- Submissions

Full Text
Perceptions in Reproductive Medicine
Craniotomy-An Art to Recast
Prabha Lal, Kanika Chopra*, Anuradha Singh and Meena Parihar
Department of Obstetrics and Gynaecology, Lady Hardinge Medical College, New Delhi, India
*Corresponding author: Kanika Chopra, Department of Obstetrics and Gynaecology, Lady Hardinge Medical College, New Delhi, India
Submission: November 11, 2021;Published: November 30, 2021

ISSN: 2640-9666Volume5 Issue1
Abstract
Background: Destructive operations in obstetrics are performed to allow vaginal delivery and avoid
cesarean section in moribund fetus and mother. The incidence of destructive procedure ranges from
0.21-0.5%, craniotomy being the most common of all. The most common indication is obstructed labor
followed by hydrocephalus.
Cases: We here discuss series of cases where craniotomy was done without any side effects to the mother.
The cases were of arrest of descent of head and obstructed labour with intrauterine demise and one was
hydrocephalus baby.
Conclusion: It is important to revisit and master the technique of destructive procedures to save the
obstetric future of young mothers.
Keywords: Coagulopathy;Craniotomy; Destructive obstetric procedure; Intrauterine demise; Obstructed labour
Introduction
Destructive operations in obstetrics are performed to allow vaginal delivery and avoid cesarean section in moribund fetus and mother. Its main purpose is to reduce the size of the dead fetus [1]. The various methods available are craniotomy, decapitation, cleidotomy, embryotomy and craniocentesis. The incidence of destructive procedure ranges from 0.21- 0.5%, with craniotomy being the most common of all [2,3]. The most common indication for performing destructive procedure is obstructed labor with dead fetus followed by hydrocephalus.
We present the case series of craniotomy done in our hospital with the aim to highlight the importance of knowing the art of performing it and also emphasizing the need to make all young obstetrician well versed with its technique. Destructive procedure when performed in expert hands, prove to be highly beneficial to the mother by saving her obstetric future. The aim of our study was to analyze the indications of performing the craniotomy and its associated complications in detail to highlight the importance of these forgotten procedures in modern obstetrics.
Case Series
A 30-year-old, primigravida at 38 weeks+ 4 days presented with gestational diabetes mellitus with pre-eclampsia with intrauterine demise with premature rupture of membranes in labour. She complaint of pain abdomen and leaking per vaginum for 6 hours at the time of admission to our emergency ward. She was a booked case but was non-compliant. She was diagnosed as a case of gestational diabetes mellitus and was advised insulin in view of deranged blood sugars. At her last visit in antenatal out-patient department, she was diagnosed as a case of gestational hypertension at 30 weeks of gestation and was advised admission to which women did not comply. She lost to follow up thereafter.
On presentation, her general condition was fair, she was afebrile, vitals were stable and blood pressure was 150/90mmHg. Her body mass index was 30.2kg/m2. On per-abdominal examination, obesity was present, uterus was term size with cephalic presentation, head was 4/5th palpable. Uterine contraction were 2-3/ 20-25 seconds/ 10 minutes. Tone was normal and fetal heart sound was not audible. On per vaginal examination, cervix was 4cm dilated, effacement was 40-50%, vertex was at -3 station, membranes absent and minimal amount of thick meconiumstained liquor was draining. Pelvis seemed adequate for the baby. Labour progressed spontaneously and was charted on partograph. After, entering the second stage of labour, head descent was not appreciated even after 2 hours of good uterine contractions. So, it was decided to take up the patient for craniotomy after written and informed consents.
Patient was laid in lithotomy position after adequate anesthesia. The per-vaginum findings were cervix fully dilated and effaced, vertex at -1 station, membranes absent and sutures in transverse. Long sturdy scissors were used to perforate the anterior fontanelle at right angle to the fetal skull and blades pushed in till its shoulders. The blades were then opened in one and then other direction and suction catheter used to suction out brain matter followed by delivery of the head by applying traction with the help of vulsellum. This was followed by delivery of the body. 3kg male baby was delivered. Mild atonic post-partum hemorrhage was managed medically. Post-delivery patient was started on triple antibiotics and thromboprophylaxis. Blood pressure and sugar charting were done and antihypertensive and oral hypoglycemics were started and patient was discharged on day 7.
Case 2
A 20-year-old, primigravida presented to gynae-emergency at 9 months of gestation with very severe anemia with intrauterine demise in second stage of labor. She complaint of pain abdomen and leaking per vaginum for 12 hours before admission. Patient was unbooked and uninvestigated. On presentation, general condition was poor, she was dehydrated and febrile, pulse rate was 112 beats/minute, blood pressure was 110/70mmHg, respiratory rate was 35/min, temperature was 102-degree Fahrenheit and saturation on room air was 90%. Pallor was present, clinically she appeared 4gm%, pedal edema, icterus, cyanosis was absent and JVP was not raised. Cardiovascular and chest examination was within normal limits. On per abdominal examination, uterus was term size, contour normal, cephalic presentation, liquor clinically decreased, relaxed uterus, non-tense and non-tender. Fetal heart sound was absent.
On per-vaginal examination, vagina was hot and edematous, cervix was fully dilated and effaced, membranes were absent, and no liquor was draining, vertex was at 0 station with caput and grade 3 molding. Patient was catheterized under all aseptic precautions. In her investigations, her hemoglobin was 3.5gm%, total leukocyte count was 20,000/mm3, platelet count was 40,000/ mm3, blood urea/serum creatinine were 42mg/dl and 0.4mg/dl, liver function test and coagulation profile were normal. Arterial blood gas analysis showed severe metabolic acidosis. In view of her poor clinical profile, after anesthesia and medicine consultation,adequate blood products were arranged and high-risk consents were taken and patient planned for craniotomy. Patient was intubated and craniotomy done in similar way as described above and she delivered a 1.7kg male baby. The most probable cause for obstructed labor in this case was uterine dystocia owing to improper management of the labour. She received 2 units of packed cell volume and 8 units of random donor platelets. She was extubated on post-partum day 2. She had multiple fever spikes till post-partum day 4 and was afebrile thereafter. She was given triple antibiotics and thromboprophylaxis for 7 days and discharged thereafter.
Case 3
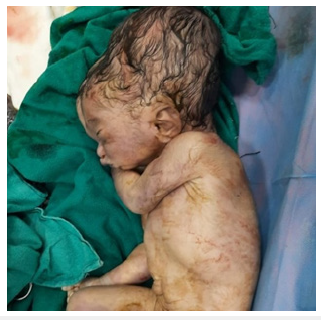
A 30-year-old, G3P2L2 at 37 weeks plus 4 days, presented to our emergency with compliant of leaking per vaginum in early labour. On evaluating her records, it was found that the baby had a gross hydrocephalus with Bi Parietal Diameter (BPD) of 123mm with marked thinning of brain parenchyma. She was unbooked at our hospital with single visit at 35 weeks of gestation in a dispensary nearby, where ultrasound obstetrics was advised that revealed above mentioned findings. Fetal medicine opinion was sought, and poor prognosis was explained. On examination, her general condition was fair, vitals stable. On per-abdominal examination, uterus was term size, with cephalic presentation, liquor was adequate, and was having 1-2 contractions/15 seconds/ 10 minutes. Fetal heart sound was 110 beats/minute. Ultrasound was done to assess the BPD and was 143mm. We decided to do abdominal cephalocenteis after written and informed consents. Around 1litre of cerebrospinal fluid was drained and BPD post-procedure was 9.4mm. Fetal heart sound was not seen post-procedure. Labour was allowed to progress, but in second stage of labor, vertex descent was not appreciated in spite of good uterine contractions for 2 hours and so decision was craniotomy was taken and proceeded. A, 2.6kg baby was delivered, as in Figure 1. Patient stood the procedure well and was discharged on post-partum day 4.
Figure 1: Dead baby with gross hydrocephalus delivered vaginally following craniotomy.
Discussion
Craniotomy is known to be one of the most common of all the destructive procedures performed, the incidence of it ranging from 68-90% [4,5]. It is becoming a lost art, but is deemed to be of utmost importance in cases such as in our series. Most common indications are obstructed labor with moribund fetus, gross hydrocephalus with poor prognosis and after coming head of the breech. The major contraindication of the destructive procedure is grossly contracted pelvis.
Case 2 in our series was a case of neglected obstructed labour with dead fetus and severely anemic mother with sepsis. In, this case, decision of craniotomy as the first choice proved to be beneficial even in current era of modern obstetrics which helped by saving obstetric carrier of the woman. Singhal SR et al. [5] did a study and also had cases of obstructed labor, teenage pregnancies, unattended labor, unbooked women presenting to emergencies benefitting with destructive procedures. Operative morbidity is lower with destructive procedures as compared to cesarean section being done in advanced second stage of labour with week and infected uterus.
The complications associated with destructive procedures are atonic postpartum hemorrhage, vaginal or perineal lacerations, urinary tract injury, sepsis and maternal death [4,5]. A study done by Gupta U et al. [6], showed that cesarean done for similar indications had higher rates of postpartum hemorrhage, sepsis, shock as compared to destructive procedures. These complications are known to be more likely to be related to the underlying factors causing obstructed labor and intrauterine fetal demise. Mild atonic post-partum hemorrhage was seen in our case series that was successfully managed medically and one had fever in post-partum but that was related to her pre-existing condition.
Conclusion
Young obstetrician should be trained and become well learned and master the technique of destructive operations till the goals of 100% antenatal registration and delivery by trained birth attendants is fulfilled by developing countries. Presence of skilled senior obstetrician is the most important prerequisite prior to retorting to destructive procedures.
References
- Bihash S, Gupta S, Lomi C, Khaniya B (2014) Fetal Craniotomy. J Nepal Med Ass 52(194): 825-827.
- Sikka P, Chopra S, Kaipdev A, Jain V, Dhaliwal L (2011) Destructive operation-a vanishing art in modern obstetrics: 25-year experience at a tertiary care center in India. Arch Gynaecol Obstet 283(5): 929-933.
- Adaji SE, Shittu SO, Sulle ST (2009) Operative vaginal delivery in Zaria, Nigeria. Ann Afr Med 8(2): 95-99.
- Umar AG, Maiahu AI, Pauti AA, Hassan M, Tunau K, et al. (2018) Destructive operative vaginal delivery in a tertiary health institution in Northwestern Nigeria: A ten-year review. World J Res Rev 6(1): 68-71.
- Singhal SR, Chaudhary P, Sanghwan K, Singhal SK (2005) Destructive operations in modern obstetrics. Arch Gynaecol Obstet 273(2): 107-109.
- Gupta U, Chitra R (1993) Destructive operations still have a place in developing countries. Int J Gynecol Obstet 44(1): 15-19.
© 2021 Kanika Chopra. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






