- Submissions

Full Text
Techniques in Neurosurgery & Neurology
Diagnostic Capabilities of Brain Encephalovisiometry in the Correction of Vascular and/or Vertebral Disorders-A Clinical Case
Alexandra Maximova and Andrey Maximov*
Miraculum Medical Center, Georgia
*Corresponding author: Maximov, Miraculum Medical Center, Georgia
Submission: July 16, 2021;Published: September 01, 2021

ISSN 2637-7748
Volume4 Issue3
Abstract
As a result of a brain Encephalovisiometry (EV) of a child with a diagnosis of disintegrative disorder and childhood autism, gross vascular and vertebral disorders were diagnosed, and vascular and rehabilitation therapy courses were recommended. A repeated EV study showed that the implementation of a fifteenweek protocol led to the disappearance of vascular disorders, restoration of blood flow, and normalization of metabolic processes in the patient’s brain. Negative behavior and other violations also disappeared. The patient behaved as a neurotypical child and rapidly overcame a lag in speech development.
Abbreviations: DCP: Direct Current Potentials; EEG: Electroencephalography; EV: Encephalovisiometry; ICD: International Classification of Diseases, NEM: Neuroenergy Mapping; SWBA: Slow-Wave Brain Activities
Introduction
The presented case is one among a cohort of 203 young patients with various diagnoses of developmental disorders who underwent EV at Miraculum Center in March and May 2021 in Belarus, Georgia, and Ukraine. All, except for one child, had various disorders of the central nervous system. Primarily, these were cerebrospinal fluid, vascular, and vertebral disorders, as well as disorders of venous outflow, microcirculation, and encephalopathy. Statistics for the medical problems in this cohort will be published in the coming months. The clinical case under consideration is interesting because, for five years, none of the involved specialists suspected the existence of vascular disorders, and his treatment was limited to behavioral correction. However, because of new pharmaceutical and rehabilitative interventions, his brain function was normalized in just fifteen weeks, and the patient, diagnosed with disintegrative disorder, became a neurotypical child. EV or NEM of the brain is the study of Slow-Wave Brain Activity (SWBA) using an encephalovisor (in the first case) or a Neuroenergocartograph (in the second). The fundamental principles of neuroenergo mapping and encephalovisiometry are the same. SWBA has been recorded at the brain’s low frequency electrical activity (less than 0.5Hz) through indicators of the stable potentials difference (direct current potentials or DC-potentials) of the millivolt range between the brain (or extracerebral structures) and reference areas using DC amplifiers [1,2]. The difference between NEM and EV is that neuroenergo mapping uses a stationary device, and encephalovisiometry uses a compact, wireless mobile device with remote patient access that was developed at Miraculum. The latter device is currently undergoing testing as an industrial prototype. Significant deviations from the norm of brain energy metabolism correlate with a variety of biochemical parameters of the brain and main bodily systems. These are not, however, practically used in mass clinical practice. In 2020-2021, the Miraculum Center, based on the author’s interpretation of SWBA indicators, developed new and unique methods for diagnosing and correcting comorbid pathology in patients with developmental disorders. Currently, these methods show high diagnostic efficiency in the Center’s clinical practice and are in the process of being patented (Application No. 2021118656 of 26.06.2021) in the Russian Federation for the invention, “The method for diagnosing cerebrospinal fluid, vascular, and related disorders in the central nervous system”.
Case Report
This is the clinical case of a five-year-old boy diagnosed with disintegrative disorder (F84.3) and children’s autism (F84.0), based on the classical signs of a developmental disorder. These include: a complete lack of communication coupled with constant fears and panic attacks; a severe delay in speech development, with only a few words used with an urgent need (request) coupled with a small, uncontrolled, and unconscious echolalia. These were accompanied by severe sleep disorders, obsessive stereotypical and repetitive movements, emotional lability with frequent crying attacks, and an extremely high level of anxiety and fear of new places and routes of movement. All of these are often typical for a child with autism. Specialists prescribed ABA and other corrective therapies with little positive results. At the parents’ initiative, the patient was treated by geneticists, who put him on a diet with many dietary supplements. The parents confirmed later that in communication with doctors and other specialists, there was never any question of finding and diagnosing neurological, vascular, hypoxic, or vertebral disorders. However, the brain EV (March 2, 2021) identified gross vascular and vertebral disorders with pronounced foci of hypoxia in the occipital and left temporal lobes of the patient’s brain. Recording the brain activities at rest (the first scan), EV immediately showed the presence of severe hypoxia (blue color, turning into blue). To determine possible causes of the hypoxia, a tape was applied to the cervical spine area, after which brain function normalized (the second scan). That suggests a high probability of vertebral disorders. During the stimulation “head turns” test (the third scan), and despite the presence of tape, a hypoxia focus appeared in the occipital lobe. After removing the tape, hypoxia began to increase rapidly (the fourth scan), and when turning the head, it moved to the left temporal lobe (the fifth scan) (Figure 1).
Figure 1:
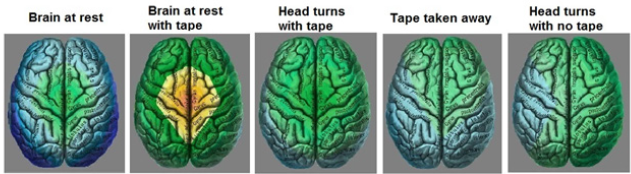
The preliminary EV diagnosis was subsequently confirmed by traditional studies (X-ray of the cervical region in three projections and ultrasound of the neck and brain vessels), which revealed instability of the C3-C5 vertebrae and blood flow disorders. These occurred especially on the left side, particularly in the left vertebral artery and especially when conducting a test with rotation. The latter is associated with a corresponding violation in speech development. Based on the EV conclusion, recommendations were issued for vascular therapy, including vascular preparations based on such active substances as vinpocetine, ethylmethylhydroxypyridine succinate, dry horse chestnut seed extract, and a central-acting myorelaxant Mydocalm. At the same time, recommendations for rehabilitation therapies included osteopathy (twice a week), massage (three times a week), physical therapy (two to three times a week), and constant taping to stabilize the muscular frame of the cervical spine. Fifteen weeks after starting vascular and correctional therapy protocols, the patient was referred by the attending neurologist for a second EV study. The doctor suggested that taping had fulfilled its function of restoring blood flow but wanted to confirm this instrumentally (Figure 2). The patient came with permanently worn tapes, and initially the EV study (left scan) showed a rapid development of hypoxia, turning even into cortical ischemia. However, after removing the tapes, all DCP indications returned to normal in just a few seconds. This confirmed the improvement of metabolic processes in the patient’s brain and its normal approximation. Thus, the EV results made it possible to stop using the tapes in a timely manner because their use became counterproductive after successfully correcting the vascular disorders. With the removal of the tapes (right scan), which successfully fulfilled their original function, the EV confirmed the disappearance of vascular disorders, the elimination of previously existing hypoxia foci, the restoration of blood flow, and the normalization of metabolic processes in the patient’s brain. A survey of parents and teachers working with the child showed that after the protocol’s implementation, the child exhibited a neurotypical state. Moreover, he actively overcame his lag in speech development and began to show a complete understanding of speech by giving answers to questions and successfully building sentences from several words.
Figure 2:

Discussion
Many diagnostic criteria for autism and other developmental disorders in accordance with recommendations of the ICD-10 and ICD-11, namely: negative, antisocial, stereotypical, and repetitive behavior together with a huge, constantly growing variety of other external signs - phobias; aggression and self-aggression; toilet, sleep and nutrition disorders [3,4] - coincide with clinical symptoms of gross cerebrospinal fluid and vascular disorders. As a result, if a diagnosis of autism has been made, many doctors, even specialized ones, do not consider the above symptoms as diagnostic criteria for such conditions as chronic hypoxia. They are often simply written off as autism. On the other hand, it is well known that serious vascular and hypoxic disorders lead to changes in the brain, and in severe cases, to neurodegeneration, which can often serve as a trigger for negative behavioral development [5-9]. Therefore, both neurologists and pediatricians, as well as parents, when working with such patients, need to pay close attention to the possibility of vascular disorders in such patients and conduct necessary studies to determine whether this diagnosis is warranted. Since EV is not yet available in most of the world’s countries, studies such as an ultrasound of the vessels of the neck and brain, X-rays of the cervical and thoracic spine, and, in some cases, night EEG monitoring, can indicate whether vascular and/or vertebral disorders are present. The clinical case presented in this publication (as well as others from the above-mentioned cohort of patients) clearly confirms that autism and other developmental disorders are secondary in nature. The negative behavior of children with such diagnoses is not a feature of neurodevelopment but a consequence of comorbid pathology that is a complex of various interrelated pathologies and diseases. Their successful diagnosis and correction lead to a decrease or disappearance of negative behavior and other violations, and to the blurring of the criteria for the official diagnoses themselves. The degree of this decrease depends on how long a child’s underlying disease or diseases were ignored and how long they freely caused irreparable harm to body and brain. In other words, not all children can be completely returned to a neurotypical state. But it is possible to remove gross sleep and nutrition disorders from everyone, significantly reduce negative behavior, and significantly improve the quality of life for a child and a family.
Author Contribution
Alexandra Maximova led the entire clinical practice of the patient (from EV and diagnostics to the development of treatment and rehabilitation protocols) and prepared the concept; Andrey Maximov wrote the main manuscript text, prepared figures, and reviewed the manuscript.
References
- Maximova AA (2021) Neuroenergy mapping diagnostic capabilities in hypoxic brain lesions. J Angiol Vasc Surg 6: 057.
- (2021) Potential of neuroenergy mapping in diagnosis of pathophysiological changes in the central nervous system in patients with developmental disorders. Maximova AA (Edr.), Universum: Medicine and Pharmacology: Electron. Scientific Zhurn 1(74).
- International statistical classification of diseases and related health problems 10th
- International classification of diseases 11th The global standard for diagnostic health information.
- Di Tommaso MC (2012) A comparative study of bipolar disorder and attention deficit hyperactivity disorder through the measurement of regional cerebral blood flow. J Biol Regul Homeost Agents 26(1): 1-6.
- Ferro MF, Pezzini R, Lorizio A (1967) Clinical and electroencephalograhic study of children who have suffered from perinatal hypoxia. Riv Neurobiol 13(1): 11-39.
- Kenzhibaeva KA (1970) Effect of umbilical cord twisting around the neck on the psychophysical development of the child. Vopr Okhr Materin Det 15(10): 48-52.
- Dougherty M, Wright FS, Loewenson RB, Torres F (1985) Cerebral dysfunction after chronic hypoxia in children. Neurology 35(1): 42-46.
- Tran K, Wu J (2019) Case report: neuroimaging analysis of pediatric ADHD-related symptoms secondary to hypoxic brain injury. Brain Inj 33(10): 1402-1407.
© 2021 Andrey Maximov. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






