- Submissions

Full Text
Research in Pediatrics & Neonatology
Necrotizing Enterocolitis & Feeding …An Update
Amr Ismael M Hawal*
Specialist Pediatrics & Neonatology, Prime Multispeciality Medical Center, UAE
*Corresponding author: Dr. Amr Ismael M Hawal, Specialist Pediatrics & Neonatology, Prime Health Care Group, Prime Multispeciality Medical Center, Ajman, UAE, Tel: +971504822408/+971582221971; Email:amr106@gmail.com,dr.amrhawal@primehealth.ae
Submission: October 02, 2017; Published: December 21, 2017

ISSN: 2576-9200 Volume1 Issue3
Introduction
I. Epidemiology
II. Pathophysiology
III. Diagnosis
IV. Management
V. Prevention
The Case Begins
a) RK is a male baby (31+6wks. gestation), born to a 29 years old woman, Primipara, A positive, with negative serology and her antenatal scan revealed twins.
b) Three days prior to delivery she was given Betamethasone because of preterm labor.
c) The baby was delivered by preterm NVD.
d) Cried soon after birth but owing to poor respiratory efforts, needed intubation and ventilation.
e) APGAR scores of 6 and 8 at 1 & 5 minutes respectively.
f) He was admitted to the NICU for management of prematurity and respiratory support (Figure 1).
Figure 1:

g) His initial chest x-ray was unremarkable. Started on IV Ampicillin and Gentamicin owing to high risk of infection but were discontinued after 48 hours as he remained well and sepsis screen was normal along with sterile blood culture.
h) He could be extubated to non invasive ventilator.
i) He could be trialled off to room air by day 5 of life and remained on room air that well tolerated.
j) The baby could be commenced on feeds and could be graded up to nearly full feeds (4ml per kg per hour) by day 5 of life. Feeds were well tolerated.
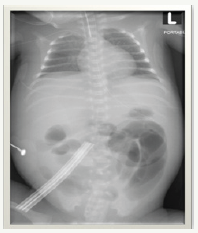
k) On day 7 of life, he was noted to have abdominal distension that was rapidly progressive to a shiny red abdomen with increased gastric aspirates (Figure 2 & 3).
Figure 2:
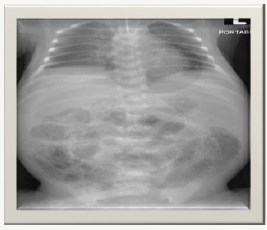
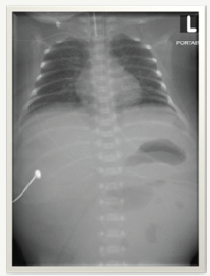
Figure 3:

So, baby was kept NPO and commenced on antibiotics but as there was rapid deterioration in his clinical condition, over a period of couple of hours, baby was started on Meropenem along with Amikacin & Metronidazole. Baby needed ventilation with high parameters demonstrated low white cell count, absolute neutropenia, thrombocytopenia and a CRP of 108mg/L. He grew Klebsiella pneumoniae in the blood and this was sensitive to Meropenem.
In the subsequent 72hours, due to features of DIC, he needed blood and fresh frozen plasma along with platelet concentrates infusion. Supportive treatment with immunoglobulin was given. He needed inotropes support with Dopamine for a period of 72hours and could be weaned down. There was hypoalbuminemia noted and was treated with Albumin infusion. Acidosis, Hyperglycemia and raised lactate were also noted and treated. All these features were suggestive of Multi organ Dysfunction.
24hours later, baby was noted to have pneumo-peritoneum that was treated by insertion of a multi drain (too sick to be exposed to surgical exploration).
His abdominal distension was noted to gradually resolve and once he was noted to be hemodynamically stable along with improving platelet counts, normalized coagulation profile with declining CRP levels and sterile blood culture (Figure 4).
Figure 4:
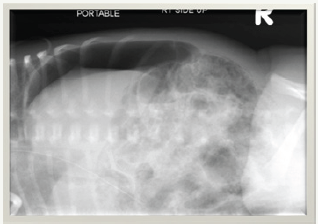
Figure 5:
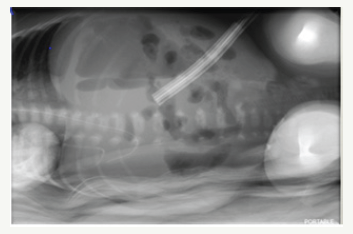
Baby underwent laparotomy with resection and Anastomosis of his intestine and formation of ileostomy on (day 13 of life and 6 days following drain insertion).One perforation was noted at DJ junction and multiple perforations were noted proximal to ileocecal valve and approx. 15cms of bowel resection was performed followed by end to end anastomosis. The histopathology of the bowel specimen sent revealed Necrotizing Enterocolitis (Figure 5).
NEC Introduction
Necrotizing enterocolitis (NEC) was first described by Mizrahi et al. in 1965, and was classified into three stages based on the severity of the clinical presentation and treatment strategies by Bell et al. in 1978.
• NEC is a disease of premature infants
• Complicated perinatal course
• Factors that promote abnormal bacterial colonization and overgrowth
• A history of enteral formula feeding
No consistent association; gender, race or socioeconomic status.
Epidemiology of NEC
a. Affects 6-8% of VLBW infants.
b. Widely varying incidence between centers.
c. Incidence inversely related to degree of prematurity.
d. No seasonal or sex predilection.
e. There are inverse correlations between gestational age or birth weight and the incidence of NEC, as demonstrated in multicenter and large population-based studies, its prevalence being 7%–11% in very low birth weight infants who weight less than 1,500g.
Age at diagnosis is inversely related to gestational age and degree of prematurity [1]
Table 1:
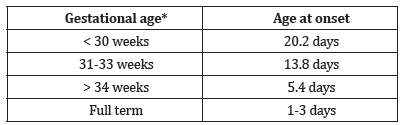
Factors that alter patterns of bacterial colonization in ill premature infants
a. Widespread use of broad-spectrum antimicrobials promotes colonization by invasive and opportunistic microbial pathogens.
b. Clinical illness reduces enteral feeding, influencing intestinal bacterial colonization, immune system maturation and barrier function.
c. Reduction in BM feeding due infants’ clinical illness, reduced availability BM, or alterations due to freeze/thawing of BM.
d. Despite this progress in technologies there has been no method to identify infants who would be ideal candidates for therapy or those who will progress to more severe stages of disease.
Pathophysiology of NEC
Figure 6:
Diagnosis of NEC
a. High index of suspicion based on history and physical findings.
b. Early appearances are subtle and easily confused with neonatal sepsis.
c. Apnea (pause in breathing)
d. Bradycardia (slowing of heart rate)
e. lethargy
f. temperature instability
Diagnosis and Staging of NEC:
i. Early gastrointestinal findings may be non-specific:
a) Poor motility
b) Blood in stool
c) Vomiting
d) Diarrhea
e) Guarding
f) Distension
g) Feeding intolerance
ii. Later signs reflect progression of illness.
a) Abdominal tenderness
b) Abdominal wall erythema
c) Peritonitis
d) Ascites
e) Palpable mass
f) Hypotension
g) Bleeding disorders
h) Acidosis
Classification of NEC
Stage 1: suspect NEC - signs of sepsis, feeding intolerance ± bright red blood per rectum
Stage 2: Proven NEC- all of the above, pneumatosis, ± portal vein gas ± metabolic acidosis ± ascites
Stage 3: Advanced NEC- all of the above, clinical instability, definite ascites ± pneumoperitoneum
Modified Bells Classification of NEC
Figure 7:
How do you make the Diagnosis
Think of the diagnosis!
1. Serial physical examination.
2. Laboratory testing.
3. Abdominal x-rays.
Near-infrared spectroscopy measurement of abdominal tissue oxygenation is a useful indicator of intestinal blood flow and necrotizing enterocolitis in premature piglets
• A major objective of necrotizing enterocolitis (NEC) research is to devise a noninvasive method of early detection. We hypothesized that abdominal near-infrared spectroscopy (A-NIRS) readings will identify impending NEC in a large animal model.
• Concluded that abdominal near-infrared spectroscopy is capable of detecting alterations in intestinal oxygenation and perfusion in neonatal piglets and may allow early detection of neonates at risk for NEC [2].
Abdominal near-infrared spectroscopy measurements are lower in preterm infants at risk for necrotizing enterocolitis
• Near-infrared spectroscopy is a noninvasive method of measuring local tissue oxygenation (StO2).
• Abdominal StO2 measurements in preterm piglets are directly correlated with changes in intestinal blood flow and markedly reduced by necrotizing enterocolitis.
• The objectives of this study were to use near-infrared spectroscopy to establish normal values for abdominal StO2 in preterm infants and test whether these values are reduced in infants who develop necrotizing enterocolitis.
• This study establishes normal values for abdominal StO2 in preterm infants and demonstrates decreased values and increased variability in those with necrotizing enterocolitis. Abdominal nearinfrared spectroscopy monitoring of preterm infants may be a useful tool for early diagnosis and guiding treatment of necrotizing enterocolitis [3].
What is the Medical Treatment
• Stop feedings.
• Parenteral antibiotics
• Nasogastric decompression
• Parenteral nutrition
• Fluid resuscitation
Newly emerging therapeutic strategies
There are many evidence-based approaches to prevent NEC, these includes:
1. Withholding enteral feedings.
2. Using enteral antibiotics.
3. Feeding the infant with the mother’s expressed breast milk.
4. Administering probiotic agents, prebiotic agents, or both.
5. Administering various growth factors, anticytokine agents, and glucocorticoids.
Nutritional support to preserve the epithelial barrier
1. Human milk is able to protect against the development of NEC via induction of intestinal maturation and healing.
2. This is attributed to several factors that influence host immunity, inflammation, and mucosal protection, but a specific component to transfer in preterm formula has not been definitively identified, still no evidence between premature formula and NEC.
Feeding Practices and NEC
1. The evidence is convincing that human milk feeding, as compared to formula feeding, reduces the incidence of NEC in preterm infants.
2. Minimal enteral nutrition is a safe alternative to complete fasting before initiation of progressive feedings and does not increase the incidence of NEC in extremely preterm infants.
NEC Management Updates
• There is no evidence that trophic feeding has adverse effects for necrotizing enterocolitis [4].
Feeding Practices and NEC
1. In clinically stable VLBW infants, early introduction of progressive feeds and advancement of feeds at a faster rate (30– 35ml/kg/day) is safe and does not increase the incidence of NEC.
2. There is no evidence supporting continuous over intermittent tube feedings in preterm infants.
Slow Advancement of Enteral Feed Volumes to Prevent
Necrotising Enterocolitis in very Low Birth Weight Infants
1. Data suggest that advancing enteral feed volumes at daily increments of up to 30 to 40 mL/kg does not increase the risk of feed intolerance, necrotizing enterocolitis (NEC), or death in (VLBW) infants.
2. Increasing the volume of enteral feeds at slow rates (less than 24mL/kg/day) resulted in several days of delay in the time taken to regain birth weight and establish full enteral feeds, and increased the risk of late-onset invasive infection [5].
3. In a feed-intolerant preterm infant without any other clinical and radiological evidence of NEC, minimal enteral nutrition rather than complete suspension of enteral feeding may be alternative.
4. Human milk-based fortifier as compared to bovine-based fortifier may reduce the incidence of NEC but additional studies are required [6].
Nutritional support to preserve the epithelial barrier
1. The Cochrane review (2014) by Kuschel and Harding, presents the result of 13 randomized controlled trials that examined the long and short-term outcomes of preterm infants fed on a diet of fortified expressed breast milk.
2. They found that the use of a fortifier was associated with improved growth, with no significant increase in the adverse outcomes, including NEC.
Modification of gut microbiota composition
I. Probiotic colonization improves GI health and prevents proinflammatory signaling and disease progression by:
a) Increasing mucosal barrier function and by up-regulating the immune system.
b) Reduces mucosal colonization of potential pathogens.
c) Alters the key components of intestinal inflammation.
II. Several studies have demonstrated the efficacy and safety of prophylactic enteral probiotic administration in the prevention of NEC in infants with very low birth weight.
III. In these studies, the administered probiotics were Lactobacillus alone or in combination with Bifidobacterium.
IV. In a recent Cochrane Database Systematic Review and meta-analysis published, 16 randomized or quasi-randomized controlled trials that enrolled a total of 2,842 preterm infants at < 37 weeks gestational age and/or with a birth weight of < 2,500 kg were evaluated
Probiotics and Prebiotics
Probiotics: Nonpathogenic, live microorganisms that are capable of conferring a health benefit to the host -Bifidobacteria, Lactobacilli, Yeasts (S. boulardii)
Prebiotics: Non-digestible carbohydrates that selectively stimulate the growth or activity of certain bacteria in the gut that have the potential to benefit the human host – Galacto-oligosaccharides, Fructo-oligosaccharides (inulin, FOS in vegetables)
Modification of gut microbiota composition
a. They concluded that enteral supplementation of probiotics significantly reduced the incidence of severe NEC (stage II or more) and mortality in preterm infants weighing < 1,500 kg at birth. On the other hand, there are currently insufficient data with regard to the benefits and potential adverse effects in the most at risk infants, namely those weighing < 1,000 kg at birth.
b. Another proposed preventive strategy is to supplement with prebiotics, which enhance the growth of potentially beneficial intestinal microbes such as Bifidobacterium.
c. While the theoretical benefit has been reviewed, little information is currently available to support the benefit from their use in the prevention of NEC.
The Role of Immunonutrients in the Prevention of Necrotizing
Enterocolitis in Preterm very Low Birth Weight Infants
1. Enteral supplementation of probiotics is evident in NEC prevention, but clinical guidelines in terms of timing, strains, dose, length of therapy and contraindications are urgently needed for PVLBW.
2. Bovine Enterocolitis seems to be a promising diet in replacement of IF to stimulate the development of the immature intestine while waiting for the mother’s own milk during the first days of life.
3. LCPUFAs and HMOs might be directly supplemented to human milk or used to produce better preterm IF for those who have limited access to human milk.
4. The aforementioned amino acids and LCPUFA might also be added to parenteral nutrition preparations.
5. Clearly, more animal studies and clinical trials are required to further investigate the biological functions and to verify the safety and effectiveness of supplementation with immunonutrients in NEC prevention in PVLBW infants before recommendation of their routine use in the clinics [7].
Evidence-based Feeding Strategies guideline for necrotizing enterocolitis (NEC) among very low birth weight infants
1. It is recommended that infants be fed with mother’s own milk to decrease the risk of necrotizing enterocolitis (NEC). a. Note 1: The number of infants needed to treat with an exclusively human milk-based diet to prevent 1 case of NEC is 10 (number needed to treat [NNT] for NEC = 10). The number needed to prevent 1 case of surgical NEC or death is 8 (NNT for surgical NEC or death = 8).
2. It is recommended that donor milk be considered, if accessible, as an alternative to formula when mother’s own milk is unavailable.
3. It is recommended that enteral fasting* not be used as a strategy to decrease NEC risk.
a. Note: A meta-analysis of nine trials (n=754) did not detect a significant effect of early trophic feeding** versus enteral fasting on incidence of NEC: typical relative risk 1.07 (95% confidence interval [CI] 0.67, 1.70); typical risk difference 0.01 (95% CI -0.04, 0.05) [8].
*Enteral fasting is defined as delaying the introduction of enteral feeds until after five to seven postnatal days [8].
**Studies included in the meta-analysis used early trophic feeding of enteral milk volumes up to 24ml/kg/day (1mg/kg/hour) beginning within four days after birth and continuing until at least one week after birth [8].
4. It is recommended, when the infant is judged ready to tolerate feeding advancement, that feeding volume be advanced by 15 to 35ml/kg/day.
a. Note 1: No difference in NEC risk was observed in three trials (396 total infants) of feeding volume advancement as low as 15ml/ kg/day and as high as 35ml/kg/day.
b. Note 2: Slow advancement of feeding volume may lengthen the need for parenteral nutrition and its associated complications.
Prevention: protecting infants at greatest risk for NEC
1. Clinical stability (respiratory, cardiovascular, renal, and hematologic; use renal function as a guide)
2. Normal abdominal exams.
3. Absence of retrograde flow: (no bilious drainage or emesis; feeding intolerance)
4. Normal digestive function (absence of reducing substance, clinical tolerance of feeds)
5. No evidence of mucosal injury (absence of mucosal bleeding (occult/frank blood)
Predicting Disease Severity of Necrotizing Enterocolitis:
How to Identify Infants for Future Novel Therapies
1. Surgically treated NEC can be very devastating. Surviving infants require attentive healthcare and often need invasive catheters for parenteral nutrition. Our current ability to medically treat NEC is limited.
2. A scoring system to predict surgical NEC and mortality needs to be established in order to achieve this goal [9].
Firm Indications for Surgical Intervention
a. Perforated viscus
b. Abdominal mass
c. Fixed, dilated loop
d. Positive paracentesis
What is the outcome
a. Infants treated medically survival is > 95%
b. Infants requiring surgery survival is 70-75%
Conclusion
a. Prematurity is the single greatest risk factor for NEC & avoidance of premature birth is the best way to prevent NEC.
b. The role of feeding in the pathogenesis of NEC is uncertain, but it seems prudent to use breast milk (when available) and advance feedings slowly and cautiously.
c. NEC is one of the leading causes of mortality, and the most common reason for emergent GI surgery in newborns.
d. NEC remains a major unsolved medical challenge, for which no specific therapy exists, and its pathogenesis remains controversial.
e. A better understanding of the pathophysiology will offer new and innovative therapeutic approaches, and future studies should be focused on the roles of the epithelial barrier, innate immunity, and microbiota in this disorder.
f. Bioinformatics modeling is a new emerging strategy aimed at understanding the dynamics of various inflammatory markers and their application in early diagnosis and treatment.
References
- Stoll et al (1980) Age at diagnosis is inversely related to gestational age and degree of prematurity. J Ped 96: 447.
- Gay AN, Lazar DA, Stoll B, Naik-Mathuria B, Mushin OP, et al. (2011) Nearinfrared spectroscopy measurement of abdominal tissue oxygenation is a useful indicator of intestinal blood flow and necrotizing enterocolitis in premature piglets. J Pediatr Surg 46(6): 1034-1040.
- Patel AK, Lazar DA, Burrin DG, Smith EO, Magliaro TJ, et al (2014) Abdominal near-infrared spectroscopy measurements are lower in preterm infants at risk for necrotizing enterocolitis. Pediatr Crit Care Med 15(8): 735-741.
- Morgan J, Bombell S, McGuire W (2013) There is no evidence that trophic feeding has adverse effects for necrotizing enterocolitis. Cochrane Database of Systematic Reviews 3.
- Morgan J, Young L, McGuire W (2015) Slow advancement of enteral feed volumes to prevent Necrotising enterocolitis in very low birth weight infants. Cochrane Database Syst Rev (10): CD001241.
- Ramani, Ambalavanan (2013) Human milk-based fortifier as compared to bovine-based fortifier may reduce the incidence of NEC but additional studies are required. Clin Perinatol J 40(1): 1-10.
- Ping Zhou, Yanqi Li, Li-Ya Ma, Hung-Chih L, (2015) The Role of Immunonutrients in the Prevention of Necrotizing Enterocolitis in Preterm Very Low Birth Weight Infants. Nutrients 7(9): 7256-7270.
- Bombell, McGuire (2009) The enteral fasting not be used as a strategy to decrease NEC risk. Local Consensus
- Markel TA, Engelstad H, Poindexter BB (2014) Predicting Disease Severity of Necrotizing Enterocolitis: How to Identify Infants for Future Novel Therapies. J Clin Neonatol 3(1): 1-9.
© 2018 Amr Ismael M Hawal. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






