- Submissions

Full Text
Research & Investigations in Sports Medicine
Achilles tendon Injuries: Tendinopathy and Rupture-A Mini Review
Tabinda Hasan1*, Kavita Ganesh1, Zenat Ahmed Khired1 and Khadijah Khader2
1 College of Medicine, Princess Nourah University, KSA
2 College of Pharmacy, Al Maarefa Colleges, KSA
*Corresponding author: Tabinda Hasan, College of medicine, Princess Nourah University, Riyadh, KSA
Submission: March 07, 2018; Published: March 26, 2018

ISSN: 2577-1914 Volume2 Issue3
Introduction
Achilles tendon, the largest and strongest tendon in the human body is formed by fusion of the tendinous portion of calf muscles; the gastrocnemius and soleus [1,2]. Achilles tendon can largely with stand tensional forces of locomotion. The incidence of Achilles tendon injuries has increased considerably during the pastdecade [1-5]. Such injuries account for 45% of all sports related injuries among athletes and general public. Achilles tendon complaints generally represent most tendon problems in any population and can be divided into “Spontaneous ruptures” (excessive loadinginduced injury/degeneration of tendon without any predisposing systemic diseases); and “Overuse injuries” (traced to sports and exercise-related overuse). Sometimes, a systemic disease, such as rheumatoid arthritis may manifest with Achilles tendon symptoms, but this represents only a minority (~2%) of all cases [1,6].
Epidemiology of Achilles Tendinopathy
The clinical syndrome characterized by combination of pain, diffuse/ localized swelling in and around the Achilles tendon and impaired locomotive performance is called Achilles tendinopathy [7,8]. Based on histopathologic findings, tendinopathy can be divided into Peritendinitis and Tendinosis (tendon degeneration). Some investigators avoid the term ‘‘degeneration’’ because they believe it is a misleading term denoting an irreversible pathologic process; where-as tendinosis is most likely reversible (Figure 1 & 2).
Figure 1: The pathophysiologic mechanisms of Achilles tendon overuse injuries and disorders, which also may lead to Achilles ruptures.

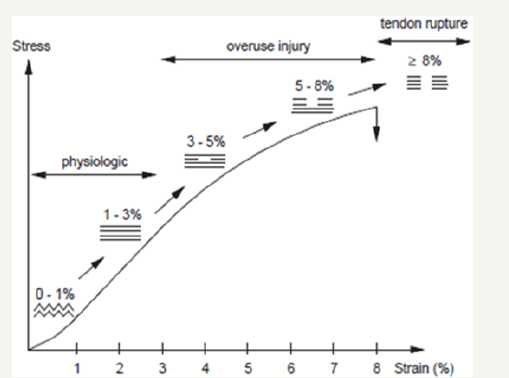
Figure 2: A schematic presentation of the development of the chronic tendon disorders. According to current concepts, repetitive tendon strain (3-5-8% srain) may lead to cumulative fiber microtrauma. If the reparative capacity of the tendon is exceeded, inflammation, edema, pain and tendon degeneration (overuse injury) can enuse.
Predisposing intrinsic factors related to achilles tendinopathy in sports
1. General factors
2. Gender
3. Age
4. Overweight
5. Constitution: Weak or Strong
6. Blood group
7. HLA-types
8. Predisposing diseases
9. Blood supply
1) Ischemia
2) Hypoxia
3) Hyperthermia
Local (anatomic) factors on the liver limb
1. Malalignments
1) Foot hyper- or hypopronation
2) Forefoot varus or valgus
3) Hindfoot varus or valgus
4) Pes planus or cavus
2. Leg length discrepancy
3. Muscle weakness and imbalance
4. Decreased flexibility
5. Joint laxity
Predisposing extrinsic factors related to achilles tendinopathy in sports
General factors
1. Theraupeutic agents
1) Corticosteroids (local and systematic)
2. Fluoroquinolone
1) Antibiotics
2) Weight-lowering drugs
3. Drugs
1) Anabolic steroids
4. Drugs/narcotics
1) Canabis
2) Heroin
3) Cocaine
Sports-related factors
1. Excessive loads on the lower extremities
1) Speed of movement
2) Type of movement
3) Number of repetitions
4) Footwear/Sportswear
5) Training surface
2. Training errors
1) Over distance
2) Fast progression
3) High intensity
4) Fatigue
5) Poor technique
3. Environmental conditions
1) Heat or Cold
2) Humidity
3) Altitude
4) Wind
4. Poor equipment
Achilles Tendon Rupture Management
Achilles tendon rupture is a common injury with an ever mounting incidence [9]. Paradoxically in 21st century medicine with all modern aids available; there is yet no unequivocal ideal standard treatment. For Achilles tendon rupture both surgical and non-surgical management techniques are often employed. The treatment method is usually chosen based on patient’s age type of sport or work practice and life style. Apart from traditional conservative therapy other minimally invasive procedures could be valid treatment modalities for Achilles tendon repair such as; ‘End-to-End’ suturing techniques ‘Bosworth technique’ ‘Chigot technique’ and ‘Tendon augmentation’ methods [10]. All can be combined in the form of ‘Krakow locking loop’ technique and ‘Triple bundle procedure’ to increase the tendons’ post rupture strength [11]. Conservative treatment comprises the use of a stretchable cast just above or below the knee. Interestingly knee position rarely affects the space between ruptured tendon ends [11]. For surgical procedures; generally spinal or epidural anesthesia is given. In open injury cases thorough wound wash and exposing the ruptured tendon end is essential. For closed injury a precise subcutaneous tissue dissection followed by alignment of ruptured fiber ends usually suffices [11]. It is largely agreed that open surgery with early mobilization is one of the best treatment methods [10].
Outcomes of Surgical and Conservative Management
Surgical treatment escalates the risk of wound infection contracture fistula sural nerve damage because of its proximity granuloma and wound necrosis. However it is still generally agreed that operative repair is associated with overall improved patient satisfaction rapid rehabilitation earlier resumption of work and sport activities [9]. Complications of non-operative management include tendon elongation and weak plantar flexion. Nevertheless available evidence from long term prospective cohorts suggest that the advantages of surgical repair over non-surgical management only affect individuals’ life quality on short term while in the long run these differences remain non-significant [11]. Overall there is no significant difference in re-rupture rates between surgical and non-surgical conservative management [9].
Conclusion
Achilles tendon is the sturdiest tendon in the human body. The incidence of Achilles tendon overuse injuries and widespread spontaneous ruptures has increased in industrialized countries during the past decades because of life style changes and increased participation in sports. The basic etiology of Achilles tendinopathy is known to be multi-factorial; several predisposing extrinsic and intrinsic factors having been attributed to the problem. Epidemiologic studies report misalignment of lower extremity and biomechanical faults as playing a causal role in two thirds of athletes with Achilles tendon disorders. Increased foot pronation limited subtalar mobility leg length discrepancy and limited range of ankle joint motion were more frequent among athletes with Achilles tendinopathy than those who had other complaints. Extrinsic factors like extreme loading of lower extremities prolonged monotonous actions training errors in running (extreme distance or intensity too much uphill or downhill work) as well as poor technique and fatigue are further risk factors for Achilles tendon overuse injuries. However a general lack of evidence based high quality prospective studies limits the strength of the conclusions that can be drawn regarding these extrinsic risk factors. The most common clinical diagnosis of Achilles overuse injuries is tendinopathy which represents a combination of pain and swelling in the Achilles tendon together with reduced ability to perform strenuous activities. Achilles tendinopathy is common in sports that require strenuous physical activity. Among all the diverse ruptures of human tendons a complete split of Achilles tendon is one that is accompanied most closely with sports activities. The incidence of Achilles tendinopathy peaks among individuals who participate in long-distance running mountaineering track and field top level runners tennis badminton volleyball and soccer [5]. Chronic Achilles tendon disorders are more common in older athletes than in young athletes (teenage and child athletes). Although histopathologic studies show that ruptured Achilles tendons have clear degenerative changes before the rupture many Achilles tendon ruptures take place suddenly without any prior warning signs or symptoms. Considering that professional ‘white-collar’ jobs comprise an overwhelming number among patients who have Achilles tendon rupture in combination with the degenerative changes; a potential causative effect of sedentary lifestyle on the increased prevalence of spontaneous tendon ruptures cannot be ignored. It has been proposed that sedentary life style accompanied by long sitting and standing hours with dependent position of calf predisposes to poor circulatory perfusion of the tendon and related muscles which later leads to degenerative changes. In all cases lack of flexibility or a stiff tendon increases the risk of injury. On a closing note muscle strength endurance and flexibility are an important part of any physical performance and thus can play a pivotal role in preventing certain sports injuries particularly related to Achilles tendon injuries. A fatigued muscle cannot protect the tendon from strain injury and subsequent inflammation and pain. Thus the energy absorbing capacity of the whole “Muscle tendon unit” is crucial in maintaining the health of the Achilles tendon. Targeted life style modifications can improve the rapture and re-rapture rates in tendinopathy.
References
- Jozsa L, Kannus P (1997) Human tendons: anatomy, physiology, and pathology. Human Kinetics, Champaign, Illinois, USA.
- Maffulli N (1999) Rupture of the Achilles tendon. J Bone Joint Surg 81A(7): 1019-1036.
- Paavola M, Kannus P, Järvinen TA, Khan K, Józsa L, et al. (2002) Achilles tendinopathy. J Bone Joint Surg 84-A(11): 2062-2076.
- Maffulli N, Kader D (2002) Tendinopathy of tendo achillis. J Bone Joint Surg 84(1): 1-8.
- Kvist M (1994) Achilles tendon injuries in athletes. Sports Med 18(3): 173-201.
- Kannus P, Jozsa L (1991) Histopathological changes preceding spontaneous rupture of a tendon. A controlled study of 891 patients. J Bone Joint Surg 73(10): 1507-1525.
- Maffulli N, Khan KM, Puddu G (1998) Overuse tendon conditions: time to change a confusing terminology. Arthroscopy 14(8): 840-843.
- Khan KM, Cook JL, Kannus P, Maffulli N, Bonar SF (2002) Time to abandon the ‘‘tendinitis’’ myth. BMJ 324(7338): 626-627.
- Holm C, Kjaer M, Eliasson P (2015) Achilles tendon rupture--treatment and complications: a systematic review. Scand J Med Sci Sports 25(1): e1-e10.
- Hani R, Kharmaz M, Berrada MS (2017) Should we prefer a surgical technique in the treatment of Achilles tendon ruptures? Pan Afr Med J 20: 285
- Gulati V, Jaggard M, Al-Nammari SS, Uzoigwe C, Gulati P, et al. (2017) Management of Achilles tendon injury: A current concepts systematic review. World J Orthop 6(4): 380-386.
© 2018 Tabinda Hasan. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






