- Submissions

Full Text
Degenerative Intellectual & Developmental Disabilities
Effects of a Multi-Component Exercise Program on Physical Activity, Cardiorespiratory Fitness, Self-Efficacy and Social Support of Adults with Intellectual Disabilities Living in Group Homes
Bik C Chow1, Peggy HN Choi2* and Chien-Yu Pan3
1Department of Sports and Health Sciences, Hong Kong Baptist University, Hong Kong
2Department of Sport and Recreation, Technological and Higher Education Institute of Hong Kong, Hong Kong
3Department of Physical Education, National Kaohsiung Normal University, Taiwan
*Corresponding author: Peggy HN Choi, Department of Sport and Recreation, Technological and Higher Education Institute of Hong Kong, Hong Kong
Submission: February 25, 2026; Published: March 12, 2026

Volume2 Issue2 March 12, 2026
Abstract
The purpose of the study was to examine the effect of a multi-component exercise program on Physical Activity (PA), aerobic fitness, self-efficacy and social support of adults with Intellectual Disabilities (ID) living in Group Homes (GHs). Participants were fifty-nine adults with ID from two GHs. A GH was assigned to be either the Experimental Group (EG) or Wait-List Control Group (WLG). Participants of the EG received group exercise 3 days per week for 10 weeks and 3 educational talks. Participants of the WLG received intervention in the 11th week. Study outcomes included baseline, postintervention and 10-week follow-up measures of accelerometry, Six Minutes’ Walk Test (6MWT), self-efficacy and social support. Analyses of all intervention participants showed a significant increase in light PA and decrease in Sedentary Behavior (SB) in the postintervention with no differences in the 10-week follow-up as compared to baseline. Participants had a significant drop in the 6MWT in the follow-up and perceived lower social-support from staff in the postintervention as compared to baseline. The findings show that the exercise program is effective for adults with ID to increase LPA and reduce SB but is ineffective on moderate-intensity PA, aerobic fitness and self-efficacy.
Keywords:Intellectual disabilities; Six minutes’ walk test; GHs; Sedentary behavior; PA; Aerobic fitness
Introduction
Intellectual Disability (ID) is defined as a disorder with onset before the age of 18 years with significant limitations in adaptive behavior and intellectual functioning [1] and persons with ID have difficulty in performing daily activities independently. In Hong Kong, the estimation of people with ID is about 67,000 to 80,000 [2], which is 1%-1.4% of the population. This prevalence rate is similar to high-income countries of 0.9% [3]. This population includes subgroups such as Down syndrome, cerebral palsy and autism spectrum disorders and they have significant health deficits associated with disease-specific conditions. Overall, people with ID are more likely to have risk of health complications with shorter life expectancy and increased morbidity than the general population. Nevertheless, the health disparities between these individuals and the general population become larger when the lifespans of people with ID have increased, resulting in a greater health burden on health care services. Adults with ID are often physically inactive. The sedentariness lifestyle of this population is particularly prominent as evidenced by a recent systematic review. [4] reported that 91% of the participants with ID in the 15 studies could not fulfill the global physical activity recommendation of 150 minutes weekly of Moderate-To-Vigorous Physical Activity (MVPA). Due to their physical inactivity, adults with ID tend to have lower fitness levels and higher obesity rates which lead to increased risk of overall mortality and morbidity [3]. Exercise is one of the health promotion interventions that has been recognized as an effective means to increase fitness of individuals with ID [5,6]. On the other hand, recent reviewer indicated no conclusive findings for increasing activity levels by PA intervention for adults with ID [7,8] or improving body composition by either aerobic exercise or muscular fitness programs [6]. Although researchers have advocated tailor-made PA programs targeted at this special population [9,10], very few PA interventions have been offered to adults with ID in Asian countries. A recent review of PA interventions for individuals with ID using Randomized Controlled Trials (RCTs) included nine studies, none of them were conducted in Asia [7]. When searching studies that included non-RCTs, reviewers [6] reported 44 studies about the effects of exercise on the physical fitness levels of adults with ID out of which only 3 were conducted in Asian countries (2 from Korea, 1 from Taiwan).
In studies examining exercise programs for adults with ID, Social Cognitive Theory (SCT) has been the most adopted theoretical basis [11]. SCT considers human behavior as a result of dynamic interaction between individual, behavioral and environmental influences [12]. Self-efficacy, being the most important construct of SCT found in the PA literature [13], is the confidence that one has in control over one’s health [12]. In SCT, social support is one of the social factors influencing physical activity behavior in which it can mediate the influence of self-efficacy on behavior [14]. Researchers found self-efficacy and social support predicted PA participation in adults with mild and moderate ID receiving supported-living [15]. In PA intervention studies, there were positive changes in selfefficacy with the provision of social support [16,17]. Hong Kong is a highly urbanized and densely-populated modern city. Currently, there are 1,745 places in 44 group homes offering 24 hours care (ranged from 20 to 108 resident places) for Hong Kong adults of mild-grade and moderate-grade ID (Social Welfare Department). Hence, the mean number of residents per home exceeds 50, as opposed to 4 to 8 residents in a licensed home in western countries [18]. In view of the unique group home setting for adults with ID in Hong Kong, there is a need to study the exercise intervention effect for this sample of participants living in group homes. The purpose of the current study was to determine the effectiveness of a multicomponent exercise intervention program in improving physical activity levels, aerobic fitness, self-efficacy and social support of the adults with ID who reside in group homes in Hong Kong.
Materials and Methods
The study participants were residents of Group Home A (GHA) and Group Home B (GHB). Both group homes receive government subventions and are managed by a non-profit social service organization. Particularly, they provide 24-h support and care in a restrictive environment that all residents have to obtain permission leaving the home area. Each of these homes is located in a building block with only indoor area, each is also paired with a sheltered workshop in the same building providing full-time employment for its residents. Work in the sheltered workshop mainly involves simple repetitive tasks performed in a sitting position such as sticking labels onto a product or packaging goods. During weekdays, the residents have the longest resting period between post-dinner and pre-bed time. Both homes offer regular recreational activities (e.g., drawing class, dancing class) in the evenings for residents but the participation is on a voluntarily basis. GHA has 55 residents and 21 staff with a hostel area of 699m2 (i.e., 12.7m2 per resident) while GHB has 71 residents and 30 staff with a hostel area of 1069m2 (i.e., 15.1m2 per resident). Activity area of GHA is 135m2 (19% of total area) comprising of a dining room (93m2), a multi-purpose room (9m2) and a fitness room (32.5m2). Activity area of GHB is 258m2 (24% of total area) comprising of a dining room (218m2) and a multi-purpose room (40m2). The inclusion criteria for the study participants from GHA and GHB were: (i) adults aged 18-60; (ii) individuals of mild or moderate ID, (iii) able to walk without an assisting device and (iv) informed consent given by parents or guardian. Based on power analysis reported in an earlier paper [19], 30 residents from each group home should be recruited. The study was approved by the University’s Human Ethics Committee and the group home managing board. Data collection took place between October 2015 and March 2016.
Research Design
This study was a non-randomized pre-post control delayed treatment research design with two phases of intervention implementation. Each phase marked the beginning of the intervention program provided to either GHA or GHB, separately. In the first phase, the Experimental Group (EG), residents of GHA, received intervention while the Wait-List Control Group (WLG), residents of GHB, followed their own daily routines and no intervention was assigned. In the second phase (immediately after EG completed intervention), WLG received intervention while EG entered into follow-up. As shown by the participant flowchart (Figure 1), all outcome measures were assessed at four separate time points. The EG participants were assessed at baseline (Time 0), 10 weeks postintervention (Time 1) and at a 10-week follow-up (Time 2). The WLG participants were assessed at the first baseline (Time 0) and then the second baseline (equivalent to EG’s baseline) at Time 1, prior to WLG started their intervention and lastly at postintervention (Time 2) and 10-week follow-up (Time 3).
Figure 1:Study designs for data analysis.
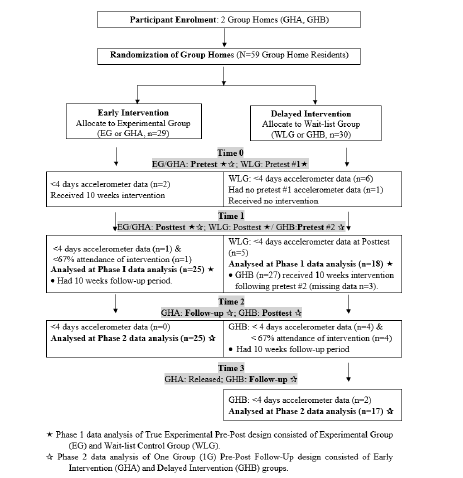
Intervention program
The physical activity multi-component intervention program was conducted in the group homes which lasted for 10 weeks and comprised of (i) a structured group exercise program (3X per week, 60min duration per session), (ii) three educational sessions for participants (60min per session) and (iii) one staff training session of 90min. The contents of the educational component were based on SCT focusing on improving self-efficacy and social support in PA behavior. The staff training focused on skills in teaching PA. The intervention program was described in details elsewhere [19]. The main emphasis of the intervention program was the structured group exercise program. Prior to its implementation, five lesson plans were constructed mainly with physical exercises aiming to train aerobic fitness. Participants were prompted to do fundamental movements of walking, jogging and jumping with gradual increase in intensity from the first lesson plan to the latter ones. An instructor with university graduate degree in physical education was responsible in for conducting the program. Furthermore, for each intervention group, the lead author of the study observed five exercise classes by 2-week interval and affirmed that the instructor followed the lesson plans.
Measurement
The main outcome measures were PA and cardiorespiratory fitness. The secondary outcome measures were PA-related psychosocial variables of self-efficacy and social support by family, home staff and peers. In addition, anthropometric measures, including height (m), weight (kg), Body Mass Index (BMI), Waist Circumference (WC, cm), Hip Circumference (HC, cm) and percent body fat (% body fat, assessed by TBF-410 Body Composition Analyzer; Tanita Corp, Japan), were collected. All outcome measurements were taken three times for the EG but four times for the WLG.
Physical activity levels
PA levels were assessed by an accelerometer (GT3X-BT, triaxial activity monitor, Actigraph LLC, Pensacola, FL, USA). Participants wore the accelerometer consecutively for a minimum of five days. Accelerometer has been used extensively in PA studies that involved adults with ID [20]. On each measurement day, the test assistant helped each participant to wear an accelerometer (attached to a belt) at the waist level (right side) when they first met in the morning. Participants were told to wear it at all times with the exception of bath time and bedtime. Accelerometer was set to capture with a 60-s epoch length periods with and non-wear time being defined as ≥60 consecutive minutes of zero recording. Only accelerometry data consisting of a minimum of four days [21,22] with at least 10h recording [23] was analyzed. According to the cutoffs from [24], the definitions of PA levels were set as: Moderate-To- Vigorous (MVPA), as >1951 counts counts·min-1; sedentary time, as <100 counts·min-1 [24] and light-intensity PA (LPA), as 100- 1951 counts·min-1. Data were reported by percent of time spent in PA levels in sedentary (SB%), light PA (LPA%) and MVPA (MVPA%).
Cardiorespiratory fitness
Cardiorespiratory fitness was assessed by the 6-Minute Walk Test (6MWT) that measures the maximum walking distance covered by the participant in 6 minutes. Its validity and reliability were established for adults with ID. The participants had to walk as fast as possible in a 25-meter distance (outdoor) for 6 minutes. During testing, the administrator delivered words of encouragement (preset) regularly by every 30-sec.
Psychosocial characteristics
The Self-Efficacy/Social Support for Activity for persons with Intellectual Disability (SE/SS-AID) scale was used with proven psychometric properties [25]. The scale consists of two parts: first, Self-Efficacy (SE) with 6 items and second, Social Support (SS) with 18 items allocated in 3 subscales in which family, staff and peers have 7, 6 and 5 items, respectively. A Chinese translation of these items was conducted using forward-backward translation procedures. The internal consistency reliability of the SE/SS-AID in Chinese was determined by Cronbach’s alpha in data analysis.
Analysis of data
Data were analyzed if participants had a minimum of four days of valid accelerometer data and attended at least 67% of the exercise sessions and educational talks. Data were analyzed by IBM SPSS (version 25, IBM Corp., Armonk, NY, USA). Prior to undertaking inferential statistical tests, data normality was checked by for skewness and kurtosis. Independent t-tests were computed to determine any mean differences between experimental treatment (EG, WLG), gender (Male, Female) and ID type (Mild, Moderate) in the pretest (Time 0) measures existed. In order to determine the intervention effect of the PA program, results were determined based on two separate analysis plans according to the two phases of study implementation. The two plans were taken just as data were collected under a true experimental and a one-sample pretestposttest- follow-up design, respectively. Our first analysis involved measures taken in the first phase satisfying the true experimental setting, a two-way mixed-design ANOVA was computed to compare the mean differences between EG and WLG of pretest and posttest in each outcome measure. Our second analysis involved measures taken in the second phase (began at WLG receiving intervention) satisfying the one sample pretest-posttest-follow-up setting, a one-way repeated measure ANOVA was computed to compare differences in outcome measures at among three time periods of all intervention participants.
Result
Among 59 study participants (41 males, 18 females), 29% of them were of mild-grade ID (n=17) and the rest (n=42) were of moderate-grade ID. Besides, 32% (n=19) had Down syndrome, 81% (n=48) had comorbidity (such as hypertension, hyperlipidemia). Twenty-nine residents were from GHA (EG) and 30 residents were from GHB (WLG, receiving delayed treatment). Final analyses for Phase 1 and Phase 2 included 43 and 42 adults with ID, respectively (see Figure 1 for the flowchart of study procedures and analysis). In checking for data normality, only accelerometry data were skewed positively, hence, natural log transformation for normality on all PA measures was conducted. Meanwhile, Cronbach’s alpha for the Chinese SE/SS-AID was 0.74 indicating acceptable scale reliability. In terms of descriptive statistics for baseline characteristics, the mean age and its standard deviation of EG and WLG were 42.6±6.4 and 45.11±6.7, respectively; and their mean BMI values were nearly the same (EG: 23.8±4.0, WLG: 23.9±4.6) (Table 1). There were sex differences in these baseline anthropometric variables: body height, BMI, HC and % body fat. However, no differences were found in all baseline anthropometric variables between mildgrade and moderate-grade ID. In regard to pretest differences of the intervention outcomes, WLG had significantly higher means in MVPA% (p=0.002) but lower means in social support of family (p=0.012) (Table 1).
Table 1:Physical activity and physical fitness of adults with Intellectual Disabilities (ID) overall and by sex and severity of intellectual disabilities in the baseline assessments.
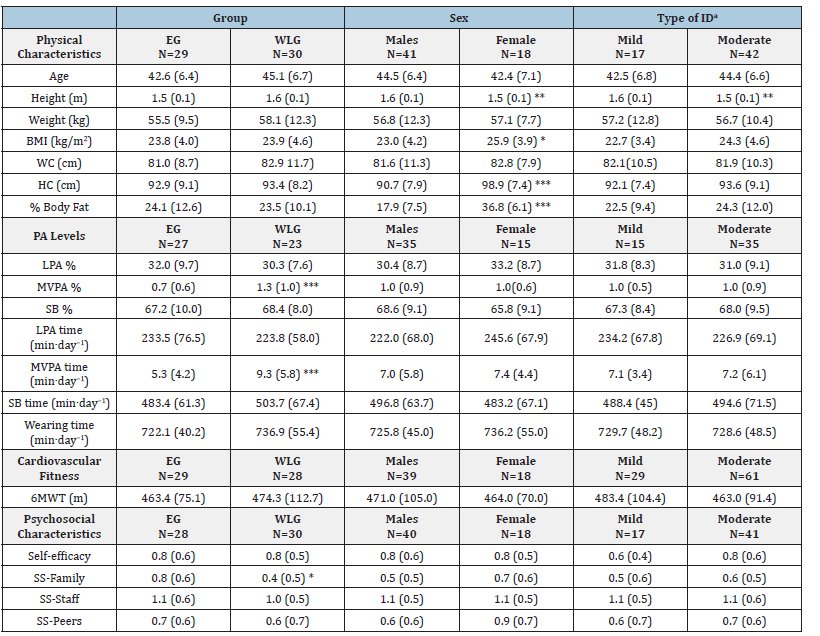
Note: *p<0.05; **p<0.01; ***p<0.001. Statistical tests were adjusted for Group and Sex.
Abbreviations: 6MWT-Six-Minute Walk Test; BMI-Body Mass Index; HC-Hip Circumference; LPA-Light-Intensity
Physical Activity; MVPA-Moderate-To-Vigorous Physical Activity; SB-Sedentary Behavior; WC-Waist Circumference; SSSocial
Support.
First phase of study: True experimental design
Analyses of true experimental with pretest-posttest design were based on 43 participants fulfilling criteria for analysis with four days of valid accelerometer data and 67% exercise attendance. When adjusted by age and sex, the 2X2 mixed-design ANOVA (intervention by time) results showed that there was no interaction effect on any of the outcome variables (Table 2). For the intervention (EG vs WLG) main effect, participants of WLG had significant higher overall mean in MVPA% than EG (adjusted transformed means: EG=- 0.55, WLG=0.194, p=0.014, ES=0.169). For the time (Time 0 vs Time 1) main effect, significant changes were found in 6MWT and social support-staff. Both EG and WLG participants walked more distance in 6MWT (p=0.045, ES=0.119) in posttest (mean=519.10±20.76) than pretest (mean=484.79±20.46). In addition, both EG and WLG participants perceived less social support from staff (p=0.011) in posttest (mean=1.28±0.13) than in pretest (mean=0.93±0.07).
Table 2:Adjusted means (SE)s and pairwise comparisons of physical activity, physical fitness and psychological characteristics of adults with ID according to center by time trial (N=43) for the true experimental pre-ost design.
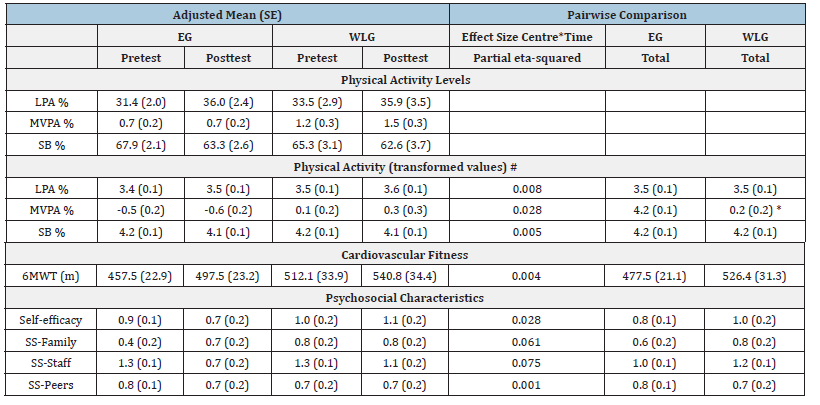
Note: # based on natural log transformation. * p<0.05. Abbreviation: LPA-light-Intensity Physical Activity; MVPA-Moderate-To-Vigorous Physical Activity; SB-Sedentary Behavior; 6MWT-Six-Minute Walk Test; and SS-Social Support.
Second phase of study: One-sample pretest, posttest and follow-up design
Analyses of the one group pretest-posttest, follow-up design were based on the same data selection criteria (N=42) when data were matched by their respective time trials. There were significant differences in LPA%, SB%, 6 MWT, and social supportstaff over the three time points (Table 3). By multiple comparisons with Bonferroni adjustment on PA levels based on nature log transformation, LPA% had a significant increase (p=0.035) in posttest (3.61±0.07) as compared to pretest (3.45±0.06), however, the mean value had a decrease in the follow-up (3.41±0.07; p=0.009). The same change but reverse pattern was observed in SB%, that intervention participants had a significant reduction (p=0.015) in posttest (4.07±0.04) as compared to pretest (4.18±0.03) but the mean value had an increase in the follow-up (4.19±0.03; p=0.005). In regard to cardiorespiratory fitness, intervention participants had a significant drop in the follow-up compared to posttest (posttest: 523.95±20.81m vs. follow-up: 454.33±18.26m, p<0.001) and there was no significant difference between pretest and posttest in 6MWT see (Table 3). Lastly, all participants perceived lower social support from staff in posttest compared with pretest (pretest: 1.18±0.085 vs. posttest: 0.89±0.12; p=0.039) and there was no significant difference between posttest and follow-up. The overall exercise compliance for all participants was 85%. GHA had relatively higher compliance rate (GHA: 93%, GHB: 77%). The compliance in wearing accelerometer was also high with two participants refusing to wear it. Also, 83% of all participants yielded a minimum of 4 days accelerometer data across three time points in the second phase of study.
Table 3:Adjusted means (SE)s and pairwise comparisons of physical activity, physical fitness and psychological characteristics of adults with ID according to center by time trial (N=43) for the true experimental pre-ost design.
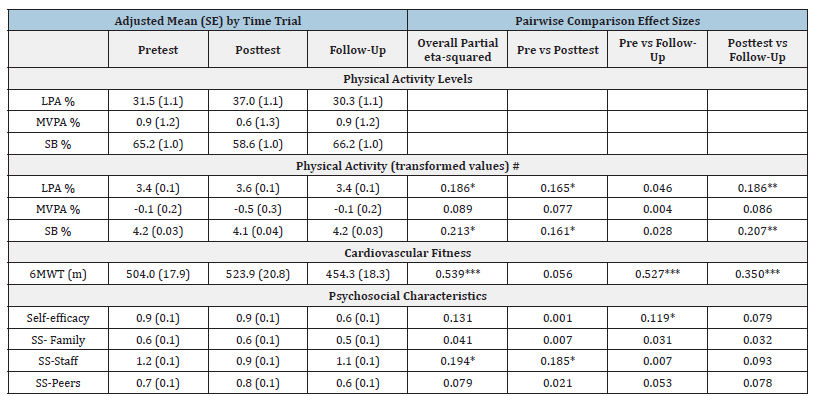
Note: # based on natural log transformation. * p<0.05; ** p<0.01; *** p<0.001. Abbreviation: LPA-light-Intensity Physical Activity; MVPA-Moderate-To-Vigorous Physical Activity; SB-Sedentary Behavior; 6MWT-Six-Minute Walk Test; and SS-Social Support.
Discussion
The main purpose of the PA intervention was to increase PA and cardiorespiratory fitness for adults with mild-grade and moderate-grade ID living in group homes. One-way repeated analyses with three time-points in Phase 2 revealed that there was significant time effect and PA intervention is successful in increasing the participants’ LPA%, reducing their SB% at postintervention as compared with baseline. The results were similar to [26] of a weight loss 24 weeks intervention comprising of PA component without a control group comparison. Although MVPA has been the focus in PA recommendation by WHO, LPA has been recognized for its role in yielding positive health benefits for inactive individuals [27,28]. Our study result is not successful in increasing the percentage of daily time engaging in MVPA. It was different to [29] of an exercise intervention of aerobic and strength training twice a week, 90-minute duration for 12 weeks, their findings showed a significant increase in minutes of MVPA per day compared with the control. Similar finding of insignificant effects on MVPA were reported by [30], who conducted 12 weeks walking program with adults with ID. The reason for no impact on MVPA in the present study might be due to the intensity of the structured group exercise sessions. Although the intervention was originally targeted to increase MVPA, the exercise intensity might have set at lower exercise intensity mostly in the earlier lesson plans. However, our findings indicated significant increase in LPA% and decrease in SB% in posttest as compared to pretest. These intervention effects were lost in the 2-month follow-up that their LPA% and SB% regressed to the baseline levels. In addition to the insignificant result on MVPA%, the intervention program was not effective in increasing cardiorespiratory fitness by pre-post comparison.
As opposed to [31] study in which their intervention group increased in 6MWT after 40 sessions of 20 weeks in aerobic and combined aerobic and resistance training. The training duration of the present study was only half of [31]. that might be the reason for non-significant result. Similarly, [32] also found insignificant change in 6MWT after 8 weeks of walking program of young adults with Down syndrome. However, there was significant reduction in distance walked in the follow-up as compared to the post-intervention in the present study. This may translate to bigger decline in cardiorespiratory fitness when intervention was withdrawn for a period of time as reflected by the follow-up results. These significant differences in the outcomes indicated that the multicomponent PA intervention effects on LPA%, SB% and 6MWT were not sustainable. As shown by baseline data, adults with ID were mostly sedentary (SB%=~67 to 68%) with 0.7% to 1.3% daily time spent in MVPA. In other words, adults with ID had less than 8 minutes of total time engaging in MVPA each day, which were at least 94 minutes short in meeting the WHO’s PA weekly recommendation of 150 minutes MVPA. The time engaging in MVPA in the present study was less than those reported in previous studies [26,33]. One possible explanation might be due to differences in the available facilities as evidenced by limited open space available in the group homes in the current study.
In addition, results from the data analyses of true-experimental design in Phase I revealed that there was variability of PA levels between group homes of EG and WLG and that EG had significantly lower MVPA% in posttest than pretest as compared to WLG. This unexpected result might be due to the John Henry effect experienced by the WLG participants that they might have felt differently in the posttest meeting outsiders (testers) the second time while experimental participants met with outsiders (instructor and exercise assistants) constantly during the intervention. In terms of cardiorespiratory fitness, a significant time effect was found that all participants did better in posttest than pretest, however, there was no intervention effect. Again, WLG participants might be influenced by the John Henry effect, together with EG, all adults with ID did better in posttest. Indeed, findings from a recent meta-analytical study [34] reported a range of no effect or small effect in cardiorespiratory fitness assessed by 6MWT when comparing exercise intervention to sedentary controls. In regard to psychosocial characteristics, participants gave lower score in perceived social support-staff in posttest than pretest. This might be explained by having outsiders visiting the two centers twice resulting in having all participants perceived less social support given from staff in the posttest. On the whole, Phase 1 analyses found no significant interaction effect between intervention (EG vs. WLG) and time (pretest vs. posttest). The reason could be due to a relatively small sample size of 43 participants for final analysis in which the power in significance has been affected. Research findings have shown better outcomes by multi-component intervention. For example, on reviewing qualitative studies about program conditions that foster quality PA participation experiences for people with a physical disability [35], found that group-based programing and instructor-led leadership were important for fostering quality activity experience. The present study involved instructor-led group exercises. Based on interviews with group home staff [36], the feedbacks of group home staff showed that some participants of the present study seemed to be eager to do the exercise program and they would remind staff to clear the venue for exercise preparation.
In terms of psychosocial changes on PA intervention, based on Social Cognitive Theory, this study provided education talks to the participants, which was similar to the study designed by [37] providing PA and education program as intervention treatment. However, the present study outcomes did not show any perceived changes in self-efficacy and social support given by peers. Selfefficacy, an important component related to PA participation, as contradictory to our result, was found to be significantly increased after a PA intervention in previous studies [29,38,39]. Possible explanation for no effect on self-efficacy and social support given by peers might be due to the participants’ difficulty in understanding complex behavior change concepts. In terms of exercise compliance, our study has shown high exercise compliance with 86% on average of attendance for all participants in the total of 30 exercise sessions, compared favorably with other intervention studies on adults with ID, e.g. 96% exercise compliance in 8 weeks of scheduled walking sessions [32].
On the other hand, the compliance in wearing the accelerometer was also high. On the contrary [40], study could only get 59% (N=42) of adults with ID providing full dataset (4 days of accelerometer data) compared to 71% (N=59) having accelerometer data of a minimum of four days in three time points in our present study. On the other hand, a history event occurred in GHA (EG) that a resident not involving in the study passed away during the study intervention period. It was not known about its possible effect on the emotional state of the study participants of GHA. Also, an adverse event occurred in GHB during an exercise session in which a participant, with a previous history of fainting, hence, wearing a soft helmet, fainted while slow jogging and he was unharmed. There were few limitations of the study. Our study was a non-randomized trial; randomized controlled trial should be conducted in the future studies. In addition, for educating participants to do more exercise through three seminars, our educational contents focused on doing more physical exercises by talking about health benefits as well as achieving it through social support among peers. However, we did not use knowledge test in assessing their cognitive attainment. Likewise, for outcome measures, muscular strength tests were not conducted in this study. On the other hand, our design included 10- week follow-up tests, which seems to be a rarity in which we found very few studies providing follow-up measurements.
Conclusion
Our study is successful in increasing light physical activities and reducing sedentary behavior after intervention. Specific to Hong Kong group home context, adults with ID reside at confined indoor environment having very limited space for physical activities and most are in sitting position during non-work time. It seems prudent to suggest future study to focus on increasing light intensity rather than moderate-to-vigorous exercise intensity for adults with ID.
Acknowledgement
We would like to thank all volunteers for participation in this study.
References
- American Association of Intellectual and Developmental Disabilities. Definition of Intellectual Disability.
- Census and Statistics Department HKSAR (2015) Persons with Disabilities and Chronic Diseases in Hong Kong; Hong Kong Monthly Digest of Statistics. Census and Statistics Department of the HKSAR, Hong Kong.
- Maulik PK, Mascarenhas MN, Mathers CD, Dua T, Saxena S (2011) Prevalence of intellectual disability: A meta-analysis of population-based studies. Res Dev Disabil 32(2): 419-436.
- Dairo YM, Collett J, Dawes H, Oskrochi GR (2016) Physical activity levels in adults with intellectual disabilities: A systematic review. Prev Med Reports 4: 209-219.
- Heller T, Fisher D, Marks B, Hsieh K (2014) Interventions to promote health: Crossing networks of intellectual and developmental disabilities and aging. Disabil Health J 7(1): S24-S32.
- Bouzas S, Martínez-Lemos RI, Ayán C (2019) Effects of exercise on the physical fitness level of adults with intellectual disability: A systematic review. Disabil Rehabil 41: 3118-3140.
- Hassan NM, Landorf KB, Shields N, Munteanu SE (2019) Effectiveness of interventions to increase physical activity in individuals with intellectual disabilities: A systematic review of randomised controlled trials. J Intellect Disabil Res 63(2): 168-191.
- Temple VA, Frey GC, Stanish HI (2017) Interventions to promote physical activity for adults with intellectual disabilities. Salud Publica Mex 59(4): 446-453.
- Michalsen H, Wangberg SC, Hartvigsen G, Jaccheri L, Muzny M, et al. (2020) Physical activity with tailored mHealth support for individuals with intellectual disabilities: Protocol for a randomized controlled trial. JMIR Res Protoc 9 (6): e19213.
- Pitchford EA, Dixon-Ibarra A, Hauck JL (2018) Physical activity research in intellectual disability: A scoping review using the behavioral epidemiological framework. Am J Intellect Dev Disabil 123(2): 140-163.
- Bondár RZ, Di Fronso S, Bortoli L, Robazza C, Metsios GS, et al. (2020) The effects of physical activity or sport-based interventions on psychological factors in adults with intellectual disabilities: A systematic review. J Intellect Disabil Res 64(2): 69-92.
- Bandura A (1986) Social foundations of thought and action: A social cognitive theory. Prentice-Hall, Englewood Cliffs NJ, USA.
- Rhodes RE, Nigg CR (2011) Advancing physical activity theory: A review and future directions. Exerc Sport Sci Rev 39(3): 113-119.
- Young MD, Plotnikoff RC, Collins CE, Callister R, Morgan PJ (2014) Social cognitive theory and physical activity: A systematic review and meta-analysis. Obes Rev 15(12): 983-995.
- Peterson JJ, Lowe JB, Peterson NA, Nothwehr FK, Janz KF, et al. (2008) Paths to leisure physical activity among adults with intellectual disabilities: Self-efficacy and social support. Am J Heal Promot 23(1): 35-42.
- Bazzano AT, Zeldin AS, Diab IRS, Garro NM, Allevato NA, et al. (2009) The healthy lifestyle change program: A pilot of a community-based health promotion intervention for adults with developmental disabilities. Am J Prev Med 37(6): S201-S208.
- Marks B, Sisirak J, Chang YC (2013) Efficacy of the health matters program train-the-trainer model. J Appl Res Intellect Disabil 26(4): 319-334.
- Clement T, Bigby C (2010) Group homes for people with intellectual disabilities: Encouraging inclusion and participation. Jessica Kingsley, London, UK.
- Chow BC, Huang WYJ, Choi PHN, Pan C (2016) Design and methods of a multi-component physical activity program for adults with intellectual disabilities living in group homes. J Exerc Sci Fit 14(1): 35-40.
- Chow BC, Choi PHN, Huang WYJ (2018) Physical activity and physical fitness of adults with intellectual disabilities in group homes in Hong Kong. Int J Env Res Public Heal 15(7): 1370.
- Hart TL, Swartz AM, Cashin SE, Strath SJ (2011) How many days of monitoring predict physical activity and sedentary behaviour in older adults? Int J Behav Nutr Phys Act 8: 62.
- Tudor-Locke C, Camhi SM, Troiano RP (2012) A catalog of rules, variables, and definitions applied to accelerometer data in the national health and nutrition examination survey, 2003-2006. Prev Chronic Dis 9: E113.
- Troiano RP, Berrigan D, Dodd KW, Mâsse LC, Tilert T, et al. (2008) Physical activity in the United States measured by accelerometer. Med Sci Sport Exerc 40(1): 181-188.
- Freedson PS, Melanson E, Sirard J (1998) Calibration of the computer science and applications, Inc. accelerometer. Med Sci Sport Exerc 30(5): 777-781.
- Lee M, Peterson JJ, Dixon A (2010) Rasch calibration of physical activity self-efficacy and social support scale for persons with intellectual disabilities. Res Dev Disabil 31(4): 903-913.
- Melville CA, Boyle S, Miller S, Macmillan S, Penpraze V, et al. (2011) An open study of the effectiveness of a multi-component weight-loss intervention for adults with intellectual disabilities and obesity. Br J Nutr 105(10): 1553-1562.
- Füzéki E, Banzer W (2018) Physical activity recommendations for health and beyond in currently inactive populations. Int J Env Res Public Heal 15(5): 1042.
- Warburton DER, Bredin SSD (2016) Reflections on physical activity and health: What should we recommend? Can J Cardiol 32(4): 495-504.
- Jo G, Rossow-Kimball B, Lee Y (2018) Effects of 12-week combined exercise program on self-efficacy, physical activity level, and health related physical fitness of adults with intellectual disability. J Exerc Rehabil 14: 175-182.
- Melville CA, Mitchell F, Stalker K, Matthews L, Mc Connachie A, et al. (2015) Effectiveness of a walking programme to support adults with intellectual disabilities to increase physical activity: Walk well cluster-randomised controlled trial. Int J Behav Nutr Phys Act 12: 125.
- Calders P, Elmahgoub S, deMettelinge TR, Vandenbroeck C, Dewandele I, et al. (2011) Effect of combined exercise training on physical and metabolic fitness in adults with intellectual disability: A controlled trial. Clin Rehabil 25(12): 1097-1108.
- Shields N, Taylor NF (2015) The feasibility of a physical activity program for young adults with down syndrome: A phase II randomised controlled trial. J Intellect Dev Disabil 40(2): 115-125.
- Spanos D, Hankey CR, Melville CA (2016) The effectiveness of a weight maintenance intervention for adults with intellectual disabilities and obesity: A single stranded study. J Appl Res Intellect Disabil 29(4): 317-329.
- St John L, Borschneck G, Cairney J (2020) A systematic review and meta-analysis examining the effect of exercise on individuals with intellectual disability. Am J Intellect Dev Disabil 125(4): 274-286.
- Shirazipour CH, Evans MB, Leo J, Lithopoulos A, Martin Ginis KA, et al. (2020) Program conditions that foster quality physical activity participation experiences for people with a physical disability: A systematic review. Disabil 42(2): 147-155.
- Chow BC, Choi PHN, Huang WY, Pan C (2020) Promoting physical activity in group home settings: Staff perspectives through a SWOT analysis. Int J Environ Res Public Health 17(16): 5805.
- Van Schijndel-Speet M, Evenhuis HM, van Wijck R, van Montfort KCAGM, Echteld MA (2016) A structured physical activity and fitness programme for older adults with intellectual disabilities: Results of a cluster-randomised clinical trial. J Intellect Disabil Res 61(1): 16-29.
- Heller T, Hsieh K, Rimmer JH (2004) Attitudinal and psychosocial outcomes of a fitness and health education program on adults with down syndrome. Am J Ment Retard 109(2): 175-185.
- Pérez-Cruzado D, Cuesta-Vargas AI (2016) Changes on quality of life, self-efficacy and social support for activities and physical fitness in people with intellectual disabilities through multimodal intervention. Eur J Spec Needs Educ 31(4): 553-564.
- Bodde AE, Seo DC, Frey GC, Van Puymbroeck M, Lohrmann DK (2012) Correlates of moderate-to-vigorous physical activity participation in adults with intellectual disabilities. Health Promot Pract 14(5): 663-670.
© 2026 Peggy HN Choi. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






