- Submissions

Full Text
Perceptions in Reproductive Medicine
Risk Reduction Strategies for Breast-Cancer Related Lymphedema in Democratic Republic of the Congo: Narrative Review
Jacques Lukenze Tamuzi1*, Jean Paul Muambangu Milambo2, Valery Kazadi Tshilombo3 and Leonidas N dayisaba4
1Department of Health Systems and Public Health, Stellenbosch University, South Africa
2Department of Pathology, Stellenbosch University, South Africa
3Department of Global Health, Stellenbosch University, South Africa
4Department of Respiratory Intensive Care, Groote Schuur Hospital, South Africa
*Corresponding author: Jacques Lukenze Tamuzi, Division of Health Systems and Public Health, Faculty of Medicine and Health Sciences, Stellenbosch University, Cape Town, South Africa
Submission: March 22, 2018;Published: May 31, 2018

ISSN: 2640-9666Volume2 Issue2
Abstract
Breast Cancer Related Lymphedema (BCRL) is a significant long-term co morbidity associated with (BC) management. BCRL impacts significantly on physical, psychosocial and economic implications of BC survivors, as a result of lymphatic system dysfunction related to breast injury. Many modifiable and non-modifiable risk factors for BCRL were identified in literature; these have contributed to cure progress and advanced knowledge on BCRL diagnosis and management at clinical stage. However, most of these studies were conducted in developed countries with limited information on such predictors and successful management strategies within African settings. Therefore, this review was conducted to summarize the available evidence on BCRL risk factors, incidence and management pathway in Democratic Republic of the Congo.
Keywords: Breast cancer; Lymphedema; Democratic republic of the congo
Abbreviations: BIS: Bioimpedance Spectrometry; BCRL: Breast Cancer Related Lymphoedema; CDT: Complex Decongestive Therapy; DRC: Democratic Republic of the Congo, LE: Lymphoedema; MLD: Manual Lymphatic Drainage; MSEP: Medically Supervised Exercises program; ISL: International Society of Lymphology; HRQOL: Health Related Quality of Life; QOL: Quality of Life; ROM: Range of Motility
Introduction
There is increased number of breast cancer survivors globally because of population growth and advanced in aging. It is estimated that approximately 1.7 million new cases of breast cancer cases diagnosed in 2012; accounting about 12% of incidence of all new cancer cases and 25% of all cancers in women. BC is classified the 5th cause of mortality among women [1]. In several countries, with advanced oncological techniques developed to manage breast cancer; the survivorship rate of early detection of BC was increased from 80% to 90%, fallowing to 25 percent for BCs detected at advanced stage [1,2]. BC is more prevalent in developed countries, but estimated 55% of breast cancer deaths occur in lower and developing countries [1]. A relative 5-years survivorship have been improved from 80% to 90% in developed countries, to 60% in developing countries, to below 40% in low income countries; within African continent, it may be as low as 11,99% [2].
Democratic Republic of the Congo (DRC) is a low income country located in middle Africa with life expectancy at birth of total 52 years; males=50 years and females=53 [1]. BC mortality profile in DRC reported by World Health Organization (WHO) in 2014 was 16. 00%, age standardized incidence rate (ASIR) of 4. 570 per 1000 females at risk [1]. The recent data demonstrate that 60% of population living in DRC are women; the most common cancers in prevalence and mortality for women are cervical cancer and BC (Figure 1 & 2 are attached at the bottom of the manuscript show the burden of cancers in DRC), yet there is no screening program for early detection of cancers [1]. A number of breast cancer patients are diagnosed at delayed stage of the condition and the prognostic is likely poor in most of the cases. Although BC treatment, includes surgery, radiation therapy, chemotherapy and hormonal therapy, have improved the outcomes resulting to prolonged survivorship; these techniques have also led BC survivors to potentially suffer from different comorbidities [3]. Many studies have demonstrated that BCRL is the most prevalent comorbidity associated with BC treatments [4-10]. Lymphoedema (LE) is the stasis of lymphatic fluid in interstitial tissues as result of dysfunction related to lymphatic system drainage of protein-rich liquid [5]. The consequences of lymphatic fluid stasis can lead to edema and hypoxia which are more observed in peripheral tissues [5]. The affected area can become swollen and distorted in shape [6-10]. This can result in pain, disfigured body parts, heaviness, discomfort, impairment of movement and it impacts on daily activities [11-14]. The details on international Classifications of Lymphoedema and the common symptoms can be found in International Society for Lymphoedema (ISL) guideline [7]. BCRL decreased the Health Related quality of life (HRQOL) and it is a life-long complication and considered the major sequelae associated with BC management [8]. Given that high incidence of BC in DRC with advanced techniques to manage BC; the comorbidities associated with BC management such as BCRL should be increased. However, there is no standardized BC guideline in DRC, the true prevalence and incidence of BC is not known because of lack of cancer registry in each province, data provided in this paper cannot be representative to all DRC. There is a Scarce of data on incidence, risk factors and management of BCRL in African countries such as DRC. This review aims to inform all stakeholders on awareness of BCRL among breast cancer survivors in DRC; so the evidence based healthcare approaches can be developed to mitigate BCRL occurrence.
Figure 1: Estimated age-standardized incidence and mortality rates from cancers: in women: DRC.
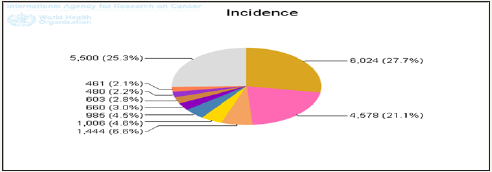
Figure 2: Standardized mortality rate of cancers in DRC.

Methods
MEDLINE, EMBASE, PubMed and Cochrane breast cancer registry were searched to identify the published articles focused on prevalence, incidence, risk factors and management of BCRL in DRC. MeSH term included: ((“breast cancer lymphedema”[MeSH Terms] OR (“breast”[All Fields] AND “cancer”[All Fields] AND “lymphedema”[All Fields]) OR “breast cancer lymphedema”[All Fields] OR (“breast”[All Fields] AND “cancer”[All Fields] AND “related”[All Fields] AND “lymphedema”[All Fields]) OR “breast cancer related lymphedema”[All Fields]) AND (“democratic republic of the congo”[MeSH Terms] OR (“democratic”[All Fields] AND “republic”[All Fields] AND “congo”[All Fields]) OR “democratic republic of the congo”[All Fields])) AND DRC [All Fields].
Current Status of Knowledge
One case report of BCRL was reported in the province of Katanga; a female BCRL patient was identified in Hospital of Lubumbashi after 2 years post mastectomy and actually on Tamoxifen 20mg/ daily [15]. The management of BCRL of this patient was not reported on the paper and the authors concluded that there is no evidence based study on this condition in our country, there is lack of an appropriate organized service to manage this type of complications and the prognosis is poor [15]. Although the incident cases are common in DRC; but there is lack of knowledge related to diagnosis and management of BCRL in DRC. Furthermore, financial concern, scare on appropriate materials related to socio-economic characteristics of the country, these impact in reducing in QOL and survivorship of BCRL patients [15].
Our review shows that there is lack of data on risk factors, incidence and management pathway of BCRL in DRC. A number of barriers were identified through the case report; these including lack of awareness on BCRL risk assessment, lack of healthcare workers knowledge in management of BCRL, lack of national guideline and policy for cancers prevention and control, lack of specialized facilities in lymphedema management and socioeconomic determinants of the country are more concerned [15]. This condition need awareness of health systems providers and policy makers for it prevention.
The incidence of LE among women undergoing BC treatment varies from 6% to 83% in literature [6]; the pooled incidence rate of LE reported in recent systematic review was 40% in 2010 [9]. BCRL incidence increases with the time since the diagnosis period. The incidence rates of LE can be under or over reported because of lack of standard protocol for diagnosis and measurement tools [9]. Further, the incidence of BCRL depends on the number of nodes removed during the breast surgery, types of BC treatment and the techniques used to measure LE volume [13].
There is a possible inaccuracy related to risk factors of the BCRL in many studies. The notable predictor of LE is extended BC surgery; this including axillary lymphatic node dissection and number of lymphatic nodules removed [9]. Other study have revealed that radiotherapy is associated with increased risk of developing BCRL [9], but other studies did not find the association between LE and radiation therapy [13, 14].This contradiction may be partially related to radiation doses used to treat the patients [9]. Of the clinical parameters associated with high risk to develop BCRL, the elevated body mass index (BMI>25), being obese (BMI>30) are the most consistent risk factors to LE [13,14]. In addition, positive lymphatic nodes and advanced stage of diseases are also reported in the review [15]. Moreover, recent development in molecular analysis demonstrated that congenital lymphatic system dysfunctions can be associated with various candidate genes to be established in early onset of LE for it prevention or management [15]; these including genes FLT4, FOXC2, HGF, GJC2 and SOX-18 [15]; American African women has also been reported being associated with BCRL risk factors in one pathway study [14]. In contrast to one review, such association was not statically significant. Growing in age, high level of education and socioeconomic indications were found to be both risk factors and risk reduction in some studies [9]. ISL purposes to promote all activities associated with knowledge translation in the field of lymphedema management, establishes relationship between researchers and clinicians working in the field of lymphology as well as allied healthcare workers [7]. ISL provides the platforms to exchange the ideas with different experts in lymphology field and collaborate with other national and international organizations [7]. Further, ISL also organizes international congresses yearly and postgraduate training in lymphology and wound care [7].
Table 1: BCRL risk assessment.
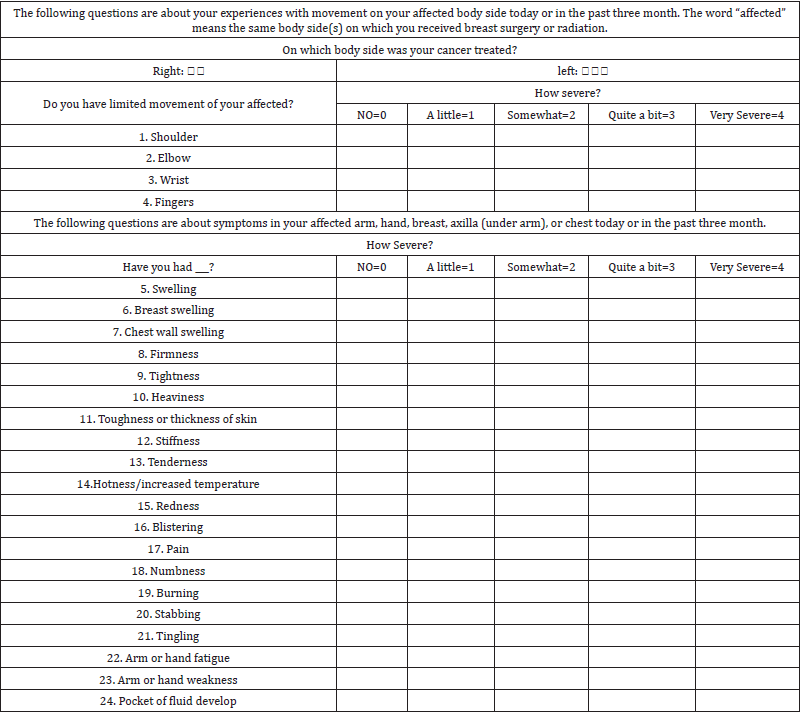
Table 2: International classification of lymphedema: 2013.

Various methods can be found in literature which can be used to diagnose or to measure BCRL and its incidence varies according to the methods used, such as circumferential limbs measurements, perometry, bioimpedance Spectrometry (BIS) and water displacement [9,16]. BIS is considered gold standard for LE diagnosis [14]; although; the review advocates that perometry should be more accurate than BIS, but the level of evidence for perometry still need to be established [16]. Table 1 & 2 at the bottom of the manuscript show the most common symptoms considered for LE diagnosis and ISL staging of LE respectively.
LE is does not have a curative treatment; the Complex Decongestive therapy (CDT) is considered the standard care internationally for LE management but the level of evidence is not yet established for each component of this intervention [16,17]. CDT enhances limb functions, maintains arm volume, reduces swelling and pain, and minimize disfiguration of the body shape. It includes four components: Manual Lymphatic Drainage (MLD), compression sleeves, remedial limb and deep-breathing exercises to promote venous and lymphatic flow and patient self-care. There are 2 CDT phases: the intensive phase includes all 4 components provided by LE therapists; in maintenance phase or secondary phase of CDT, a patient practices MLD assisted by physiotherapists or a trained care giver and skin care to prevent infections; this last phase is life-long therapy [17]. Additionally, maintenance phase of CDT is challenged for the patients to monitor and practice selfcare which is associated with noncompliance and can result to increase LE volume; recommended exercises purpose to restore range of motility (ROM) and to strength of affected limbs. There is inconsistency on exercise prescription and use of MLD; as the result there is lack of standardized exercise protocol for different stages of BCRL. Moreover, providing patients education on LE risk reduction among patients at risk was proved effective in improving a quality of life [17,18]. This risk reduction program including lifestyle interventions (eating healthy foods and participation in weekly regimen of supervised exercises) to be combined with CDT at maintenance phase of the treatment [19-23].
Conclusion
There is scarce of data on BCRL risk factors and management in DRC. No evidence based standardized guideline have been developed to date to assess the efficacy of a number of treatment options implemented in developed countries. More studies are needed to extend the knowledge, skills, and awareness of secondary lymphoedema throughout all the stakeholders. BCRL is life-threating condition associated with breast cancer management. Patient education on risk reduction strategies such as lifestyle, proactive risk factor managements, and developing specialized services with acquainted healthcare providers in lymphoedema management pathway should improve patients HRQOL. Cancer registry and innovative clinical studies should be conducted to mitigate its occurrence. The following recommendations are addressing to healthcare providers, researchers, policy makers and the funders:
A. Organisation of undergraduate and postgraduate training in cancer rehabilitation, especially in physiotherapy.
B. Provide evidence based research platforms to inform healthcare providers and patients on awareness of LE.
C. Develop a national cancer clinical guideline and surveying database to inform all stakeholders on impact of BCRL.
D. Develop the preclinical diagnosis (gene expressing) for lymphoedema prevention.
E. Develop a palliative care conceptual framework for cancer rehabilitation and secondary lymphoedema.
F. Collaborate with the national and internal experts in the field of cancer rehabilitation, research and management
What is already known on this Topic?
BCRL is common side effects associated with breast cancer management, impacts on BC survivors in reducing health related quality of life worldwide. The healthcare providers should be able to identify onset symptoms of BCRL, provide patients education on BCRL risk reduction and refer patients to specialized service for compression therapy. Breast Surgery, radiation therapy, hormonal therapy, chemotherapy, age, menopausal status, high body mass index and genetic predispositions are the consistent risk factors for breast cancer related lymphedema development.
What this Study Adds?
Many healthcare providers in DRC are not aware of risk factors and management of breast cancer related lymphedema. Complex Decongestive Therapy is the standard of care for lymphedema internationally, it comprises 4 components: manual lymphatic drainage, compression sleeves, decongestive exercises and selfcare. In addition, many countries lack their own guideline for lymphedema such as DRC. There is no curative treatment for BCRL at clinical stage, genotyping is recommended for BCRL risk prediction among patients at highest risk.
Authors’ Contribution
A. Designing, search strategy, writing, critical appraisal, edition and collaboration with other experts;
B. Designing figures, tables and critical appraisal, edition and search strategy;
C. Designing figures, tables and critical appraisal, edition and proofreading;
D. Design, search strategy, writing and critical appraisal, edition and collaboration with other experts.
Acknowledgement
Dr. Landry Kabego, Prof. V. Sewram, Prof. Delva Shamley, Prof. Maritha J Kotze, Prof. John Agadugu and Prof. G Mji contributed to designing of research question, acted like first reviewers and compiled the first draft. All authors approved to the last version of this manuscript after contributing as required.
References
- Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, et al. (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136(5): E359-E386.
- De Santis CE, Lin CC, Mariotto AB, Siegel RL, Stein KD, et al. (2014) Cancer treatment and survivorship statistics, 2014. CA Cancer J Clin 64(4): 252-271.
- Kwan ML, Darbinian J, Schmitz KH, Citron R, Partee P, et al. (2010) Risk factors for lymphedema in a prospective breast cancer survivorship study: the pathways study. Arch Surg 145(11): 1055-1063.
- Soran A, Ozmen T, McGuire KP, Diego EJ, McAuliffe PF, et al. (2014) The importance of detection of subclinical lymphedema for the prevention of breast cancer-related clinical lymphedema after axillary lymph node dissection; a prospective observational study. Lymphat Res Biol 12(4): 289-294.
- Lyman GH, Weaver DL, Somerfield MR, Bosserman LD, Perkins CL, et al. (2017) Sentinel lymph node biopsy for patients with early-stage breast cancer: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol 35(5): 561-564.
- Krok SJL, Oliveri JM, Kurta ML, Paskett ED (2015) Breast cancer-related lymphedema: risk factors, prevention, diagnosis and treatment. Breast Cancer Management 4(1): 41-51.
- International Society of Lymphology (2013) The diagnosis and treatment of peripheral lymphedema: 2013 consensus document of the international society of lymphology. Lymphology 46: 1.
- Fu MR, Ridner SH, Hu SH, Stewart BR , Cormier JN, et al. (2013) Psychosocial impact of lymphedema: a systematic review of literature from 2004 to 2011. Psycho‐Oncology 22(7): 1466-1484.
- Cheifetz O, Haley L (2010) Management of secondary lymphedema related to breast cancer. Can Fam Physician 56(12): 1277-1284.
- Stout NL, Pfalzer LA, Springer B, Levy E, McGarvey CL, et al. (2012) Breast cancer-related lymphedema: comparing direct costs of a prospective surveillance model and a traditional model of care. Phys Ther 92(1): 152-163.
- Pusic AL, Cemal Y, Albornoz C, Klassen A, Cano S, et al. (2013) Quality of life among breast cancer patients with lymphedema: a systematic review of patient-reported outcome instruments and outcomes. J Cancer Surviv 7(1): 83-92.
- Karlsson KY, Wallenius I, Nilsson-Wikmar LB, Lindman H, Johansson BB (2015) Lymphoedema and health-related quality of life by early treatment in long-term survivors of breast cancer. A comparative retrospective study up to 15 years after diagnosis. Supp Care Cancer 23(10): 2965-2972.
- Bell RJ, Robinson PJ, Barallon R, Fradkin P, Schwarz M, et al. (2013) Lymphedema: experience of a cohort of women with breast cancer followed for 4 years after diagnosis in Victoria, Australia. Support Care Cancer 21(7): 2017-2024.
- Kwan ML, Lee VS, Roh JM, Ergas IJ, Zhang Y, et al. (2015) Race/ethnicity, genetic ancestry, and breast cancer-related lymphedema. Cancer Res 75(15): 3724-3724.
- Léon KN, Ignace BK , Chantal MN, Migrette NT, John NL, et al. (2014) Massive pleural effusion after surgery of breast cancer and early discontinuation of tamoxifen: About an observation. Pan African Medical Journal 17: 129.
- Beth N, Felicity L, Mary-Anne K, Mathias F, Kaltin F (2012) Possible genetic predisposition to lymphedema after breast cancer. Lymphatic Research and Biology 10(1): 2-13.
- Jain MS, Danoff JV, Paul SM (2010) Correlation between bioelectrical spectroscopy and perometry in assessment of upper extremity swelling. Lymphology 43(2): 85-94.
- Lasinski BB (2013) Complete decongestive therapy for treatment of lymphedema. Semin Oncol Nurs 29(1): 20-27.
- Shaitelman SF, Cromwell KD, Rasmussen JC, Stout NL, Armer JM, et al. (2015) Recent progress in the treatment and prevention of cancerrelated lymphedema. CA Cancer J Clin 65(1): 55-81.
- Singh B, Disipio T, Peake J, Hayes SC (2016) Systematic review and meta-analysis of the effects of exercise for those with cancer-related lymphedema. Arch Phys Med Rehabil 97(2): 302-315.
- McNeely ML, Peddle CJ, Yurick JL, Dayes IS, Mackey JR (2011) Conservative and dietary interventions for cancer-related lymphedema: a systematic review and meta-analysis. Cancer 117(6): 1136-1148.
- Doyle C, Kushi LH, Byers T, Courneya KS, Demark-Wahnefried W, et al. (2013) Nutrition and physical activity during and after cancer treatment: an American cancer society guide for informed choices. CA Cancer J Clin 56(6): 323-353.
- Christine JC, Janice NC (2013) Lymphedema interventions: exercise, surgery, and compression devices. Seminars in Oncology Nursing 29(1): 28-40.
© 2018 Jacques Lukenze Tamuzi. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






