- Submissions

Full Text
Research in Pediatrics & Neonatology
Harlequin Fetus: A Rare and Unique Ichthyosis. A Case Report at the Sikasso Hospital (Mali)
Cissouma Assetou1*, Traore Soumaila Alama2, Traore-Kissima Abdoulaye3, Kassogué Djibril4 Coulibaly Mamadou Bernard5, Dembele Guediouma, Sidibé Moro and Traore Mamadou6
1Pediatric Department of Sikasso Hospital, Mali
2Gynecology and Obstetrics Department of Sikasso Hospital, Mali
3Cardiology Department of Sikasso Hospital, Mali
4Pediatric Department of Timbuktu Hospital, Mali
5Pediatric Department of the Mali Hospital, Mali
6Referral Health Center of the commune 5, Mali
*Corresponding author: Assetou Cissouma, Pediatrician, Research Fellow at Sikasso Hospital, Mali
Submission: August 29, 2021; Published: October 26, 2021

ISSN: 2577-9200 Volume6 Issue1
Abstract
Ichthyosis is clinically characterized by the existence of visible flakes on the skin. The four main hereditary ichthyosis are: ichthyosis vulgaris autosomal dominant transmission, X-linked ichthyosis, lamellar ichthyosis, and congenital ichthyosiform necrolysis. At birth, the ichthyosis can be unapparent or realize collodion baby or Harlequin fetus. The Harlequin fetus is the most severe form and usually lethal ichthyosis. It is transmitted as an autosomal recessive. This is clinically a rare form of skin disease with large, thick, and yellowish scales, separated by deep red crevices giving the appearance of a baby frog. We here review a rare form of Harlequin fetus admitted to the neonatal unit at day 1 of life.
Keywords: Harlequin fetus; Ichthyosis; Newborn
Introduction
The term ichthyosis comes from the Greek word ichthyus: fish scale. It brings together a heterogeneous set of congenital or acquired pathologies characterized by cutaneous xerosis with excessive desquamation, skin inflammation [1-3]. They are distinguished by their mode of transmission, age of onset, clinical appearance and causal genetic abnormality [1-3]. The baby Harlequin is an extremely serious and often lethal form of ichthyosis, its incidence is approximately 1 in 300,000 births, it is transmitted in an autosomal recessive manner by mutations in the ABCA12 gene [3,4]. This rare ichthyosis is clinically manifested from birth by an appearance of skin enclosed in large, thick, yellowish scales, separated by deep red crevices [4].
Observation
This is a newborn female child admitted on the first day of life, third sibling, from the Sikasso region. Third administrative region of Mali (South of Mali), of first-degree consanguineous parents, in the history we find: a pregnancy not followed and carried to term, the infectious anamnesis was negative with an absence of medication or toxic substances. during pregnancy, an absence of similar cases in the family and vaginal delivery. The somatic examination showed a weight of 3.5kg, a height of 50cm, a head circumference of 34cm, a heart rate of 140 beats/minute, a respiratory rate of 32cycles/minute and pulsed oxygen saturation. at 98%. From birth, mucocutaneous examination showed skin with large, thick, yellowish scales separated by deep red crevices (Figure 1), a particular facies with splitting and ectropion, and edematous extremities (Figure 2). The biological assessment including a normal blood count, a normal ionogram and a C reactive protein at 12mg/ml. An x-ray workup including chest x-ray, abdominal ultrasound, cardiac ultrasound and transfontanellar ultrasound were normal. Given the severity of the skin involvement and the resulting dehydration, our patient received symptomatic treatment and broad-spectrum antibiotic therapy (central route given the difficulty of taking the peripheral route). The evolution was marked by the worsening of the clinical picture despite wellconducted treatment, resulting in death at one week of life in a picture of severe collapse. The genetic study was not carried out due to lack of funds, genetic counseling was offered to parents, and counseling for monitoring future pregnancies.
Figure 1: The baby harlequin showing skin with large, thick, yellowish scales separated by deep red crevices.
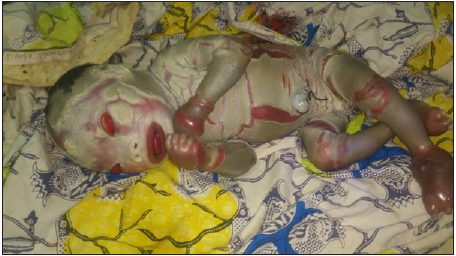
Figure 2: The baby harlequin with characteristic eversion of the eyelids (ectropion) and characteristic eversion of the lips (eclabion), ears and nose.

Discussion
Ichthyosis is clinically characterized by the existence of visible
scales on the skin. The positive diagnosis of hereditary ichthyosis
was easy given the scaling appearance of our patient’s skin. An
ichthyosis is first defined on clinical examination by [1,3,5]: the
appearance of the scales (size, color, thickness); retention (respect
for large folds) or proliferative (non-respect for large folds); the
existence of erosion or bubbles. The other elements used to classify
the different forms are the age of onset, the type of inheritance. The
typing of the different forms still needs to progress with the study
of the biological abnormalities involved and the characterization
of the genetic abnormalities which are already specified in certain
cases [2,3,5].
Characterization of the type of ichthyosis was more difficult, due
to the technical and financial difficulties in obtaining pathological
examination and genetic tests. According to the consensus meeting
of international ichthyosis experts in Sorèze in 2009 [1,2,7], the
decision tree remains based on easily accessible clinical and
paraclinical data: syndromic or not, semiological characteristics,
type of transmission. , age of onset. The involvement of the major
folds (proliferative hyperkeratosis) led us to rule out the diagnosis
of ichthyosis vulgaris and the female involvement that of X-linked ichthyosis. The absence of erythroderma led us to rule out the
diagnosis of dry congenital ichthyosiform erythroderma (EICS).
The appearance of the scales (large adherent scales), and their
generalized arrangement with involvement of the large folds and
the absence of erythema, led us to classify our patient in the group
of lamellar ichthyosis proper. Harlequin ichthyosis is the most
serious and often fatal form. It is inherited autosomal recessively
[5-7]. This syndrome results clinically at birth by a newborn
enclosed in large, thick, yellowish scales, separated by deep red
crevices. The extreme skin tension is responsible for the particular
frog face with characteristic eversion of the eyelids (ectropion), and
also a characteristic eversion of the lips (eclabion), ears and nose.
The extremities are swollen as a result of strictures by massive
thickening of the skin as in our newborn [6-8]. Children alive at birth
quickly die within days of respiratory, infectious or dehydration
complications [8]. There is currently no specific curative treatment
for ichthyosis. The care given several times a day, without curing,
nevertheless allows an acceptable social life. Treatment is most
often symptomatic only and consists of daily local care sometimes
combined with systemic treatments. Multidisciplinary care, most
often hospital, is necessary. Emollient and retinoid treatments are
the treatment of choice for severe ichthyosis, their use improves
skin condition by reducing hyperkeratosis and increasing heat
tolerance, it prevents or improves ectropions [9]. This treatment
requires close medical supervision [8,9].
Rajpopat S et al. [5] reported in a study of 45 cases of baby
harlequin in 2011 that the overall survival rate was 56% in this
study. Death usually occurs within the first three months of life
from sepsis or respiratory failure in 75% of cases. The antenatal
diagnosis of the baby harlequin is possible two methods are
proposed [1,5,9,10]: the study of the amniotic fluid at 17 weeks
of pregnancy can show lipid droplets characteristic of the baby
harlequin and the examination by electron microscopy of the fetal
skin biopsy performed between 19 and 23 weeks of intrauterine
life show early hyper keratinization of the stratum corneum. A few
authors have successfully diagnosed cases of baby harlequin with
a family history of ichthyosis by prenatal 3D and 4D ultrasound;
ultrasound signs were skin contracture, flattened ears, nasal
hypoplasia, everted eyelids, a fish-like mouth, macroglossia, and
a persistent open fetal mouth [11,12]. Given the catastrophic
prognosis and the pain suffered by the child, when the diagnosis
is made before birth, other teams in France evoke the possibility
of a medical termination of pregnancy or else propose the
implementation of focused palliative care. on pain management
and comfort [13]. Likewise, palliative care is offered from the outset
if the diagnosis is made at birth. This team reports the observation
of a baby harlequin, diagnosed in utero at 32 weeks; the birth took
place at 35 weeks old, the child lived for 12 hours in palliative care
with his mother, in a mother-child room in the neonatal unit.
Conclusion
Baby harlequin is a rare and severe form of congenital ichthyosis, which can be fatal through dehydration and infection. It requires multidisciplinary care from birth. Treatment with emollients and oral retinoids could improve patient survival, however medical termination of pregnancy or palliative care remains possible due to the extreme severity of the prognosis and the pain endured by the child.
Parental Consent
Informed consent from the parents was obtained for the publication.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Lorette G, Arbeille B, Grangeponte MC (1999) Ichtyoses. Encycl Med Chir Dermatol 98-195-A-10:12.
- Rodríguez-Pazos L, Ginarte M, Vega A, Toribio J (2013) Autosomal recessive congenital ichthyosis. Actas Dermosifiliogr 104(4): 270-284.
- Chiavérini C (2009) The French Society of Pediatric Dermatology. Genetic ichthyosis. Ann Dermatol Venereol 136: 923-934.
- Harvey HB, Shaw MG, Morrell DS (2010) Perinatal management of harlequin ichthyosis: A case report and literature review. J Perinatol 30(1): 66-72.
- Rajpopat S, Moss C, Mellerio J, Vahlquist A, Ganemo A, et al. (2011) Harlequin ichthyosis: A review of clinical and molecular findings in 45 cases. Arch Dermatol 147(6): 681-686.
- Martínez-García S, Vera A, Romero J, Crespo V (2003) Feto Arlequin. Actas Dermosifiliogr 94(6): 392-394.
- Oji V, Tadini G, Akiyama M, Bardon CB, Bodemer C, et al. (2010) Revised nomenclature and classification of inherited ichthyoses: Results of the first ichthyosis consensus conference in sorèze 2009. J Am Acad Dermatol 63(4): 607-641.
- Ortiz-Brugués A (2013) Harlequin ichthyosis. Piel (barc) 28(10): 583-590.
- Thomas AC, Cullup T, Norgett EE, Hill T, Barton S, et al. (2006) ABCA12 is the major harlequin ichthyosis gene. J Invest Dermatol 126(11):2408-2413.
- Ahmed H, O’Toole EA (2014) Recent advances in the genetics and management of harlequin ichthyosis. Pediatr Dermatol 31(5): 539-546.
- Bongain A, Benoit B, Ejnes L, Lambert JC, Gillet JY (2002) Harlequin fetus: Three-dimensional sonographic findings and new diagnostic approach. Ultrasound Obstet Gynecol 20(1):82-85.
- Basgul AY, Kavak ZN, Guducu N, Durukan B, Isci H (2011) Prenatal diagnosis of congenital harlequin ichthyosis with 2D, 3D, and 4D ultrasonography. Clin Exp Obstet Gynecol 38(3): 283-285.
- Bétrémieux P, Druyer J, Bertorello I, Huillery ML, Brunet C, et al. (2016) Antenatal palliative plan following diagnosis of fetal lethal condition: Rennes teaching hospital experience. J Gynecol Obstet Biol Reprod (Paris) 45(2): 177-183.
© 2021 Assetou Cissouma. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






