- Submissions

Full Text
Gerontology & Geriatrics Studies
Beyond the Blueprint: Dermatological and Systemic Implications of Cement Exposure in Gloveless Construction Workers
Mahin Jamil1, Zeenat Khan2* and Daud Khan3
1 Department of Civil Engineering, University of Engineering and Technology (UET), Pakistan
2 Department of Bioinformatics and Biosciences, Capital University of Science & Technology, Pakistan
3 Department of Civil Engineering, Capital University of Science & Technology, Pakistan
*Corresponding author:Zeenat Khan, Department of Bioinformatics and Biosciences, Capital University of Science & Technology, Islamabad, Pakistan
Submission: March 17, 2026; Published: March 30, 2025

ISSN 2578-0093Volume10 Issue 2
Abstract
Cement, a cornerstone of modern construction, carries hidden occupational hazards that extend far beyond its structural role. Workers handling cement without protective gloves are exposed to its highly alkaline and chemically complex nature, leading to a cascade of dermatological and systemic effects. Direct skin contact precipitates irritant and allergic dermatitis, chemical burns, chronic eczema and hyperkeratosis, with hexavalent chromium and trace metals acting as potent sensitizers that amplify immune responses. Beyond the skin, cement dust inhalation and accidental ingestion trigger systemic biochemical perturbations, including oxidative stress, depletion of antioxidant defenses, elevated liver and kidney enzymes and activation of inflammatory pathways. The resulting multi-organ impact underscores cement as a silent but pervasive occupational toxin. Epidemiological and toxicological studies reveal widespread prevalence of skin disorders and biochemical disruptions among exposed construction workers, highlighting an urgent need for innovative protective strategies. Implementation of high-quality personal protective equipment, chromium-reduced cement formulations, workplace ventilation and biomarker-based health surveillance can mitigate these risks. Future research must integrate mechanistic, longitudinal and socio-economic perspectives to elucidate dose-response relationships, cumulative effects and molecular pathways of toxicity. By reframing cement not just as a building material but as a bioactive occupational hazard, this review emphasizes the critical intersection of industrial practice, human health and material innovation, advocating for science-driven protective measures that safeguard worker well-being in construction environments.
Keywords: Cement dust; Occupational toxicity; Dermatitis; Oxidative stress; Heavy metal exposure
Highlights
A. Cement acts as both a structural material and a hidden occupational toxin with dermatological and systemic impacts.
B. Hexavalent chromium and trace metals drive oxidative stress, immune sensitization and multi-organ dysfunction.
C. Innovative prevention including chromium-reduced cement, PPE and biomarker monitoring is essential for worker safety.
Introduction
Cement, a fundamental material in the construction industry, is chemically complex, comprising major oxides such as calcium oxide, silicon dioxide, aluminum oxide, iron oxide and magnesium oxide, along with secondary compounds like sulfur trioxide and trace alkali oxides [1]. Upon hydration, these constituents create a highly alkaline environment, primarily due to calcium hydroxide formation, which can disrupt the skin’s natural protective barrier [2]. Additionally, trace metals including chromium, nickel, cobalt, selenium, thallium and lead, either inherent in raw materials or introduced during manufacturing, elevate the potential for toxic and allergenic reactions [3]. Prolonged dermal exposure, especially among workers who handle cement without gloves or protective clothing, can result in irritant and allergic contact dermatitis, chemical burns, chronic eczema and systemic inflammatory responses [4]. The combination of chemical reactivity, alkalinity and abrasive particles underscores cement as a significant occupational hazard, highlighting the critical need for awareness and preventive safety measures in construction environments [5].
Construction workers are frequently exposed to cement, which poses significant dermatological hazards due to its highly alkaline nature, abrasive particles and sensitizing metals such as chromium and cobalt [6]. Direct contact, particularly with wet cement and in the absence of protective equipment, can lead to a spectrum of skin disorders ranging from mild irritation, dryness and scaling to severe conditions including irritant and allergic contact dermatitis, chemical burns and chronic hyperkeratosis [7]. Repeated exposure disrupts the skin barrier, increases trans epidermal water loss and facilitates deeper penetration of toxic compounds, thereby predisposing workers to persistent inflammation, secondary infections and long-term sensitization [8]. Epidemiological studies consistently demonstrate that hands, forearms and lower limbs are the most affected sites and chronic exposure can compromise both occupational performance and quality of life [9]. These observations underscore the need for preventive strategies, including protective clothing, hygiene practices and workplace interventions, as well as heightened awareness of cement-related dermatological risks in occupational health planning [10].
Exposure to cement dust poses significant biochemical and cellular risks due to its complex composition, including toxic elements such as chromium, cadmium, lead, nickel, cobalt and fine mineral oxides [11]. Inhalation, dermal contact, or ingestion of cement dust can lead to systemic absorption and bioaccumulation of these substances in organs including the liver, kidneys and lungs, disrupting normal cellular metabolism [12]. Occupational studies have demonstrated that prolonged exposure induces oxidative stress, evidenced by elevated reactive oxygen species and lipid peroxidation, depletion of antioxidant defenses and activation of inflammatory pathways [13]. These biochemical disturbances manifest as elevated liver and kidney enzymes, impaired renal function and chronic inflammatory responses, while heavy metals such as hexavalent chromium can trigger immune sensitization, DNA damage and carcinogenic effects [14]. Additionally, cement’s alkaline and abrasive nature compromises skin barrier integrity, facilitating further penetration of toxic compounds and increasing susceptibility to dermatitis and secondary infections [15]. Collectively, these findings highlight the multi-systemic toxic potential of cement dust and underscore the critical need for protective measures, occupational monitoring and regulatory strategies to mitigate health risks in construction environments [16].
Prolonged exposure to cement, especially among construction workers who do not use protective gloves, constitutes a significant occupational health concern with both dermatological and systemic implications [17]. Cement dust, rich in alkaline compounds and trace heavy metals such as hexavalent chromium, can cause irritant and allergic contact dermatitis, eczema, chemical burns and chronic skin disorders, while also promoting systemic biochemical disturbances, including oxidative stress and impaired antioxidant defenses [18]. Epidemiological evidence indicates that a considerable proportion of workers experience workrelated skin diseases, underscoring the widespread nature of this hazard [19]. Effective risk reduction depends on consistent use of personal protective equipment, adherence to hygiene protocols, proper workplace ventilation, material substitution and regular health monitoring, yet these measures are often inconsistently applied [20]. Future research should emphasize longitudinal and mechanistic studies to clarify dose-response relationships, investigate innovative cement formulations or chromium-reduced alternatives and explore molecular pathways underlying toxicity, while also addressing socio-economic barriers to occupational safety [21]. Such integrated efforts are essential to protect workers’ health and translate scientific findings into practical preventive strategies [22].
Chemical Composition of Cement and Potential Skin Hazards
Cement used in the construction industry is a chemically complex material composed of multiple mineral oxides and trace elements that can exert significant effects on human skin upon prolonged exposure [23]. The primary constituents of cement include calcium oxide, silicon dioxide, aluminum trioxide, ferric oxide and magnesium oxide, which collectively contribute to the structural and binding properties of the material (Table 1) [24]. When cement is mixed with water during construction processes, these compounds undergo hydration reactions that produce a highly alkaline environment [25]. The elevated alkalinity, primarily due to calcium hydroxide formation, can disrupt the natural protective barrier of the skin [26]. Continuous exposure to wet cement therefore causes irritation and dryness by damaging the lipid layer that maintains skin hydration [27]. In addition to the major oxides, cement also contains trace elements and impurities such as chromium, nickel, cobalt, selenium, thallium and lead [28]. These metals are introduced either naturally from raw materials such as limestone and clay or during the manufacturing process [29]. The presence of such elements increases the potential for toxic interactions with human tissues [30]. In occupational settings, workers frequently come into direct contact with cement while mixing, pouring, or finishing concrete, allowing these chemical constituents to interact directly with exposed skin surfaces [31]. Prolonged dermal exposure is particularly common in situations where workers do not use protective equipment such as gloves or protective clothing [32]. Repeated contact can gradually weaken the epidermal barrier, making the skin more susceptible to irritation and chemical penetration [33]. As a result, the complex chemical composition of cement represents a significant occupational hazard that can lead to both immediate and long-term dermatological effects in construction workers [34,35].
Table 1:Chemical composition and typical oxide content ranges of Portland cement used in construction materials [24,35].
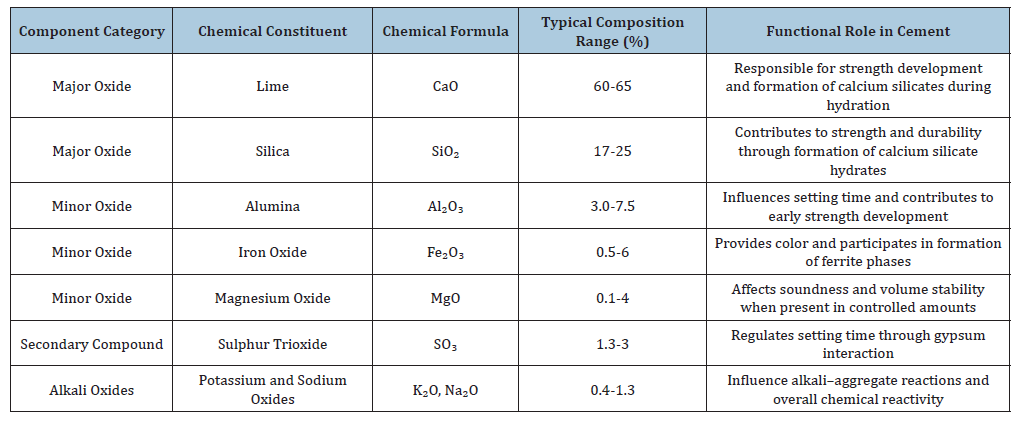
The interaction between cement constituents and the skin can lead to a variety of dermatological conditions ranging from mild irritation to severe inflammatory responses [36]. Wet cement is strongly alkaline and can produce irritant contact dermatitis through prolonged exposure, particularly when it remains trapped against the skin under clothing or footwear [37]. The abrasive nature of sand particles in cement mixtures further exacerbates this effect by mechanically damaging the skin surface, allowing chemical components to penetrate deeper layers [38]. Among the trace elements present in cement, chromium is recognized as one of the most potent sensitizing agents capable of inducing allergic contact dermatitis [39]. Sensitization occurs when repeated exposure triggers an immune response that results in persistent itching, redness, swelling and scaling of the skin [40]. In addition to chromium, metals such as cobalt and nickel can also contribute to hypersensitivity reactions and chronic eczema in exposed individuals [41]. Workers who regularly handle cement without protective barriers often develop symptoms including dryness, fissuring, pruritus and erythema, particularly on the hands and forearms [42]. In more severe cases, prolonged exposure to highly alkaline cement can cause chemical burns that damage deeper skin tissues and lead to ulceration or permanent scarring [43]. The accumulation of heavy metals within the skin may also contribute to chronic dermatological disorders and systemic inflammatory responses [44]. Over time, these chemical interactions can impair the natural regenerative capacity of the skin and increase susceptibility to secondary infections [45].
Dermatological Effects of Cement Exposure
Dermatological disorders represent one of the most frequently reported occupational health problems among workers in the construction and cement industries [46]. Continuous contact with cement, particularly in its wet form, exposes workers to highly alkaline compounds, abrasive particles and sensitizing metals that can damage the skin barrier and initiate inflammatory responses [47]. Cement handling tasks such as mixing, transporting, pouring and finishing concrete frequently involve direct dermal contact, especially in situations where personal protective equipment is not consistently used [48]. The chemical composition of cement, which includes calcium oxide, silica, aluminum compounds and trace metals such as chromium and cobalt, contributes to a variety of dermatological reactions [49]. These reactions range from mild skin irritation and dryness to severe allergic dermatitis and chemical burns [50]. The hands, forearms and lower limbs are the most commonly affected areas because these body parts are directly exposed during construction activities [51]. Workers in cement manufacturing plants, cement transport operations and construction sites are therefore at a heightened risk of developing skin disorders associated with occupational exposure [52].
The prevalence and severity of cement-related dermatological conditions depend on several factors including duration of exposure, concentration of chemical components, environmental conditions and individual susceptibility [53]. Prolonged exposure to wet cement can disrupt the natural protective barrier of the skin, increasing its permeability and making it more vulnerable to irritants and allergens [54]. In addition, abrasive particles present in cement mixtures can cause microtrauma to the skin, facilitating deeper penetration of harmful substances [55]. Epidemiological observations from different occupational settings indicate that irritant contact dermatitis, allergic contact dermatitis and chemical burns are among the most common skin disorders associated with cement exposure [56]. Chronic dermatological conditions such as fissured skin, hyperkeratosis and secondary infections may also develop after repeated exposure [57]. The evidence from occupational health studies demonstrates that dermatological effects are not only common but can significantly impact workers’ productivity, quality of life and long-term health outcomes [58]. Table 2 summarizes selected observational studies and surveillance reports describing dermatological outcomes associated with cement exposure in occupational environments [59].
Table 2:Selected studies reporting dermatological effects of cement exposure in workers.

Irritant Contact Dermatitis
Irritant contact dermatitis is widely recognized as one of the most common dermatological conditions affecting workers exposed to cement in occupational settings [60]. The primary mechanism underlying this condition is the highly alkaline nature of wet cement, which can reach a pH level close to 12 during hydration reactions [61]. Such alkalinity disrupts the natural lipid barrier of the skin and leads to direct chemical irritation of the epidermal layer [62]. Workers frequently come into contact with cement while mixing or applying concrete and prolonged dermal exposure allows alkaline compounds to penetrate the skin surface [63]. This penetration results in inflammation characterized by redness, dryness, itching and burning sensations [64]. Mechanical abrasion caused by sand particles in cement mixtures can further aggravate the condition by producing micro-injuries that increase the permeability of the skin barrier [65]. In many occupational environments, irritant dermatitis develops gradually after repeated contact with cement without adequate protective equipment [66]. Environmental conditions such as moisture, sweating and prolonged working hours can also intensify skin irritation [67].
The progression of irritant contact dermatitis often begins with mild symptoms but can evolve into more severe dermatological complications if exposure continues [68]. Initial manifestations typically include dryness and erythema, followed by scaling, fissuring and increased sensitivity of the affected skin areas [69]. Over time, repeated chemical irritation can weaken the epidermal barrier and increase trans epidermal water loss, indicating impaired skin integrity [70]. Occupational studies have demonstrated that workers exposed to cement frequently exhibit signs of compromised skin barrier function, which predisposes them to further irritation and inflammation [71]. The hands are the most commonly affected region due to direct contact with wet cement mixtures during manual work tasks [72]. In addition to discomfort and pain, persistent irritant dermatitis can reduce manual dexterity and limit a worker’s ability to perform routine construction activities [73]. Secondary infections may also occur when cracks or fissures in the skin allow microorganisms to enter deeper tissues [74]. Without proper protective measures and medical management, irritant dermatitis may progress into chronic dermatological disease [75]. These outcomes emphasize the importance of preventive strategies such as protective gloves, improved hygiene practices and education about the risks of cement exposure [76].
Allergic Contact Dermatitis
Allergic contact dermatitis associated with cement exposure occurs primarily due to sensitization to hexavalent chromium compounds present in cement [77]. Chromium is widely recognized as one of the most potent allergens encountered in occupational environments and repeated dermal exposure can trigger immune-mediated hypersensitivity reactions [78]. Unlike irritant dermatitis, which results from direct chemical damage, allergic dermatitis develops when the immune system becomes sensitized to chromium ions that penetrate the skin barrier [79]. Once sensitization occurs, even minimal exposure to chromiumcontaining cement can provoke a strong inflammatory response [80]. Workers handling cement without gloves or protective clothing are particularly vulnerable because wet cement facilitates the release and penetration of chromium compounds into the skin [81]. Clinical symptoms often include itching, redness, swelling and eczema-like lesions, which frequently appear on the hands and forearms [82]. Occupational health investigations have shown that chromate sensitivity represents a significant proportion of cementrelated dermatological disorders among construction workers [83].
The long-term consequences of allergic contact dermatitis can be substantial because sensitization to chromium often persists even after exposure has been reduced [84]. Once the immune system becomes sensitized, workers may experience recurring episodes of eczema whenever they come into contact with chromiumcontaining materials [85]. This persistent hypersensitivity can lead to chronic dermatitis characterized by itching, inflammation and scaling of the skin [86]. In some occupational settings, workers who develop severe allergic reactions may need to change their job roles or avoid cement exposure entirely [87]. However, symptoms may still continue due to previous sensitization or accidental exposure to chromium in other materials [88]. Clinical observations indicate that allergic dermatitis can significantly affect the quality of life of affected workers by causing discomfort, sleep disturbances and reduced work performance [89]. Additionally, co-sensitization with other metals such as cobalt has been reported in workers exposed to cement, further complicating the clinical condition [46]. Preventive strategies such as reducing the concentration of hexavalent chromium in cement through chemical treatment have been introduced in some regions to minimize sensitization risk [47].
Cement Burns and Skin Ulceration
Cement burns are severe dermatological injuries that occur when wet cement remains in prolonged contact with the skin, resulting in chemical damage caused by highly alkaline compounds [48]. The hydration of cement generates calcium hydroxide, which produces a strongly alkaline environment capable of damaging skin tissues through chemical corrosion [49]. Workers performing tasks such as kneeling in wet concrete, handling cement mixtures, or working with soaked clothing are particularly susceptible to these injuries [50]. Unlike thermal burns, cement burns develop gradually and may not cause immediate pain, which often leads to delayed recognition of the injury [51]. Initial symptoms typically include mild irritation, redness and a burning sensation that may appear several hours after exposure [52].
If contact continues, alkaline substances penetrate deeper layers of the skin and cause progressive tissue damage [53]. The abrasive properties of cement mixtures, which contain sand and other particulate materials, can also damage the skin surface and facilitate deeper penetration of corrosive chemicals [54]. As a result, the injury can progress from superficial irritation to deeper ulceration [55]. Cement burns therefore represent a serious occupational hazard for construction workers who frequently come into contact with wet concrete during their daily tasks [56]. The clinical progression of cement burns may lead to severe skin damage if exposure is not promptly recognized and treated [57]. Within several hours after exposure, affected areas may develop blisters, inflammation and intense pain [58]. In more severe cases, chemical corrosion may extend into deeper skin layers, producing partial-thickness or full-thickness burns [59]. These injuries often require medical treatment and may result in permanent scarring or loss of skin function [60].
Chronic Skin Conditions in Construction Workers
Chronic dermatological conditions frequently develop among construction workers who experience long-term exposure to cement and related construction materials [61]. Continuous contact with cement dust and wet cement mixtures gradually weakens the skin barrier and reduces its natural protective capacity [62]. As a result, workers often develop persistent dryness, scaling and thickening of the skin after repeated exposure [63]. These conditions commonly appear on the hands and fingers, which are the body parts most frequently exposed during manual construction work [64]. Chronic irritation may stimulate excessive keratin production, resulting in hyperkeratosis characterized by thickened and hardened skin [65]. Although this response may initially act as a protective mechanism, it often leads to painful cracking and fissuring that can interfere with manual work activities [66]. Repeated exposure to cement dust also removes natural oils from the skin surface, contributing to dehydration and roughness [67].
Over time, these changes can lead to persistent dermatological problems that remain present even when acute inflammation subsides [68]. Observational studies summarized in Table 2 indicate that construction workers exposed to cement frequently report chronic dermatological symptoms affecting their hands and forearms [69]. These findings emphasize the cumulative effect of cement exposure on skin health among workers in the construction industry [70]. The long-term impact of chronic dermatological conditions can significantly affect both the health and occupational performance of construction workers [71]. Persistent dryness and cracking of the skin create openings that allow microorganisms to penetrate deeper tissues, increasing the risk of bacterial and fungal infections [72]. Such infections may lead to further inflammation and delayed healing of affected areas [73]. In some cases, workers may develop chronic eczema or other inflammatory skin disorders due to repeated irritation and sensitization [74]. Poor workplace hygiene conditions and limited use of protective equipment can further exacerbate these dermatological problems [75]. Workers employed in cement factories, transportation operations and construction sites therefore face a continuous risk of developing chronic skin conditions associated with cement exposure [76]. The cumulative nature of occupational exposure means that symptoms may worsen with increasing years of employment in the construction sector [77]. Chronic dermatological disorders can also reduce a worker’s ability to perform manual tasks and may lead to reduced productivity or work absence [78]. These outcomes highlight the need for improved occupational health practices, including protective equipment, worker education and regular medical surveillance [79]. Therefore, chronic skin conditions associated with cement exposure represent a significant occupational health challenge in the construction industry [80].
Biochemical and Cellular Effects of Cement Exposure
Cement dust exposure has been widely recognized as a significant occupational health concern due to its complex chemical composition (Figure 1) and potential to induce systemic biochemical disturbances [63]. Cement dust contains several toxic elements including silicon oxide, aluminum oxide, iron oxide, chromium, lead, cadmium, nickel, cobalt, arsenic, sodium, potassium, sulphur and magnesium compounds [60]. These substances can act as environmental xenobiotics that interact with biological tissues after inhalation, ingestion, or dermal contact [68]. Once inhaled, fine cement particles can be trapped in the respiratory tract and subsequently transported through the mucociliary clearance mechanism to the gastrointestinal system, where they may be absorbed into systemic circulation [61]. Following absorption, these toxic constituents can accumulate in various organs such as the liver, kidneys, lungs and gastrointestinal tissues [80]. Bioaccumulation of heavy metals and particulate matter can disrupt normal cellular metabolism and lead to structural and functional damage in multiple organs [66]. Evidence from toxicological studies indicates that these interactions may result in oxidative stress, cellular damage and inflammatory responses that contribute to the development of several diseases including respiratory disorders, liver abnormalities and gastrointestinal dysfunction [72].
Figure 1: Dust generation throughout the different phases of cement manufacturing [57].
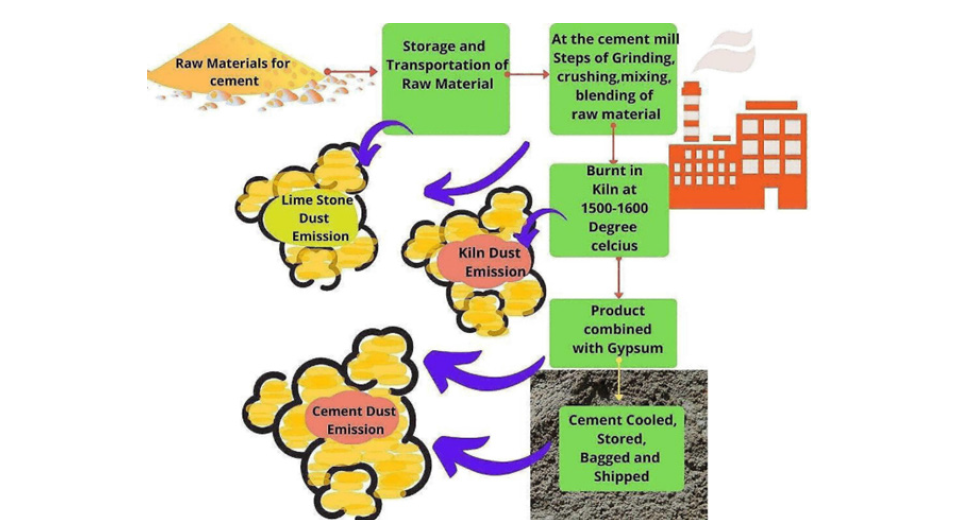
Experimental and epidemiological studies have demonstrated that cement dust exposure can trigger multiple biochemical alterations within the body (Table 3) [64]. Inhalation of cement dust particles has been associated with elevated levels of liver enzymes such as Aspartate Aminotransferase (AST), Alanine Aminotransferase (ALT) and Alkaline Phosphatase (ALP), which indicate hepatic tissue injury [81]. Similarly, increased serum concentrations of creatinine and urea have been reported in exposed individuals, suggesting impaired renal function [71]. These biochemical abnormalities are often accompanied by increased lipid peroxidation and depletion of antioxidant enzymes such as Superoxide Dismutase (SOD) and Catalase (CAT), reflecting oxidative damage at the cellular level [62]. Furthermore, inflammatory markers such as C-reactive protein and nitric oxide have been observed to increase in individuals exposed to cement dust, indicating the activation of immune responses and inflammatory pathways [82]. These findings suggest that prolonged exposure to cement dust can disrupt cellular homeostasis and contribute to tissue degeneration through biochemical and molecular mechanisms [74].
Table 3:Selected case studies on biochemical and cellular effects of cement dust exposure.
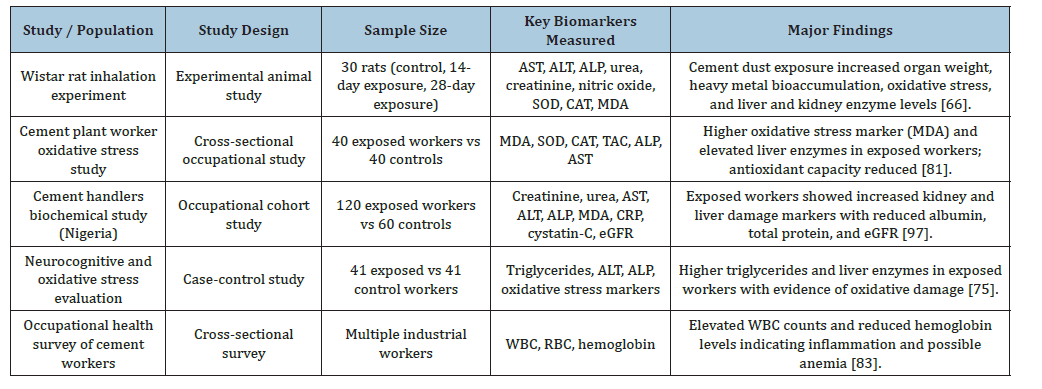
Skin Barrier Disruption
Cement exposure can significantly impair the integrity of the skin barrier, primarily due to its highly alkaline nature and abrasive particulate composition [69]. Wet cement typically has a high pH that can reach levels above 12, which is capable of disrupting the protective lipid layers of the epidermis [83]. The outermost layer of the skin, the stratum corneum, serves as a protective barrier that prevents the entry of harmful substances and regulates water loss [70]. When cement particles come into prolonged contact with the skin, the alkaline compounds dissolve lipids and denature structural proteins within the epidermal layers [84]. This process weakens the protective barrier and increases skin permeability to irritants and allergens [60]. Mechanical abrasion from sand and silica particles further damages the epidermal surface, creating micro-injuries that facilitate deeper penetration of toxic substances [85]. As a result, workers frequently exposed to cement dust often experience dryness, redness, itching and scaling of the skin [75].
Repeated exposure can lead to chronic skin conditions characterized by progressive deterioration of epidermal tissue [86]. The disruption of the skin barrier increases trans epidermal water loss, causing persistent dehydration and reduced elasticity of the skin [77]. In severe cases, prolonged exposure may lead to fissures, ulcerations and inflammatory lesions that compromise normal skin function [87]. Occupational surveys have reported a high prevalence of dermatitis, eczema and skin irritation among cement factory workers and construction laborers [79]. In some cases, these dermatological conditions are aggravated by the presence of heavy metals such as chromium in cement dust, which can induce allergic sensitization [88]. Chronic skin barrier disruption may also allow microbial pathogens to penetrate the damaged epidermis, increasing the risk of secondary infections [80]. These findings highlight the importance of protective measures such as gloves, protective clothing and proper hygiene practices in minimizing dermal exposure to cement dust in occupational environments [89].
Oxidative Stress and Inflammatory Responses
Exposure to cement dust has been shown to induce oxidative stress through the generation of Reactive Oxygen Species (ROS) within cells [81]. The fine particulate nature of cement dust allows it to penetrate deeply into the respiratory tract and enter systemic circulation, where it can interact with cellular components [90]. Once inside the body, toxic metals and particulate matter stimulate the production of ROS such as superoxide radicals and hydrogen peroxide [82]. These reactive molecules can damage cellular membranes, proteins and DNA through oxidative reactions [91]. Lipid peroxidation is one of the primary consequences of oxidative stress, leading to the formation of Malondialdehyde (MDA), a biomarker commonly used to assess oxidative damage [83]. Occupational studies have consistently reported elevated levels of MDA in individuals exposed to cement dust, indicating increased oxidative damage at the cellular level [92]. Simultaneously, antioxidant defense systems such as superoxide dismutase and catalase may become depleted due to prolonged oxidative challenges [84].
The oxidative imbalance caused by cement dust exposure can trigger inflammatory responses in multiple tissues [93]. Reactive oxygen species activate signaling pathways that stimulate immune cells to release inflammatory mediators such as cytokines and nitric oxide [85]. Increased nitric oxide levels have been observed in experimental models exposed to cement dust, suggesting activation of inflammatory processes within organs such as the liver and kidneys [94]. These inflammatory responses may contribute to tissue damage, fibrosis and impaired organ function over time [86]. Elevated levels of inflammatory markers such as C-reactive protein have also been reported among occupationally exposed cement workers [95]. Persistent oxidative stress and inflammation can therefore lead to chronic diseases affecting multiple organs, including the liver, lungs, kidneys and cardiovascular system [87]. These findings demonstrate that oxidative stress plays a central role in the pathophysiological effects of cement dust exposure [96- 100].
Toxicological Effects of Heavy Metals
Heavy metals present in cement dust contribute significantly to its toxicological effects on human health [61]. Elements such as chromium, cadmium, lead, cobalt and nickel are commonly detected in cement dust and can accumulate in biological tissues following prolonged exposure [97]. Among these metals, hexavalent chromium is particularly hazardous due to its strong oxidizing properties and ability to penetrate biological membranes [62]. Once absorbed into the body, chromium compounds can interact with cellular proteins and nucleic acids, leading to structural damage and interference with normal metabolic processes [98]. Toxicological studies have shown that chromium exposure can induce genetic mutations, DNA damage and chromosomal abnormalities, which may increase the risk of cancer [63].
In addition to its carcinogenic potential, chromium exposure can also disrupt immune system function [99]. Chronic exposure to heavy metals may alter the activity of immune cells, including neutrophils and lymphocytes, thereby affecting the body’s ability to respond to infections and inflammatory stimuli [64]. Studies have reported reduced phagocytic activity of polymorphonuclear neutrophils in individuals exposed to cement dust containing high concentrations of cadmium and other metals [100]. This reduction in immune defense can increase susceptibility to infections and inflammatory diseases [65]. Furthermore, bioaccumulation of heavy metals in organs such as the kidneys and liver can lead to long-term toxic effects, including renal dysfunction and hepatic injury [66]. These toxicological mechanisms highlight the significant health risks associated with occupational exposure to cement dust and underscore the need for strict environmental and workplace safety regulations to limit heavy metal exposure [68].
SIRT1-Mediated Effects of Cement
Sirtuin 1 (SIRT1), a NAD⁺-dependent deacetylase, plays a central role in regulating cellular aging, oxidative stress responses and metabolic homeostasis, making it highly relevant in occupational exposure contexts [101]. Cement dust contains a complex mixture of xenobiotics, including alkaline compounds and trace heavy metals such as hexavalent chromium, which can interfere with intracellular signaling pathways and contribute to SIRT1 inactivation [102]. The suppression of SIRT1 activity has been linked to increased production of reactive oxygen species, impaired DNA repair mechanisms and the activation of pro-inflammatory pathways, ultimately accelerating cellular senescence and tissue damage [103]. In construction workers exposed to cement without protective gloves, these molecular disruptions may exacerbate dermatological deterioration while simultaneously promoting systemic toxicity affecting multiple organ systems [104].
Furthermore, the balance between SIRT1 activators and inhibitors is increasingly recognized as a determinant of cellular resilience against environmental stressors, suggesting that occupational exposures may shift this balance toward a pro-aging phenotype [105]. Reduced SIRT1 expression has been associated with metabolic dysregulation, hepatic dysfunction and chronic inflammatory conditions, all of which have been reported in populations exposed to cement dust and related pollutants [101]. Monitoring plasma or tissue levels of SIRT1 in exposed workers may therefore provide an early biomarker for cumulative toxic effects and disease progression [102]. Future research should focus on elucidating dose–response relationships between cementderived xenobiotics and SIRT1 modulation, as well as exploring targeted interventions that could restore its protective functions in high-risk occupational groups [103].
Occupational Health Implications, Preventive Strategies and Future Research Directions
Prolonged exposure to cement, particularly among construction workers who handle it without protective gloves, presents significant occupational health concerns well supported by epidemiological evidence [106]. Occupational dermatosis due to cement exposure is one of the most frequently reported work-related skin disorders globally, with prevalence estimates ranging from 5 to 15 percent of construction workers developing dermatitis during their careers, most commonly among masons and concrete workers [107]. In some hospital-based assessments, nearly 46 percent of construction workers examined exhibited work-related skin diseases such as contact dermatitis and callosities, with contact dermatitis present in nearly 20 percent of cases [108]. Direct dermal contact with cement dust, rich in alkaline compounds and trace heavy metals like hexavalent chromium, can provoke acute irritant reactions, allergic dermatitis, eczema and in severe cases chemical burns and ulceration [109]. Beyond visible dermatological manifestations, emerging evidence from occupational exposure studies indicates systemic biochemical disturbances, including elevated markers of oxidative stress such as malondialdehyde and reduced antioxidant capacity in exposed workers compared with controls, reflecting cellular injury [110]. Such multi-systemic impacts underscore the complexity of cement dust as an occupational hazard that not only compromises immediate health but may predispose workers to long-term chronic conditions [111].
Mitigation of these risks relies on the implementation of comprehensive protective measures that go beyond basic awareness [112]. The consistent use of personal protective equipment, particularly high-quality gloves and protective clothing, remains the most direct barrier against contact with irritants and sensitizing agents and periodic workplace training enhances hazard recognition and compliance [113]. Efforts such as adding ferrous sulfate to cement to reduce chromate sensitization have shown promise in significantly lowering allergic dermatitis incidence, though such interventions are not yet universally adopted [114]. Complementary workplace strategies, including improved ventilation to control airborne dust, substitution of highrisk materials where feasible, routine skin hygiene protocols and health surveillance with targeted biomarker monitoring, further strengthen occupational safety frameworks to minimize both acute and long-term effects [115].
Future research should seek to broaden and deepen our understanding of cement-induced health effects through welldesigned longitudinal and mechanistic studies that integrate both dermatological and systemic outcomes [116]. While cross-sectional studies have documented associations between cement dust exposure and oxidative stress parameters, there remains a need for research that clarifies dose-response relationships, temporal progression of biochemical alterations and the cumulative effects of mixed exposures in construction settings [117]. Investigations into innovative materials, such as bioengineered surface treatments or chromium-reduced cement formulations, could provide transformative occupational safety solutions [118]. Further, elucidating molecular pathways affected by chemical irritants and heavy metals may reveal targeted strategies to counteract toxicity and prevent cellular damage [119]. Finally, socio-economic dimensions, including equitable access to personal protective equipment, training programs and occupational health services across diverse construction environments, must be integrated into future research and policy frameworks to ensure that scientific insights are translated into practical protections for vulnerable worker populations [120].
Conclusion
Cement, a chemically complex and widely used construction material, poses significant occupational hazards for workers, particularly those handling it without proper protective gloves and clothing. The combination of high alkalinity, abrasive particles and sensitizing heavy metals such as hexavalent chromium, cobalt and nickel contributes to both dermatological and systemic health effects. Chronic dermal exposure frequently leads to irritant and allergic contact dermatitis, chemical burns, eczema and hyperkeratosis, with the hands, forearms and lower limbs being the most affected regions. Epidemiological and occupational studies demonstrate the prevalence of these conditions among construction workers, highlighting the need for preventive interventions in workplace settings.
Beyond the visible dermatological effects, cement dust exposure induces substantial biochemical and cellular disturbances. Inhalation, dermal contact or ingestion of fine cement particles allows toxic elements including silicon oxide, aluminum oxide, chromium, cadmium, lead and other heavy metals to accumulate in organs such as the liver, kidneys and lungs, disrupting cellular homeostasis. Prolonged exposure triggers oxidative stress, lipid peroxidation, depletion of antioxidant enzymes such as SOD and CAT and activation of inflammatory pathways, as reflected in elevated liver and kidney enzymes, creatinine, urea, malondialdehyde and C-reactive protein levels. Experimental and occupational studies confirm these biochemical alterations, including oxidative damage and organ dysfunction in both animal models and human workers.
Preventive strategies remain the cornerstone for mitigating cement-related health risks. The consistent use of high-quality gloves, protective clothing, workplace ventilation, hygiene protocols and health surveillance can substantially reduce both acute and chronic adverse effects. Interventions such as the addition of ferrous sulfate to cement to reduce hexavalent chromium content show promise in lowering the incidence of allergic dermatitis, while education and regular training enhance compliance with protective measures. Despite these solutions, gaps remain in adoption and awareness, particularly in developing countries or informal construction sectors, emphasizing the need for stricter occupational safety regulations and effective implementation of protective practices.
Future research should focus on longitudinal and mechanistic studies that evaluate the cumulative effects of cement exposure on dermatological, biochemical and systemic outcomes. Investigations into innovative materials including chromium-reduced cement formulations and bioengineered surface treatments can offer transformative solutions to reduce occupational hazards. Furthermore, integrating socio-economic considerations such as equitable access to protective equipment and health monitoring will be essential to ensure that scientific findings translate into effective protection for construction workers. Taken together, these insights underscore the multi-systemic impact of cement exposure and the critical importance of combining preventive strategies, policy measures and research advancements to safeguard worker health in the construction industry.
Conflict of Interest
The author declares no conflict of interest.
References
- Winder C, Carmody M (2002) The dermal toxicity of cement. Toxicol Ind Health 18(7): 321-331.
- Rauf AU, Mallongi A, Astuti RD (2020) Heavy metal contributions on human skin disease near cement plant: A systematic review. Open Access Macedonian Journal of Medical Sciences 8: 117-122.
- Afridi HI, Kazi TG, Kazi N, Kandhro GA, Baig JA, et al. (2011) Evaluation of cadmium, chromium, nickel and zinc in biological samples of psoriasis patients living in Pakistani cement factory area. Biol Trace Elem Rese 142(3): 284-301.
- Koh DH, Kim TW, Jang SH, Ryu HW (2011) Cancer mortality and incidence in cement industry workers in Korea. Saf Health Work 2(3): 243-249.
- Lushniak BD (2004) Occupational contact dermatitis. Dermatologic Therapy 17(3): 272-277.
- Cha KT, Oh SS, Yoon JH, Lee KH, Kim SK, et al. (2011) Adverse health outcomes in residents exposed to cement dust. Toxicology and Environmental Health Sciences 3: 239-244.
- Thyssen JP, Jensen P, Carlsen BC, Engkilde K, Menné T, et al. (2009) The prevalence of chromium allergy in Denmark is currently increasing as a result of leather exposure. Br J Dermatol 161(6): 1288-1293.
- Sigvardsen NM, Ottosen LM (2019) Characterization of coal bio ash from wood pellets and low-alkali coal fly ash and use as partial cement replacement in mortar. Cement and Concrete Composites 95: 25-32.
- Aljeesh Y, Al Madhoun W, El Jabaly S (2015) Effect of exposure to cement dust on pulmonary function among cement plants workers in the middle governorate, Gaza, Palestine. Public Health Research 5(5): 129-134.
- Spiro J (2008) Occupational skin diseases. Principles and Practice of Skin Toxicology 27(4): 259-277.
- Normohammadi M, Kakooei H, Omidi L, Yari S, Alimi R (2016) Risk assessment of exposure to silica dust in building demolition sites. Saf Health Work 7(3): 251-255.
- Mallongi A, Stang, Syamsuar M, Fajar MN, Pujiastuti RD, et al. (2019) Risks assessment of silica contamination on the communities living surround the cement industry, Pangkep Indonesia. Indian Journal of Public Health Medical Research 10(10): 1619.
- Omrani MA, Modarres A (2018) Emulsified cold recycled mixtures using cement kiln dust and coal waste ash-mechanical and environmental impacts. Journal of Cleaner Production 199: 101-111.
- Thomas B, Kulichova D, Wolf R, Summer B, Mahler V, et al. (2015) High frequency of contact allergy to implant and bone cement components, in particular gentamicin, in cemented arthroplasty with complications: Usefulness of late patch test reading. Contact Dermatitis 73(6): 343-349.
- Stern AH, Bagdon RE, Hazen RE, Marzulli FN (1993) Risk assessment of the allergic dermatitis potential of environmental exposure to hexavalent chromium. J Toxicol Environ Health 40(4): 613-641.
- Hedberg YS, Lidén C, Lindberg M (2016) Chromium dermatitis in a metal worker due to leather gloves and alkaline coolant. Acta Dermato-Venereological 96(1): 104-105.
- Nijhawan RI, Molenda M, Zirwas MJ, Jacob SE (2009) Systemic contact dermatitis. Dermatologic Clinics 27(3): 355-364.
- Achmad RT, Auerkari EI (2017) Effects of chromium on human body. Annual Research and Review in Biology 13(3): 1-8.
- Bermudez GM, Moreno M, Invernizzi R, Plá R, Pignata ML (2010) Heavy metal pollution in topsoils near a cement plant: The role of organic matter and distance to the source to predict total and Hcl-extracted heavy metal concentrations. Chemosphere 78(4): 375-381.
- Elhosary N, Maklad A, Soliman E, El-Ashmawy N, Oreby M (2014) Evaluation of oxidative stress and DNA damage in cement and tannery workers in Egypt. Inhal Toxicol 26(5): 289-298.
- Khatami A, Nassiri-Kashani M, Gorouhi F, Babakoohi S, Kazerouni-Timsar A, et al. (2013) Allergic contact dermatitis to metal allergens in Iran. Int J Dermatol 52(12): 1513-1518.
- Rycroft RJ (2001) Textbook of contact dermatitis. Springer, Berlin, Germany.
- Thyssen JP, Ross-Hansen K, Menné T, Johansen JD (2010) Patch test reactivity to metal allergens following regulatory interventions: A 33-year retrospective study. Contact Dermatitis 63(2): 102-106.
- Wong CC, Gamboni SE, Palmer AM, Nixon RL (2015) Occupational allergic contact dermatitis to chromium from cement: Estimating the size of the problem in Australia. Australas J Dermatol 56(4): 290-293.
- Kowalik T, Logoń D, Maj M, Rybak J, Ubysz A, et al. (2019) Chemical hazards in construction industry. E3S Web of Conferences 97: 03032.
- Bedoya-Marrugo EA, Severiche-Sierra CA, Sierra-Calderon DD, Jaimes-Morales J, Marrugo-Ligardo YA, et al. (2017) Conditions of work and dermatitis in workers exposed to chemical risks by cement. International Journal of Applied Engineering Research 12(22): 12119-12126.
- Chou TC, Wang PC, Wu JD, Sheu SC (2016) Chromium-induced skin damage among Taiwanese cement workers. Toxicol Ind Health 32(10): 1745-1751.
- Saji KG, Zubair M, Varghese PR (2014) Health risk in workers exposed to wet cement. International Journal of Research 4(5): 2307-2083.
- Nunes RA, De Alencar DB, Bezerra CM, Bezerra IFO (2019) Health damage to civil construction workers due to use and exposure to cement. ITEGAM-JETIA 5(20): 116-120.
- Shanshal SA, Al-Qazaz HK (2022) The impact of exposure to cement dust on the parameters of oxidative stress among cement plant workers. Global Journal of Public Health Medicine 4(1): 570-578.
- Abdel-Hamid IA, Agha SA, Moustafa YM, El-Labban AM (2003) Pityriasis amiantacea: A clinical and etiopathologic study of 85 patients. Int J Dermatol 42(4): 260-264.
- Afridi HI, Brabazon D, Kazi TG, Naher S, Nesterenko E (2011) Evaluation of essential trace and toxic elements in scalp hair samples of smokers and alcohol user hypertensive patients. Biol Trace Elem Res 143(3): 1349-1366.
- Ala S, Shokrzadeh M, Golpour M, Salehifar E, Alami M, et al. (2013) Zinc and copper levels in Iranian patients with psoriasis: A case control study. Biol Trace Elem Resh 153(1-3): 22-27.
- Arora PN, Dhillon KS, Rajan SR, Sayal SK, Das AL (2002) Serum zinc levels in cutaneous disorders. Med J Armed Forces India 58(4): 304-306.
- Basavaraj K, Darshan M, Shanmugavelu P, Rashmi R, Mhatre AY, et al. (2009) Study on the levels of trace elements in mild and severe psoriasis. Clin Chim Acta 405(1-2): 66-70.
- Brown KM, Arthur JR (2001) Selenium, selenoproteins and human health: A review. Public Health Nutr 4(2B): 593-599.
- Chen W, Zhou X, Zhu W (2019) Trace elements homeostatic imbalance in psoriasis: A meta-analysis. Biol Trace Elem Res 191(2): 313-322.
- Elder JT, Nair RP, Henseler T, Jenisch S, Stuart P, et al. (2001) The genetics of psoriasis 2001: The odyssey continues. Arch Dermatol 137(11): 1447-1454.
- Gelfand JM, Weinstein R, Porter SB, Neimann AL, Berlin JA, et al. (2005) Prevalence and treatment of psoriasis in the United Kingdom: A population-based study. Arch Dermatol 141(12): 1537-1541.
- Ginarte M, Pereiro M, Fernandez-Redondo V, Toribio J (2000) Pityriasis amiantacea as manifestation of tinea capitis due to microsporum canis. Mycoses 43(1-2): 93-96.
- Hanel KH, Cornelissen C, Luscher B, Baron JM (2013) Cytokines and the skin barrier. International Journal of Molecular Sciences 14(4): 6720-6745.
- Kim JE, Yoo SR, Jeong MG, Ko JY, Ro YS (2014) Hair zinc levels and the efficacy of oral zinc supplementation in children with atopic dermatitis. Acta Dermato-Venereologica 94: 558-562.
- Kolachi NF, Kazi TG, Baig JA, Kandhro GA, Khan S, et al. (2010) Microwave assisted acid extraction of selenium from medicinal plants followed by electrothermal atomic absorption spectrometric determination. J AOAC Int 93(2): 694-702.
- Kolachi NF, Kazi TG, Afridi HI, Kazi N, Kandhro GA, et al. (2011) Distribution of Copper, iron and zinc in biological samples (scalp hair, serum, blood and urine) of Pakistani viral hepatitis (A-E) patients and controls. Biol Trace Elem Res 143(1): 116-130.
- Lin PH, Matthew S, Li H, Lee PH, Steinberg SM, et al. (2018) Zinc in wound healing modulation. Nutrients 10(1): 16.
- McKenzie RC (2000) Selenium, ultraviolet radiation and the skin. Clin Exp Dermatol 25(8): 631-636.
- Mohamad NS (2013) Trace elements homeostatic imbalance in mild and severe psoriasis: A new insight in biomarker diagnostic value for psoriasis. Our Dermatology Online 4(4): 449-452.
- Naziroglu M, Yildiz K, Tamturk B, Erturan I, Flores-Arce M (2012) Selenium and psoriasis. Biol Trace Elem Res 150(1-3): 3-9.
- Park K (2015) Role of micronutrients in skin health and function. Biomol Ther 23(3): 207-217.
- Pisoschi AM, Pop A (2015) The role of antioxidants in the chemistry of oxidative stress: A review. Eur J Med Chem 97: 55-74.
- Rayman MP (2008) Food-chain selenium and human health: Emphasis on intake. Br J Nutr 100(2): 254-268.
- Rayman MP (2012) Selenium and human health. Lancet 379(9822): 1256-1268.
- Rostan EF, DeBuys HV, Madey DL, Pinnell SR (2002) Evidence supporting zinc as an important antioxidant for skin. Int J Dermatol 41(9): 606-611.
- Salgueiro MJ, Zubillaga M, Lysionek A, Sarabia MI, Caro R, et al. (2000) Zinc as an essential micronutrient: A review. Nutrition Research 20(5): 737-755.
- Samejo S, Kazi AG, Afridi HI, Kazi TG (2019) Evaluate the effect of cadmium on levels of zinc in scalp hair and blood samples of smoker and nonsmoker psoriatic patients at different stage. Environ Sci Pollut Res int 26(31): 31763-31769.
- Schwart JR, Marsh RG, Draelos ZD (2005) Zinc and skin health: Overview of physiology and pharmacology. Dermatol Surg 31(7 Pt 2): 837-847.
- Serwin AB, Wasowicz W, Gromadzinska J, Chodynicka B (2003) selenium status in psoriasis and its relations to the duration and severity of the disease. Nutrition 19(4): 301-304.
- Shahidi DM, Namazi N, Khalilazar S, Younespour S (2012) Trace elements status in psoriasis and their relationship with the severity of the disease. Iranian Journal of Dermatology 15: 38-41.
- Shahrad MB, Behnam SE, Koo JY (2005) Smoking and psoriasis. SKINmed 4: 174-176.
- Stehbens WE (2003) Oxidative stress, toxic hepatitis and antioxidants with particular emphasis on zinc. Exp Mol Pathol 75(3): 265-276.
- Stewart MS, Spallholz JE, Neldner KH, Pence BC (1999) Selenium compounds have disparate abilities to impose oxidative stress and induce apoptosis. Free Radic Biol Med 26(1-2): 42-48.
- Tisma VS, Basta-Juzbasic A, Jaganjac M, Brcic L, Dobric I, et al. (2009) Oxidative stress and ferritin expression in the skin of patients with rosacea. J Am Acad Dermatol 60(2): 270-276.
- Trouba KJ, Hamadeh HK, Amin RP, Germolec DR (2002) Oxidative stress and its role in skin disease. Antioxid Redox Signal 4(4): 665-673.
- Verardino GC, Azulay-Abulafia L, Macedo PM, Jeunon T (2012) Pityriasis amiantacea: Clinical-dermatoscopic features and microscopy of hair tufts. An Bras Dermatol 87(1): 142-145.
- Wolff K, Goldsmith LA, Katz SI, Gilcherest BA, Paller AS, et al. (2008) Fitzpatrick’s Dermatology in General Medicine. (7th edn), McGraw-Hill Medical, New York, USA.
- Yang L, Wang W, Hou S, Peterson PJ, Williams WP (2002) Effects of selenium supplementation on arsenism: An intervention trial in inner mongolia. Environmental Geochemistry and Health 24: 359-374.
- Yildirim M, Inaloz HS, Baysal V, Delibas N (2003) The role of oxidants and antioxidants in psoriasis. J Eur Acad Dermatol Venereol 17(1): 34-36.
- Zhou Q, Mrowietz U, Yazdi MR (2009) Oxidative stress in the pathogenesis of psoriasis. Free Radic Biol Med 47(7): 891-905.
- Zoidis E, Seremelis I, Kontopoulos N, Danezis GP (2018) Selenium-dependent antioxidant enzymes: Actions and properties of selenoproteins. Antioxidants 7(5): 66.
- Kridin K, Bergman R, Khamaisi M, Zelber-Sagi S, Weltfriend S (2016) Cement-induced chromate occupational allergic contact dermatitis. Dermatitis 27(4): 208-214.
- Saji KG, Zubair M, Nair SB, Varghese PR (2018) An epidemiological study on effect of occupational exposure of cement. International Journal of Community Medicine and Public Health 5: 5105-5109.
- Kazi AG, Afridi HI, Arain MB, Kazi TG (2021) Adverse impact of occupational exposure on laborers of cement industry have scalp psoriasis and pityriasis amiantacea with deficiency of zinc and selenium: Impact of mineral supplement. Environ Sci Pollut Res Int 28(48): 68330-68337.
- Abrams K, Harvell JD, Shriner D, Wertz P, Maibach H, et al. (1993) Effect of organic solvents on in vitro human skin water barrier function. J Invest Dermatol 101(4): 609-613.
- American Conference of Governmental Industrial Hygienists (ACGIH) (2005) Threshold limit values for chemical substances and physical agents and biological exposure indices. ACGIH, Cincinnati, Ohio.
- Avnstorp C (1992) Cement eczema: An epidemiological intervention study. Acta Derm Venereol Suppl 179: 1-22.
- Brown CP, Spivey GH, Valentine JL, Browdy BL (1980) Cigarette smoking and lead levels in occupationally exposed lead workers. J Toxicol Environ Health 6(4): 877-883.
- Bock M, Schmidt A, Bruckner T, Diepgen TL (2003) Occupational skin disease in the construction industry. Br J Dermatol 149(6): 1165-1171.
- Boyd AS, Stasko T, King LE, Cameron GS, Pearse AD, et al. (1999) Cigarette smoking-associated elastotic changes in the skin. J Am Acad Dermatol 41(1): 23-26.
- Chen CJ, Shih TS, Chang HY, Yu HS, Wu JD, et al. (2008) The total body burden of chromium associated with skin disease and smoking among cement workers. Sci Total Environ 391(1): 76-81.
- Chou TC, Shih TS, Sheu HM, Chang SJ, Huang CC, et al. (2004) The effect of personal factors on the relationship between carbon disulfide exposure and urinary 2-thiothiazolidine-4-carboxylic acid levels in rayon manufacturing workers. Sci Total Environ 322(1-3): 51-62.
- Chou TC, Shih TS, Tsai JC, Wu JD, Sheu HM, et al. (2004) Effect of occupational exposure to rayon manufacturing chemicals on skin barrier to evaporative water loss. J Occup Health 46(5): 410-417.
- Chou TC, Chang HY, Chen CJ, Yu HS, Wu JD, et al. (2008) Effect of hand dermatitis on the total body burden of chromium after ferrous sulfate application in cement among cement workers. Contact Dermatitis 59(3): 151-156.
- Chuong CM, Nickoloff BJ, Elias PM, Goldsmith LA, Macher E, et al. (2002) What is the ‘true’ function of skin? Viewpoint 1. Exp Dermatol 11(2): 159-187.
- Elias PM (2005) Stratum corneum defensive functions: An integrated view. J Invest Dermatol 125(2): 183-200.
- Ernster VL, Grady D, Miike R, Black D, Selby J, et al. (1995) Facial wrinkling in men and women, by smoking status. Am J Public Health 85(1): 78-82.
- Fowler JF, Kauffman CL, Marks JG, Proctor DM, Fredrick MM, et al. (1999) An environmental hazard assessment of low-level dermal exposure to hexavalent chromium in solution among chromium-sensitized volunteers. J Occup Environ Med 41(3): 150-160.
- Freiman A, Bird G, Metelitsa AI, Barankin B, Lauzon GJ (2004) Cutaneous effects of smoking. J Cutan Med Surg 8(6): 415-423.
- Gammelgaard B, Fullerton A, Avnstorp C, Menne T (1992) Permeation of chromium salts through human skin in vitro. Contact Dermatitis 27(5): 302-310.
- Hui X, Elkeeb R, Chan H, Maibach HI (2012) Ability to estimate relative percutaneous penetration via surrogate marker-Transepidermal water loss? Skin Res Technol 18(1): 108-113.
- Machado M, Salgado TM, Hadgraft J, Lane ME (2010) The relationship between transepidermal water loss and skin permeability. Int J Pharm 384(1-2): 73-77.
- Morita A (2007) Tobacco smoke causes premature skin aging. J Dermatol Sci 48(3): 169-175.
- Pflücker F, Wendel V, Hohenberg H, Gartner E, Will T, et al. (2001) The human stratum corneum layer: An effective barrier against dermal uptake of different forms of topically applied micronised titanium dioxide. Skin Pharmacol Appl Skin Physiol 14: 92-97.
- Pinnagoda J, Tupker RA (1995) Measurement of the transepidermal water loss. In: Serup J, Jemec GB (Eds.), Handbook of Non-Invasive Methods and the Skin. CRC Press, Boca Raton, Florida, USA, pp. 173-178.
- Rougier A, Dupuis D, Lotte C, Roguet R, Wester RC, et al. (1986) Regional variation in percutaneous absorption in man: Measurement by the stripping method. Arch Dermatol Res 278(6): 465-469.
- Roberts MS, Walters KA (1998) The relationship between structure and barrier function of skin. In: Roberts MS, Walters KA (Eds.), Dermal Absorption and Toxicity Assessment. Marcel Dekker, New York, USA, pp. 1-42.
- Rubio L, Alonso C, Lopez O, Rodriguez G, Coderch L, et al. (2011) Barrier function of intact and impaired skin: Percutaneous penetration of caffeine and salicylic acid. Int J Dermatol 50(7): 881-889.
- Shelnutt SR, Goad P, Belsito DV (2007) Dermatological toxicity of hexavalent chromium. Crit Rev Toxicol 37(5): 375-387.
- Stern AH, Bagdon RE, Hazen RE, Marzulli FN (1993) Risk assessment of the allergic dermatitis potential of environmental exposure to hexavalent chromium. J Toxicol Environ Health 40(4): 613-641.
- Tsai JC, Hung PL, Sheu HM (2001) Molecular weight dependence of polyethylene glycol penetration across acetone-disrupted permeability barrier. Arch Dermatol Res 293(6): 302-307.
- Tsai JC, Sheu HM, Hung PL, Cheng CL (2001) Effect of barrier disruption by acetone treatment on the permeability of compounds with various lipophilicities: implications for the permeability of compromised skin. J Pharm Sci 90(9): 1242-1254.
- Zhou Q, Chen W, Gu C, Liu H, Hu X, et al. (2023) Selenium-modified bone cement promotes osteoporotic bone defect repair in ovariectomized rats by restoring Gpx1-mediated mitochondrial antioxidant functions. Regen Biomater 10: rbad011.
- Li Y, Zhang W, Cai Y, Yang D (2025) Ginsenoside Rb2 inhibits the pyroptosis in myocardial ischemia progression through regulating the SIRT1-mediated deacetylation of ASC. Biochem Genet 63(3): 2623-2637.
- Wang J, Lin J, Liu L, Liu S, Xie Z, et al. (2026) Ciprofol promotes SIRT1-mediated raf regulation of ERK1/2 hyperphosphorylation. Neurochem Res 51(1): 62.
- She P, Mo F, Zhu P, Zhong TP (2026) Regulation of mitochondrial biogenesis and energy metabolism in the heart. Chin Med J.
- Zhang C, Sun R, Jiang Q (2026) Establishment and research progress of animal models for intervertebral disc degeneration. Open Life Sci 21(1): 20251295.
- Ulenbelt P, Lumens ME, Géron HM, Herber RF, Broersen S, et al. (1990) Work hygienic behaviour as modifier of the lead air-lead blood relation. Int Arch Occup Environ Health 62(3): 203-207.
- Wang BJ, Wu JD, Sheu SC, Shih TS, Chang HY, et al. (2011) Occupational hand dermatitis among cement workers in Taiwan. J Formos Med Assoc 110(12): 775-779.
- Wen CP, Levy DT, Cheng TY, Hsu CC, Tsai SP (2005) Smoking behaviour in Taiwan, 2001. Tob Control 14: I51-I55.
- Yosipovitch G, Xiong GL, Haus E, Lundeen LS, Ashkenazi I, et al. (1998) Time-dependent variations of the skin barrier function in humans: Transepidermal water loss, stratum corneum hydration, skin Surface pH and skin temperature. J Invest Dermatol 110(1): 20-23.
- Zhai H, Leow YH, Maibach HI (1998) Human barrier recovery after acute acetone perturbation: An irritant dermatitis model. Clin Exp Dermatol 23(1): 11-13.
- Keram SP, Deshmukh GD (2025) Bioaccumulation of trace elements exposed to pollution from ultratech cement factory area near Gadchandur, Maharashtra, India. Biochemical & Cellular 25(2): 2041-2048.
- Magnano GC, Malard V, Crosera M, Marussi G, Debellemanière O, et al. (2025) Evaluation of metal removal from skin exposed to stainless steel and cement particles: Insights from an in vitro permeation study. Toxicol in Vitro 111: 106173.
- Alabi OA, Ayeni FE, Afolabi TA (2025) health risk assessment of toxic metals and DNA damage in somatic and germ cells by soil and groundwater of a major cement factory in Nigeria. Toxicol Sci 203(2): 227-241.
- Islam MM, Akhter S, Khanam S, Nasrin T, Gupta AD, et al. (2025) Effect of cement pollution on serum creatinine and blood urea in cement factory workers. Chattagram Maa-O-Shishu Hospital Medical College Journal 24(2): 86-90.
- Helen OA, Temilade TA, Olwapelumi OE, Ebun AB, Olatunbosun AF, et al. (2025) Effects of cement dust exposure on liver function among construction workers in akala express. International Research Journal of Gastroenterology and Hepatology 8(1): 28-39.
- Ahmad R, Haque M, Abira M, Akhter QS (2026) Hepatic effects of chronic occupational cement dust exposure: Enzyme profile analysis. Bangladesh Journal of Medical Science 25(1): 91-102.
- Piemonte ED, Panico R, Gilligan GM, Lazos JP (2026) Effects of chronic sun exposure on the labial mucosa. Lifestyle in Oral Health and Disease 293-327.
- Aulia NS, Charisma N, Laoli VT, Nasirah T, Salsabila AP, et al. (2026) Risk control of exposure to hazardous chemicals in the workplace. International Conference of Public Health 352-362.
- McKay RL, Wu S (2026) Blue light and ultraviolet radiation: Comparative biophysical properties and their roles in skin carcinogenesis and photoaging. J Derm Oncol 2(1): 2595383.
- Liao Z, Parumasivam T, Xiao Z, Zhu X, Yeoh YK, et al. (2026) Emerging therapeutic and cosmeceutical applications of phenylalanine and its metabolites. Cutan Ocul Toxicol 45(1): 1-18.
© 2025 Zeenat Khan. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






