- Submissions

Full Text
Techniques in Neurosurgery & Neurology
A Treatable Leukodystrophy Presenting as Familial Spastic Paraparesis with Homozygous Variation in MTHFR Gene- A Case Report
Aswin G1, Philo Hazeena P2*, Javed Ahmed3 and Shankar V4
1Senior resident Neurology, India
2Neurology, India
3Consultant neurologist, India
4Professor and Head Neurology, India
*Corresponding author: Philo Hazeena, Senior resident Neurology, India
Submission: August 02, 2021;Published: September 29, 2021

ISSN 2637-7748
Volume4 Issue4
Abstract
The MTHFR enzyme deficiency is an autosomal-recessive inborn error of folate metabolism. The Clinical presentation can vary from asymptomatic to severe neurological manifestations with pyramidal, cerebellar signs, dementia, and epileptic seizures. We report a 23-year-old male with familial gradually progressive spastic paraparesis with seizures and poor scholastic performance. Patient was diagnosed with MTHFR enzyme deficiency presenting as leukodystrophy with spastic paraparesis, which is treatable on early diagnosis.
Keywords: Methylene tetrahydrofolate reductase; Spastic paraparesis; Leukoencephalopathy
Introduction
Methylenetetrahydrofolate reductase (MTHFR) is a cytoplasmic enzyme that catalyses’ the reduction of 5,10- methylenetetrahydrofolate to 5-methyl tetrahydrofolate. Mutations in MTHFR gene lead to hyperhomocysteinemia and homocystinuria due to abnormalities in the remethylation of homocysteine to methionine. Even mild hyperhomocysteinemia represents an important risk factor for atherosclerosis and vascular disease, including stroke, and it also contributes to the development of cognitive impairment [1]. Patients may present with a wide spectrum of clinical features, including cognitive and neuropsychiatric changes, movement disorders, spasticity and seizures. Hereditary spastic paraplegia is described as a genetic, heterogeneous disorder leading to axonal degeneration of the spinal pathways and mostly classified in either pure or complex [2]. The MTHFR enzyme deficiency is an autosomal-recessive inborn error of folate metabolism. Clinical manifestations can vary from asymptomatic to severe neurological manifestations with pyramidal, cerebellar signs, dementia, and epileptic seizures. Hereby, we report a 23-year-old male with familial gradually progressive spastic paraparesis with seizures and poor scholastic performance. Patient was diagnosed with a type of leukodystrophy, which is treatable on early diagnosis.
Case Report
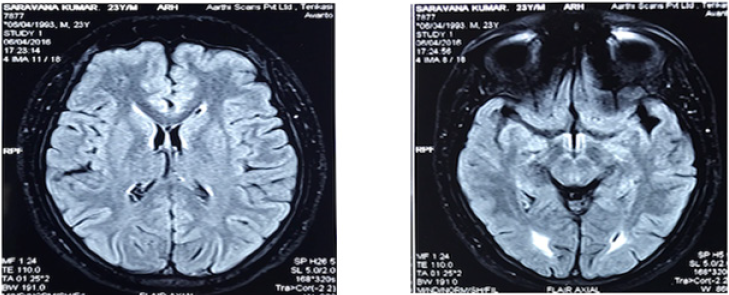
A 23-year-old male patient born out of 3rd degree consanguineous parentage with normal perinatal history, presented to us with unsteadiness while walking and stiffness of both lower limbs. The symptoms had worsened after a fall. Patient had difficulty to grip slippers for the past 3 years, which was gradual in onset and slowly progressing to an extent that he has changed his slippers to one with a strap. Past two years patient noticed that he was tripping over small objects due to the stiffness and has difficulty in wearing his pants while standing, as he would lose balance. For the past one year he also noticed difficulty in going up and down the stairs with tightness of legs. He had poor scholastic performance since 8th standard. He had an episode of tonic clonic movements of both upper limbs and lower limbs with tongue bite 1 ½ years back and is being treated with Tablet Leviteracetam. He was able to perceive the sensations normally in the lower limbs. There was no worsening of symptoms in the dark. He didn’t have any cranial nerve and bladder involvement. There was a significant family history with his younger brother having similar complaints of spastic paraparesis. He complained of headache 6-8 episodes per month lasting more than 6 hours, throbbing type, associated with photophobia and phonophobia. Clinical examination revealed normal cognitive assessment with no cranial nerve deficits. Motor system evaluation revealed hypertonia of both lower limbs, reflexes were brisk in both lower limbs with bilateral extensor plantar response and a spastic gait. His investigations showed a normal hemogram, renal, liver and thyroid function tests. His vitamin B12 levels were found to be low (123pg/ml). On evaluating further for low vitamin B12 levels, his serum homocysteine levels were found to be high. Serum Homocysteine levels were (>50). Neuroimaging showed a patchy T2 hyperintensities involving the bilateral occipital periventricular white matter with confluent T2 hyperintensities involving the bilateral centrum semiovale and high frontal deep white matter (Figure 1). MRI spine and nerve conduction study of all four limbs was normal. In view of a significant family history with features of spastic paraparesis along with MRI showing white matter changes, we evaluated him further for the hereditary causes of spastic paraparesis. The genetic panel for leukodystrophy and hereditary spastic paraplegia was sent, which showed a homozygous missense variation in the exon 2 of MTHFR gene (c.459C>G) (p.lle153Met) .Patient was diagnosed to have methylene tetrahydrofolate reductase deficiency. Patient was treated with vitamin B12 (1.5mg/day), folic acid (15mg/day), and vitamin B6 (30mg/day) and on initial follow up, patient showed improvement in his gait.
Figure 1: MRI brain.
Discussion
The MTHFR enzyme deficiency is an autosomal-recessive
inborn error of folate metabolism. Clinical manifestations can vary
from asymptomatic to severe neurological manifestations with
pyramidal, cerebellar signs, dementia, and epileptic seizures. The
symptoms can manifest over a wide range of age from neonates to
the adulthood. Infants presents with seizures, hypotonia, apnoea,
microcephaly, progressing to coma, and death if untreated due
to severely reduced residual enzyme activity [3]. Developmental
delay, seizures including progressive myoclonic epilepsy,
psychiatric disturbances, spastic gait, and ataxia occur in childhood
and adolescent onset. In adult-onset enzyme deficiency, spastic
paraparesis mimicking hereditary spastic paraplegia, psychotic
episodes, cognitive disorder, stroke, peripheral neuropathy, and
relapsing encephalopathy are the clinical manifestations [4].
Patients show moderate homocystinuria, hyperhomocysteinemia
with low or low-normal methionine levels, radiologically, they
show brain white matter changes (leukoencephalopathy). The
leukoencephalopathy is usually periventricular, with a posterior
predominance, and can involve U fibers. Our patient presented with
gradually progressive spastic paraplegia with imaging features of
leukoencephalopathy. Serum homocysteine was high with low
vitamin B12 levels. Genetic testing showing a homozygous missense
variation in the exon 2 of MTHFR gene (c.459C>G) (p.lle153Met)
[5]. He was diagnosed to have methylene tetrahydrofolate
reductase deficiency Mahale R et al5 in India observed similar kind
of case report in child with rapidly progressive spastic paraplegia
and behavioural disturbance of 3 month duration. Another case
report by Gales et al. [6] of two adult siblings who experienced
focal epilepsy at 18 years old as a first disease manifestation, without other symptom during several years. Upon diagnosis, both
patients received metabolic treatment comprising B9, B12 and
betaine which has stopped the occurrence of seizures, allowing
discontinuation of anti-epileptic drugs. Brain MRI showed a mostly
periventricular white matter changes in 71% of cases. All patients
stabilized or improved following metabolic treatment. Despite being
rare, adolescence/adult onset MTHFR deficiency can nevertheless
be successfully treated. Therefore, homocysteine levels should be
tested in various unexplained neuro-psychiatric syndromes like
epilepsy or spastic paraparesis, even if isolated, since waiting for
completion of the clinical picture is likely to increase the risk of
irreversible neurological damage.
Our patient’s presentation was similar to the study by Lossos
et al. [7] where both pairs of siblings presented with a similar
combination of progressive spastic paraparesis and polyneuropathy,
variably associated with behavioural changes, cognitive
impairment, psychosis, seizures, and leukoencephalopathy,
beginning between the ages of 29 and 50 years. The finding was in
contrast to a study by Iida S et al. [8] where a 15-year-old boy with
MTHFR deficiency who presented with a slowly progressive decline
of school performance and a spastic gait. Rapidly deteriorating
psychosis and repetitive seizures triggered by a febrile infection
prompted neurological investigation. He had significantly elevated
total plasma homocysteine and urinary homocystine levels, as
well as a decreased plasma methionine level. Brain magnetic
resonance imaging (MRI) revealed leukoencephalopathy. DNA
gene sequencing showed c.446_447 del GC ins TT and c.137G >
A and c.665C > T heterozygous mutations in the MTHFR gene of
the patient. Oral administration of betaine drastically improved
his clinical symptoms within a few months. After 8 months
of treatment, his total plasma homocysteine level moderately
decreased; and the plasma methionine concentration became
normalized. Timely molecular diagnosis and treatment with high
dose of methyl donors is critical for the survival of these patients.
Identification of the pathogenic variants of MTHFR gene may extend
the knowledge about the spectrum of mutations and highlight the
proper genotype-phenotype correlation.
Conclusion
In adults presenting with familial gradually progressive spastic paraparesis, homocysteine levels should be evaluated. Generally, leukodystrophies are considered non treatable. Though, MTHFR deficiency is rare, it should be considered as an important differential while evaluating patients presenting with familial spastic paraparesis as it can be treated with early diagnosis.
References
- Vieira D, Florindo C, Tavares De Almeida I, Macário MC (2020) Adult-onset methylenetetrahydrofolate reductase deficiency. BMJ Case Rep 13(3): 13-16.
- Beukelaer N, Bar On L, Hanssen B, Peeters N, Prinsen S, et al. (2021) Muscle characteristics in pediatric hereditary spastic paraplegia vs. bilateral spastic cerebral palsy: an exploratory study. Front Neurol 12: 1-10.
- Khan FMA, Dave D, Rohatgi S, Nirhale S, Rao P, Naphade P (2019) MTHFR mutation- A rare potentially treatable cause of adult-onset complicated hereditary spastic paraplegia. J Neurol Sci 405: 325.
- Lynch DS, Wade C, Paiva ARB De, John N, Kinsellaja, et al. (2019) Practical approach to the diagnosis of adult-onset leukodystrophies: an updated guide in the genomic era. J Neurol Neurosurg Psychiatry 90(5): 543-554.
- Mahale R, Gautam J, Arunachal G, Alappati S, Varghese N, et al. (2021) Rapidly progressive spastic paraplegia due to hyperhomocysteinemia in child with MTHFR gene mutation and mitochondrial Complex I deficiency: A rare association. J Pediatr Neurosci.
- Gales A, Masingue M, Millecamps S, Giraudier S, Grosliere L, et al. (2018) Adolescence/adult onset MTHFR deficiency may manifest as isolated and treatable distinct neuro-psychiatric syndromes. Orphanet J Rare Dis 13(1): 1-8.
- Lossos A, Teltsh O, Milman T, Meiner V, Rozen R, et al. (2014) Severe methylenetetrahydrofolate reductase deficiency: Clinical clues to a potentially treatable cause of adult-onset hereditary spastic paraplegia. JAMA Neurol 71(7): 901-904.
- Iida S, Nakamura M, Asayama S, Kunieda T, Kaneko S, et al. (2017) Rapidly progressive psychotic symptoms triggered by infection in a patient with methylenetetrahydrofolate reductase deficiency: A case report. BMC Neurol 17(1): 47.
© 2021 Philo Hazeena P. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






