- Submissions

Full Text
Advancements in Case Studies
Case Report-Subdural Empyema as a Life-threatening Complication of Acute Sinusitis
Meghana Pisupati1, Emily L Siegler1*, Ning Zhong2 And Forshing Lui1
1California North state University College of Medicine, USA
2Kaiser Permanente Roseville Medical Center, USA
*Corresponding author: Emily L Siegler, College of Medicine, California North state University, USA
Submission:August 01, 2022;Published: August 08, 2022

ISSN 2639-0531Volume3 Issue4
Abstract
Case Description: A 22-year-old woman initially presented to the emergency department with acute onset of headache and fever. Workup revealed pyogenic meningitis, likely secondary to acute sinusitis. Her condition quickly deteriorated with repeated seizures requiring continuous EEG monitoring. MRI revealed findings compatible with acute bilateral frontal subdural empyema. The patient underwent endoscopic sinus surgery with image guidance for drainage of the empyema. The patient became apneic shortly after the surgical procedure; a repeat CT revealed diffuse cerebral edema and she died despite external ventricular drainage.
Conclusion: Though common and mostly benign, acute sinusitis can lead to disastrous outcomes if the infection spreads to adjacent structures and becomes an intracranial process. Progression can be rapid. Management typically involves broad-spectrum antibiotics as well as surgical debridement and intervention. Subdural empyema, a rare complication of sinusitis, should be suspected if there is clinical evidence of mental status change, meningeal signs, focal neurological findings, or seizures. Interventions, including medications, the timing of surgery, and surgical approach, need to be optimized via collaborative efforts of all physicians and surgeons involved in caring for the patient. A high index of suspicion is the first step in arriving at a correct diagnosis to improve patient outcomes.
Keywords:Sinusitis; Bacterial sinusitis; Meningitis; Empyema; Subdural empyema; Case report
Introduction
Acute sinusitis is a very prevalent, commonly benign condition estimated to affect 1 in 7 adults annually, yet it is also the leading cause of intracranial abscess which has an estimated mortality rate between 10-20% [1,2]. The disease process is characterized by inflammation of the mucosal lining of paranasal sinuses and is sometimes grouped with rhinosinusitis due to the contiguous nature of mucosa in the paranasal sinuses with that of the nasal passages. Acute sinusitis is most commonly viral in etiology, and an estimated two-thirds of patients will experience significant improvement of symptoms without treatment, which typically consists of antibiotics with or without steroids [2]. Today, treatment is largely supportive, with a focus on improving sino-nasal drainage [3]. If symptoms do not improve in a timely fashion, usually within 10 days with typical symptoms or 3-5 days with severe symptoms, a bacterial etiology should be considered [1]. Isolated acute bacterial frontal sinusitis is not common, but its occurrence tends to be highest among adolescents and young adults. This trend tends to be attributed to rapid pneumatization of frontal sinuses that occurs between 6 to 20 years of age [3]. Bacterial sinusitis is most often caused by Haemophilus influenzae, Streptococcus pneumoniae and Moraxella catarrhalis [3]. Sinusitis can affect any of the paranasal sinuses, including the frontal, maxillary, ethmoid and sphenoid sinuses [2]. Of these, frontal sinusitis is associated with a higher risk of intracranial complications due to its close relation to critical structures; frontal sinus infection has the potential to spread to the orbit resulting in blindness or can extend into the anterior and middle cranial fossa leading to intracranial complications, namely meningitis and epidural or subdural empyema or abscess [2,4].
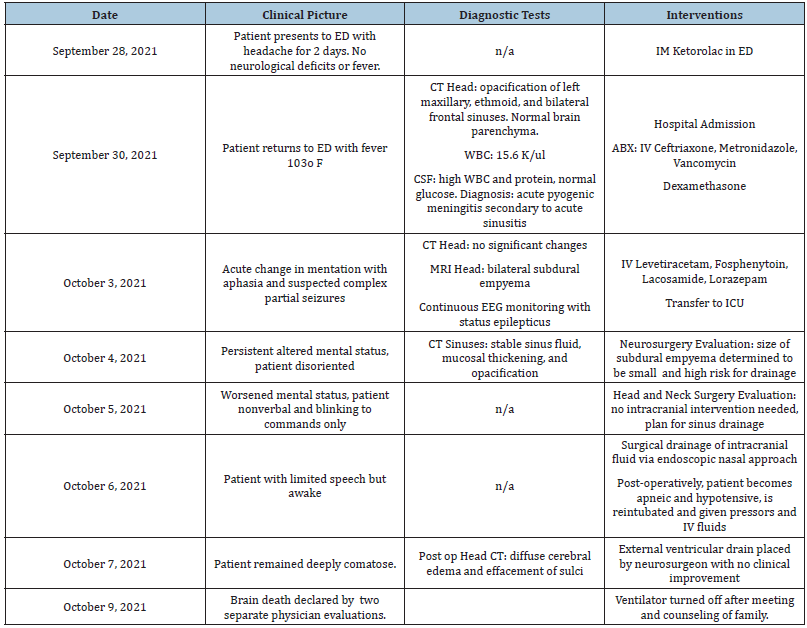
Subdural empyema is the most common intracranial complication and its clinical course can become rapidly fatal if not addressed properly due to severe elevation in intracranial pressure resulting in diffuse cerebral edema, herniation and death [5]. While this phenomenon is well documented in the literature, it has become a relatively uncommon sequence of events over the last decade due to the widespread use of antibiotics. Appropriate treatment with craniotomy and surgical drainage should always be considered instead of limited draining approaches (Table 1).
Table 1: Timeline of patient’s clinical course.
Case Presentation
A 22-year-old woman with obesity and hypertension presented to the emergency department with a throbbing temporal headache for two days. Her headache had initially improved with Acetaminophen, but quickly recurred. Her general and neurological exams were normal. Because the patient was stable and afebrile, she was discharged after her symptoms resolved with an intramuscular injection of Ketorolac and was advised to return if symptoms worsened.
She returned to the emergency department two days later due to new onset of 103 ˚F fever and worsening frontal pulsatile head pain. She had significant bilateral upper extremity myalgia, although she denied any numbness, tingling or weakness in her extremities. There was also no nausea, vomiting, double vision, cough and shortness of breath. Her neurological exam revealed mild neck rigidity. She was mentally clear and alert with no focal neurological signs. Her chest x-ray was normal and CT head revealed opacification of the left maxillary, ethmoid and bilateral frontal sinuses and normal brain parenchyma (Figure 1). The patient’s lab studies showed anelevated WBC count at 15.6K/ul (normal 4-11), with left shift and 88% neutrophils. A spinal tap was performed revealing cloudy CSF with opening pressure 35cm CSF, protein 148mg/dL (normal 15- 45), glucose 45mg/dL (normal) and WBC 3662/dL (normal <4) with 92% polymorphs. Based on these findings, the diagnosis was acute pyogenic meningitis, complicating acute sinusitis. The patient was admitted to the hospital and started empirically on broad spectrum antibiotics with intravenous Ceftriaxone, Metronidazole and Vancomycin as well as dexamethasone. Her fever and headache improved with initiation of treatment. Serology and PCR tests were negative for HIV, HSV, treponema, and enterovirus. CSF gram stain was positive for WBCs but no organisms.
The patient remained clinically stable with minimal symptoms until hospital day four, when she had an acute change in mentation with delirium and aphasia. Neurological examination revealed difficulty finding words, repeatedly asking same questions and where objects were and inability to read. She was unable to answer questions appropriately and was witnessed to have staring spells during which she became unresponsive. IV Levetiracetam was started for complex partial seizures as the clinical diagnosis. Her staring spells continued resulting in addition of IV Fosphenytoin, Lacosamide and intermittent doses of IV Lorazepam. She was also placed on continuous EEG monitor and managed in the intensive care unit.
Repeat head CT did not reveal any significant changes. MRI head then revealed bilateral subdural collections with restricted diffusion, most compatible with bilateral subdural empyema (Figure 2). Extensive paranasal sinus disease was still present. The patient’s neurological status remained the same the following day Neurosurgery was consulted for the subdural empyema. Their initial assessment was that the fluid collections were too small to warrant drainage. The patient was nonverbal and only blinked to commands. Sinus surgery was reconsidered upon stabilization of epileptic activity and the patient was taken for drainage of intracranial fluid by the head and neck surgery team through an endoscopic intranasal approach. The frontal sinuses were micro debrided with thick purulent drainage flushing out.
Figure 1:Admission CT with complete opacification of the left frontal sinus and near-complete opacification of the visualized portions of the left maxillary and ethmoid sinuses. The right frontal sinus is nearly completely opacified. The anterior right ethmoid sinus is opacified. There are no focal calvarial abnormalities.
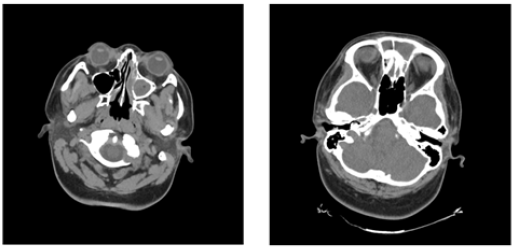
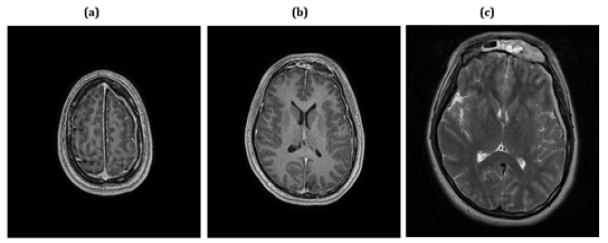
Figure 2: (a) and (b) are T1 weighted MRI with contrast showing bilateral L>>R subdural collections with contrast enhancement. (c) is a diffusion weighted image showing restricted diffusion of the subdural collections compatible with empyema. This combination of findings is compatible with bilateral left more than right subdural empyema.
During the immediate post-operative period in the postanesthetic care unit, the patient became apneic and hypotensive. She was reintubated and started on pressors and IV fluids. At this time, the patient’s pupils were fixed and dilated with GCS 3. Repeat head CT showed diffuse cerebral edema and effacement of sulci (Figure 3). External ventricular drain was placed by the neurosurgeon with no clinical improvement. The patient then lost all her brainstem reflexes. The patient finally passed away in the intensive care unit.
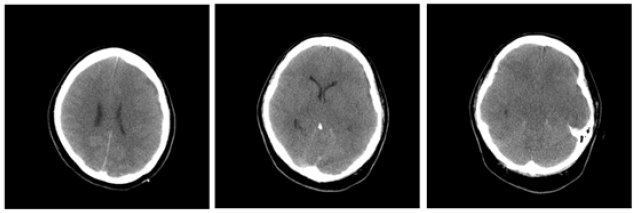
Figure 3:Post-surgical CT showed loss of grey-white differentiation diffusely over both hemispheres, accompanied by diffuse loss of sulcation and loss of the basal cisterns throughout, most compatible with diffuse severe generalized cerebral edema. (R>L).
Discussion
We reported a tragic case of the uncommon and devastating complications of a relatively common problem of acute sinusitis. Sinusitis is a common and manageable condition with rare intracranial complications. When sinusitis complications do occur, they most commonly involve local tissues and the orbit [6]. Intracranial complications are considered most rare, encompassing subdural and extradural empyema, brain abscess, meningitis, cavernous sinus thrombophlebitis and sphenoid osteomyelitis. Of these, subdural empyema is the most common [6]. Mortality rate of subdural empyema has historically been as high as 15-41% despite timely and appropriate care [7]. However, imaging modalities such as CT and MRI, as well as more widespread access and use of antibiotics, have improved early diagnosis and treatment. Recent studies indicate that subdural empyema mortality has decreased to 6-15% [7]. Of note, there is also a trend of susceptible immunocompromised patients accounting for a greater portion of cases overall [8,9].
When it does occur, subdural empyema requires immediate recognition and management, as the disease process may rapidly increase intracranial pressure and lead to death or coma within 24- 48 hours [10]. Subdural empyema is more common in men, who make up 80% of cases and are within individuals 10-40 years of age [11]. Intracranial empyema in the clinical setting is associated with signs of infection including fever, headache, seizures, nausea, vomiting and acute mental status changes. However, due to this vague symptomatic presentation, early diagnosis is difficult and CT head may be required, with a median time to diagnosis of 2 days from initial presentation [11].
Management of subdural empyema involves but is not limited to empirical treatment with broad spectrum antibiotics, prophylactic anticonvulsants, and surgical treatment including craniotomy or burr hole approaches [12,13]. The antibiotics need to cover the usual rhinosinus organisms including Haemophilus influenzae, Streptococcus pneumoniae, Moraxella catarrhalis and anaerobes [3]. As in our case, the use of antibiotic therapy alone is not enough. Surgical drainage is nearly always indicated. The patient’s mental status at the time of surgery is the best indicator for mortality. Of the two surgical methods, craniotomy has a better clearance of empyema and reduces the need for reoperation [11]. Additionally, burr hole or endoscopic trans-nasal approaches may be used for drainage, as was pursued in this case and has demonstrated similar efficacy to open neurosurgical approaches [14]. Unfortunately, our patient did not respond to the limited surgical approach. Overall, delay in surgery is correlated with worse clinical prognosis. However, surgical outcome depends on several factors, including preoperative level of consciousness, timing and aggressiveness of treatment and progression of disease. Additional poor prognostic factors include encephalopathy and sterile cultures, which were present in this case [15].
In our patient, clinical decision making prioritized surgical debridement of the sinus infection for source control. The above literature supports such an approach, as obtaining source control is key for patient survival. In retrospect, we were debating if the patient’s outcome may have been better if the surgical approach was craniotomy [11]. The size and volume of the subdural collections may be misleading especially in a young patient like ours. Any small increase in subdural collection may lead to large increase in intracranial pressure and the complications of herniations. We retrospectively observe that the patient’s instability may not have been fully apparent at time of evaluation for surgery. Her inflammatory state from persistent meningitis and recent status epilepticus likely predisposed the patient to cerebral edema. We also hypothesize that the stress of anesthesia and surgery may have contributed to a hypoxic-ischemic cerebral state, exacerbating an underlying inflammatory process and diffuse cerebral edema and the patient’s tragic death. In general, intracranial complications of sinusitis are more commonly seen in children and young adults, with a peak age of 13 years old [2]. The rare but severe complications of sinusitis must be vigilantly watched for, as young patients who develop intracranial complications of sinusitis have a greater risk for edema, herniation, and irreversible damage due to lack of atrophy and potential space in younger patients [15]. Timing and risk benefit analysis for surgical intervention, and types of surgical approach in patients with subdural empyema, require further study.
Conclusion
Acute sinusitis is a common and relatively benign condition. Intracranial extension of the sinus infection is uncommon yet it can be devastating if not treated adequately and in a timely manner. Subdural empyema is the most common intracranial complication of acute frontal sinusitis. Careful observation of the patient clinically with laboratory and imaging studies will alert clinicians to these serious complications. Once the diagnosis of pyogenic meningitis or subdural empyema is made, collaborations in management among infectious disease physicians, intensivists, neurologists and surgeons is most important in improving the outcome. These consist of the use of appropriate antibiotics, use and choice of anticonvulsants, and type and timing of surgical approaches. The surgical approach choices between a limited burr hole or endoscopic drainage versus craniotomy needs further study and clarification. A high index of suspicion, especially with acute subdural empyema as a life-threatening complication of acute sinusitis, is of utmost importance for improving the clinical outcomes of patients.
Author Contributions
MP, ELS, and NZ participated in the extraction of case information. MP and ELS participated equally in the literature review, drafting, revision, and submission of the manuscript. FL supervised all parts of the manuscript preparation process and provided guidance for pre-submission revisions. All authors have given final approval to the manuscript.
Conflict of Interest Statement
No individual authors have any conflicts of interest to disclose.
Funding Statement
No research funding, sponsors, or other financial contributions were utilized for this study.
References
- DeCastro A, Mims L, Hueston WJ (2014) Rhinosinusitis. Primary Care 41(1): 47-61.
- Wyler B, Mallon WK (2019) Sinusitis update. Emergency Medicine Clinics of North America 37(1): 41-54.
- Sohal M, Tessema B, Brown SM (2016) Medical management of frontal sinusitis. Otolaryngologic Clinics of North America 49(4): 927-934.
- Al Yaeesh I, Al Omairin A, Al Shakhs A, Ali Almomen, Zahra Almomen, et al. (2020) The serious complications of frontal sinusitis, a case series and literature review. J Surg Case Rep 2020(12): rjaa474.
- Quraishi H, Zevallos JP (2006) Subdural empyema as a complication of sinusitis in the pediatric population. International Journal of Pediatric Otorhinolaryngology 70(9): 1581-1586.
- Benevides GN, Salgado GA, Ferreira CR, Felipe-Silva A, Gilio AE (2015) Bacterial sinusitis and its frightening complications: subdural empyema and Lemierre syndrome. Autops Case Rep 5(4): 19-26.
- Osborn MK, Steinberg JP (2007) Subdural empyema and other suppurative complications of paranasal sinusitis. The Lancet Infectious Diseases 7(1): 62-67.
- Bruner DI, Littlejohn L, Pritchard A (2012) Subdural empyema presenting with seizure, confusion and focal weakness. West J Emerg Med 13(6): 509-511.
- Goodkin HP, Harper MB, Pomeroy SL (2004) Intracerebral abscess in children: historical trends at Children’s Hospital Boston. Pediatrics 113(6): 1765-1770.
- Waseem M, Khan S, Bomann S (2008) Subdural empyema complicating sinusitis. The Journal of Emergency Medicine 35(3): 277-281.
- French H, Schaefer N, Keijzers G, Barison D, Olson S (2014) Intracranial subdural empyema: A 10-Year case series. Ochsner J 14(2): 188-194.
- Mat Nayan SA, Mohd Haspani MS, Abd Latiff AZ, Abdullah JM, Abdullah S (2009) Two surgical methods used in 90 patients with intracranial subdural empyema. Journal of Clinical Neuroscience 16(12): 1567-1571.
- Garin A, Thierry B, Leboulanger N, Blauwblomme T, Grevent D, et al. (2015) Pediatric sinogenic epidural and subdural empyema: The role of endoscopic sinus surgery. International Journal of Pediatric Otorhinolaryngology 79(10): 1752-1760.
- Agrawal A, Timothy J, Pandit L, Shetty L, Shetty JP (2007) A review of subdural empyema and its management. Infectious Diseases in Clinical Practice 15(3): 149-153.
- Peters R (2006) Ageing and the brain. Postgrad Med J 82(964): 84-88.
© 2022 Emily L Siegler. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






