- Submissions

Full Text
Research & Investigations in Sports Medicine
Functional Reeducation and Taping is Early Treatment Protocol to Recovery of the Shoulder Rom in Athletes
Rosa Grazia Bellomo1, Claudia Barbato1*, Annamaria Porreca2, Roberto Buda3 and Raoul Saggini4
1Department of Biomolecular Sciences, Italy
2Department of Economics, Italy
3Department of Medicine and Aging Sciences, Italy
4Department of Medical, Italy
*Corresponding author:Claudia Barbato, Department of Biomolecular Sciences, Urbino, Italy
Submission: January 21, 2022;Published: October 20, 2022

ISSN: 2577-1914 Volume9 Issue2
Abstract
Objective: To compare the results obtained in the reduction of pain symptoms, and in the recovery of the right shoulder joint range in athletes presenting acute pain and functional limitation on the right shoulder, through two different approaches: planned physical activity and planned physical activity with application of taping rubber band.
Design: Case-control study.
Setting: University of Urbino (Italy).
Subjects: Thirty athletes subjects suffering from acute painful symptoms of the right shoulder with reduction of the joint ROM.
Interventions: 30 people divided into two randomized groups: Group A consisting of 15 people undergoing scheduled physical activity and weekly application of elastic taping (36 sessions of scheduled physical activity and 12 of tape applications) and group b of 15 people undergoing only scheduled physical activity (36 sessions of scheduled physical activity).
Main measures: Vas scale, R.O.M. Protractor evaluation, Functional tests
Results & Conclusion: All patients achieved positive results with pain reduction and shoulder rom but the patients treated with elastic taping and planned physical activity achieved a more significant recovery of joint Rom (extra rotation and abduction) and a greater reduction of pain measured with the vas scale.
Keywords: Kinesio-taping; Shoulder; Shoulder re-education
Introduction
When in physiological conditions, the shoulder joint allows us to relate and manage the external environment in the act of prehension, grasping, lifting an object in the most planes of space. But in case of painful shoulder we begin to avoid carrying out all those acts that activate pain and gradually, this anatomical area becomes more and more rigid [1]. Shoulder pain-which by diffusion in the population is second only to back pain-is really annoying and limiting, and when it becomes chronic, it is among the most frequent causes of abstention from jobs [2,3]. The first symptom of the painful shoulder is pain in the upper and lateral part of the arm and in the front area of the right and left shoulder [1,4]. Pain that occurs in conjunction with specific movements compatible with myofascial syndrome and which triggers the onset of movement deficit and strength deficit [1,5]. The clinical journal of pain [5]. If not treated promptly, it can modify the complex biomechanics of the shoulder causing chronic pain, therefore, it is desirable to identify the origin of the pain and to make an early and personalized diagnosis and therapeutic path, recognizing an effective therapeutic strategy in the shortest possible economic and decisive time [6]. In the literature, within most of the proposed therapeutic projects, physical activity/therapeutic exercise or better said programmed motor activity is constant [7]. The dynamic balance of the muscles surrounding the shoulder and the elasticity of the joint components are essential elements to ensure harmony and fluidity of movement and to minimize harmful forces [7,8].
The sequential objectives of shoulder rehabilitation are:
A. Restore complete active and passive articulation.
B. Restore the synchrony of the movement.
C. Quickly reduce painful symptoms.
Fundamental premise highlighted in every scientific work for the rehabilitation of the shoulder, and the achievement of a normal glenohumeral and bachelor-thoracic rhythm in order to guarantee the correct biomechanics of the joint [9]. Planned physical activity represents the first step for shoulder recovery. The motor activity programmed by us was identified with a sequence of eight exercises identified as those reported in the largest number of scientific articles and to which a good result is attributed on acute pain and rapid recovery of the joint range and therefore inserted as movement therapy, in good clinical practices for acute shoulder pain [9,10]. The use of taping in combination with a correct programmed activity plan is believed to be rationally correct both for the fast application method and for the low cost and above all for the rapid recovery [11]. In particular, the KINESIO taping is a tool used to facilitate the natural healing process of the tissues, providing support and stability to the osteo-myo-fascial system, without limiting the range of movement, favoring the rapid return to the field for the sportsman or daily activities for the population. The Kinesio Taping method, and its application “tool”, the kinesio tex tape were born, in 1973, from an intuition of Dr. Kenzo Kase. In his clinical experience, he found that the main physical and psychological suffering complained of by his patients was pain. He therefore had the idea of finding a “solution” that could maintain the results acquired with the treatment between one session and another [12,13].
Taping has as main objective to act on pain reduction. Inducing exchange of information between afferent (towards the spinal cord) and efferent (from the spinal cord) communication systems, by means of skin modulations associated with body movement” as defined by the Kenzo KASE school in harmony with the global vision of the organism of applied kinesiology and with the stimulus principle that helps the organism to put into action the natural mechanisms of self-healing, with respect for a three-dimensional vision of the organism, through relationships between muscle tone, posture and state of health [13,14]. He therefore hypothesized that the reported pain of his patients could be reduced through a modification of the tension of the skin, obtained by affixing a patch at the end of the proposed treatment [15]. Dr. Kase imagined that, by lifting the skin, the normal circulation of interstitial fluids through the superficial lymphatic vessels would be restored (homeostasis). The subsequent decrease in fluid pressure would have led to an improvement in muscle function by decreasing edema and pain. Since the branch of medical science that deals with muscle function and movement was kinesiology, he had the idea of using the term “Kinesio Tape” [13,14]. In this context, the application of the tape represents the final act of the re-education session, it can therefore be easily added or supported alongside all other commonly used therapeutic techniques [16].
Methods and Materials
The volleyball athletes examined are 30 divided into two groups through randomization 15 for group A to which programmed exercise and tape was proposed and 15 subjects for group B who carried out only scheduled exercise. The inclusion criteria have been defined: acute right shoulder pain for more than a month and less than three months corresponding to a reported vas over 6 and reduction of the limiting joint range in daily life activities; male individuals aged between 30 and 40 years; moderate physical activity according to the definition oms; no full-blown pathologies no diabetes no hypertension no hypercholesterolemia in good general health conditions; no habitual use of drugs. The exclusion criteria have been defined: patients with bilateral shoulder pain or with pain exclusively on the left shoulder or presence of positivity at least one of the evaluation tests carried out, and/or not meeting the inclusion criteria thirty (n=30) subjects with time to, i.e., at the beginning of the activity and time T1 after 12 weeks or 36 sessions carried out three per week were evaluated. All 30 subjects were evaluated through tests: Neer test, Jobe test, Hawkins test, Gerber test, Yokum test, Patte test, Lift - off test, Napoleon test and Load and Shift test. The joint ROM of the shoulder was measured using the protractor pain was assessed using the vas subjective rating scale.
Weight versus disease risk was assessed using the BMI formula solution
The physical exercise scheduled for both groups was performed, for 36 sessions each session lasted ninety minutes and realized twice for week. The sessions were held in relationship. 1/1 patient/ operator. Each week, after re-evaluating the subject, the exercises were increased by the number of sets and repetitions in relation to the improvement of the vas and joint range. The programmed motor activity includes streatching exercises, joint exercises and muscle strengthening exercises, in relation to the peak percentage of force developed by the individual muscles as detected by Towsend et al. (AISM 1991) and which allows the execution of the exercise in a precise muscular commitment guaranteeing selective work. The programmed physical activity sequence consisted of: streatching of the lower capsule, streatching of the posterior capsule, streatching of the anterior and lower shoulder structures in passive and active aimed at reducing painful retractions and decreasing intra-articular pressure and eight specific exercises like: (Treatment of Lesions of The Rotator Cuff, [17])
A. Flexion:Subject in sitting position, and/or standing, performs upper limb flexion with and without progressive weight, resulting in a percentage muscle engagement of the anterior deltoid, medium deltoid, supraspinatus, subscapular and supraspinatus muscles [18]. Examination of the shoulder. The complete guide. New York [1,19].
B. Abduction on the scapular plane in rotation:The patient sitting or standing with a progressive possible increase in weight with a percentage muscular effort of the anterior deltoid, medium deltoid, supraspinoso, subscapular muscles [20].
C. Abduction:Abduction of the scapular plane in external rotation. The patient sitting or standing with a possible progressive increase in weight with a percentage muscular effort of the anterior deltoid, medium deltoid, supraspinosus and sub-spinous muscles [21].
D. Traction:Subject in prone position, cervico-brachial complex facing the limb that performs the movement, elbow engaged at 90° with progressive weight stress, percentage muscle commitment of the middle deltoid and posterior deltoid muscles [16,22].
E. Horizontal abduction from prono in internal rotation: Subject in prone position with cervico-brachial engaged in the movement direction, muscular percentage commitment of the muscles medium deltoid, posterior deltoid, sub-spinous, small round.
F. Horizontal abduction from prono in exernal rotation:Subject in prone position with cervico-brachial engaged in the direction of movement, muscular percentage commitment of the muscles medium deltoid, posterior deltoid, subspinous, small round [23].
G. External rotation:subject lengthened in lateral decubitus, analysis of the muscular engagement of the posterior deltoid, subspinous and small round muscles.
H. Pendulum starting position:Relaxation and decatting exercise for the shoulder can be performed in 3 positions, sitting, standing or in a prone position.
I. Execution:With the arm completely relaxed, small and slow movements of swinging or circling must be made, with a maximum weight of 2kg in the hand or fixed to the wrist.
J. Muscle percentage engagement of the muscles:Anterior, middle and posterior deltoid, supraspinous, subspinous, small round, large pectoralis major and latissimus dorsi [22]. The application of the tape always carried out by the same operator (specialized in kinesiology taping therapy) took place once a week, on Monday, using the Y application in decompression. positioned on the deltoid muscle to increase external rotation, and abduction, movements that are usually difficult to achieve in its entirety.
The number of 18 applications aimed at
A. Reduce pain
B. Improve posture
C. Improve the shoulder joint function
No patient had adverse events such as and allergies, no one complained of difficulties due to the tape. Excellent compliance of the tape.
Statistical analysesR statistical environment version 3.6 was used for all data analysis. Descriptive statistics: Mean±SD was calculated to characterize the study variables. Unpaired t-test was used to investigate whether there were differences between the exercise plus taping group and exercise group compute using the differences in the patient’s conditions between the baseline and after the treatments. Normality distribution of variables was tested by Jarque-Bera test.
Results
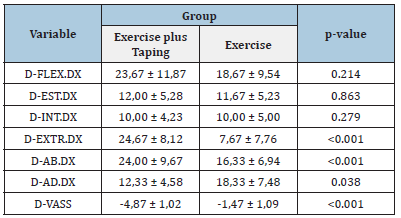
Table 1 shows the descriptive statistics for the all variables in the study and the p-value from unpaired t-test to assess the not differences at baseline between groups. We can state that there are not differences at the baseline for all variables in the study and for the main anthropometric patients’ characteristics (Table 2).
Table 1: Descriptive statistics: Mean ± SD of all variables in the study, and p-value from unpaired t-test to assess no difference at baseline between groups.

Legends: T0= baseline; T1=after treatment; VAS=visual analogic scale.
Table 2: Mean ± SD for difference in variables between baseline and post treatment patient’s conditions. P-value from unpaired t-test.
Discussion
Patients in both groups showed a significant reduction in pain and an increase in the joint range of the right shoulder. Planned physical activity, as already documented in the literature, is an integral part of shoulder rehabilitation. It is important to set the planned physical activity path only after a correct evaluation of the somatic osteo-fascial complex in dysfunction and the execution of the tests and evaluations proposed can be understood as a simple and immediate approach for a correct identification of the myofascial syndrome. The proposed planned physical activity was identified in a repeated and repeatable series of exercises allowing to document an accredited protocol (long-term results of rehabilitative management with extracorporeal shockwave therapy in rotator cuff disease with partial tears [24].
The tape is a practical aid, easy to apply, non-invasive, with excellent compliance, and economic, which has made it possible to amplify the result obtained from scheduled physical activity and a reduction in pain. The group that performed exercises and kinesio taping has improved especially in the movements of external rotation and abduction due to an increase in the joint range and a reduction in painful symptoms. The appropriateness of the tape instrument is evident from the results obtained in the external rotation and abduction as the tape has been positioned specifically on the deltoid. The overall improvement could be the result of normalization of muscle function and not simply an analgesic effect. The effect of taping on muscle activity has been studied by several authors [23,24], who have shown that in healthy subjects performing an isometric contraction of the quadriceps muscle, kinesio taping modifies the bioelectric activity of the vastus medialis. with an increase in the recruitment of motor units [25]. Found a significant increase in the speed of activation of the vastus medialis in patients with femoropatellar syndrome compared to control subjects and placebo after the application of kinesio taping) [26] and showed an improvement in epicondyllic muscles that slip during wrist movements in two patients with hepato-condylalgia after applying the kinesio taping technique [27].
Conclusion
Once the number of athletes suffering from shoulder pain and functional impotence has been assessed, it is essential to identify an effective and sport-treatment protocol. Having assessed the progressive evolution of acute shoulder pain into highly validating chronic pain until it is documented among the most numerous causes of leaving the workplace, it is essential to identify an early treatment protocol. The data on pain, joint shoulder movement and function obtained from this study could contribute to clarifying the planned physical activity and the complementarity of the tape in the treatment of painful shoulder. However, further research is needed, both clinical and neurophysiological, to clarify the mechanisms and effects of the kinesio taping technique [28-32].
References
- Buckup K (2008) Clinical test for the musculoskeletal system. Examination-sings-phenomena. 2nd (Edn.), Thieme Publishers, USA, p. 1-70.
- Alexander CM, Stynes S, Thomas A, Lewis J, Harrison PJ (2003) Does tape facilitate or inhibit the lower fibres of trapezius? Manual Therapy 8(1): 37-41.
- Alexander CM, McMullan M, Harrison PJ (2008) What is the effect of taping along or across a muscle on motoneurone excitability? A study using triceps surae. Man Ther 13(1): 57-62.
- Chen W, Hong W, Huang T, Hsu H (2007) Effects of kinesio taping on the timing and ratio of vastus medialis obliquus and vastus lateralis muscle for person with patellofemoral pain. Journal of Biomechanics 40(S2): 318.
- De Andres J, Cerda-Olmedo G, Valia JC, Monsalve V, Lopez Alarcon, et al. (2003) Use of botulinum toxin in the treatment of chronic myofascial pain. Clin J Pain 19(4): 269-275.
- Cools AM, Witvrow EE, Danneels LA, Cambier DC (2002) Does taping influence electro-myographic muscle activity in the scapular rotators in healthy shoulders? Manual Therapy 7(3): 154-162.
- Ebbers J, Pijnappel H (2006) The involved of curetape on the sit-and-reach test. Sportmassage International 8: 232-238.
- Drummond S, Fox K (2004) Feasibility of kinesiotape application for treatment of dysarthria. ASHA Convention, USA, pp. 18-20.
- Edwards J, Knowles N (2003) Superficial dry needling and active stretching in the treatment of myofascial pain. A randomised controlled trial. Acupunct Med 21(3): 80-86.
- Fischer AA (1997) Algometry in the daily practice of pain management. J Back Musculoskelet Rehabil 8(2): 151-163.
- Fischer AA (1988) Documentation of myofascial trigger points. Arch Phys Med Rehabil 69(4): 286-291.
- Fu TC, Wong AM, Pei YC, Wu KP, Chou SW, et al. (2008) Effect of kinesio taping on muscle strength in athletes-A pilot study. Journal of Science and Medicine in Sport 1(2): 198-201.
- Kase K, Tatsuyuki H, Tomoko O (1996) Development of kinesio tape. Kinesio taping perfect manual. Kinesio Taping Association 6(10): 117-118.
- Hanten WP, Olson SL, Butts NL, Nowicki AL (2000) Effectiveness of a home program of ischemic pressure followed by sustained stretch for treatment of myofascial trigger points. Physical Therapy 80(10): 997-1003.
- Gam AN, Warming S, Larsen LH, Jensen B, Høydalsmo O, et al. (1998) Treatment of myofascial trigger-points with ultrasound combined with massage and exercise -- A randomised controlled trial. Pain 77(1): 73-79.
- Hong CZ, Simons DG (1998) Pathophysiologic and electrophysiologic mechanisms of myofascial trigger points. Arch Phys Med Rehabil 79(7): 863-871.
- Saggini R, Cavezza T, Pancrazio L, Pisciella V, Saladino G, et al. (2010) Treatment of lesions of the rotator cuff. Journal of Biological Regulators & Homeostatic Agents 24(4): 453-459.
- McFarland EG (2006) Examination of the shoulder: The complete guide. 1st (), Thieme Publishers, USA, pp. 1-304.
- Maitland G, Hengeveld E, Banks K, English KM (2007) Spinal manipulation. 7th (Edn.), Elsevier Publishers, USA, 1-241.
- Simons DG, Travell JG, Simons LS (2002) Myofascial pain and dysfunction. The manual of hammer points. Upper half of the body. 2nd (Edn.), Editorial Medica Panamericana, Spain.
- Simons DG (1996) Clinical and etiological update of myofascial pain from trigger points. Journal of Musculoskeletal Pain 4(1-2): 93-121.
- Travell JG, Simons DG (1999) Myofascial pain and dysfunction, the trigger point manual. Williams and Wilkins Publishers, USA.
- Slupik A, Dwornik M, Biaoszewski D, Zych E (2007) Effect of kinesio taping on bioelectrical activity of vastus medialis muscle. Preliminary report. Ortop Traumatol Rehabil 9(6): 644-651.
- Saggini R, Coco V, Pancrazio L, Megna M, Iodice P, et al. (2012) Long-term results of rehabilitative management with extracorporeal shockwave therapy in rotator cuff disease with partial tears. European Journal of Inflammation 10(3): 487-494.
- Yasukawa A, Patel P, Sisung C (2006) Pilot study: investigating the effects of kinesio taping in an acute paediatric rehabilitation setting. American Journal of Occupational Therapy 60(1): 104-110.
- Yoshida A, Kahanov L (2007) The effect of kinesio taping on lower trunk range of motions. Res Sports Med 15(2): 103-112.
- Zajt KJ, Rajkowska LE, Skrobot W, Bakula S, Szamotulska J (2007) Application of kinesio taping for treatment of sport injuries. Research Year- book 13(1): 130-134.
- Jaraczewska E, Long C (2006) Kinesio taping in stroke: Improving functional use of the upper extremity in hemiplegia. Topics in Stroke Rehabilitation 13(3): 31-42.
- Kamanli A, Kaya A, Ardicoglu O, Ozgocmen S, Zengin FO, et al. (2005) Comparison of lidocaine injection, botulinum toxin injection, and dry needling to trigger points in myofascial pain syndrome. Rheumatol Int 25(8): 604-611.
- Liu YH, Chen SM, Lin CY, Huang CI, Sun YN (2007) Motion tracking on elbow tissue from ultrasonic image sequence for patients with lateral epicondylitis. Conf Proc IEEE Eng Med Biol Soc 2007: 95-98.
- Niddam DM, Chan RC, Lee SH, Yeh TC, Hsieh JC (2007) Central modulation of pain evoked from myofascial trigger point. Randomized Controlled Trial 23(5): 440-448.
- Simoneau G, Degner R, Kramper C, Kittleson K (1997) Changes in ankle joint proprioception resulting from strips of athletic tape applied over the skin. Journal of Athletic Training 32(2): 141-147.
© 2022 Claudia Barbato. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






