- Submissions

Full Text
Degenerative Intellectual & Developmental Disabilities
Case Report on the Management of Multiple Organ Failure Following Ruptured Cerebral Aneurysm
Mengling Chang1, Fenglin Zhang2 and Jianchu Lin3*
1The Affiliated Huai’an No. 1 People’s Hospital of Nanjing Medical University, China
2The Second People’s Hospital of Huai’an/The Affiliated Huai’an Hospital of Xuzhou Medical University, China
3Huai’an University, Faculty of Computer and Software Engineering, China
*Corresponding author: Jianchu Lin, Huai’an University, Faculty of Computer and Software Engineering, 223003, Huai’an, China
Submission: March 28, 2026; Published: April 21, 2026

Volume2 Issue 3April 21, 2026
Abstract
Objective: To review the diagnosis and treatment of patients with multiple organ failure after cerebral
aneurysm surgery, and to provide a reference for further improving clinical practice.
Methods: The clinical data of a 52-year-old female patient were retrospectively analyzed, summarizing the
process from emergency admission, interventional surgery, occurrence of postoperative complications,
multidisciplinary collaborative treatment to recovery and discharge.
Result: After interventional therapy and active management of related complications, the patient
regained consciousness, achieved stable respiration and circulation, and was discharged in improved
condition.
Conclusion: Multiple organ failure after ruptured aneurysm surgery is complex and critical, requiring
multidisciplinary collaboration and timely surgical intervention. Electroencephalogram and braincomputer
interface can help evaluate the patient’s condition and improve prognosis.
Keywords:Posterior communicating artery aneurysm; Subarachnoid hemorrhage; Multiple organ failure; Electroencephalogram; Brain-computer interface
Introduction
Intracranial aneurysm is a pathological dilation formed by local weakness of the intracranial arterial wall. After rupture, it can cause Subarachnoid Hemorrhage (SAH), which is the main cause of SAH, accounting for 80% [1]. It is highly likely to result in death or disability. This report retrospectively reviews the diagnosis and treatment of a patient with ruptured right posterior communicating artery aneurysm complicated with SAH and postoperative multiple organ failure, to provide a reference for clinical practice.
Case Data
A 52-year-old female patient was admitted to the emergency department of our hospital on August 25, 2025, due to “sudden unconsciousness for 3 hours”. Emergency imaging examinations were performed, followed by tracheal intubation. She was then admitted to the Department of Neurosurgery for emergency surgery. A series of complications occurred during the course of the disease. With multidisciplinary collaboration, the patient finally recovered and was discharged. The relevant diagnosis and treatment process are shown in Table 1.
Table 1:Timeline of clinical course, interventions, and outcomes.
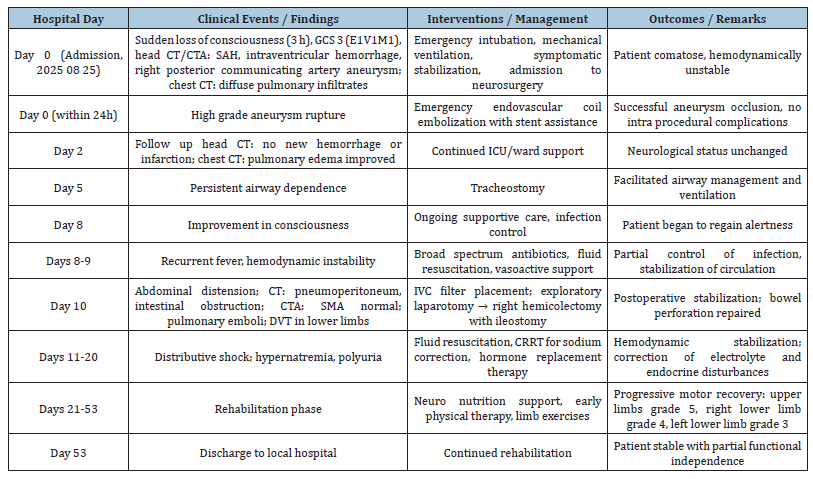
Discussion
Primary disease
The patient had a right posterior communicating artery aneurysm with a Glasgow Coma Scale (GCS) score of 3 on admission. Surgical timing was strictly controlled, and endovascular embolization was performed within 24 hours after admission, resulting in initial postoperative improvement. The patient was classified as Hunt-Hess grade was grade V. Relevant clinical studies have shown that the in-hospital mortality of such patients is as high as 71% [2]. These studies indicate that reducing early brain injury and rebleeding of aneurysms after SAH, as well as preventing and treating complications, can further lower the mortality after SAH. Current surgical treatments for ruptured intracranial aneurysms include craniotomy, endovascular treatment, and hybrid surgery. For aneurysmal SAH, the optimal treatment timing is within 24 hours after onset; early surgery helps improve prognosis. For patients with internal carotid artery and posterior communicating artery aneurysms, endovascular embolization yields better outcomes [3].
Complications
The patient developed infectious complications such as pneumonia and sepsis during the course of the disease. The infection was controlled after active treatment, but recurrent fever persisted. Further hormonal examinations suggested hypothalamic insufficiency. Such patients often present with systemic inflammatory response syndrome, so it is necessary to distinguish infectious from non-infectious causes [3]. Vascular ultrasound after cerebral hemorrhage showed venous thrombosis in multiple parts of both lower extremities, and an inferior vena cava filter was implanted. The incidence of Venous Thromboembolism (VTE) is high in such patients. The safety and efficacy of pharmacological prophylaxis for VTE have been verified by clinical trials. Early pharmacological thromboprophylaxis [4] may be safe in patients with ruptured aneurysms or diffuse SAH with negative angiography. Delayed cerebral ischemia and cerebral vasospasm are also common complications of aneurysmal SAH. The patient underwent regular imaging re-examinations, showing no new cerebral infarction. Relevant imaging examinations [5] include DSA, CTA, CTP, and magnetic resonance angiography for diagnosis and evaluation. The patient developed significant hormonal disorders during the course, considered to be related to catecholamine storm after SAH [6], leading to paralytic ileus, intestinal ischemia, and intestinal perforation. After early active surgical intervention by gastrointestinal surgery, combined with anti-infection, anti-shock, and nutritional support treatments, the patient’s vital signs finally stabilized.
Prognosis
Rehabilitation plays a crucial role in promoting functional recovery and improving overall prognosis. Previous studies have confirmed that early rehabilitation is both safe and effective, and that higher-intensity activity is not associated with postoperative complications [7]. Long-term rehabilitation should also focus on the patient’s psychological, cognitive, and mental status [3]. Multidisciplinary team-based treatment and rehabilitation can shorten hospital stay and improve prognosis [8]. Although the patient recovered and was discharged, there is still room for improvement in the diagnosis and treatment process.
Assessment and monitoring of consciousness disturbance
Clinically, impaired consciousness is often assessed using bedside neurological examination. Electroencephalogram (EEG) is a non-invasive method for monitoring cortical electrical activity and an important tool for clinicians to evaluate the consciousness status of patients with disturbance. It reflects dynamic changes and functional alterations of subtle brain structures by recording postsynaptic potentials of cortical neurons, determines the integrity of the corticothalamic pathway to assess brain injury, and detects abnormal brain function that cannot be demonstrated by CT or MRI. The severity of EEG abnormalities is also well correlated with GCS score and prognosis [9], so it can help further evaluate the patient’s condition both pre- and postoperatively. Noninvasive EEG-based Brain-Computer Interface (BCI) has also been applied clinically. BCI establishes a novel signal pathway between the brain and computers or other electronic devices to achieve brain-machine control. It assists in examining and diagnosing the consciousness status of critically ill patients, helps patients with damaged neural pathways communicate with the outside world, and may even become the only communication method for those with consciousness disturbance [10]. Through BCI, the accuracy of voluntarily generated EEG signals during rehabilitation training can be monitored, enabling precise active regulation. Indirect modulation enhances rehabilitation signals to achieve neural remodeling in target areas and functional recovery.
Doctor-patient communication and ethics
Unexpectedly, the family filed a medical complaint after the patient’s discharge. The family believed that severe complications resulted from improper medical management, leading to prolonged hospitalization, increased financial burden, and physical and psychological harm. Reviewing the overall treatment, the patient’s condition was extremely critical with an extremely high theoretical mortality risk, complicated with pulmonary edema. Statistics show that the mortality of SAH patients complicated with pulmonary edema is nearly twice that of those without pulmonary edema (40.2% vs. 22.5%) [11]. The Department of Neurosurgery, Intensive Care Unit, and Gastrointestinal Surgery of our hospital actively treated the primary disease and complications sequentially according to the characteristics and progression of the disease, and the patient finally turned the corner. We not only successfully saved her life but also restored her ability of self-care. Overall, the treatment was reasonable and appropriate, and the outcome far exceeded theoretical expectations [12]. Although we repeatedly communicated the condition with the family during hospitalization, the critical illness placed huge psychological and financial pressure on them, which easily triggers doctor-patient conflicts.
Conclusion
Multiple organ failure after ruptured aneurysm surgery is complex and critical. Successful treatment requires multidisciplinary collaboration, precise anti-infection, timely surgical intervention, and continuous organ support. EEG can evaluate disease severity, and BCI can accurately guide early rehabilitation to improve prognosis. The treatment should not only be rational but also strengthen doctor-patient communication, ensure the patient’s full understanding of disease severity and medical costs, reduce financial burden, and provide humanistic care to minimize the risk of medical disputes.
References
- Neifert SN, Chapman EK, Martini ML, William HS, Alexander JS, et al. (2021) Aneurysmal subarachnoid hemorrhage: The last decade. Transl Stroke Res 12(3): 428-446.
- Lantigua H, Ortega-Gutierrez S, Schmidt JM, Kiwon L, Neeraj B, et al. (2015) Subarachnoid hemorrhage: Who dies and why. Crit Care 19(1): 309.
- Society of Neurosurgery of Chinese Medical Association, Society of Cerebrovascular Surgery of Chinese Stroke Association, National Center for Neurological Disorders, National Clinical Research Center for Neurological Diseases (2024) Chinese guideline for the clinical management of patients with ruptured intracranial aneurysms (2024). Zhonghua Yi Xue Za Zhi 104(21): 1940-1971.
- Manoel AL, Turkel-Parrella D, Germans M, Ekaterina K, Priscila SA, et al. (2014) Safety of early pharmacological thromboprophylaxis after subarachnoid hemorrhage. Can J Neurol Sci 41(5): 554-561.
- Smith NM, Sweeney EM, Gupta A, Athos P, Pina S, et al. (2022) Diagnostic accuracy of shuttle CT angiography (CTA) and helical CTA in the diagnosis of vasospasm. Clin Imaging 81: 37-42.
- Inamasu J, Moriya S, Oheda M, Yuichi H (2015) Role of catecholamines in acute hypertensive response: Subarachnoid hemorrhage versus spontaneous intracerebral hemorrhage. Blood Press Monit 20(3): 132-137.
- Karic T, Røe C, Nordenmark TH (2017) Effect of early mobilization and rehabilitation on complications in aneurysmal subarachnoid hemorrhage. J Neurosurg 126(2): 518-526.
- Nussbaum ES, Mikoff N, Paranjape GS (2021) Cognitive deficits among patients surviving aneurysmal subarachnoid hemorrhage: A contemporary systematic review. Br J Neurosurg 35(4): 384-401.
- Qu N, Zhang GL (2024) Research progress of electroencephalogram monitoring in patients with consciousness disturbance after brain injury. Chinese Journal of Integrative Medicine on Cardio-Cerebrovascular Disease 22(19): 3570-3573.
- Fu JY, Wang LP (2021) Clinical application progress of non-invasive brain-computer interface based on electroencephalogram. Medical Recapitulate 27(23): 4694-4699.
- Pando A, Tenneli AK, Pradeep T, Priyanka A, Balamurali K, et al. (2025) Acute pulmonary edema after subarachnoid hemorrhage: Risk factors and comorbidities-an analysis of a nationwide database from the United States. J Intensive Care 13(1): 25.
- Guo M, Li BJ, Mei LP (2024) Analysis of the correlation between Hunt-Hess classification and complications and dysfunction in patients with aneurysmal subarachnoid hemorrhage. Neural Injury and Functional Reconstruction 19(4): 217-221.
© 2026 Jianchu Lin. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






