- Submissions

Full Text
Research in Medical & Engineering Sciences
Mycoleptodiscus indicus in an Heart-Transplant Recipient. A Case Report and Review of the Literature
Passera M1, Ortalli G1, Vittori C2, Cavallini M1, Guarneri D1 and Farina C1*
1Microbiologia e Virologia, ASST Papa Giovanni XXIII, Bergamo, Italy
2Cardiologia, ASST Papa Giovanni XXIII, Bergamo, Italy
*Corresponding author: Farina C, SMeL Microbiologia e Virologia, ASST Papa Giovanni XXIII, Piazza OMS 1, 24127, Bergamo, Italy
Submission: February 06, 2021Published: March 11, 2021

ISSN: 2576-8816Volume9 Issue2
Abstract
Mycoleptodiscus indicus, a phytopathogenic dematiaceous hyphomycete, has only sporadically been described as an agent of subcutaneous infections in immunocompromised patients. A case of M. indicus abscess infection is reported here in a patient undergoing orthoptic heart transplantation. Surgical debridement together with Amphotericin B followed by a long-term therapy with Itraconazole cured the patient.
Keywords: Mycoleptodiscus indicus; Subcutaneous infection; Heart transplant
Abbreviations: MOFS: Multi-Organ Failure Sepsis; LSU gene: Large Subunit gene; HIV: Human Immunodeficiency Virus; HCV: Hepatitis C VirusRNA: RiboNucleic Acid
Introduction
Mycoleptodiscus indicus, a dematiaceous hyphomycete, is a common contaminant of tropical or subtropical soils and occurs on the leaves of different plants for which it is pathogenic, particularly but not exclusively monocotyledons [1]. It has only been sporadically described as a subcutaneous infection agent in immunocompetent animals [2-4] and in immunocompromised patients. Compared to the general population, this type of patient has an increased risk of developing opportunistic fungal infections with greater morbidity and mortality. A case of M. indicus abscess infection is reported here in a patient undergoing orthoptic heart transplantation.
Case Presentation
D.M., a 27-year-old Senegalese woman, undergoing immunosuppressive therapy due to a heart transplant, was admitted at the "Cardiovascular Department - Heart Failure and Transplantation" of the “Papa Giovanni XXIII” hospital in Bergamo, Italy. She presented a Multi-Organ Failure Sepsis (MOFS), with unknown bacterial etiology, and a Cytomegalovirus infection with intestinal localization. During hospitalization, the development of an abscess infection of the left lower limb was observed. Collected purulent material from the abscess was cultured for aerobic and anaerobic bacteria and fungi: it resulted positive for a dematiaceous fungus identified as Mycoleptodiscus indicus. The patient was subjected to induction treatment with liposomal Amphotericin B, followed by long-term therapy with Itraconazole. The treatment, together with the drain of the abscess, allowed the complete resolution of the lesion [1-9].
The fungus was thermotolerant, growing well at 25 °C and 35 °C but not at 42 °C, on Sabouraud Dextrose Agar after a 5-day incubation. Flat colonies grew, presenting velvety texture, macroscopically whitish soon which turned yellowish gray with a brownish reverse (Figure 1). Microscopically, hyphae were septate, branched, only later showed the presence of a dark pigment. No conidia were present (Figure 2). Subcultures on Potato Agar and on Malt Agar did not present any sporulation. The fungal identification, performed by gene sequencing with amplification of the D2 region of LSU gene (Large Subunit rRNA), confirmed the presence of a Mycoleptodiscus indicus strain.
Figure 1: Colonies grown on Sabouraud Dextrose Agar (a. recto; b. verso).
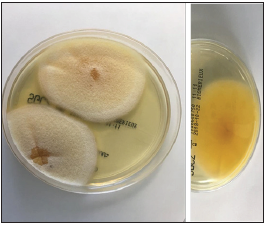
Figure 2: Lactophenol Cotton Blue staining, 25x magnification, showing septate hyphae, with the absence of conidia.
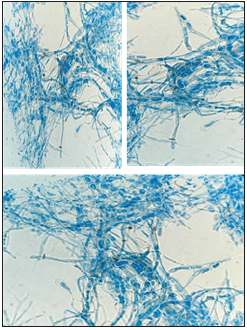
Discussion
Finding in culture of the phytopathogenic black fungus Mycoleptodiscus indicus is absolutely sporadic in human pathology. Only few human cases have been reported in the scientific literature. In Padhye AA et al. [5] firstly described a subcutaneous infection of the prepatellar bursa of his right knee in a 72-year-old male, immunocompromised because of a Wegener’s granulomatosis chronically treated with methotrexate and prednisone [5]. In Garrison AP et al. [6] reported M. indicus as the etiologic agent of nodular lesions: it was initially observed on the dorsum of the right hand of a 51-year-old man affected by HIV and HCV co-infection. Later, it assumed a sporothrichosis-like lymphangitic distribution at the forearm. The patient underwent a liver transplant and was thus treated with tacrolimus and steroids [6]. In 2010 Dewar et al. [7] described the first case of M. indicus infection in a normal competent 54-year-old male presenting a patellofemoral osteoarthritis at his left knee [7]. In 2012 Koo et al. [8] reported a myositis following a progressive necrotizing cellulitis in a leg of an immunocompromised patient treated with temozolomide and steroids because of a glioblastoma multiforme [8]. All cases mentioned as possible the direct inoculation of M. indicus through the injured skin during their staying in tropical or subtropical countries: lower coastal South Carolina [5], Florida [6], Costa Rica [7]. Similarly, to others, our case too occurred in an immunocompromised woman, returning for heart failure from Senegal. All cases included ours, which occurred in immunocompromised people were treated with concomitant Amphotericin B and surgical debridement, followed by azole (Itraconazole or Voriconazole).
Opportunistic fungal infections in severely immunocompromised patients are burdened with increased morbidity and mortality. The correct identification of Mycoleptodiscus indicus is absolutely difficult, requiring highly specialized operating conditions and the use of genetic identification methods. It must be noted that the Mycoleptodiscus taxonomy has been recently revised, suggesting that the identifications of M. indicus described in all the previously referred clinical cases may be incorrect and have to considered as caused by Muyocopron laterale [9]. The correct microbial identification has allowed the adoption of adequate therapy schemes that have permitted the clinical resolution.
References
- Sutton B (1973) Pucciniopsis, Mycoleptodiscus and Amerodiscosiella. Trans Br Mycol Soc 60(3): 525-536.
- Hull W, McNamara T, Ireland G (1997) Subcutaneous phaeohyphomycosis due to Mycoleptodiscus lateralis in a cat. In: Anals do XXV Congresso Brasileiro de Medicina Veterinaria, XIII Congresso Estadual de Medicina Veterinaria, II Congresso de Medicina Veterinaria do Cone Sul. Gramado, Rio Grande do Sul, Brasil.
- Metry CA, Hoien PS, Maddox CW, Thompson EH, Sutton DA, et al. (2010) Subcutaneous Mycoleptodiscus indicus Infection in an Immunosuppressed Dog. J Clin Microbiol 48(8): 3008-3011.
- Maboni G, Krimer P, Baptista R, Lorton A, Anderson C, et al. (2019) Laboratory diagnostics, phylogenetic analysis and clinical outcome of a subcutaneous Mycoleptodiscus indicus infection in an immunocompetent cat. BMC Vet Res 15(1): 354.
- Padhye AA, Davis MS, ReddickA, Bell MF, Gearhart ED, et al. (1995) Mycoleptodiscus indicus: a new etiologic agent of phaeohyphomycosis. J Clin Microbiol 33(10): 2796-2797.
- Garrison AP, Procop GW, Vincek V, Moon J, Morris MI, et al. (2008) A case of subcutaneous Mycoleptodiscus indicus infection in a liver transplant recipient successfully treated with antifungal therapy. Transpl Infect Dis 10(3): 218-220.
- Dewar CL, Sigler L (2010) Fungal arthritis of the knee caused by Mycoleptodiscus indicus. Clin Rheumatol 29(9): 1061-1065.
- Koo S, Sutton DA, Yeh WW, Thompson EH, Ligler L, et al. (2012) Invasive Mycoleptodiscus fungal cellulitis and myositis. Med Mycol 50(7): 740-745.
- Hernandez M, Bezerra JP, Tan YP, Wiederhold N, Crous PW, et al. (2019) Re-evaluation of Mycoleptodiscus species and morphologically similar fungi. Persoonia 42: 205-227.
© 2021 Farina C. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






