather to the autoantibodies. The risk is about 2% (one in fifty). However, again, regardless of the mother’s health status, if a previous pregnancy resulted in a child with heart block, the odds of another child having the condition are about 18%. If a mother has a child with a rash, the odds of another child having a rash are about 30%, but heart block is about 13%. Pregnant women with anti-Ro or anti-La antibodies all pass the antibodies to the developing fetus, but as mentioned above, only about one in 50 children will develop neonatal lupus syndrome. Since most women with these disorders have children who do not develop neonatal lupus, researchers believe that other factors, most likely genetic or environmental, are necessary to cause the disorder (Figure 4) [1,3].
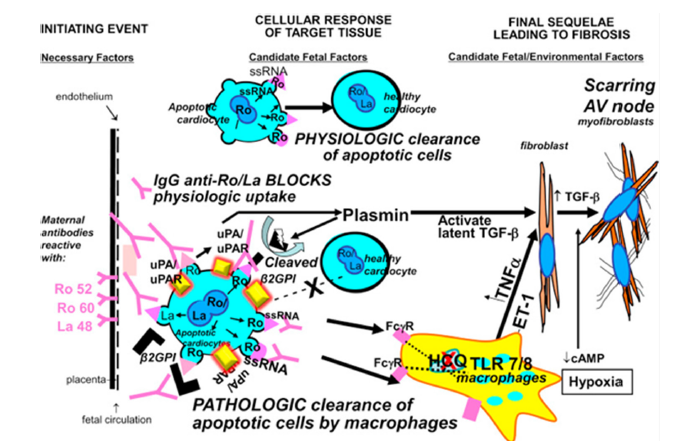
Figure 4:Schematic of the physiological and pathological mechanism of RO/LA antibody [1].
Neonatal lupus is a rare disease that occurs slightly more often in female infants, but is much less common in females than in systemic lupus erythematosus. Most symptoms of the disorder, except for congenital heart block, are temporary (transient) and usually resolve within a few months. The exact incidence is unknown, but it is estimated that congenital heart block occurs in 1 in 15,000 live births. In general, heart block associated with maternal autoantibodies occurs in the absence of any structural abnormalities of the heart [1,4]. The symptoms of the following disorders can be similar to those of neonatal lupus. Comparison may be helpful for differential diagnosis: There are several syndromes characterized by skin rashes at birth (congenital), including Bloom syndrome, Rothmund-Thompson syndrome, Langerhans cell histiocytosis, granuloma annulare, juvenile dermatomyositis, tinea versicolor, corporis, erythema multiforme, atopic dermatitis, and psoriasis. There are several infections that can occur weeks before or after birth (perinatally), including congenital rubella, congenital syphilis, cytomegalovirus, and group B streptococcus. These disorders usually have additional findings that distinguish them from neonatal lupus (Figure 5) [1,5].
Figure 5:Schematic of RO/SSA antibodies in infants (A and B on the right) and adults (A and B on the left) [1].
The diagnosis, of course, depends on the presentation. If the fetal heart rate is slow during pregnancy, an echocardiogram is ordered. An echocardiogram is a test that uses reflected sound waves to create an image of the heart and is needed to assess heart function and diagnose heart block. The mother should be tested immediately for anti-Ro and anti-La antibodies. The diagnosis of a skin rash is based on a thorough clinical evaluation. It may not always be necessary to test the infant or fetus for antibodies because the mother’s blood test will reveal the signs of most cases of the disease or disorder in the fetus [1,6]. Treatment for neonatal lupus is directed at the specific symptoms that are evident in each individual. Skin symptoms usually resolve without treatment (spontaneously) within the first few months of life. Infants diagnosed with neonatal lupus should receive a thorough evaluation to determine whether there are also blood (hematologic) or liver complications [1,7].
Sun protection (such as sunscreen and protective clothing) is recommended for infants initially. Mild topical steroids may be used to treat skin symptoms, but in most cases, treatment is not necessary and should be discussed with the paediatrician. The rash may be purely cosmetic and not require treatment [1,8]. Infants with a rash should have an EKG. However, if there are no signs of a heart problem during pregnancy or at birth, those with other manifestations of neonatal lupus do not need ongoing cardiac evaluation. For infants with congenital heart block, many will require pacemaker implantation. In infants with less severe heart disease, periodic monitoring of heart function should be performed in case a pacemaker is needed later in childhood. Other treatment is symptomatic and supportive [1,9].
Fluorinated steroids such as dexamethasone have been used during pregnancy to treat fetuses with heart disease before birth (in the womb). This has shown some benefit in some cases where there is incomplete heart block. However, some studies of fluoro steroids have shown no benefit. More research is needed to determine the long-term safety and effectiveness of this potential treatment. Some studies have shown that the antimalarial drug hydroxychloroquine may reduce the risk of heart disease in families with a previously affected child or prevent recurrence of heart disease. A large NIH-supported study is nearing completion, and results should be published next year. Intravenous immunoglobulin has shown potential in treating cardiomyopathy with neonatal lupus, both in utero and after birth [1,9].
Case Reports
According to a case report in the research of Ping Li from Shenzhen University, China, Department of Dermatology in 2025 Case Report: Siblings with neonatal lupus erythematosus.
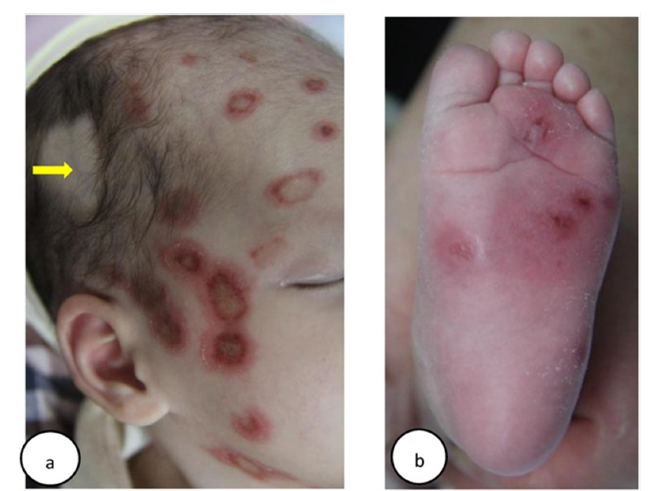
Case 1: In October 2015, a 15-day-old girl (patient 1) presented with erythema on her body. Born via vaginal delivery at 40 weeks to a 29-year-old mother, she exhibited targetoid erythematous plaques with central atrophy and raised margins on her face (Figure 1a), trunk, extremities, palms, and soles (Figure 1b). Laboratory tests indicated that the liver and kidney functions and the complete blood count were normal. Serologic tests revealed strongly positive SSA (Ro) and SSB (La) antibodies, a reactive ANA titer of 1:1000 with a speckled nuclear pattern by Indirect Immunofluorescence (IIF), and a negative syphilis test. Echocardiogram and Electrocardiogram (ECG) results were normal. NLE was diagnosed based on the clinical presentation and serologic findings [10].
Case 2: Six years later, the mother became pregnant again. At 4 weeks of gestation, serologic tests revealed strongly positive SSA and SSB antibodies, a reactive ANA (>1:1000) with a speckled nuclear pattern (as determined by IIF), consistent with findings from 6 years prior, and an elevated erythrocyte sedimentation rate (ESR) of 90mm/h (normal <10mm/h). The mother was prescribed prednisone (10mg/day), hydroxychloroquine (400mg/day), and calcium carbonate (600mg/day) due to her active condition. However, she poorly adhered to the regimen, stopping medications at 20 and 35 weeks of pregnancy due to a cold. Missed doses limited medication use during pregnancy to <20 weeks. At the 32nd week of gestation, her Oral Glucose Tolerance Test (OGTT) was normal, but recommended prenatal screenings, such as fetal echocardiograms, were inconsistently performed due to non-adherence.
A male infant (patient 2) was delivered via cesarean section at 39 weeks’ gestation due to fetal macrosomia, with a birth weight of 4,500g, and normal fasting blood glucose (5.1mmol/L) in the newborn. The ECG result of patient 2 at birth indicated sinus tachycardia, with atrial and ventricular rates of 166bpm, a P-R interval of 100ms, and a QRS duration of 77ms. Although this heart rate was slightly above the normal range for newborns (120- 160bpm), subsequent monitoring revealed stabilization at 140bpm without the development of CHB (Figure 6) [10].
Figure 6:(a) Case 1: Clinical appearances of head lesions: Inflammatory annular plaques, with hyperkeratotic borders and atrophic centers. The alopecia spot on the right side of the head was due to shave by healthcare workers, which could expose the superficial vein of the scalp (yellow arrow), for the purpose of taking blood tests. (b) Case 1: Multiple discoid skin lesions on the left plantar. Despite their rarity in NLE, plantar lesions are significant indicators of potential systemic involvement, requiring comprehensive evaluations and appropriate management for a favorable prognosis [10].
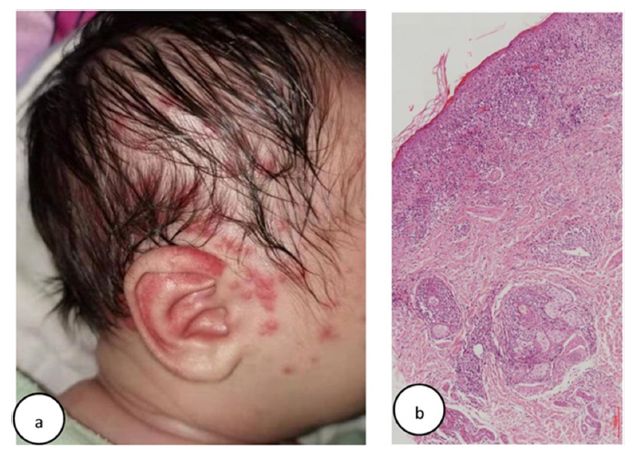
At 1 week after birth, he gradually developed a localized rash on the scalp and face, characterized by erythema and papules (Figure 2a), distinct from his sister’s (Case1) widespread targetoid plaques. Laboratory tests revealed positive SSA, SSB, and ANA (1:100) with a speckled nuclear pattern, as determined by IIF. Skin biopsy revealed a vacuolar change of epidermal basal cells and perivascular and periadnexal mononuclear infiltrate in the dermis (Figure 2b). A diagnosis of NLE for Case 2 was made [10]. In Case 2, the rash resolved by 5.5 months without treatment, with no residual pigmentation or telangiectasia. At 8 months, ANA and SSB were negative, with transient Anti-dsDNA elevation (161IU/ ml), which later turned negative after 2 years. At present, both siblings remain free of skin lesions and autoimmune diseases, under ongoing follow-up [10]. Consent for publication of this case report and accompanying images was obtained from the patient’s parents after they were fully informed and had provided written authorization (Figure 7) [10].
Figure 7:(a) Case 2: Multiple erythema and papules on one face. (b) Case 2: Histology of lesional skin: Slight epidermal atrophy and hyperkeratosis, vacuolar degeneration at the dermal-epidermal junction, perivascular and periadnexal mononuclear infiltrate in the dermis (Hematoxylin–eosin stain, original magnifification, ×100) [10].
Discussion and Conclusion
Neonatal lupus is not the neonatal form of lupus (systemic lupus erythematosus). The disorder is so named because the skin rash resembles the rash associated with lupus. The affected infant or child does not have systemic lupus erythematosus, and the mother often does not have the disease either (this is often passed on to the mother by mistake, but she has a 20% risk of developing lupus later). Neonatal lupus is a separate disorder. The face and scalp are most commonly affected. The raccoon eye patch, if present, is a big clue to the diagnosis. Rarely, the rash may appear on the trunk, arms, and legs. Some affected infants may also show an abnormal sensitivity to sunlight (photosensitivity), which may initially cause the rash. Although the most common time for the rash to appear is about 6 weeks after birth, sometimes the rash may not appear until 2 to 3 months later. It is important to note that breastfeeding is not associated with an increased risk of the rash (Figure 1). The exact underlying process by which maternal autoantibodies affect the fetus is not fully understood. Mothers of infants with neonatal lupus do not necessarily have lupus themselves. Women who have anti- Ro or anti-La antibodies may have a different rheumatic disorder, such as Sjögren’s syndrome or rheumatoid arthritis. In many cases, women with these antibodies may have no symptoms of rheumatic disease (asymptomatic) or only vague symptoms such as sensitivity to light or discoloration of the fingers in cold weather (Raynaud’s) suggestive of rheumatic disease, or they may only be diagnosed with an autoimmune disorder after their baby is diagnosed with neonatal lupus. Regarding the risk of congenital heart block, this is not related to lupus or SS, but rather to the autoantibodies. The risk is about 2% (one in fifty). However, again, regardless of the mother’s health status, if a previous pregnancy resulted in a child with heart block, the odds of another child having the condition are about 18%. If a mother has a child with a rash, the odds of another child having a rash are about 30%, but heart block is about 13%. Pregnant women with anti-Ro or anti-La antibodies all pass the antibodies to the developing fetus, but as mentioned above, only about one in 50 children will develop neonatal lupus syndrome. Treatment for neonatal lupus is directed at the specific symptoms that are evident in each individual. Skin symptoms usually resolve without treatment (spontaneously) within the first few months of life. Infants with a rash should have an EKG. However, if there are no signs of a heart problem during pregnancy or at birth, those with other manifestations of neonatal lupus do not need ongoing cardiac evaluation. For infants with congenital heart block, many will require pacemaker implantation [1-10].
References
- Asadi S (2017) Pathology of Medical Genetic Books (26 vols). Amidi Publications, Iran.
- Izmirly P, Saxena A, Buyon JP (2017) Progress in the pathogenesis and treatment of cardiac manifestations of neonatal lupus. Curr Opin Rheumatol 29(5): 467-472.
- Saxena A, Izmirly PM, Han SW, Briassouli P, Rivera TL, et al. (2015) Serum biomarkers of inflammation, fibrosis, and cardiac function in facilitating diagnosis, prognosis, and treatment of anti-SSA/Ro-associated cardiac neonatal lupus. J Am Coll Cardiol 66(8): 930-939.
- Brito-Zeron P, Izmirly PM, Ramos-Casals M, Buyon JP, Khamashta MA (2015) The clinical spectrum of autoimmune congenital heart block. Nat Rev Rheumatol 11(5): 301-312.
- Morel N, Georgin-Lavialle S, Levesque K, Guettrot-Imbert G, Guern VL, et al. (2015) Neonatal lupus syndrome: Literature review. Rev Med Interne 36(3): 159-166.
- Levesque K, Morel N, Maltret A, Baron G, Masseau A, et al. (2015) Description of 214 cases of autoimmune congenital heart block: results of the French neonatal lupus syndrome. Autoimmune Rev 14(12): 1154-1160.
- Saxena A, Izmirly PM, Mendez B, Buyon JP, Friedman DM (2014) Prevention and treatment of in utero of autoimmune-associated congenital heart block. Cardiol Rev 22(6): 263-267.
- Chen CC, Lin KL, Chen CL, Wong AM, Huang JL (2013) Central nervous system manifestations of neonatal lupus: A systematic review. Lupus 22(14): 1484-1488.
- Femia AN, Callen JP, Vleugels RA (2018) Neonatal and pediatric lupus erythematosus. Medscape.
- Tang P, Zhang H, Li P (2025) Case Report: Siblings with neonatal lupus erythematosus. Front. Pediatr 13: 1518881.
© 2026 Shahin Asadi. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






