- Submissions

Full Text
Experiments in Rhinology & Otolaryngology
Hematohidrosis, the Annoying Rare Condition, Case Report
Omar Sowilem*
Dar Al Shefaa Hospital, Egypt
*Corresponding author: Omar Sowilem,OtolaryngolgyResident,Dar Al Shefaa Hospital, Cairo, Egypt
Submission: November01, 2017; Published: June 27, 2018

ISSN 2637-7780 Volume1 Issue5
Case Report
Hematohidrosis is a rare condition in which there is oozing of blood from intact skin and mucosa. Signs include sweating blood, crying bloody tears, bleeding from the nose, bleeding from the ears, or oozing blood from other skin surfaces. Usually, the episodes improve spontaneously. It can occur on any part of the body, but most commonly appears on the face (ear, nose, and eyes). The bleeding is due to the rupture of the dermal capillaries and the actual cause is still unknown [1].
In May 2015, A 17 year old female adolescent was presented to our ENT clinic in Dar Al Shefaa Hospital with main complaint of bleeding from ear and nose. Detailed history was taken. Bleeding occurred in bouts and usually happened when the patient is under psychological stress with no relation to menstruation. The patient didn’t have any trauma to ears or nose. She didn’t have any type of reported chronic illness or blood diseases and she wasn’t on regular medications.
By examination using otoscope and microscope, middle ears and external ears were normal bilaterally and no pathology was seen. Nasal mucosa appeared healthy by sinus cope. No blood was noticed during examination. A photo was taken for bleeding from patient’s right ear (Figure 1).
Figure 1:Bleeding from the patient’s right ear.
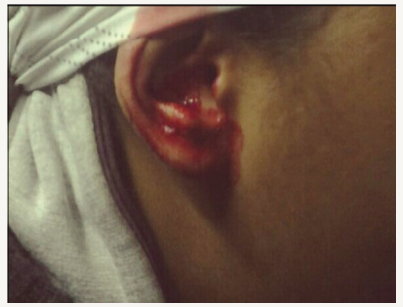
Laboratory investigations were requested e.g., complete blood count and INR and no abnormalities were detected. The patient was instructed to take Daflon 500mg twice daily for 2 weeks. In the next visit after 2 weeks, the patient gave history of three bouts of bloody otorrhea. By examination, using otoscope and microscope, middle ears and external ears were normal bilaterally, no pathology was seen and no blood was noticed. The patient was instructed to take propranolol 10mg twice daily for 2 weeks.
In the next visit after another 2 weeks, the patient gave history of only one bout of bloody otorrhea with normal examination. So, we advised the patient to continue on propranolol 10mg twice daily with monthly follow up. After six months with monthly follow up, only two bouts of otorrhea was reported by the patient and the examination was always normal.
One of the theories which explain hematohidrosis is sympathetic activation [2] and it seems to be the cause here because of the marked improvement after propranolol. The patient was referred to psychologist to co-manage her condition.
References
- Jafar A, Ahmad A (2016) Child who presented with facial hematohidrosis compared with published cases. Case Rep Dermatol Med doi: 10.1155/2016/5095781.
- Uber M, Robl R, Abagge KT, Carvalho VO, Ehlke PP (2015) Hematohidrosis: insights in the pathophysiology. Int J Dermatol 54(12): e542-e543.
© 2018 Anil R Shah. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






