- Submissions

Full Text
Developments in Anaesthetics & Pain Management
A Ten-Years Review of Palliative Procedures for Congenital Heart Diseases in KATH Kumasi: The Need for a Paradigm Shift in Africa
Sanjeev Singh1,2* and Isaac Okyere3,4
1Department of Anaesthesiology and Intensive Care, Ghana
2Directorate of Anaesthesia and Intensive Care, Komfo Anokye Teaching Hospital, Ghana
3Department of Surgery, Ghana
4Cardiovascular and Thoracic Surgery Unit, Ghana
*Corresponding author: Sanjeev Singh, Department of Anaesthesiology and Intensive Care, Ghana
Submission: March 02, 2021;Published: April 26, 2021

ISSN: 2640-9399 Volume2 Issue1
Abstract
Background: Congenital Heart Disease (CHD) is one of the leading causes of infant death from congenital malformations. The incidence of CHD is about 8 cases per 1,000 live births with a higher absolute number in African countries. The fifty-four countries in Africa have an estimated total annual CHD birth prevalence of 300,486 cases. Out of this 51.4% of the continental birth prevalence occurs in only seven African countries. CHD primarily remains a paediatric health issue in Africa because of the deficient health-care systems. Insufficient infrastructure adds to the list of obstacles to Open-Heart Surgery (OHS) in this region. Africa has one Cardiac-centre for 50 million inhabitants. Komfo Anokye Teaching Hospital (KATH), Kumasi provides surgical and perioperative care to CHD patients going for OHS from the Ashanti region, other regions of Ghana as well as neighbouring countries. The purpose of this study was to describe the types of palliative surgical procedures performed in the last ten years, to compare the change in trends before and after 2014, to assess the efficiency and quality of palliative care provided patients with congenital heart diseases in a low resource setting at KATH, Kumasi.
Methods: A retrospective study from 2007 to 2016 involved 118 patients from either sex, undergone OHS under general anaesthesia after obtaining approval from Committee on human research publications and ethics
Results: The average ICU Length of Stay (LOS) in days and average hospital LOS in days were (3.15±2.37 and 1.37±2.85), and (6.86±3.50 and 4.21±3.67) before 2014 and after 2014 respectively. Increase in the number of on-table extubations from 7.2% to 39.7% whereas a decrease in average mechanical ventilation time from 82.35±11.71 to 23.49±7.93 hrs in group after 2014. Postoperative chest tube drainage in the first 48 hours decreased from 133±28.4 to 95±20.3 ml and re-exploration from 11.6% to 2.7%, which reduced postoperatively bleeding and re-exploration with the use of tranexamic acid after 2014.
Conclusion: The surgeries that have been performed provided good palliation for congenital heart diseases in this environment thus there is a need for a paradigm shift to achieve long-term sustainability of OHS in Africa.
Keywords: Congenital heart disease; Kumasi; Open-heart surgery; Palliative procedure; paradigm shift
Abbreviations: CHD: Congenital heart disease; WHO: World Health Organisation; RHD: Acquired Rheumatic Heart Disease; UNDP: United Nations Development Program; NCD: Non-Communicable Diseases; OHS: Open-Heart Surgery; KATH: Komfo Anokye Teaching Hospital; VSD: Ventricular Septal Defect; DORV: Double Outlet Right Ventricle; ACC: Aristotle’s Comprehensive Complexity; TXA Tranexamic Acid; BT: Blalock-Taussig
Introduction
Congenital Heart Disease (CHD) is the most common class of major congenital
malformations. Although there is a slight variation between many population-based studies,
CHD affects ≈1% of or about 40,000 live births per year in the United States [1]. The incidence
of CHD is 6-13 per 1000 live births in sub-Saharan Africa. In Ghana, the estimated burden
of CHD is in the region of 372 per million of the population [2]. In addition to CHD, the
prevalence of Acquired Rheumatic Heart Disease (RHD) is also high in Africa and Asia. It
ranges from 2.7 to 20/1,000 population. According to the World Health Organisation (WHO),
in developing countries, RHD attacks more than four million people and causes about 90,000
deaths per year, [3] which is quite different from the developed world. During the next 20-
40 years, low-middle-income countries will be confronted with the persistence of RHD [4]. We know from the current United Nations Development Program
(UNDP) data that roughly 70 million children may die before
reaching their 5th birthday and most will be from sub-Saharan
Africa [5]. These together cause a problem even more complex
and bigger in Africa. There has been a 50% global decrease in the
incidence of preventable deaths of children since 1990. However,
the mortality from Non-Communicable Diseases (NCD) such as
CHD has not changed. Of the estimated 1.3 million children born
with CHD annually, over 90% do not have access to cardiac care
[6]. The high fertility rate in much of sub-Saharan Africa leads to a
disproportionate number of children born with CHD in this part of
the world [2]. Many such children have no geographical or financial
access to medical and surgical treatment.
Only three West-African countries have regular open-heart
surgery activity, including centres in Ghana (National Cardiothoracic
Center-Accra), Senegal (Centre Cardio-Pédiatrique Cuomo-Dakar)
and Cote d’Ivoire (Heart Institute-Abidjan). The average number
of operations performed in these three countries is insignificant,
faced with the yearly number of cardiovascular patients in West-
African countries [1]. Insufficient infrastructure adds to the list of
obstacles to Open-Heart Surgery (OHS) in this region. The United
States of America (USA) and Europe have one OHS centre per 150
thousand and one million inhabitants, but Africa has one centre for
50 million inhabitants [7] .Ghana is one of the few low-to-middleincome
countries in West Africa that has one officially accredited
tertiary center that is the National Cardiothoracic Centre (NCTC)
in Accra. Currently, the Komfo Anokye Teaching Hospital (KATH),
Kumasi consistently sustains a cardiothoracic program for more
than one decade and slowly building towards its independent
centre. The Ashanti Region is the third large administrative region
in Ghana with a population of more than 2 million [8]. KATH
provides surgical and perioperative care to patients with CHD
going for OHS. Our efforts have primarily focused on the selection
of simple cases in which a life expectancy of less than 1-2 years
without corrective surgery. Expectedly, practicing cardiothoracic
surgery in such a resource-poor setting has peculiar challenges.
Despite challenges, human and economic we sustained our OHS
programme. We accepted challenges and promise to continue our
services in OHS to develop KATH as a new cardiothoracic centre
in Ghana. The purpose of this study was to describe the types of
surgeries performed in the last ten years, to compare the change
in trends before and after 2014, to assess the efficiency and quality
of care provided by the cardiac anesthesiologist in the delivery of
care in a low resource setting. This review also discusses how lowmiddle
income countries in Africa with limited resources continue
their OHS programme. This needs a paradigm shift to achieve longterm
goals.
Methods
This study was performed through a retrospective chart review of 118 cases out of 121 cardiac surgeries performed from 2007-2016. Patients with insufficient data were excluded from the relevant analysis (in one case the intraoperative record was missing, and three patients’ post-operative records were missing). Institutional approval for the study was obtained from the Komfo Anokye Teaching Hospital (KATH) Committee on human research publications and ethics. KATH is the second-largest teaching hospital in Ghana and the only tertiary institution in the Ashanti region with 1264 beds. (KATH Annual Report, 2019). This study describes the types of surgeries performed in the last ten years, to compare the change in trends before and after 2014, to assess the efficiency and quality of care provided by the cardiac anaesthesiologist in the delivery of this care in a low resource setting in Ghana at KATH Kumasi.
Result
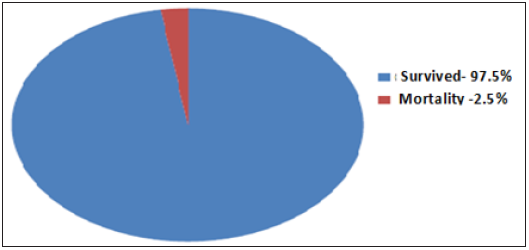
A comprehensive demographic profile of the study population is shown in Table 1. All the demographic profiles in the group before 2014 and after 2014 were comparable. As patients’ average age, weight, body surface area were 5.61±1.05 and 5.69±1.01 years, 16.38± 0.65 and 17.46 ± 0.69Kg, and 0.57± 0.11 and 0.59 ± 0.15m2, whereas the male to female ratio before and after 2014 was 1:1.8 and 1:1.5 respectively (p>0.05). Data are presented as means±Standard Error of the Mean (SEM), Kg-Kilogram, Body surface area-BSA, F- Female, m- meters, M- Male. p-*Significant; **highly significant; NS-Not significant (>0.05). The types of surgeries that have been performed from 2007 till 2016 at Komfo Anokye Teaching Hospital including Ventricular Septal Defect (VSD) closure, Atrial Septal Defect (ASD) closure, Patent Ductus Arteriosus (PDA) ligation, Double Outlet Right Ventricle (DORV) repair and others as shown in Table 2 & Figure 1. ASD-atrial septal defect, DORV- double outlet right ventricle, PDA- patent ductus arteriosus, PFO-patent foramen ovale, PS-pulmonary stenosis, VSD-ventricular septal defect. Only three mortalities occurred in the last ten years, which shows a total mortality rate of 2.5%. All mortalities occurred before 2014, first was the result of cerebral malaria, and the rest two were associated with ventilator failure (Figure 2).
Table 1: Distribution of patient’s demographic profile.

Table 2: Type of surgeries.

Figure 1: Percentage of cardiac surgeries performed during the last ten years at KATH.
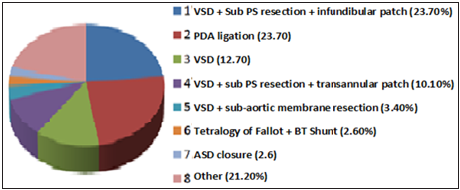
Figure 2: Post-cardiac surgery mortality rate in the last ten years at KATH.
Aristotle’s Comprehensive Complexity (ACC) level and NYHA/ Ross pre-operative functional class are shown in Table 3. The complexity level of cardiac operations performed in ten years had a mean of 7.1 whereas ACC means before 2014 and after 2014 were 6.9±0.35 and 7.3±0.32 respectively (p>0.05). They all belong to ACC level 2 as it represents 6.0-7.9 as shown in Table 3. Aristotle comprehensive Complexity -ACC, New York Heart Association- NYHA, P-*Significant; **highly significant; NS-Not significant (>0.05). The postoperative percentage of patients extubated in the operating room was 7.2% and 39.2% before 2014 and after 2014 which statistically significantly improved after 2014 (P<0.05). The number and duration of inotropes administered before 2014 and after 2014 groups are shown in Table 4. Adrenaline was the most commonly used in 84% and 79%, and milrinone the least commonly used inotrope 6% and 4% in before 2014 and after 2014 groups respectively. The number of hours adrenaline and dopamine required were significantly lesser after 2014 group (p<0.05) as shown in Table 4. The duration of postoperative mechanical ventilator support in hours, average ICU Length of Stay (LOS) in days, and average hospital LOS in days were (82.35±11.71 and 23.49±7.93), (3.15±2.37 and 1.37±2.85), and (6.86±3.50 and 4.21±3.67) before 2014 and after 2014 respectively. Postoperative chest tube drainage in the first 48 hours was significantly less after 2014 (95±20.3ml) as compared with before 2014 (133±28.4 ml) as shown in Table 5 (P<0.05). Data are presented as means±standard deviation (SD), and percentage, hrs= Hours; P-*Significant; **highly significant; NS -Not significant (>0.05).
Table 3: Complexity level.

Table 4: Comparison of inotropic drugs infused.

Table 5: Comparison of mechanical ventilation and Length of Stay LOS.

Discussion
Anaesthesia is a speciality with a severe deficit in many developing countries of Africa and anaesthetic services are often underdeveloped [9]. Similarly, it is a well-known fact that the number of the trained paediatric cardiac anaesthesiologist in developing countries is very few [10]. Anaesthesia is a technologybased speciality and relay on functioning monitoring devices and equipment [11]. Providing anaesthesia in developing countries becomes highly challenging because more than 19% of operation theatres in this part of the world have no pulse oximeter, [12] basic equipment, and drugs. We lost two patients due to ventilator failure and one due to cerebral malaria before 2014 study group. The main focus of our anaesthetic team is to reduce total perioperative and anaesthetic-related mortality with the help of evidence-based best practices. The appropriate selection of cases including patients with simple cardiac defects is one of the most important contributing factors for decreasing morbidity and mortality rate in paediatric cardiac surgery patients in developing paediatric cardiac surgery centres [13]. We selected simple cases as visible from Aristotle Comprehensive Complexity (ACC) level we had a mean of 7.1 for our cases which represent ACC level 2.
As proved in some studies that fast track surgery and early extubation reduced mortality [13]. Before 2014 on table extubation rate was 7% as compared to after 2014 which was 39%. In our study due to ventilator failure, there was 3.9% mortality before 2014. Simplification of the care and early extubation reduced mortality and complications after 2014. During paediatric cardiac surgery, a large increase in blood glucose has been reported when exogenous glucose was added intraoperatively. However, when glucose was excluded, hypoglycaemia occurred as mentioned by Singh et al. [14] One of our cases had hypoglycaemia due to tight glycaemic control before 2014. There is simply not enough evidence to suggest that tight glycaemic control would be of benefit in this paediatric patient population because the risks of hypoglycaemia are felt to be too great. CPB significantly affects glucose homoeostasis in children, hence it seems prudent to administer a small amount of dextrose in the pre-bypass period to avoid hypoglycaemia but the rate and dose of insulin we adjusted with glycaemic levels without tight glycaemic control due to simplification of the care protocol after 2014. In cardiac surgery postoperative bleeding is associated with an increased incidence of surgical re-exploration to identify the source of bleeding. Increased use of blood causes significant morbidities such as renal failure, sepsis, arrhythmias, a prolonged requirement for mechanical ventilatory support, longer hospital stay, and increased mortality [13]. The main focus of our anaesthetic team was to reduce post-operative complications of bleeding and reexploration. As many studies suggested the use of Tranexamic Acid (TXA) safe in paediatric cardiac surgery, TXA effectively reduces postoperative blood loss as well as re-exploration [15,16]. As an evidence-based best practice, we use TXA as a bolus of 20mg/kg after anaesthetic induction and 20mg/kg after protamine during major surgeries. Postoperative chest tube drainage in the first 48 hours decreased from 133±28.4 to 95± 20.3 ml and re-exploration rate from 11.6% to 2.7% before 2014 and after 2014 groups, respectively. It was reduced significantly with TXA use in the group after 2014 which reduce post-operative complications of bleeding and re-exploration.
The low cardiac output syndrome is a common complication in cardiac surgery patients [17] and inotropic support is frequently initiated to improve post bypass ventricular function. Inotropes may improve haemodynamics, but there is a potential risk for increased myocardial oxygen and energy consumption. [17,18]. It has been suggested that an increase in contractility of the hibernating but viable myocardium by low doses of inotropes can lead to a perfusion contraction mismatch with activation of anaerobe glycolysis and eventually myocardial necrosis [19-21]. Thus, the use of inotropes has been associated with adverse clinical outcomes as shown in a few studies. In a study by Fellahi et al. [22] use of dobutamine was associated with increased postoperative morbidity. This has resulted in an ongoing debate on the value or harm associated with the use of inotropes in cardiac surgery [22,23]. The number and duration of inotropes administered before 2014 and after 2014 in our study showed a significant reduction in their use as well as reduced mortality and morbidity of patients. Inotrope management is highly dependent on the patient requirement.Conclusion
The types of surgeries that have been performed from 2007 till 2016 at Komfo Anokye Teaching Hospital including Blalock- Taussig (BT) shunt, Ventricular Septal Defect (VSD) closure, Atrial Septal Defect (ASD) closure, Patent Ductus Arteriosus (PDA) ligation, Double Outlet Right Ventricle (DORV) repair provided good palliation for advanced congenital heart diseases in this environment at KATH. Efforts by the cardiac anaesthesia team to diligently avoid anaesthetic complications by appropriate selection of cases, minimise post-operative bleeding, and re-exploration through aggressive use of tranexamic acid, on-table extubation, and per-patient basis use of inotropic drugs with caution. All these contributed successes for our group’s experience to serve as a model for others that wish to develop a programme aimed at providing surgical care for patients with congenital heart disease in low- middle-income countries. There is a need for a paradigm shift to achieve the long-term sustainability of OHS in Africa.
References
- Reller MD, Strickland MJ, Colarusso RT, Mahle WT, Correa A (2008) Prevalence of congenital heart defects in Atlanta, 1998-2005. J Pediatr 153(6): 807-813.
- Edwin F, Tettey M, Aniteye E, Tamatey M, Sereboe L, et al. (2011) The development of cardiac surgery in West Africa--the case of Ghana. Pan Afr Med J 9:15.
- Yangni Angate KH (2016) Open heart surgery in sub-Saharan Africa: challenges and promise. Cardiovascular Diagnosis and Therapy 6(Suppl): S1-S4.
- Howson CP, Reddy KS, Ryan TJ (1998) Control of cardiovascular diseases in developing countries. Research, development, and institutional strengthening. Institute of medicine, National Academy Press; Washington, DC, USA.
- United Nations Development Program (UNDP) data.
- WHO (2017) Global health observatory data. Causes of child mortality.
- Pezzella TA (2005) Global expansion of cardiothoracic surgery-The african challenge. African Annals of Thoracic and Cardiovascular Surgery 1: 9-11.
- (2012) World Gazetteer online.
- Walker I, Wilson I, Bogod D (2007) Anaesthesia in developing countries. Anaesthesia 62(Suppl 1): 2-3.
- Doherty C, Holtby H (2011) Pediatric cardiac anaesthesia in the developing world. Paediatr Anaesth 21(5): 609-614.
- Hoffman JIE (2013) The global burden of congenital heart disease. Cardiovasc J Afr 24(4): 141-145.
- Hodges SC, Mijumbi C, Okello M, Mc Cormick BA, Walker IA, et al. (2007) Anaesthesia services in developing countries: defining the problems. Anaesthesia 62(1): 4-11.
- Cvetkovic M (2018) Challenges in pediatric cardiac anesthesia in developing countries. Front Pediatr 6: 254.
- Singh S, Zanwar YN, Okyere I (2020) Does meticulous blood glucose control during cardiopulmonary bypass improves outcome in paediatric patients? EAS J Anesthesiol Crit Care 2: 151-159.
- Zhang Y, Zhang X, Wang Y, Shi J, Yuan S, et al. (2019) Efficacy and safety of tranexamic acid in pediatric patients undergoing cardiac surgery: A single center experience. Front Pediatr 7: 181.
- Singh S, Annamalai A (2017) The efficacy of tranexamic acid versus epsilon amino caproic acid in decreasing blood loss in patients undergoing Mitral valve replacement surgery. Journal of Anesthesiology 5(2): 11-18.
- Ahmed I, House CM, Nelson WB (2009) Predictors of inotrope use in patients undergoing concomitant coronary artery bypass graft (CABG) and aortic valve replacement (AVR) surgeries at separation from cardiopulmonary bypass (CPB). J Cardiothorac Surg 4: 24.
- Nielsen DV, Hansen MK, Johnsen SP, Hansen M, Hindsholm K, et al. (2014) Health outcomes with and without use of inotropic therapy in cardiac surgery: results of a propensity score-matched analysis. Anesthesiology 120(5): 1098-1108.
- Indolfi C, Piscione F, Filardi P, Prastaro M, Di Lorenzo E, et al. (1996) Inotropic stimulation by dobutamine increases left ventricular regional function at the expense of metabolism in hibernating myocardium. Am Heart J 132(3): 542-5
- Schulz R, Rose J, Martin C, Brodde OE, Heusch G (1993) Development of short-term myocardial hibernation. Its limitation by the severity of ischemia and inotropic stimulation. Circulation 88: 684-695.
- Singh S, Okyere I, Singh A (2020) Team-based approach to surgical and anaesthetic care for children with congenital heart disease in a low resource setting in Ghana West Africa. RA journal of applied research 6(1): 2610-2615.
- Fellahi JL, Parienti JJ, Hanouz JL, Plaud B, Riou B, et al. (2008) Perioperative use of dobutamine in cardiac surgery and adverse cardiac outcome: propensity-adjusted analyses. Anesthesiology 108(6): 979-987.
- Shahin J, DeVarennes B, Tse CW, Amarica DA, Dial S (2011) The relationship between inotrope exposure, six-hour postoperative physiological variables, hospital mortality and renal dysfunction in patients undergoing cardiac surgery. Crit Care 15(4): R162.
© 2021 Sanjeev Singh. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






