- Submissions

Full Text
Advances in Complementary & Alternative medicine
Exploring Yoga Therapists’ Perceptions of the Impact of Therapeutic Interventions on Health: A Call for Interprofessional Collaboration
Jennifer Vasquez1* and April C Bowie Viverette2
1School of Social Work, Texas State University, USA
2Department of Social Work, University of North Alabama, USA
*Corresponding author:Jennifer Vasquez, PhD, LCSW-S, Texas State University, 601 University Drive, San Marcos, TX 78666, USA
Submission: January 31, 2026;Published: February 09, 2026

ISSN: 2637-7802 Volume 9 Issue 2
Abstract
Yoga therapy is a personalized, integrative approach rooted in traditional Indian medicine and designed to complement modern allopathic healthcare. Although its benefits are widely supported anecdotally, limited empirical research examines yoga therapists’ experiences with yoga therapy across the pañcamaya model’s multidimensional framework. This mixed-methods study used univariate analysis, bivariate analysis with Fisher’s exact test and the freeman-Haltan extension, and thematic analysis to explore how yoga therapists (n=69) perceive the impact of personal therapeutic yoga practices on various health conditions and life dimensions. Quantitative findings showed varied therapist perspectives on the benefits of a personal yoga therapy practice. Qualitative results revealed yoga therapy goals across the tri krama model: Cikitsā krama goals are therapeutic and focus on healing and recovery (1) pain relief and physical healing, (2) emotional and mental health, (3) holistic balance, and (4) functional recovery; Rakṣaṇa krama goals protect and preserve, supporting ongoing wellness (1) physical strength and graceful aging, (2) mental and emotional stability, and (3) self-awareness and sustainable routines; and Śikṣaṇa krama goals develop refinement, promoting growth and learning (1) spiritual development, (2) study of yogic philosophy and sacred texts, and (3) integration of yoga into daily life and work. Therapists’ experiences indicate that yoga therapy supports holistic well-being throughout the system, offering a comprehensive and adaptable approach to health and personal development. We build on these findings by offering suggestions for interprofessional collaboration among healthcare providers.
Keywords:Yoga therapy; Yoga therapist; Health; Healing; Pañcamaya model
Introduction
Yoga therapists’ perceptions of the impact of therapeutic interventions on health
Yoga is an ancient practice rooted in traditional Indian texts, including the Vedas, Upanishads, the Bhagavad Gītā, and Patañjali’s Yoga Sūtras, and has been practiced in Eastern societies for thousands of years [1]. The term yoga is a Sanskrit word meaning to join or unite, referring to the mind and body [1,2]. This unification is achieved through the fundamental aspects of yoga, which include breath work (pranayama), movement (asana), and meditation (dharana, dhyana, and samadhi) [3]. Yoga therapy is a holistic and comprehensive practice that uses techniques and methods to bring balance to the mind, body, and spirit [4]. This balance can be advanced beyond traditional healthcare providers through multidisciplinary or interdisciplinary approaches that treat these conditions through interprofessional collaboration. Understanding yoga therapists’ perspectives on how their personal practice affects client health and overall well-being can promote patient-centered collaborative care. Previous research has shown a positive connection between provider perceptions of their practice and client health, communication, patient satisfaction, perceived receipt of quality of care from their provider, positive clinical outcomes, client treatment adherence, and provider burnout [5,6].
This study aims to enrich existing research by analyzing the experiences and perspectives of yoga therapists themselves and presenting suggestions for interprofessional collaboration that can enhance outcomes. Interprofessional collaboration is well established in the literature and has been described as a mandate for optimal, high-quality healthcare [7-10]. This differs significantly from multidisciplinary and interdisciplinary approaches to healthcare (Smith & Clouder, 2010). McLaney et al. [11] suggest that interprofessional collaboration go beyond individual provider attributes and instead involve coordinated, partnered, and communicative efforts to meet individual needs. A “blurred” or “blending” approach, whereby disciplines use a transdisciplinary orientation to assessment, treatment, intervention, and collaboration, which requires some cross-training, is holistic [12] (Kilgore & Langford, 2009). They suggest an action-based stance of active collaboration, shared provider decision making, and shared responsibility to advance quality healthcare. This requires healthcare professionals to have a deeper understanding of each other’s roles and to engage in effective teamwork toward effective care outcomes [13]. According to Iachini et al. [14], interprofessional care requires interdependence, newly created professional activities, flexibility, collective ownership of goals, and reflection on the process. An optimal level of interdependence requires a clear understanding of each provider’s role.
For instance, providers may not be fully aware of other providers’ roles or the techniques used within those roles to work with a particular chronic condition; thus, interdependence can be fostered through knowledge and understanding. This can result in the maximum use of each provider’s skills to address the conditions we have studied [14]. Newly created professional activities suggest that providers include yoga therapists, requiring a partnership with communication about the client or patient [14]. Flexibility allows each healthcare provider to engage in basic information exchange with a client or patient relevant to yoga therapy and vice versa; this is not practicing outside of scopes of practice, but rather a basic acknowledgment through providing basic information while awaiting the expert provider intervention, which can be helpful [14]. Additionally, sharing ideas, agreeing and disagreeing on care or treatment plans, and evaluating goals align with interprofessional collaboration through collective ownership of goals [14]. Finally, providers reflecting on their practice with each other, rather than only with like professionals, is self-reflection on the process [14]. While this study examined yoga therapists’ perspectives and practice experiences, there is an opportunity to contribute to the literature by using these results to inform a holistic approach to working with individuals with the physical and psychological conditions under study, as it may be unclear how to interprofessionally collaborate concerning yoga therapy.
We present a discussion of an application of Iachini’s model [14] to yoga therapists and other healthcare providers who work with diabetes, cancer, back pain, headaches, depression, anxiety, Post-Traumatic Stress Disorder (PTSD), stress, arthritis, Multiple Sclerosis (MS), asthma, obesity, and menopause. This mixedmethods study examined the perspectives of yoga therapists, identifying how yoga therapy contributes to health and overall well-being and how yoga therapists can work with other healthcare professionals in the spirit of interprofessional collaboration. Yoga therapists were recruited by emailing a flyer to yoga therapy training programs certified by the International Association of Yoga Therapy (IAYT). A total of 69 yoga therapists participated in the study and completed an online survey with both closed- and openended questions to capture the full depth of their interpretations. Bivariate and thematic analyses were used in this study. Quantitative results showed that yoga therapists have varying perceptions of the effects of their personal practice on health problems. Qualitative results indicated that participants’ yoga therapy goals support healing and recovery, maintaining current health and thriving, as well as continued learning, growth, and self-discovery in their yoga therapy practice. This study supports the growing body of literature on therapeutic yoga as an effective and beneficial integrative approach to traditional interventions.
Literature Review
Yoga Therapy
Yoga therapy is a complementary healthcare practice that embodies a holistic approach, integrating physical and psychological benefits [15,16]. It empowers individuals to use the body to regulate the mind and support the recovery journey, with the overarching goal of alleviating suffering through the body, mind, and environment [15,16]. Sullivan and colleagues define yoga therapy as the “process of empowering individuals to progress toward improved health and well-being through the application of the teachings and practices of yoga” (2017, pg. 1). Yoga comprises several core components, including movement, breath, and attention, that work together within a structured practice to promote physical and psychological well-being [17]. Structure is a core element of yoga therapy, playing a crucial role in its therapeutic effectiveness [18]. Movement refers to the intentional execution of postures and sequences designed to treat the client while improving mobility, flexibility, and strength [17]. When paired with breathwork, movement supports physical engagement and serves as a tool for directing attention, thereby enhancing interoceptive and proprioceptive awareness [17]. Heightened awareness helps individuals become more attuned to their internal processes, which is essential for emotional regulation [17]. Lang and colleagues emphasize that yoga therapy involves active, deliberate regulation of attention, typically directed toward the breath, to enhance mindfulness and self-awareness (2021). Additionally, meditation within yoga therapy increases selfawareness and supports self-regulation, thereby improving mental health and overall well-being [19].
Tri krama model: Cikitsa, raksana, siksana
Yoga’s principles approach health from a perspective that differs from that of Western allopathic medicine. In the yogic tradition, health encompasses three levels: Cikitsa, Raksana, and Siksana [20]. The first level, Cikitsa, is where health begins [20]. In this state of Cikitsa, you begin to address the presenting problem of pain, illness, and/or suffering [21]. Raksana, the second level, is where the client moves from the healing phase into the maintenance phase [20]. During Raksana, the focus is on building strength and refining core yoga techniques [20]. The final stage of health, Siksana, is the pinnacle of yoga practice. Siksana embodies the utmost refinement and personal growth in yoga [20]. This stage involves delving into the deepest layers of yoga practice to achieve the highest realization [20]. The tri krama model reflects yoga’s holistic and traditional view of healing. The Tri Krama model does not just symbolize the absence of disease but the continuous process of healing and growth that leads to sustained well-being.
Pañcamaya model
Pañcamaya is a foundational model in therapeutic yoga that offers a holistic framework for understanding human experience [22]. It describes five interrelated dimensions that together constitute a person’s totality [22]. These dimensions are not isolated but deeply interconnected, so any shift, whether physical, emotional, or mental, can ripple across all layers of being [22]. The first dimension, annamaya, refers to the physical body [22]. The second, prāṇamaya, represents the breath, which governs the flow of prana throughout the system [22]. Manomaya, the intellect dimension, encompasses thoughts and processing. The fourth dimension, vijñānamaya, is the personality dimension associated with perception, communication, and individuality [22]. Lastly, ānandamaya, the dimension of emotion, represents some of the innermost layers of the human system [22]. In therapeutic yoga, practices are designed to work across dimensions to provide holistic support and well-being. This model emphasizes that health goes beyond the presence or absence of disease and encompasses balance among all human systems.
Health conditions treated by therapeutic yoga
Yoga has become an alternative healing approach for a variety of physical and psychological health conditions. Yoga combines movements, breathing, and meditation techniques, sequenced in a unique manner, to address a specific health diagnosis or symptoms. Common health conditions that respond strongly to yoga include depression, anxiety, and back pain. The impact of yoga therapy on common physical and psychological ailments has been described in the literature.
Physical ailments: Yoga therapy interventions can be used to treat a wide range of health problems because of their flexibility and emphasis on individual needs. Yoga therapy improves flexibility, strength, and mobility while being personalized to address an individual’s current condition [15]. Kishida and associates reported that yoga could directly lead to improved health and wellbeing outcomes related to physical function (2018). Shohani and associates found that yoga is a useful treatment for diseases such as multiple sclerosis, asthma, hypertension, and osteoarthritis (2018). Additionally, Forseth and colleagues found that even an eight-week therapy program can significantly reduce bodily inflammation (2022). Yoga therapy is a modality that can accommodate a wide variety of health disturbances due to its personalized nature, allowing for significant variability in treatment options. The effectiveness of yoga therapies in supporting health and managing chronic disease may be best evaluated using outcomes related to survival, longevity, and disease prevention. Yoga-based interventions have been shown to influence biological pathways associated with healthy aging, metabolic regulation, and cellular resilience, which are central to reducing chronic disease risk [22]. Research on gene regulation and epigenetic mechanisms highlights the importance of longevity-associated genes in appetite control, cellular repair, and protection against senescence and apoptosis, underscoring the relevance of biological markers for evaluating the physiological impact of lifestyle and therapeutic interventions, including yoga [23-25].
Psychological Ailments: Yoga therapy is widely recognized as a significant intervention for psychological disorders, particularly anxiety, depression, and Post-Traumatic Stress Disorder (PTSD). An essential component of yoga therapy is cultivating the ability to focus and regulate the mind and nervous system [1]. This enhanced self-regulation has been shown to alleviate symptoms of depression and other mental health disorders [1]. Another emotional benefit of yoga therapy is that it supports mindfulness, helping clients achieve a sense of calm, increase self-compassion, and reduce stress [26]. These benefits are achieved through the mind-body connection [27]. Yoga therapy facilitates the mind-body connection by creating a unique collaboration between psychological and physiological processes [28]. In a 2021 study by Fitzgerald and colleagues, yoga therapy significantly reduced psychological factors such as anger, fatigue, and tension while promoting relaxation and stress relief. Participants self-reported positive mood changes, enhanced wellbeing, and improved self-esteem [15].
Similarly, a 2022 study by Forseth and associates found that a yoga intervention significantly reduced symptoms of stress and depression. Nanthakumar conducted a literature review to analyze current trends linking yoga therapy interventions to psychological well-being (2020). Nanthakumar’s results supported the previously mentioned studies, as the reviewed studies reported reductions in anxiety, depression, and stress (2020). Nanthakumar found that yoga therapy interventions increased clients’ resilience by altering brain activity, promoting improved moods, and helping them release grief, anger, and frustration in a healthy way (2020). Nanthakumar also found that the yoga interventions presented no adverse effects, making it a safe treatment option for clients struggling with mental illnesses (2020). Specific methods of yoga therapy are also effective for treating mental illness and can be tailored to specific populations. A study by Heeter and colleagues examined the potential benefits of technology-assisted delivery of a meditation intervention among hospice and palliative care workers (2017). This approach increased accessibility for a population experiencing high-stress environments and burnout [19]. The results showed improved interoceptive awareness, reduced burnout and compassion fatigue, and overall support for professional quality of life [19]. This is just one way to use yoga therapy to target specific populations through unique means.
Another aspect of yoga therapy is tailored to trauma and PTSD. Yoga therapy has been deemed an effective intervention for managing PTSD [2,29]. A 10-week yoga intervention significantly reduced PTSD symptoms among women with treatment-resistant PTSD [30]. One form of trauma-specific yoga intervention is trauma-sensitive yoga at trauma centers [31]. This approach has been reported to confer biopsychosocial benefits, as perceived by study participants with both childhood trauma and a current PTSD diagnosis [32]. Yoga therapy interventions, as complementary and integrative health approaches aimed at managing PTSD symptoms, have been found effective in reducing PTSD severity and improving co-occurring symptoms such as depression, anxiety, anger, sleep problems, and psychosocial disabilities [18]. Overall, yoga therapy shows promising results as an adjunct or alternative treatment for a wide range of psychological ailments. Therefore, it is vital for other healthcare providers to recognize the benefits of yoga therapy to inform interprofessional collaboration. Yoga therapy, part of the field of integrative medicine, has been increasingly recognized by other healthcare providers as an adjunct to address many health conditions. While some providers may prescribe or suggest a referral, the literature suggests there is likely a need for interprofessional collaboration between yoga therapists and other providers of an individual’s care.
Methods
This concurrently designed mixed-methods study was approved by the lead author’s institutional review board. Yoga therapists were recruited through International Association of Yoga Therapists (IAYT)-certified yoga therapy schools. The researchers’ flyer was distributed to the institute’s network of yoga therapists via the yoga school’s email system. To participate, therapists selfidentified as yoga therapists. The only exclusion was that those who did not identify as yoga therapists were not included in the study. The research flyer included references to a Qualtrics survey, in which participants could scan a barcode or click a link to begin the voluntary survey. The survey consisted of sociodemographic questions about the participant, closed-ended questions about their perceptions of the effects of therapeutic yoga interventions on physical and mental conditions, and closed-ended questions about the perceived impact of these interventions on the 5 pañcamaya domains.
Participants were asked to rate their perceptions of the impact of therapeutic Viniyoga interventions (i.e., asana, pranayama, meditation, chanting, nyasa) on each of the 5 pañcamaya domains (Annamaya/physiology, Prāṇamaya/energy, Manomaya/mind, Vijñānamaya/personality, and Ānandamaya/feelings) using a five-point Likert scale (1=not at all effective, 2=slightly effective, 3=moderately effective, 4=very effective, 5=extremely effective). Participants also rated, using a six-point Likert scale (1=I did not treat this condition, 2=not at all effective, 3=slightly effective, 4=moderately effective, 5=very effective, 6=extremely effective), the perceived impact of these interventions on physical conditions, including hypertension, diabetes (types I, II, and pre-diabetes), cancer, back pain, headaches, arthritis, multiple sclerosis, asthma, obesity, and menopause. Mental health conditions (i.e., stress, depression, anxiety, post-traumatic stress disorder) were also assessed. Participants were also asked open-ended questions about their experiences and perceptions of yoga’s impact across various domains and on their physical and mental health. Example questions included: “Tell us how you feel about yoga interventions and common physical ailments or chronic health conditions,” and “Tell us how you feel about yoga interventions and manomaya/ mind.”
Data analysis
Univariate analysis was completed, and missing cases were imputed. Multiple sclerosis and diabetes were excluded from the bivariate analysis because therapists who did not work with these conditions were overrepresented among the missing cases. The distribution of continuous data was normal. Data were analyzed using IBM SPSS version 29.0. Qualitative data were analyzed using thematic analysis and NVivo 15. The six steps of thematic analysis were followed, including Phase 1: Familiarization with the data, Phase 2: Generating initial codes, Phase 3: Searching for themes, Phase 4: Reviewing themes, Phase 5: Defining and naming themes, and Phase 6: Producing the report [33]. In Phase 1, researchers read all open-ended responses describing yoga therapists’ personal practices in the context of Cikitsā (therapeutic), Rakṣaṇa (preventive), and Śikṣaṇa (developmental) goals. Notes and initial ideas were recorded in analytic memos. Observations included frequent mentions of pain, emotional regulation, daily routines, and spiritual reflection. In Phase 2, in vivo and descriptive coding were used. Examples of initial codes include “relieve back pain” coded as ‘pain relief’, “daily practice keeps me centered” coded as ‘mental balance’, “I study the Gita every morning” coded as ‘philosophical study’, “keeping mobility in aging” coded as ‘aging gracefully’, and “deepening my awareness” coded as ‘spiritual growth’. In Phase 3, codes were clustered by similarity within each goal area.
Cikitsā codes were grouped into pain relief, emotional healing, and functional recovery; Rakṣaṇa codes into daily habits, physical maintenance, and emotional steadiness; and Śikṣaṇa codes into spiritual insight, study, and integration into life. During Phase 4, all themes were cross-checked against the raw data. Themes were removed if they were too vague (e.g., “healthy living”) or overlapped significantly with stronger themes (e.g., “alignment” folded into “functional recovery”). During Phase 5, final themes and definitions were created. In Phase 6, these themes were integrated into the Joint Display Table, providing depth and insight under the “Qualitative Themes” column. Interpretive narratives were developed that linked themes to quantitative dimensions (e.g., back pain to “pain relief” in annamaya). Direct quotes were used in the full report to support each theme [34-39].
Results
Quantitative strand
Table 1 presents descriptive and univariate analyses of the results. The mean age of participants was 41.94 years (SD=9.54). Most participants were yoga therapists (98.6%) and IAYTassociated (97.1%). Twenty-eight percent were Viniyoga-trained. Ninety-seven percent were female, and 44.9% held a master’s degree. Most (89.9%) identified the United States as their practice location, with 47.8% practicing in the suburbs. Most (75.4%) were primarily in private practice, 79.7% practiced both online and in person, and 95.7% endorsed personal practice. The sample’s median annual household income was $100,000 to $149,999..
Table 1:Sociodemographics, Sample Characteristics, & Univariate Statistics (n=69).
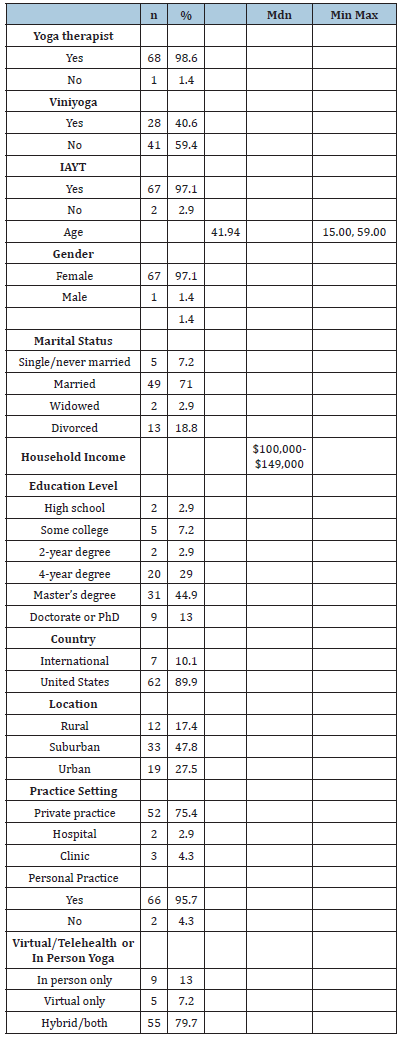
Univariate analysis of therapists’ practice in relation to the pañcamaya model & how regularly they notice a change along each of the 5 dimensions of the human system: Participants were asked about their personal practice in relation to the pañcamaya model and how often they notice changes in clients’ practice across the 5 dimensions of the human system. Univariate analysis showed that most participants usually or often notice changes in annamaya/physiology (94.2%), manomaya/mental (92.8%), prāṇamaya/energetic (66%), ānandamaya/emotional (85.5%), and vijñānamaya/personality (72.5%).
Univariate analysis of health problems and bivariate analysis between yoga therapists’ perceived self-change in doing their personal practice regularly and the perceived Effectiveness of Their Practice: Table 2 presents the results of univariate and bivariate analyses on yoga therapists’ perceived self-change in maintaining regular personal practice and perceived effectiveness of that practice. Therapists were asked about their personal practice regarding 15 presenting problems and whether they consider yoga therapy generally very effective, somewhat effective, or not effective. The following frequencies represent the number of therapists who identified with each. Some rated the following as very effective: 84.1% of participants rated back pain as very effective in their personal practice, as did 78.3% for anxiety and 87.0% for stress. Somewhat effective ratings were attributed to depression (47.8%) and menopause (53.6%). Headaches (85.5%), cancer (87.0%), PTSD (76.8%), arthritis (79.7%), asthma (89.9%), and obesity (87.0%) were rated as not applicable/I have never worked with this problem. No conditions were rated as not very effective. Associations between yoga therapists’ perceived self-change from regular practice and the perceived effectiveness of their practice across 15 health-related presenting problems were assessed using fisher’s exact test with the freeman-Halton extension.
Results (Table 2) showed several statistically significant associations. Vijñānamaya/personality was significantly associated with the following conditions: cancer (p=.002), headaches (p=.010), depression (p<.001), anxiety (p=.019), stress (p<.001), and arthritis (p=.020). Statistically significant associations were also found with annamaya/physiology for asthma (p=.009), back pain (p=.031), PTSD (p=.002), and hypertension (p=.002), and with prāṇamaya/energetic for depression (p=.026) and asthma (p=.010). Manomaya/mental was associated with depression (p=.048), stress (p=.014), and arthritis (p=.023). Finally, ānandamaya/feelings was associated with anxiety (p=.022), PTSD (p=.021), stress (p<.001), arthritis (p=.012), asthma (p=.011), cancer (p=.004), and menopause (p=.047). Regarding the vijñānamaya/personality dimension, participants usually or often had not worked with cancer or arthritis and did not rate the model’s effectiveness. They usually or often noticed a change when applying the pañcamaya model to headaches and depression, and perceived it as somewhat effective in addressing these conditions. However, therapists usually or often noticed a change in anxiety and stress and perceived the model as very effective in addressing these conditions.
Table 2:Univariate Analysis of Health Problems and the Bivariate Associations between Yoga Therapists’ Perceived Self- Change in Doing Their Personal Practice Regularly and the Perceived Effectiveness of Their Practice (n=69).
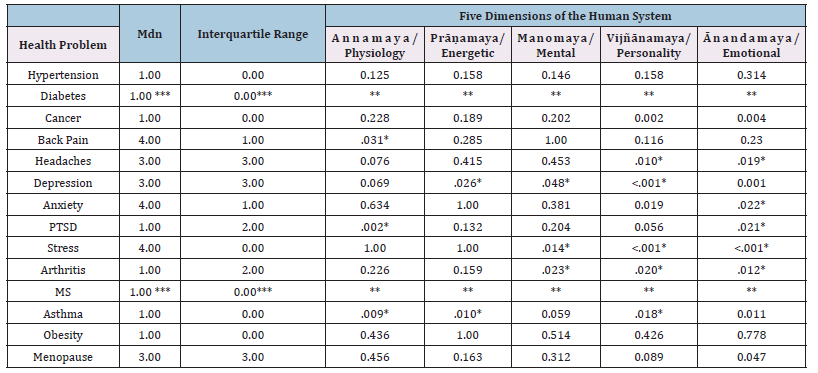
Note. p* denotes statistical significance **denotes variable removed from bivariate analysis ***diabetes n=44, multiple sclerosis n=44.
The manomaya/mental dimension results showed that a change was usually or often observed with depression, and it was somewhat effective. However, regarding stress, a change was often observed, and it was very effective. Regarding this dimension, participants had usually or often not worked with arthritis and did not rate their perceptions of the model’s effectiveness. Annamaya/ physiology results showed that therapists usually or often notice changes in clients’ back pain and found the model very effective in addressing it. Participants usually or often had not worked with hypertension or asthma and did not rate the model’s effectiveness for these conditions. The ānandamaya/feelings dimension results showed that participants usually or often did not notice changes related to cancer, arthritis, asthma, or PTSD. Therapists who have worked in this dimension with headaches usually or often perceived the model to be somewhat effective in addressing headaches and somewhat effective in addressing depression and menopause, whereas they perceived changes in clients’ anxiety and stress as very effective. Finally, in the prāṇamaya/energetic dimension, the therapist perceived a notable change in the client’s depression (p=.026) and considered the model somewhat effective in addressing it. However, they had usually or often not worked on asthma in this dimension and did not rate the model’s effectiveness for this condition.
Qualitative strand
Themes: The mixed-methods study used a convergent design that integrated qualitative questions into a Qualtrics survey alongside the quantitative strand. Yoga therapists were asked to briefly list any goals they’ve worked on in their personal practice, using the Tri Krama framework: Cikitsā, Rakṣaṇa, and Śikṣaṇa.
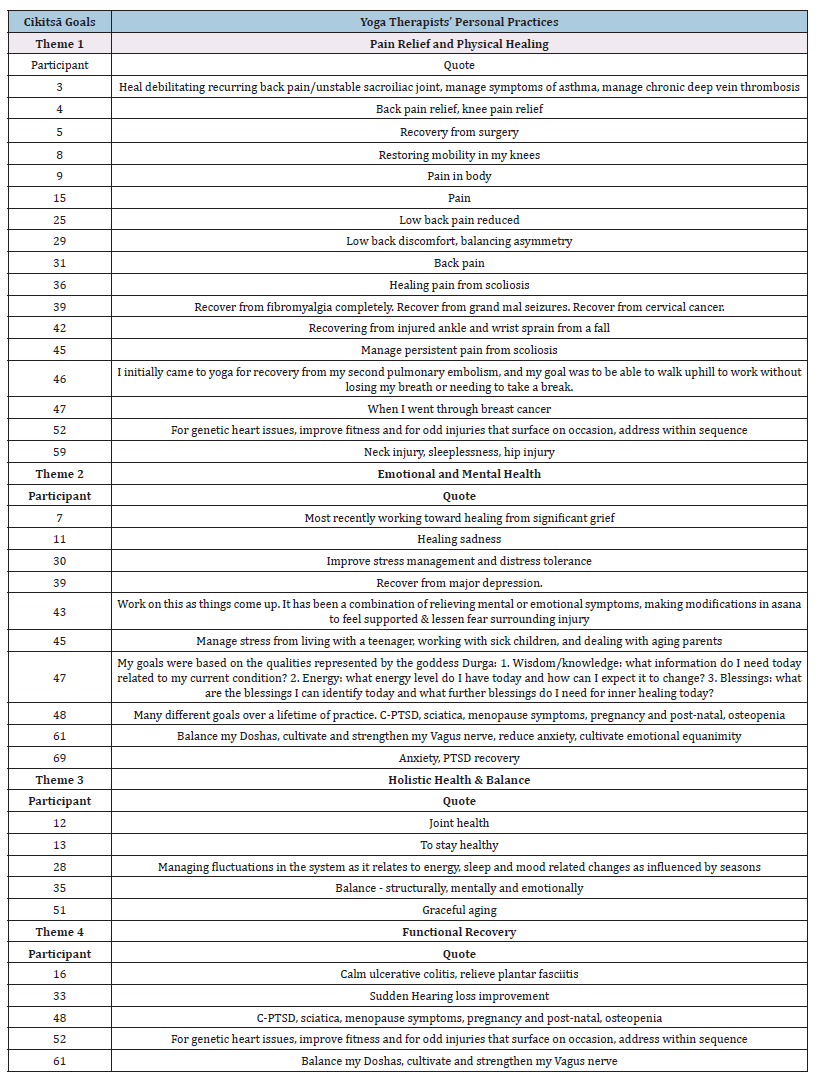
Cikitsā Goals: The first of these three traditional frameworks is cikitsā. Cikitsā is healing, recovery from illness, injury, or imbalance. It is the first stage of the healing journey. In the cikitsā stage, the focus is on relieving symptoms, restoring basic health, and bringing the body-mind system back into balance. It helps someone feel better and resume normal function. It’s where yoga tools are used therapeutically to address a specific condition or disruption. Yoga therapists identified four themes from their personal practice as cikitsā goals: 1. Pain relief and physical healing, 2. Emotional and mental health, 3. Holistic health and balance, and 4. Functional recovery. When describing the most common themes in the cikitsā stage of pain relief and physical healing, participants focused on pain reduction and injury recovery. Many participants described back pain, “Heal debilitating recurring back pain” (participant 3). Others identified recovery from surgery, “Recovery from surgery” (participant 5), or from injury, “Recovering from an injured ankle and wrist sprain from a fall” (participant 42).
Yoga therapist participants reported themes related to emotional and mental health goals, including stress management, emotional well-being, grief, and mental resilience. Participant goals included “Working toward healing from significant grief” (participant 7), “Healing sadness” (participant 11), and “Improve stress management and distress tolerance” (participant 30). Holistic health and balance themes included participant goals for overall wellness, balance, longevity, and vitality. Participants described goals such as “Managing fluctuations in the system as it relates to energy, sleep, and mood-related changes as influenced by seasons” (participant 28), “Balance - structurally, mentally, and emotionally” (participant 35), and “Graceful aging” (participant 51). Goals related to the theme of functional recovery focused on managing or recovering from specific conditions. Yoga therapist participants reported goals such as “Calm ulcerative colitis, relieve plantar fasciitis” (participant 16), “Sudden hearing loss” (participant 33), and “C-PTSD, sciatica, menopause symptoms, pregnancy and postnatal, osteopenia” (participant 48).
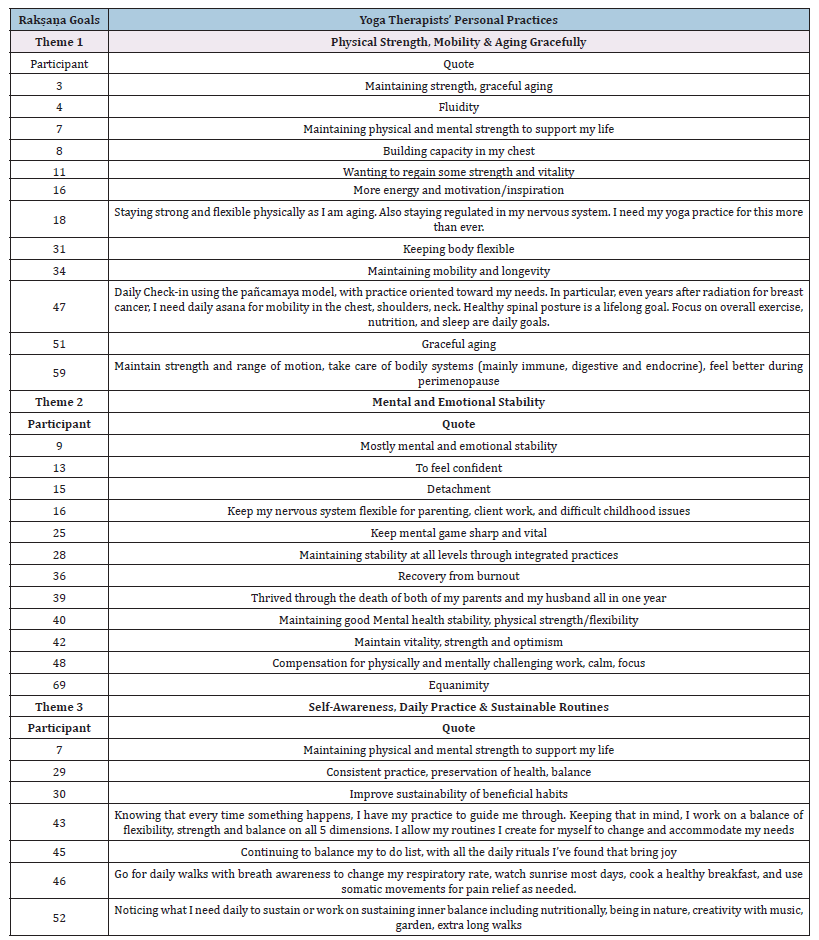
Rakṣaṇa Goals: Rakṣaṇa goals support maintenance and thriving. These include protecting and preserving health and balance. In yoga therapy, after recovery, the focus shifts to maintaining progress and preventing setbacks. It’s about building resilience and preserving what’s been gained, both physically and mentally. Yoga therapists support the client in thriving, not just surviving. The rakṣaṇa stage often involves establishing daily routines, consistent practice, and lifestyle habits that support longterm wellness. Yoga therapists identified three themes regarding rakṣaṇa goals in their personal practices: 1. Physical strength, mobility, and graceful aging; 2. Mental and emotional stability; and 3. Self-awareness, daily practice, and sustainable routines. The first theme, physical strength, mobility, and graceful aging, centers on preserving or improving physical health, mobility, and vitality as people age well. Several participants described graceful aging as a rakṣaṇa goal. Examples of rakṣaṇa goals from participants’ personal practices include “Maintaining strength, graceful aging” (participant 3), “Staying strong and flexible physically as I am aging” (participant 18), and “Graceful aging” (participant 51).
Others identified flexibility or mobility as a goal, including “Keeping body flexible” (participant 31), “Maintaining mobility and longevity” (participant 34), and “Maintain strength and range of motion” (participant 59). Explaining the theme of mental and emotional stability, participants aim to cultivate emotional resilience, mental clarity, and tools for processing life’s challenges. These goals include “Mostly mental and emotional stability” (participant 9), “To feel confident” (participant 13), and “Keep mental game sharp and vital” (participant 25). Participants shared goals related to self-awareness, daily practice, and sustainable routines. These goals focused on maintaining healthy routines, daily rituals, and inner balance through mindful living and yoga practice. Participants stated their personal rakṣaṇa goals were “Consistent practice, preservation of health, balance” (participant 29), “Improve sustainability of beneficial habits” (participant 30), and “Continuing to balance my to-do list with all the daily rituals I’ve found that bring joy” (participant 45).
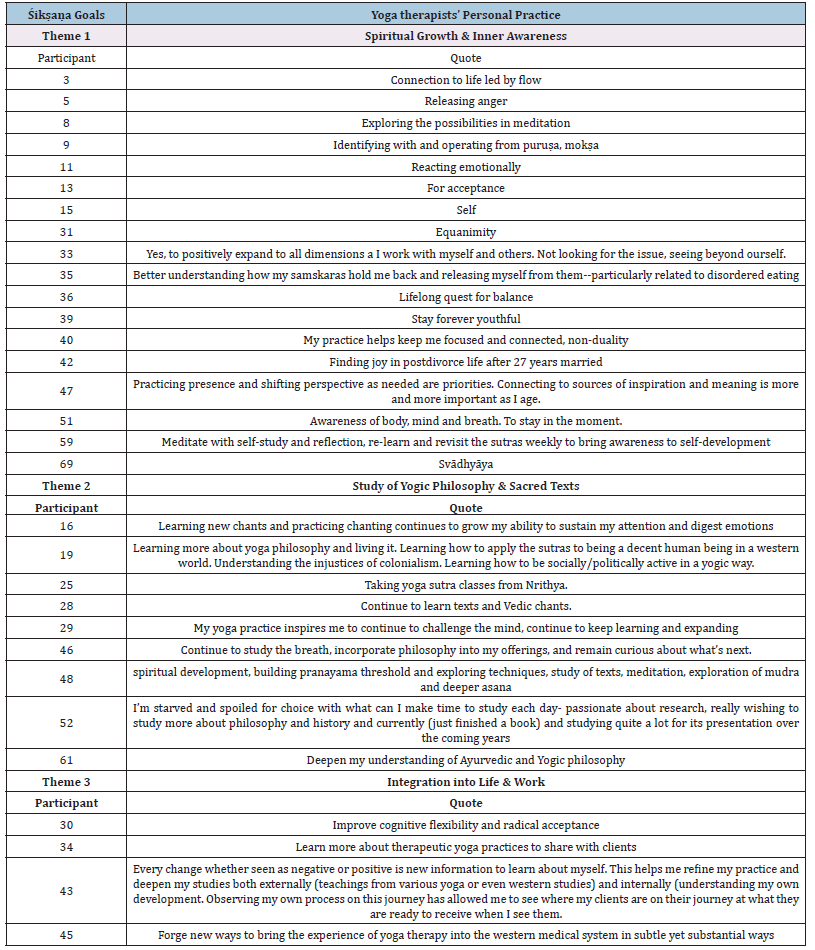
Śikṣaṇa Goals: Śikṣaṇa goals center on learning, growth, and self-discovery. Once stable and thriving, clients may feel drawn to explore deeper questions, expand their self-awareness, or refine their path. This stage focuses on personal development through yoga, not because anything is wrong, but because there’s a desire to grow. Participants in this study identified three themes related to Śikṣaṇa: 1. Spiritual growth and inner awareness, 2. Study of yogic philosophy and sacred texts, 3. Integration into life and work. They described goals related to spiritual growth and inner awareness, focusing on deepening their spiritual practices, connecting with their inner selves, and exploring higher states of consciousness. Participants reported goals from their personal practices, including “Connection to life led by flow” (participant 3), “Equanimity” (participant 31), and “Svādhyāya” (self-study) (participant 69). Another theme emerged in the study of yogic philosophy and sacred texts.
This theme includes goals such as studying texts like the Yoga Sutras, deepening philosophical understanding, and integrating that knowledge into life and teaching. Participants explained, “My yoga practice inspires me to continue to challenge the mind, continue to keep learning and expanding” (participant 29), “Continue to learn texts and Vedic chants” (participant 28), “Deepen my understanding of Ayurvedic and Yogic philosophy” (participant 61). The final theme uncovered was integration into life and work. Participants expressed a desire to apply their yoga and study to their personal development, teaching, or the broader systems they’re part of. Examples of participants’ personal goals included “Improve cognitive flexibility and radical acceptance” (participant 30), “Learn more about therapeutic yoga practices to share with clients” (participant 34), and “Forge new ways to bring the experience of yoga therapy into the western medical system in subtle yet substantial ways” (participant 45).
Discussion
Yoga therapist participants in this study report overarching themes that run through their personal practice. A common theme is that yoga therapy is used to relieve pain and promote physical healing. Across every list, goals related to relieving chronic pain, healing from injury or illness, and improving physical functioning are prominent. Examples include addressing chronic pain, arthritis, and inflammation; recovering from surgeries or injuries; managing degenerative diseases or autoimmune conditions; and improving mobility, posture, or joint health. This suggests that yoga therapist participants view yoga therapy as a modality that supports longterm, sustained healing. Yoga therapy is used to manage both acute and chronic health concerns. Another common thread identified in the qualitative strand of this study is that yoga therapy is used to address concerns related to mental health, stress management, and emotional healing. Yoga therapists report that it is used to address emotional and physiological ailments, including stress, anxiety, depression, grief, burnout, trauma, PTSD, mood regulation, and nervous system resilience. This supports the use of yoga therapy as a tool for mental health.
Yoga therapy practices help practitioners build resilience, process trauma, and find balance. Yoga therapy is used to support goals such as nervous system regulation, expanding the window of tolerance, and grounding through mindfulness techniques. Yoga therapy is also used to connect with yogic knowledge through the exploration of yoga philosophy, the study of ancient texts, the practice of the 8 limbs of yoga, and other traditional yogic practices, including chanting and mudra. Results suggest that yoga therapy may support personal development physically, mentally, and emotionally, as well as spiritually. Yoga therapy tools help practitioners make meaning and find purpose in their lives. In addition to supporting physical and mental health, yoga therapy is also used as a vehicle for self-exploration, personal growth, and inquiry. As yoga therapy is integrated into daily practice, it becomes a tool for establishing a lifestyle that supports sustainable daily practices, builds discipline and healthy habits, and fosters work-life balance through self-care practices that can support the establishment of a system for living well across the lifespan. Yoga is being used as a multidimensional tool to support the whole systemphysically, mentally, emotionally, energetically, and spiritually.
Interprofessional collaboration
While this study examined yoga therapists’ perspectives and practice experiences, this research contributes to the literature by applying an interprofessional collaboration approach to working with individuals with the physical and psychological conditions under study. Previous research showed that patients have different perceptions of their health outcomes than their providers do [32]. Thus, interprofessional collaboration can be leveraged to address these differences in perceptions. This can be achieved through the interdependence between providers and yoga therapists [14]. For instance, a yoga therapist can request information from a patient’s primary care physician about the patient’s concerns regarding medication changes. Another example is that, with the patient’s release of information, a social worker can request that the yoga therapist further work with patients on attention regulation to enhance mindfulness and self-awareness, which may align with the clinical social worker’s mental health therapy patient homework recommendations.
Yoga therapists would then follow up with the clinical social worker to discuss ways to maximize patients’ psychological wellbeing, considering factors that might be affecting their mental health. This can also be achieved by developing new professional activities [14]. A patient’s healthcare provider team, whether colocated in the same office or building or not, can foster inclusion by formally establishing meeting agendas and protocols that include each discipline. These new activities can guard against siloed practice. Flexibility is crucial [14]. For example, if a diabetes healthcare provider manager, such as a nutritionist, collaborates with yoga therapists to address patient needs over time, the yoga therapists may learn from the diabetes healthcare provider about common diabetes medication names and typical diabetes management recommendations. The therapist may be able to provide a reasonable, basic response to a patient’s question, which can acknowledge the question, although yoga therapists would ultimately still refer patients back to their diabetes healthcare provider for a more informed response. Collaboration through collective ownership of goals is also a cornerstone of an interprofessional approach [14].
This can be realized by creating new protocols that enable all patient-treating providers to work together and, through that collaboration, to include patients and their support systems in co-developing, co-implementing, and co-evaluating goals. This requires genuine unison and the willingness to disagree, with open sharing of ideas to address patient needs. Finally, all patientinvolved providers reflecting on their practice with one another, rather than only with peers, is best practice [14]. In closing, some of these suggestions may be challenging to implement due to provider schedules and timing variability. If time is invested in multidirectional interprofessional collaboration (i.e., collaboration with all patient providers), this can be realized. Starting with newly created activities may help, as it provides opportunities to plan how to proceed with interprofessional collaboration and interdependence, to explore the degree of flexibility needed or appropriate, and to determine how collective ownership will be implemented (Appendix A).
Appendix A:Themes describing Cikitsā goals in yoga therapists’ personal practices.
Limitations and opportunities for future study
This study has limitations despite the key opportunities outlined. The study used a convenience sample of therapists. Therapists’ practices were measured using Likert-scale items based on therapists’ self-reports of their perceptions; the study also asked therapists to report perceptions of conditions they may not be trained to detect. Future studies evaluating this model in practice with yoga therapists and other healthcare providers treating these conditions are recommended (Appendix B). These studies should evaluate the model, patient health outcomes, and provider well-being. Revisiting healthcare providers’ and patients’ perceptions of outcomes, and how they differ and overlap, based on interprofessional collaboration with yoga therapists is recommended. Surveying yoga therapy clients about their experiences with yoga therapy for health conditions is recommended. Studies that include focus groups or individual interviews with yoga therapists, clients, and other healthcare professionals are recommended to gather additional data on the impact of yoga therapy on a variety of health conditions.
Appendix B:Themes describing Rakṣaṇa goals in yoga therapists’ personal practices.
Conclusion
This study provided valuable insights into health from the perspective of yoga therapists. Qualitative and quantitative data were collected through a survey to understand the role of therapeutic yoga in addressing a variety of physical and mental health conditions (n=69). The results of this study support yoga therapy as an effective tool in the treatment of various health ailments, both physical and physiological. Yoga therapists are supporting practitioners in creating a pathway toward holistic wellness. There is an opportunity for therapists to further examine multiple sclerosis (Appendix C). However, many conditions were overall impacted by therapists’ personal practices, making a positive difference for clients with back pain, depression, headaches, PTSD, stress, arthritis, and asthma. This study also provides insight into how Viniyoga and yoga therapy approach health and well-being holistically for the overall good of the client. Further research is needed to expand the literature on the usefulness of therapeutic yoga and other forms of yoga therapy in promoting health and treating health disorders (Appendix D).
Appendix C:Themes describing Śikṣaṇa goals in yoga therapists’ personal practices.
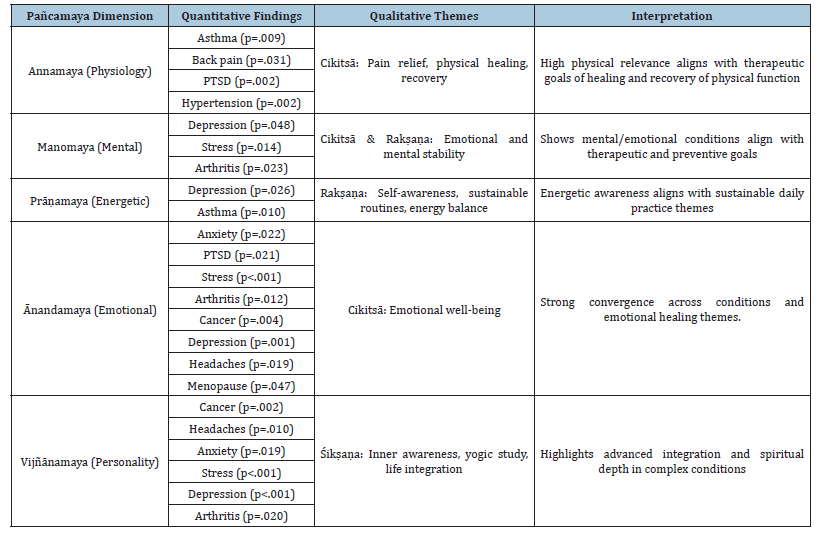
Appendix D:Joint Display: Integration of Quantitative and Qualitative Findings on Yoga Therapy Personal Practice Outcomes Using the Pañcamaya Model.
Acknowledgement
The authors would like to thank Graduate Research Assistant Cheyenne Williams for writing and editing assistance.
References
- Shohani M, Badfar G, Nasirkandy MP, Kaikhavani S, Rahmati S, et al. (2018) The effect of yoga on stress, anxiety and depression in women. International Journal of Preventative Medicine 9: 21.
- Ministry of external affairs (2015) Yoga: It’s origin, history and development. Government of India.
- Jeter P, Slutsky J, Singh N, Khalsa S (2015) Yoga as a therapeutic intervention: A bibliometric analysis of published research studies from 1967 to 2013. The Journal of Alternative and Complementary Medicine 21(10): 586-592.
- Snaith N, Schultz T, Proeve M, Rasmussen P (2018) Mindfulness, self-compassion, anxiety and depression measures in South Australian yoga participants: Implications for designing a yoga intervention. Complimentary Therapies in Clinical Practice 32: 92-99.
- Friedberg MW, Chen PG, Busum, VKR, Aunon F, Pham C, et al. (2014) Factors affecting physician professional satisfaction and their implications for patient care, health systems, and health policy. Rand Health Quarterly 3(4): 1.
- Sharkiya SH (2023) Quality communication can improve patient-centred health outcomes among older patients: A rapid review. BMC Health Services Research 23(1): 886.
- Brandt B, Lutfiyya MN, King JA, Chioreso C (2014) A scoping review of interprofessional collaborative practice and education using the lens of the triple aim. Journal of Interprofessional Care 28(5): 393-399.
- Reeves S, Pelone F, Harrison R, Goldman J, Zwarenstein M (2017) Interprofessional collaboration to improve professional practice and healthcare outcomes. Cochrane Database of Systematic Reviews 6(6): CD000072.
- World health organization (2010) Framework for action on interprofessional education & collaborative practice.
- Youngwerth J, Twaddle M (2011) Cultures of interdisciplinary teams: How to foster good dynamics. Journal of Palliative Medicine 14(5): 650-654.
- McLaney E, Morassaei S, Hughes L, Davies R, Campbell M, et al. (2022) A framework for interprofessional team collaboration in a hospital setting: Advancing team competencies and behaviours. Healthcare Management Forum 35(2): 112-117.
- Jones B, Phillips F (2016) Social work and interprofessional education in health care: A call for continued leadership. Journal of Social Work Education 52(1): 18-29.
- Konrad SC, Cavanaugh JT, Rodriguez K, Hall K, Pardue K (2017) A five-session interprofessional team immersion program for health professions students. Journal of Interprofessional Education & Practice 6: 49-54.
- Iachini AL, Bronstein LR, Mellin E (2018) A Guide for interprofessional collaboration. Council on Social Work Education, (1st edn).
- Fitzgerald C, Barley R, Hunt J, Klasto S, West R (2021) A mixed-method investigation into therapeutic yoga as an adjunctive treatment for people recovering from substance use disorders. Internation Journal of Mental Health and Addiction 19: 1330-1345.
- Sullivan M, Erb M, Schmalzl L, Moonaz S, Taylor J, et al. (2018) Yoga therapy and polyvagal theory: The convergence of traditional wisdom and contemporary neuroscience for self-regulation and resilience. Frontiers in Human Neuroscience 12: 67.
- Schmalzl L, Powers C, Blom EH (2015) Neurophysiological and neurocognitive mechanisms underlying the effects of yoga-based practices: Towards a comprehensive theoretical framework. Front Hum Neurosci 9: 235.
- Lang A, Malaktaris A, Maluf K, Kangas J, Sindel S, et al. (2021) A randomized controlled trial of yoga vs nonaerobic exercise for veterans with PTSD: Understanding efficacy, mechanisms of change, and mode of delivery. Contemporary Clinical Trails Communications 21: 100719.
- Heeter C, Lehto R, Allbritton M, Day T, Wiseman M (2017) Effects of a technology-assisted meditation program on healthcare providers’ interoceptive awareness, compassion fatigue, and burnout. Journal of Hospice and Palliative Nursing 19(4): 314-322.
- Deshmukh T (2022) Yoga therapy. Aayushi International Interdisciplinary Research Journal 9(9): 11-13.
- Buchalter J (2025) What is yoga Cikitsa (Therapy) anyway? Denver Holistic Health Collective.
- Bossart C (2007) Yoga bodies, yoga minds: How Indian anatomies form the foundation of yoga for healing. International Journal of Yoga Therapy 17(1): 23.
- Martins IJ (2016) Anti-aging genes improve appetite regulation and reverse cell senescence and apoptosis in global populations. Advances in Aging Research 5: 9-26.
- Martins IJ (2017) Single gene inactivation with implications to diabetes and multiple organ dysfunction syndrome. Journal of Clinical Epigenetics 3(3): 24.
- Martins IJ (2018) Sirtuin 1, a diagnostic protein marker and its relevance to chronic disease and therapeutic drug interventions. EC Pharmacology and Toxicology 6(4): 209-215.
- Kishida M, Mama S, Larkey L, Elavsky S (2018) “Yoga resets my inner peace barometer”: A qualitative study illuminating the pathways of how yoga impacts one’s relationship to oneself and to others. Complementary Therapies in Medicine 215-221.
- Francis A, Beemer R (2019) How does yoga reduce stress? Embodied cognition and emotion highlight the influence of the musculoskeletal system. Complimentary Therapies in Medicine 43: 170-175.
- Laplaud N, Perrochon A, Gayot MG, Moens M, Goudman L, et al. (2023) Management of post‑traumatic stress disorder symptoms by yoga: An overview. BMC Complementary Medicine and Therapies 23(1): 258.
- Sciarrino N, DeLucia C, O’Brien K, McAdams K (2017) Assessing the effectiveness of yoga as a complementary and alternative treatment for post-traumatic stress disorder: A review and synthesis. Journal of Alternative and Complimentary Medicine 23(10): 747-755.
- Kolk VDB, Stone L, West J, Rhodes A, Emerson D, et al. (2014) Yoga as an adjunctive treatment for posttraumatic stress disorder: A randomized controlled trial. Journal of Clinical Psychiatry 75(6): e559-e565.
- Dietrich K, Strumbel N, Baumann A, Feng NV (2024) Experiences with one-to-one trauma center trauma-sensitive yoga sessions: Consensual qualitative research. International Journal of Yoga Therapy (34).
- Nowell LS, Norris JM, White DE, Moules NJ (2017) Thematic analysis: striving to meet the trustworthiness criteria. International Journal of Qualitative Methods 16(1).
- Kennedy BM, Rehman M, Johnson WD, Magee MB, Leonard R, et al. (2017) Healthcare providers versus patients' understanding of health beliefs and values. Patient Experience Journal 4(3): 29-37.
- Callahan AM, Higgins DM (2023) Interprofessional social work practice: A call for a new specialization. Journal of Social Work Education 59(sup1): S5-S22.
- Dow AW, DiazGranados D, Mazmanian PE, Retchin SM (2014) An exploratory study of an assessment tool derived from the competencies of the interprofessional education collaborative. Journal of Interprofessional Care 28(4): 299-304.
- Forseth B, Polfuss M, Brondino M, Hunter S, Lawlor M, et al. (2022) Adherence to and changes in mental and physiological health during an 8-week yoga intervention: A pilot study. Journal of Bodywork and Movement Therapies 30: 203-209.
- Nanthakumar C (2020) Yoga for anxiety and depression-a literature review. The Journal of Mental Health Training, Education and Practice 15(3): 157-169.
- Sullivan M, Moonaz S, Weber K, Taylor J, Schmalzl L (2017) Toward an explanatory framework for yoga therapy informed by philosophical and ethical perspectives. Alternative Therapies in Health and Medicine 24(1): 38-47.
- Vestergaard E, Nørgaard B (2018) Interprofessional collaboration: An exploration of possible prerequisites for successful implementation. Journal of Interprofessional Care 32(2): 185-195.
© 2026 Jennifer Vasquez. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






