- Submissions

Full Text
Research in Medical & Engineering Sciences
A Case Report of Sub Periosteal Abscess
Amit Saini1, Rajender Parshad2, Munish Kumar Saroch3* and Gaveshna Gargi4
1senior resident, Govt Medical College ENT Kangra at Tanda HP, India
2Govt Medical College ENT Kangra at Tanda HP, India
3Associate Professor ENT, Govt Medical College ENT Kangra at Tanda HP, India
4Resident Department of Medicine, Govt Medical College ENT Kangra at Tanda HP, India
*Corresponding author: Munish Kumar Saroch, Associate Professor ENT, Skype dr_saroch, Govt Medical College ENT Kangra at Tanda HP, India
Submission: August 31, 2017; Published: October 05, 2017

ISSN : 2576-8816Volume1 Issue5
Introduction
Acute and chronic rhino sinusitis are amongst the most
frequently encountered conditions by the otolaryngologist in dayto-
day practice. These are usually easily manageable with proper
and effective antibiotic therapy and decongestants. However, despite
widely available appropriate antibiotics, the otolaryngologist often
finds himself face-to-face with complications of sinusitis especially
in the pediatric population. These may affect the soft tissues, bones,
the orbit and even the brain with a possible fatal or functionally
impairing outcome (visual loss) at times. Here we present a case of
orbital complication secondary to frontoethmoidal sinusitis.
Case Report
A 15-year old female was referred from the Department of Ophthalmology to the Department of Otolaryngology, Head and Neck Surgery, Dr. RPGMC, Kangra at Tanda, HP with the complaints of pain and swelling in the left eye since three days. She had a history of difficulty in eye opening. She also complained of intermittent left-sided nasal obstruction for the last three years. On ophthalmologic examination, she had a parallel visual axis, visual acuity of 6/24 (improving to 6/9 with pin-hole) and restricted elevation of the left eye along with a positive regurgitation test. There was diffusing, swelling, erythematic and tenderness in the upper eyelid and proposes. Slit lamp examination revealed anterior seborrhea blepharitis: cornea was clear, anterior chamber was normal. No abnormality was detected on fundoscopic examination. On ENT examination, there was marked tenderness over the left frontal sinus and bilateral ethnocide sinuses (L>R). Nasal patency tests revealed decreased airflow from the left nasal cavity. A high resolution computed tomography (HRCT) scan suggested the possibility of orbital cellulites with abscess and sinusitis of the left frontal and ethnocide sinuses. A combined approach frontoethmoidectomy with drainage of subperiosteal abscesses (L) was performed under general anesthesia. The intra-operative findings were: conch bullosa on the left side, purulent discharge in left middle meets region. Frontal air cells were opened using 4mm cutting burr and around 10-15cc thick yellowish non foul-smelling pus was drained. Male cot red rubber catheter was placed in the left nasal cavity and secured. Post-operatively, the patient was put on broad spectrum intravenous antibiotics, systemic and topical decongestants and antibiotic eye drops for instillation. In the post operative period, the patient developed papilloedema which resolved within three days. She was discharged on the tenth post operative day with a visual acuity of 6/6, minimal lid edema and full extra ocular movements (Figure 1-11).
Figure 1: Just before surgery.

Figure 2 Just before surgery.
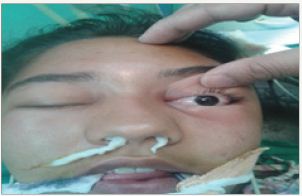
Figure 3 Intra operative.
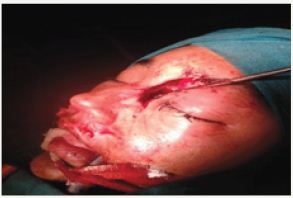
Figure 4 just postoperative.
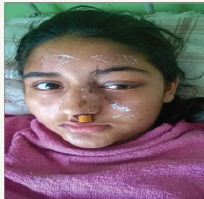
Figure 5 7th post operative day.
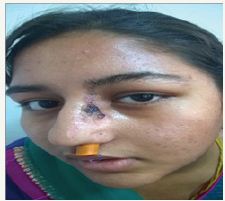
Figure 6 7th post operative day.

Figure 7 >14th post operative day.
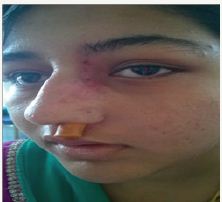
Figure 8 21st post operative day.

Figure 9 CT.
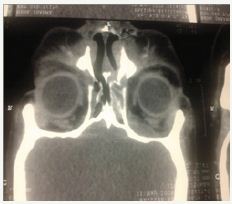
Figure 10 CT.
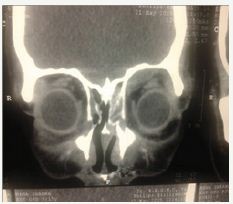
Figure 11 CT.
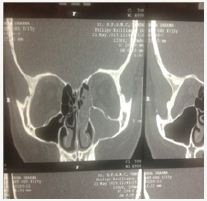
Discussion
Orbital complications of sinusitis are more common in the younger age group with male preponderance being found in most of the studies [1]. As the orbit is bordered by several sinuses-the frontal, ethnocide and maxillary-infection from any of these sinuses can potentially spread to the orbit. The ethnocide sinus is almost exclusively implicated in the spread of infection to the orbit owing to the thinness of its wall, the lamina papyracea. Most orbital infections are, therefore, on the medial side of the orbit. If an abscess forms between the wall and periosteum, it is called a subperiosteal abscess. If the periosteum is violated, then an orbital abscess may form Chandler classified orbital infection into five groups in order of increasing severity. Perceptual cellulites characterized by a swollen and hyperemic upper eyelid without proposes and chamois is the most commonly occurring orbital complication especially in the pediatric age group. Infection is limited to the skin in front of the orbital septum. The next in the spectrum of disease is the stage of orbital cellulites seen as diffuse edema of the lining of the orbits with swelling of the eyelids, painful extra ocular movements and weakening of vision due to pressure on the optic nerve. Untreated patients may land into the next stage, stage of subperiosteal abscess wherein fluid/pus collects below the periosteum leading to proposes. Group 4 orbital abscess, is characterized as a true abscess in the orbital space. This may manifest with proposes, impaired eye movement, and in the worst case, blindness. Group 5 is cavernous sinus thrombosis with rapidly progressive bilateral chamois, ophthalmoplegia, retinal engorgement, and loss of Visual acuity, along with possible meningeal signs and high fever [2,3]. CT scans played an undisputable role in the determination of a diagnosis and the correct differentiation of such pathologies. Controversy exists regarding the treatment modality for orbital complications of sinusitis. Most of the researchers seem to agree on conservative management for children with early stage disease, moving on to surgical intervention in case the patient worsens or doesn’t show expected improvement within 24hrs of adequate antibiotic therapy. The majority of small SPAs as diagnosed on CT scans in younger children can be successfully treated medically as concluded by various researchers in the past. Surgery, however, should be considered for a worsening clinical examination [4-7]. Herrmann et al. [8] found that children at the age of 7 or older have a higher risk of simultaneously developing orbital and intracranial complications. They found in their study risk factors for intracranial complications in children served with orbital complications as a result of acute rhino sinusitis. These factors included: above 7years of age, absence of response to initial treatment, neurological alterations, pacifications of the frontal sinus in CT, lateral or upper orbital abscess, the need to drain the orbital abscess, male sex, and African or American [9]. Thus, orbital complications of sinusitis should be considered severe pathologies. They are life-threatening and also threaten the patients quality of life. The appearance of edema in the corner of the eye in a case with acute sinusitis should be recognized immediately and should be taken under serious consideration [10]. Surgical approaches being used in present day practice include endoscopic, open and combined procedures. However, no clear cut benefits of endoscopic over open approaches have yet been demonstrated. In our patient, keeping in view the duration of symptoms (3days), vision threatening disease and age of the patient, urgent surgical intervention in the form of combined frontoethmoidectomy with drainage of subperiosteal abscess was preferred and resulted in full recovery of vision.
Conclusion
Orbital complications of sinusitis are still a frequently seen entity in the modern era of antibiotics with the potential to impair the quality of life of the patient by threatening the vision. In the extreme case, they might prove fatal. Prompt diagnosis by the combined efforts of the otolaryngologist, ophthalmologist, pediatrician/physician followed by early decision-making as to whether medical treatment would suffice or surgical intervention would be required is the key to best visual outcomes.
References
- Radovani P, Vasili D, Xhelili M, DervishI J (2013) Orbital Complications of Sinusitis. Balkan Med J 30(2): 151-154.
- Chandler JR, Langenbrunner DJ, Stevens ER (1970) The pathogenesis of orbital complications in acute sinusitis. Laryngoscope 80: 1414-1428.
- Moloney JR, Badham NJ, McRae A (1987) The acute orbit preseptal (periorbital) cellulites, subperiosteal abscess and orbital cellulites due to sinusitis. J Laryngol Otol Suppl 12: 1-18./a>
- Durand ML (1999) Intravenous antibiotics in sinusitis. Curr Opin in Otolaryngol 7: 7-10.
- Poole MD (1997) Antimicrobial therapy for sinusitis. Otolaryngol Clin North Am 30: 331-339.
- Singh B (1995) The management of sinogenic orbital complications. J Laryngol Otol 109: 300-303.
- Nageswaran S, Woods CR, Benjamin DK, Givner LB, Shetty AK, et al. (2006) Orbital cellulites in children. Pediatr Infect Dis J 25(8): 695-699.
- Okamoto Y, Brenner W (1964) Organic Semiconductors, Rheinhold, Germany.
- Herrmann BW, Forsen JW (2004) Simultaneous intracranial and orbital complications of acute rhinosinusitis in children. Int J of Pediatr Otorhinolaryngol 68(5): 619-625.
- souza DLA, Verde LRC (2011) Orbital and intracranial complications resulting from acute rhinosinusitis: a case report. International Archives of Otorhinolaryngology 15(2).
- Radovani P, Xhumbi K, Golemi H (1989) Enjtjet e perseritura rreth orbits. Revista Mjeksore 6: 49-52.
© 2017 Amit Saini, et al. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






