- Submissions

Full Text
Associative Journal of Health Sciences
Clinical Management Self-Efficacy Differences Between Student Program Years
Pogemiller Kelly*, Brown Angela and O’Donnell Vanessa
University of Hartford, West Hartford, CT, USA
*Corresponding author:Pogemiller Kelly PT, DPT, EdD, University of Hartford, West Hartford, CT, USA
Submission: April 06, 2026;Published: April 17, 2026

ISSN:2690-9707 Volume4 Issue4
Abstract
Self-efficacy is known to influence learning and is associated with greater clinical practice confidence in in healthcare students. There are also known differences in physical therapy student clinical reasoning self-efficacy and clinical reasoning skills based on the program year. This study explores how caseload management self-efficacy compares between physical therapy students based on competed time in a graduate program. This study evaluated self-reported clinical management self-efficacy of sixty-seven graduate physical therapy students. Results showed significantly higher total questionnaire scores and higher per question scores for first-year students compared to second-year students. The findings of this study highlight that second-year students reported lower self-efficacy in managing an unknown patient population caseload compared to first-year students, despite first-year students having less clinical education and academic experience and coursework. This trend supports a potential overestimation of self-efficacy in first-year students and greater awareness of clinical management expectations from second-year students. The implications of this research contribute to a broader understanding of differences across program years related to caseload management self-efficacy and may help direct optimal timing of learner support for academic and clinical success. In addition, a greater understanding of improving self-efficacy in physical therapy students related to clinical caseload management is needed.
Keywords: Self Efficacy; Health science education; Physical therapy education
Abbreviations: PT: Physical Therapy; PSE: Physiotherapist Self-Efficacy
Introduction
Understanding how learner characteristics may relate to student success is meaningful for educators to explore. One such learner characteristic is self-efficacy; the belief in taskspecific capabilities and confidence [1]. Student self-efficacy directly and indirectly affects academic performance and learning [2-5]. Furthermore, self-efficacy can predict student performance in clinical settings [2]. Multiple factors influence self-efficacy, such as mastery experiences, social modeling, social persuasion, and physiological responses [3]. Students with higher self-efficacy assign failures to a lack of practice, not a lack of capability, and show more persistence to overcome challenges [6].
Self-efficacy is an influential factor in students’ academic performance, positive emotions, and metacognitive learning [2,4]. Self-efficacy is strongly associated with future academic performance in both graduate dental students and freshman college students [4,5]. For physical therapy students, self-efficacy can influence learning and academic performance, and links to confidence in different clinical practice settings [2,7]. Research within health science education suggests that self-efficacy is task and situation-specific [2,7]. This research indicates that different clinical content evokes differing levels of self-efficacy regardless of general knowledge self-efficacy.
While no current comparison across physical therapy (PT) program years exists in the literature related to caseload management self-efficacy, there is evidence of increasing clinical reasoning self-efficacy in PT students over time between first-year and third-year students [8,9]. However, this previous study did not evaluate self-efficacy related to specific patient population caseload management.
Other differences in characteristics exist in the literature between PT students of different program years. First-year PT students report significantly greater stress compared to secondyear PT students [10]. Higher stress levels predict poorer academic performance in DPT students, and first-year PT students have significantly greater stress levels when compared to second-year PT students [10,11]. Interestingly, self-efficacy was a stronger predictor of student grades when compared to perceived stress levels [12].
Furthermore, there are also known differences between PT students’ clinical reasoning skills across program years [13,14]. When reasoning for case-based scenarios, first-year PT students make broad generalizations based on personal experience, whereas second and third-year students showed more developed clinical reasoning skills [13]. Therefore, understanding differences across program years related to self-efficacy may be beneficial for supporting student academic and clinical success.
Understanding that many facets of learning and performance outcomes influence self-efficacy, the authors sought to explore the clinical caseload management self-efficacy associated with novel academic content areas in our PT students. Additionally, we investigated whether there was a difference in clinical caseload management self-efficacy between first-year and second-year PT students. While the literature supports the positive relationship between self-efficacy and academic success, it also suggests that clinical exposure experience positively impacts self-efficacy in clinical content and improves over time [2,8]. Given this, it is unclear how self-efficacy may vary across program years. Understanding if a difference exists would help educators direct supportive strategies to develop self-efficacy and potentially improve student performance.
This study explored the self-efficacy level for clinical caseload management in novel clinical content for first-year and secondyear PT students. The research questions were: Is the total caseload management self-efficacy score different between firstyear and second-year PT students? Is there a difference in caseload management self-efficacy by individual question responses between first-year and second-year PT students? We hypothesized that second-year PT students would have higher self-efficacy than first-year PT students, given longer progression in the program and a prior full-time clinical experience completed, despite the level of familiarity with the clinical content topic.
Methods
This study used a non-experimental, descriptive betweensubjects quantitative research design approved by the IRB for exemption status. The study sample included first-year (DPT1) and second-year (DPT2) PT education students enrolled in the same 3-year program. All students were at the start of a patient management course for novel academic content areas (orthopaedic patient management course for DPT1 and neurological patient management course for DPT2). Subgroups were formed per program year. A nonprobability availability sampling procedure was used with a sample of convenience.
The anticipated sample size was 60 students per program year. An a priori power analysis confirmed a sufficient sample size for each research question and the associated statistical test to avoid a sampling error. For comparison analysis, a two-tailed power analysis at 80% power, a .05 alpha level, and a medium effect size (d=.5) calculated a sufficient sample size of 53 students in each group. Participant recruitment was voluntary and uncompensated, and participants understood they could withdraw from the study at any time without penalty, and informed consent was obtained. The primary researcher obtaining consent was not the course instructor for either subgroup course. Participants received information on non-discrimination based on race, color, religion, sex, age, national origin, sexual orientation, gender identity, disability, veteran status, or marital status.
Self-efficacy score was collected and calculated using the selfreported Physiotherapist Self-Efficacy (PSE) questionnaire for either neurological or orthopaedic caseload based on course enrolment [4,7]. The PSE questionnaire consisted of 13 questions on a 5-point Likert scale with established anchoring definitions as outlined in Figure 1 [4]. The PSE total score ranges from 13 to 65. Cumulative grade point average was collected from existing academic records at the time of the completion of the PSE questionnaire.
Figure 1:Physiotherapist Self-Efficacy Scale Questions. Note that “X” included the novel caseload type (orthopedic or neurological) based on enrolled course.
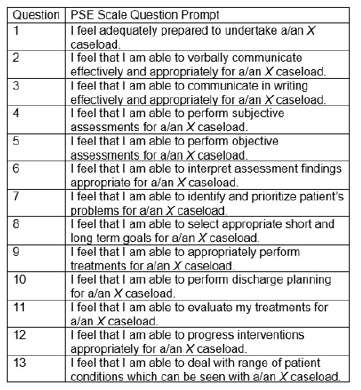
The PSE questionnaire has established rest-retest reliability and construct validity to measure DPT student self-efficacy [7]. Participants completed the PSE questionnaire at the start of their associated patient management course. The PSE total score was calculated for each participant by summing all item scores, and the median score was calculated for each question of the PSE questionnaire. Data were reviewed for accuracy and prepared for descriptive and inferential statistical analysis. Statistical analysis was conducted using IBM SPSS Statistics for Windows, Version 28. The Cronbach’s alpha score (α=0.92) for the PSE survey was determined to have high internal consistency across participant responses. Assumptions for paired samples t-test were reviewed, and in not meeting homogeneity of variances, a Mann Whitney U Test was used for group differences of PSE total score and per question score.
Results and Discussion
Sixty-seven participants consented to participate in the study, and data were analyzed (31 DPT1 and 36 DPT2; 46 female and 21 male). Sample characteristics were reported with descriptive statistics of mean and standard deviation values for cumulative grade point average for all participants and by program year in Table 1.
Table 1:GPA data for all participants and by program year.
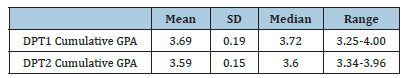
Abbreviations: GPA=grade point average; SD=standard deviation; DPT1=first-year physical therapy students; DPT2=second-year physical therapy students.
All participants answered all PSE survey questions, which allowed for a PSE total score to be calculated for each participant. One participant responded to a question with a handwritten score in between two established Likert-scale anchors, and one participant indicated two anchor scores on a single question. The anchor score for these questions was selected as the lowest Likert-scale rating in both instances for consistency.
PSE total score differences
Table 2:Descriptive data of PSE total score by program year.
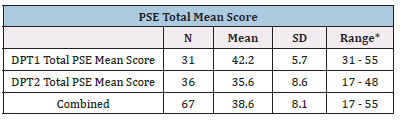
Abbreviations: SD=standard deviation; PSE=physiotherapist self-efficacy scale. *PSE Scale score ranges from 13-65 as a 13-item 5-point Likert scale.
Descriptive statistics for total PSE mean score by program year show a higher range though lower mean score for DPT2 students, as shown in Table 2. The median PSE total score was statistically significantly higher for DPT1 students (42) than for DPT 2 students (38), U=313.5, p=.002, as shown in Table 3. For overall PSE questionnaire score, first-year PT students reported significantly higher case management self-efficacy compared to second-year PT students.
Table 3:Median PSE total score by program year.
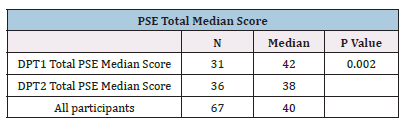
Abbreviations: PSE=Physiotherapist Self-Efficacy Scale.
PSE question score differences
A Mann-Whitney U test was performed to explore differences in PSE question scores between DPT1 and DPT2 students. Table 4 & Figure 2 present the results of the Mann-Whitney U test, showing a statistically significant difference in scores between DPT1 and DPT2 students for questions 2, 5, 8, 9, 11, 12, and 13. There was no statistically significant difference in scores between DPT1 and DPT2 students for questions 1, 3, 4, 6, 7, and 10.
Figure 2:Results of Physiotherapist Self-Efficacy scores by individual question. Q = question; *indicates significant statistical difference found.
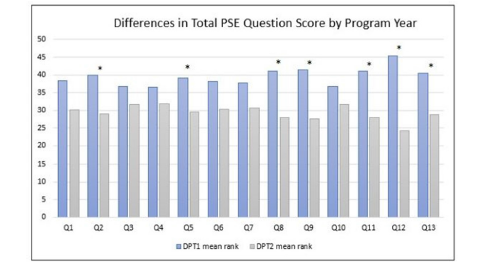
Table 4:Mann-whitney results for PSE question differences by program year.
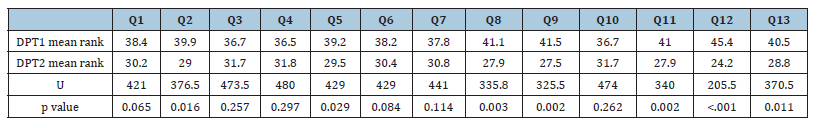
Abbreviations: PSE=physiotherapist self-efficacy scale; Q=question; U=Mann-Whitney’s U statistic.
The results do highlight several interesting factors when evaluating individual PSE questions. When considering these questions by learning domains, such as the affective domain, firstyear PT students reported greater self-efficacy with effectively communicating verbally for their caseload. The lower scores for second-year students could be related to greater contextual experience with communication challenges during patient care than first-year students. Within the psychomotor domain, firstyear PT students reported greater self-efficacy to perform objective assessments and treatments for their caseload than second-year students; however, there was no difference in perceived ability to interpret assessment findings or prioritize patient problems. Within the cognitive domain, first-year students reported higher self-efficacy in selecting goals, evaluating treatment effectiveness, progressing treatments, and overall ability to deal with the range of patient conditions than second-year students.
Conclusion
This study explored the potential differences in caseload management self-efficacy between first and second-year PT students. While it was hypothesized that second-year PT students would demonstrate higher efficacy, notably the findings of this study showed that first-year PT students in the program reported significantly higher caseload management self-efficacy than secondyear students despite completing less academic coursework and no prior clinical education experiences. Interestingly, this trend was inconsistent across individual PSE questions. Despite academic content being novel to both years, there may be self-perceived differences in managing a neurological caseload with less likelihood of exposure outside the program. Self-efficacy increases by modelling tasks and psychomotor practice [2]. Furthermore, selfefficacy of specific clinical practice areas has effectively increased with case and task simulation [7]. None of the participants had any formal practice of the clinical content assessed by the PSE. Most second-year students’ prior clinical experiences were in orthopaedic settings. The researchers acknowledge that the study did not account for participants’ backgrounds or exposure to content outside the curriculum. Students can overestimate their clinical abilities compared to others in their cohort if they have a brief exposure to a simulation of such experiences [15]. Therefore, it could be proposed that PT students who have had greater exposure to orthopaedic content through previous personal experiences with PT, employment as PT aides, or through previous coursework and social media may score higher on the PSE than expected.
Beyond student experiences outside the program, other considerations may help explain the present research’s findings. General self-efficacy scores have increased with time in a physical therapy program [9]. The current study explored student selfefficacy of clinical case load management in specific novel patient care areas, which has yet to be researched. Furthermore, prior research measured physical therapy student self-efficacy on numerous scales under multiple conditions. Prior research also suggested that self-efficacy tools use a 100-point Likert scale to increase sensitivity and reliability [1]. The PSE scale used in the current study was a 5-point Likert scale, which may have narrowed the sensitivity of our findings.
In addition, comparing multiple study results that used varying scales is challenging as questions are often not phrased similarly. A self-efficacy scale aims to evaluate intention rather than capability and, therefore, should not use questions phrased as “I will” but instead explore a student’s perceived potential to complete a task [1]. Previous studies that found an increase in physical therapy student self-efficacy have utilized such intention constructs,9 thus making a comparison to the current study challenging.
Exploring the threats to internal and external validity related to a descriptive correlational design is vital. The study’s focus on graduate physical therapy students at a single higher educational institution and the absence of random assignment limits the external validity of generalizing to a larger population. This limitation was addressed within the non-experimental study design by the confirmation of similar relevant traits, such as mean admission grade point average and sex distribution, between the study sample and the target population, which reduced the likelihood of ascertainment bias.
Perceived self-efficacy can vary with contextual factors such as social and learning environments [1]. We speculate that firstyear students may have overestimated their self-efficacy, given less awareness of expectations and experience in the classroom and clinical situations [3]. Further exploration of this trend across program years is warranted within and across specific patient caseloads. Given that self-efficacy influences academic performance by promoting metacognitive learning and positive emotions [3], further understandings of improving self-efficacy in PT students related to clinical caseload management would be valuable for educators in supporting student academic and clinical success.
Acknowledgements
None
Conflict of Interest
The authors have no financial interest or conflict of interest to declare.
References
- Bandura A (2006) Guide for constructing self-efficacy scales. In: Pajares F, Urdan T (Eds.), Self-efficacy Beliefs of Adolescents Information Age Publishing 5: 307-337.
- Hayat AA, Shateri K, Amini M, Shokrpour N (2020) Relationship between academic self-efficacy, learning-related emotions, and metacognitive learning strategies with academic performance in medical students: a structural equation model. BMC Medical Education 20(1): 76.
- Ainscough L, Foulis E, Colthorpe K, Zimbardi K, Robertson-Dean M, et al. (2016) Changes in biology self-efficacy during a first-year university course. CBE Life Sciences Education 15(2): ar19.
- Jones A, Sheppard L (2012) Developing a measurement tool for assessing physiotherapy students’ self-efficacy: A pilot study. Assessment & Evaluation in Higher Education 37(3): 369-377.
- Chemers MM, Hu L, Garcia BF (2001) Academic self-efficacy and first year college student performance and adjustment. Journal of Educational Psychology 93(1): 55-64.
- Kurbanoğlu I, Akim A (2010) The relationships between university students’ chemistry laboratory anxiety, attitudes, and self-efficacy beliefs. Australian Journal of Teacher Education 35(8): 48-59.
- Van Lankveld W, Jones A, Brunnekreef JJ, Seeger JPH, Bart Staal J (2017) Assessing physical therapist students’ self-efficacy: Measurement properties of the Physiotherapist Self-Efficacy (PSE) questionnaire. BMC Medical Education 17(1): 250.
- Bandura A (1977) Self-efficacy: toward a unifying theory of behavioral change. Psychological Review 84(2): 191-215.
- Venskus DG, Craig JA (2017) Development and validation of a self-efficacy scale for clinical reasoning in physical therapists. Journal of Physical Therapy Education 31(1): 14-20.
- Bogardus JM, Blackinton M, Litwin B, Nelson TM, Mitchell K (2021) Depression, anxiety, and stress in doctor of physical therapy students: Analysis of incidence and lived experiences. Journal of Physical Therapy Education 35(3): 251-257.
- Flower DW, Bernard A (2020) Make changes early! High stress levels predict lower academic performance in first-year physical therapy students: A pilot study. Internet Journal of Allied Health Sciences and Practice, 18(4): Article 15.
- Crego A, Carrillo-Diaz M, Armfield JM, Romero M (2016) Stress and academic performance in dental students: The role of coping strategies and examination-related self-efficacy. Journal of Dental Education 80(2): 165-172.
- Gilliland SJ (2014) Clinical reasoning in first- and third-year physical therapist students. Journal of Physical Therapy Education 28(3): 64-80.
- Black B, Lucarelli J, Ingman M, Briskey C (2016) Changes in physical therapist students’ self-efficacy for physical activity counseling following a motivational interviewing learning module. Journal of Physical Therapy Education 30(3): 28-32.
- Jones A (2011) Self-efficacy and clinical performance: A physiotherapy example. Advances in Physiotherapy 13(2): 79-83.
© 2026 Pogemiller Kelly. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






