- Submissions

Full Text
Research & Investigations in Sports Medicine
Dry Needling of the Medial Gastrocnemius as Novel Treatment for Type-VI Functional Popliteal Artery Entrapment Syndrome
Yao-Wen Eliot Hu1* and Edmund Joseph Siebel2
1Department of Physical Medicine, Uniformed Services University of Health Sciences, USA
2Department of Family and Community Medicine, Uniformed Services University of Health Sciences, USA
*Corresponding author: Yao-Wen Eliot Hu, Primary Care Sports Medicine Fellowship, Naval Hospital Camp Pendleton, Department of Family and Community Medicine, Uniformed Services University of Health Sciences, USA
Submission: December 01, 2021;Published: December 15, 2021

ISSN: 2577-1914 Volume8 Issue1
Abstract
Popliteal artery entrapment syndrome is rare, commonly overlooked, and characterized by the compression of the popliteal artery via the surrounding myofascial structures. Presented is a 28-year-old active-duty male service member with unilateral exertional left lower extremity pain, paresthesia, and discoloration. Popliteal musculoskeletal and Doppler ultrasound showed normal anatomy with functional compression of the popliteal artery by the medial head of the gastrocnemius. This is the first case in current literature to report ultrasound-guided dry needling to the medial head of the gastrocnemius as novel treatment for functional popliteal artery entrapment syndrome.
Keywords: Popliteal artery entrapment syndrome; Dry needling; Non-operative treatment; Ultrasound diagnosis; Case report
Abbreviations: PAES: Popliteal Artery Entrapment Syndrome; CECS: Chronic Exertional Compartment Syndrome; ABI: Ankle-Brachial Index; MRA: Magnetic Resonance Angiography; IVUS: Intravascular Ultrasound; EMG: Electromyography; CT: Computed Tomography; MRI: Magnetic Resonance Imaging
Introduction
Popliteal Artery Entrapment Syndrome (PAES), first described in 1879, is a rare, commonly overlooked, and potentially misdiagnosed condition preferentially seen in young males [1,2]. PAES may also present Concurrently with Chronic Exertional Compartment Syndrome (CECS), thereby necessitating thorough clinical evaluation supplemented with additional diagnostic studies for accurate confirmation leading to appropriate treatment [2,3,4]. Clinical presentation typically consists of exertional leg pain with or without lower extremity paresthesia and skin discoloration [2]. Physical examination is often normal but may reveal tenderness to palpation over the medial head of the gastrocnemius, signs of decreased perfusion including changes in skin color or temperature, a popliteal bruit that increases with ankle plantarflexion, or a diminished popliteal pulse with ankle dorsiflexion and plantarflexion [1,2,5,6].
With six distinct types of PAES, appropriate classification is essential for effective treatment [7] (Table 1). Initial lower extremity diagnostic studies performed with and without provocative maneuvers assist in diagnosis confirmation and include Ankle-Brachial Index (ABI), duplex ultrasound, and Doppler ultrasound [1,2]. Studies show that duplex ultrasound specifically correlates well with intra-operative findings [8]. There have also been reports of increased diagnostic value with the combination of dynamic Doppler ultrasound and dynamic Magnetic Resonance Angiography (MRA) [9]. Further advanced imaging, such as Computed Tomography Angiography (CTA), MRA, or conventional angiography, also helps in differentiating between the various types of PAES when performed with and without provocative maneuvers [1,2,5]. Recently, Intravascular Ultrasound (IVUS) has been introduced as an additional method for diagnosis and for optimizing surgical planning [2,10].
Table 1: Classification for popliteal artery entrapment syndrome [3,5,8].

Treatment of PAES depends on the classification and its compression site [2]. Historically, surgery has been the recommended treatment with good, reported outcomes [1]. Given its association with CECS, PAES surgical treatment may include four-compartment fasciotomy [1,2,3]. Depending on the anatomical abnormality, surgical intervention may also consist of resection of the anomalous fibrous fascial bands; resection, myomectomy, release, decompression, or division of the medial head of the gastrocnemius or the popliteus muscle; and arterial bypass or thromboendarterectomy with venous patch arterioplasty [2,5]. With regards to non-operative treatment, there have been limited reports of successful functional PAES treatment with intramuscular botulism toxin injections to the medial head of the gastrocnemius but more research is needed [11-14]. To date, no other nonoperative treatments for PAES have been reported in the current literature.
Case
Presented is a 28-year-old active duty male service member with exertional left foot and ankle pain during running and hiking. His duties as a dog handler required him to carry an exceptionally heavy pack and sometimes his canine over rough terrain. He denied specific mechanisms of injury but noted relatively rapid onset of intolerance to activity. Symptoms began to recur with less weight and shorter distances until he was unable to run one mile without significant discomfort. He also described a steady increase in symptom intensity with prolonged activity and associated generalized numbness in his foot. There were no mitigating activities except for the avoidance of running and hiking, both of which were required for his military specialty. Initial studies completed by his medical team included unremarkable radiographs of the left foot, MRI of the left ankle, and limited left lower extremity Electromyography (EMG). He had also failed a protracted course of left foot and ankle rehabilitation with physical therapy.
Physical examination of the left ankle and foot was normal at rest, but his walking gait was noted to have left greater than right overpronation and heavy heel-strike bilaterally. His lower extremity skin and neurovascular examinations were unremarkable at rest. Since his symptoms were provoked with exertion, further examination was performed after a one-mile treadmill run, which revealed pronounced flushing and discoloration in the left dorsal forefoot and medial hindfoot along with diminished sensation to light touch throughout all of his left toes, suggestive of venous congestion and stasis (Figure 1). Given the time-sensitive nature of his upcoming deployment and concerns for prior radiation exposure, lower extremity ABI, CTA, MRA, and conventional angiography were not obtained. Instead, musculoskeletal and Doppler ultrasonography was performed to evaluate for PAES, revealing normal anatomy of the vasculature and surrounding structures. But, ultrasound did show mild functional hypertrophy of the medial head of the gastrocnemius with pronounced decrease in popliteal artery blood flow aggravated by passive ankle dorsiflexion post-run compared to his pre-run baseline (Figure 2).
Figure 1: (A)Skin before 1 mile run, (B)Skin after 1 mile run.
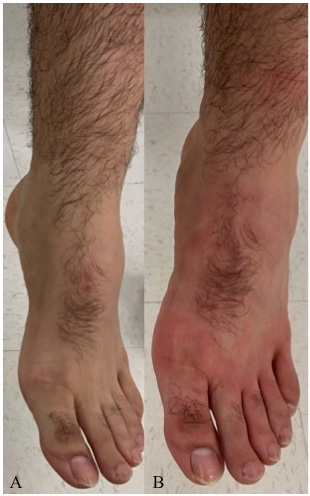
Figure 2: Dynamic Power Doppler ultrasound showing (A)Normal flow of left Popliteal Artery (PA) at ankle neutral post-1-mile run and symptomatic, (B)Normal flow of right Popliteal Artery at ankle neutral post-1-mile run and asymptomatic, (C)Decreased flow of left Popliteal Artery with ankle dorsiflexion post-1-mile run and symptomatic, (D) Normal flow of right Popliteal Artery with ankle dorsiflexion post-1-mile run and asymptomatic; PV: Popliteal Vein; MG: Medial head of the Gastrocnemius muscle.
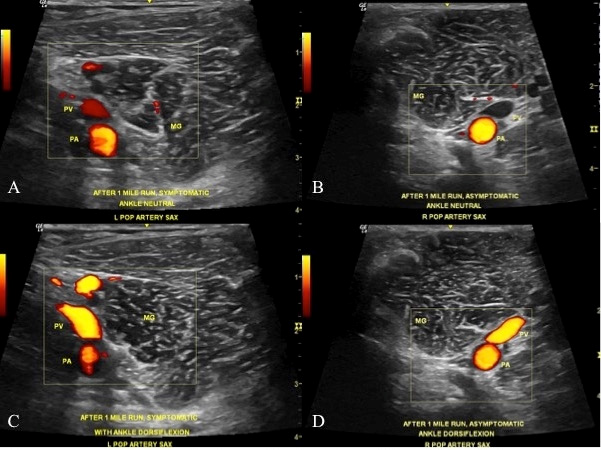
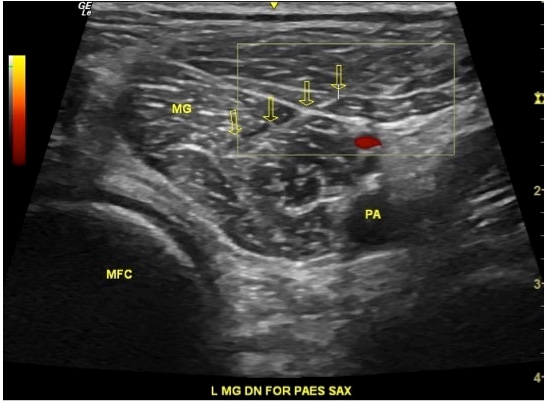
Figure 3: Ultrasound-guided dry needling of the Medial head of the Gastrocnemius (MG); arrows: acupuncture needle; PA: Popliteal Artery; MFC: Medial Femoral Condyle
After discussion of potential treatment options including consultation with vascular and orthopedic surgery, the patient declined surgical consultation due to the urgent nature of his upcoming deployment. Moreover, botulism toxin was not available for use at our clinic and the patient declined referral to another facility due to possible delays in treatment. Instead, treatment consisted of regular focused stretching of the medial and lateral gastrocnemius muscles supplemented with two sessions of ultrasound-guided dry needling of the medial head of the gastrocnemius muscle spread three weeks apart (Figure 3). Six weeks after treatment initiation, the patient was able to progress gradually from rest to 30 minutes of running while also completing a full lower body strength training session without significant exacerbation of symptoms. Ten weeks after treatment, he was able to run three miles without difficulty. He returned to full duty and deployed without issues approximately twelve weeks after initial presentation.
Discussion
Type-VI PAES, first described in 1985, is characterized by the compression of the popliteal artery via a functionally hypertrophied medial head of the gastrocnemius with normal anatomy [1,7]. It is commonly seen in young athletes who present with vague lower extremity claudication with or without paresthesia or signs of vascular compromise [1]. As with other types of PAES, dynamic diagnostic imaging studies are needed to ensure accurate diagnosis and to direct effective treatment. Initial diagnostic workup may include dynamic lower extremity ABI but it has been reported that although ABI continues to be underutilized and objectively shows arterial compromise, it is operator-dependent and often incorrectly performed [15]. Furthermore, there are reports that while the ABI decreases in PAES, it is difficult to grade the degree of compression and to identify the actual sites of compression for various types of PAES, rendering ABIs to be unreliable [12,16,17]. Given the urgent need for timely diagnosis and treatment due to our patient’s upcoming deployment, dynamic lower extremity ABI was not performed in this case after taking its clinical unreliability into consideration.
Advanced imaging and diagnostic studies for PAES include dynamic duplex ultrasound, Doppler ultrasound, CTA, MRA, and conventional angiography with provocative maneuvers in order to accurately identify the anatomical anomaly and to identify the sites of compression [1,2,3]. While CTA, MRA, and angiography remain the gold standard for diagnosis confirmation, recent literature supports the use of dynamic duplex or Doppler ultrasound, sometimes in combination with MRA, for confirmation and classification of PAES [8,9]. Furthermore, there are reports of increased diagnostic value and assistance in surgical planning with use of IVUS [10]. With regards to this case, there was considerable past exposure to radiation given the patient’s previous injuries requiring multiple Computed Tomography (CT) and Magnetic Resonance Imaging (MRI) scans. The prior radiation exposure, lack of on-site diagnostic imaging resources possibly delaying diagnosis, and emphasis on shared decision-making all contributed to the decision to use musculoskeletal and Doppler ultrasound instead of CTA, MRA, and conventional angiography for diagnosis confirmation.
Treatment for functional PAES is typically surgical via a posterior approach exposing the popliteal artery and performing adhesiolysis, side branch ligation, and partial excision of the medial head of the gastrocnemius muscle, with or without fasciotomy depending on whether there is concurrent CECS [11,18]. There have also been multiple case reports of adequate outcomes with intramuscular botulism toxin injection into the medial head of the gastrocnemius as treatment for functional PAES [11,14]. However, there are no reports of other non-operative treatment modalities for functional PAES in the literature to date. For this case, intramuscular botulism toxin injection and surgical consultation were discussed with the patient. Given the limited on-site resources possibly delaying treatment and his upcoming deployment, the patient ultimately declined referrals for botulism toxin injection and surgical consultation. After discussion of its lack of evidence, ultrasound-guided dry needling of the medial head of the gastrocnemius was performed in combination with focused stretching and rehabilitation.
Proper diagnosis and classification of PAES is critical to facilitating appropriate treatment. Ultrasound is an operatordependent yet readily available modality that can aid with diagnosis and treatment in the appropriate clinical context. This is the first case report describing ultrasound-guided dry needling as ancillary treatment for type-VI PAES. This case highlights the utility of musculoskeletal and Doppler ultrasound in diagnosing PAES and introduces ultrasound-guided dry needling of the medial head of the gastrocnemius as a non-operative, minimally invasive treatment in functional PAES.
Acknowledgements and Funding
The views expressed in this publication are those of the authors and do not reflect the official policy or position of the Department of the Navy, the Department of Defense, or the U.S. Government. The authors declare no conflicts of interest and do not have any financial disclosures.
I am a military service member of the United States Government. This work was prepared as part of my official duties. Title 17 U.S.C. 105 provides that copyright protection under this title is not available for any work of the United States Government. Title 17 U.S.C. 101 defines a U.S. Government work as work prepared by a military service member or employee of the U.S. Government as part of that person’s official duties.
Conflict of Interest Statement
Yao-Wen Eliot Hu: AMSSM – Received honorarium as scanning faculty at the Fundamentals of Ultrasound Pre-conference at the AMSSM Annual Meeting. Edmund Siebel: none
References
- Pandya YK, Lowenkamp MN, Chapman SC (2019) Functional popliteal artery entrapment syndrome: A review of diagnostic and management approaches. Vasc Med 24(5): 455-460.
- Joy SM, Raudales R (2015) Popliteal artery entrapment syndrome. Curr Sports Med Rep 14(5): 364-367.
- Turnipseed WD (2012) Popliteal entrapment in runners. Clin Sports Med 31(2): 321-328.
- Gokkus K, Sagtas E, Bakalim T, Taskaya E, Aydin AT (2014) Popliteal entrapment syndrome: A systematic review of the literature and case presentation. Muscles Ligaments Tendons J 4(2): 141-148.
- Carneiro Junior FCF, Carrijo ENDA, Araujo ST, Nakano LCU, de Amorim JE, et al. (2018) Popliteal artery entrapment syndrome: A case report and review of the literature. Am J Case Rep 19: 29-34.
- Politano AD, Bhamidipati CM, Tracci MC, Upchurch GR Jr, Cherry KJ (2012) Anatomic popliteal entrapment syndrome is often a difficult diagnosis. Vasc Endovascular Surg 46(7): 542-545.
- di Marzo L, Cavallaro A (2005) Popliteal vascular entrapment. World J Surg 29 Suppl 1: S43-5.
- Altintas U, Helgstrand UV, Hansen MA, Stentzer KF, Schroeder TV, et al. (2013) Popliteal artery entrapment syndrome: ultrasound imaging, intraoperative findings, and clinical outcome. Vasc Endovascular Surg 47(7):513-518.
- Williams C, Kennedy D, Bastian-Jordan M, Hislop M, Cramp B, et al. (2015) A new diagnostic approach to popliteal artery entrapment syndrome. J Med Radiat Sci 62(3): 226-229.
- Boniakowski AE, Davis F, Campbell D, Khaja M, Gallagher KA (2017) Intravascular ultrasound as a novel tool for the diagnosis and targeted treatment of functional popliteal artery entrapment syndrome. J Vasc Surg Cases Innov Tech 3(2): 74-78.
- Shahi N, Arosemena M, Kwon J, Abai B, Salvatore D, et al. (2019) Functional popliteal artery entrapment syndrome: A review of diagnosis and management. Ann Vasc Surg 59: 259-267.
- Hislop M, Brideaux A, Dhupelia S (2017) Functional popliteal artery entrapment syndrome: use of ultrasound guided Botox injection as a non-surgical treatment option. Skeletal Radiol 46(9): 1241-1248.
- Wadhwani A, Nutley M, Bakshi D, Mirakhur A (2018) Treatment of functional popliteal artery entrapment syndrome with ultrasound-guided botox injection. J Vasc Interv Radiol 29(12): 1780-1782.
- McGinley JC (2015) Nonsurgical treatment of cystic adventitial disease of the popliteal artery caused by functional popliteal artery entrapment syndrome. J Vasc Surg Cases 1(1): 28-31.
- Davies JH, Kenkre J, Williams EM (2014) Current utility of the Ankle-Brachial Index (ABI) in general practice: implications for its use in cardiovascular disease screening. BMC Fam. Pract 15: 69.
- Sirico F, Palermi S, Gambardella F, Capuano E, Ferrari U, et al. (2019) Ankle brachial index in different types of popliteal artery entrapment syndrome: A systematic review of case reports. J Clin Med 8(12): 2071.
- Pillai J, Levien LJ, Haagensen M, Candy G, Cluver MDV, et al (2008) Assessment of the medial head of the gastrocnemius muscle in functional compression of the popliteal artery. J. Vasc. Surg 48(5): 1189-1196.
- Lavingia KS, Dua A, Rothenberg KA, Fredericson M, Lee JT (2019) Surgical management of functional popliteal entrapment syndrome in athletes. J Vasc Surg 70(5): 1555-1562.
© 2021 Yao-Wen Eliot Hu. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






