- Submissions

Full Text
Orthopedic Research Online Journal
Micromotion and Stress Shielding Between Taper Fluted and Cylindrical Femoral Stems for Paprosky Bone Deficiency Type IIIB
Sakkadech Limmahakhun*
Assistant Professor, Chiang Mai University, Thailand
*Corresponding author: Sakkadech Limmahakhun, Assistant Professor, Chiang Mai University, 110 Intawaroros Road, Si Phum, Muang, Chiang Mai 50200, Thailand
Submission: February 07, 2022;Published: February 16, 2022

ISSN: 2576-8875 Volume9 Issue2
Abstract
Purpose: Taper fluted and cylindrical femoral stems have been commonly used for revision surgery with femoral bone loss. Shape and material differences between taper fluted and cylindrical confused surgeons whether superiority and inferiority in comparisons especially for type IIIB Paprosky bone deficiency. This study aims to investigate the micromotion between implant and bone interface and stress distribution around the implant in human cadaveric experiments.
Methods: Paired comparisons of 7 cadavers between taper fluted stem and cylindrical stem were tested under dynamic cyclic loading.
Results: The results showed appropriate bone-implant micromotions for bone osteointegration could be observed between both taper fluted and cylindrical stems (85±10m and 113±80m respectively, p=0.59). Taper fluted stem attained the load distribution from the proximal to distal surrounding bone (from 4.92±2.87MPa to 2.14±1.43MPa, p=0.43), while the cylindrical stem type obviously showed the proximal bone stress shielding (from 2.56±0.76MPa to 5.23±0.77MPa, p=0.03).
Conclusion: Both taper fluted and cylindrical stems are feasible for Paprosky type IIIB reconstruction. However, the taper fluted stem is preferred since it seems to have better bone-implant stability and no further proximal surrounding bone stress shielding, especially for the thin femoral cortex. Be aware of over-reaming and appropriate stem diameter selection are crucial to prevent an early subsidence for the taper fluted stem.
Keywords: Taper fluted stem; Cylindrical stem; Micromotions; Stress shielding; Subsidence; Femoral bone deficiency
Introduction
The primary Total Hip Arthroplasty (THA) procedure trends to increase approximately 174% by 2030. Consequently, the expected demand for revision THA procedure has predicted that volume will be double by 2026 [1]. Despite an excellent outcome of primary THA, the outcome for revision THA is relatively poor due to the high complication rate after the revision.
A high-grade femoral defect is one of the most challenging problems during revision Total Hip Arthroplasty surgery (THA) [2]. The compromised proximal femur has minimal support in the metaphysis, which prevents the usage of the metaphyseal-fit cementless femoral stem and could not acquire enough initial stability as well as achieving enough bony ingrowth [3]. The long, diaphyseal-fit femoral stem was invented to overcome this limitation by relying on distal fixation and bypass the mechanical load to the remaining femoral diaphyseal bone stocks [3,4].
Fully-coated cylindrical cobalt-chromium (CoCr) stems have been commonly used for cementless femoral component revision for some years. These constructs are an excellent option for Paprosky type I, II, and IIIA-deficient femurs [5]. Although long-term survivorship has been well established (95-96% survivorship at 10-14 years), concerns have been raised regarding postoperative thigh pain, a high incidence of intraoperative fractures, and stress shielding of the proximal femur [6].
Tapered fluted titanium (Ti) femoral stems, on the other hand, gain more popularity as a revision stem design. These stems have high early survivorship (95-98% at a mean of 2-4.2 years [7]. Ti has a lower modulus of elasticity when compared with CoCr, resulting in reduced femoral component stiffness for equivalent stem diameter. By reducing the modulus mismatch between the femoral component and the host bone, better load transfer to the surrounding bone is expected. In addition, finite element analysis reported smaller micromotion at prosthesis - bone interface in tapered stem [8]. Furthermore, the incidence of intraoperative fracture and postoperative thigh pain was lower in the tapered design [9]. The greater femoral stress shielded bone resorption may be observed in fully coated cylindrical stem compare with distal tapered stem.
Although both cylindrical and tapered fluted distal fixation stem can be used in a proximal femoral bone loss reconstruction with a good success rate [8,10,11], the difference between the two stem designs for reconstruction especially in type IIIB femoral bone loss is not well demonstrated. Paproky and Sporer [12] mentioned an increase in failure of fully porous-coated cylindrical stems in a large femoral canal diameter >18mm, which is often seen in type IIIB and IV femoral bone defects. Therefore, this study aims to investigate the stress distribution, micromotion, and migration under dynamic loading conditions between taper fluted and fully coated cylindrical femoral stems in type IIIB proximal femoral bone deficiency.
Material and Methods
Cadaver preparation
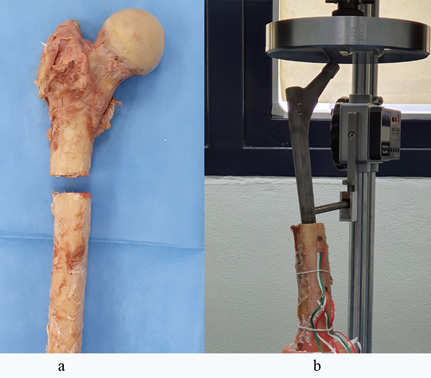
Two diaphyseal fixation stem designs were tested in this study between the taper fluted vs the cylindrical femora stem, Figure 1. Wagner SL Revision (Zimmer, Warsaw, IN) was selected as the representative of the tapered fluted design. It was made of titanium alloy with a grit-blasted surface for bony on-growth promotion. Eight resistance ribs were designed to improve torsional stability. As for the fully coated cylindrical design, Versys Porous Fullcoat (Zimmer, Warsaw, IN) was selected. This design has a cobaltchromium circular cross-section shaft with a beaded porous ingrowth coating.
Figure 1: Revision femoral stem between taper fluted stem (a) and fully coated cylindrical stem (b).

Seven pairs of fresh frozen cadaveric femurs (fourteen femora) from the cadavers of 5 female and 6 male donors were retrieved with soft tissue stripped off. All cadaveric femora were thawed at room temperature for 24 hours before implantation. Taper fluted femoral stems were randomly assigned either on the right or left side of each cadaveric femur. After that, the cylindrical full coated femoral stems were then paired to the contralateral femur. The type IIIB Praprosky proximal femoral defects were created by resection of the proximal femur 12cm from the greater trochanter, Figure 2.
Figure 2: The type IIIB Praprosky proximal femoral defects were created by resection of the proximal femur 12cm from the greater trochanter (a) and the experimental setup (b).
Fluoroscopy was used to confirm all specimens remain <4cm diaphysis for fixation. Implantation was conducted according to the manufacturer’s surgical manual in each design with proper stem size and length. All prostheses were templated and implanted to a depth of 6cm in the diaphyseal femur. X-rays were repeated after implantation to evaluate for bone-prothesis contact and any occult fractures. The research protocol was approved by the institution’s Internal Review Board, ID ORT-2556-01903.
Testing protocol
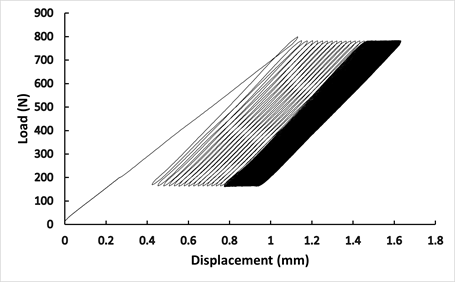
The implanted femurs were mounted distally in 9° valgus according to a natural anatomical axis in a pot using epoxy resin and fix to the loading jig that was attached to a universal testing machine with a load capacity of 30kN (Instron 5566; Instron Ltd., Buckinghamshire, England). A linear gauge was mounted to record relative bone-prosthesis displacement in a longitudinal plane. Axial preload of 200N was applied before each cyclic loading sequence. The initial subsidence by preload was excluded in analysis. Prosthesis-bone micromotion and strain pattern were continuously recorded during sinusoidal load of 750N for 200 cycles with 1Hz frequency, Figure 3. The loading for 200 cycles was found to be sufficient to reach a steady-state for bone-prosthesis micromotion.
Figure 3: The load displacement curve from 200 loading cycles.
The effectiveness of femoral stem design on promoting bone stress transfer to the periprosthetic bone was investigated. The results were compared with the taper flute and the cylindrical femoral stems. Two 120Ω strain gauge rosettes (KFGS-1- 120-D17-11; Kyowa Electronic instruments, Tokyo, Japan) were attached on the outer bony surface at 1cm and 6cm distal to the resection. The gages were aligned parallel to the longitudinal axis of the bone. Three tests were repeated under the load of 750N to calculate the average principal strain from proximal and distal strain gauge rosettes. The maximum and minimum principal strains (ε) can be calculated using 1-4 equations.
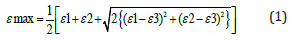
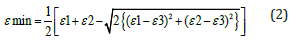
Where ε1, ε2 and ε3 are the strains in the gauge elements 1, 2 and 3. The maximum and minimum principal stresses (σ) on the tube surfaces can be calculated by
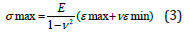
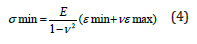
Where the Poisson’s ratio and elastic modulus of the bone material are ν = 0.3 and E = 1539MPa.
Statistical analysis
All recorded data were compared between the taper fluted femoral stem and the cylindrical femoral stem in each cadaver using STATA (version 14.0, Stata Corp LLC, College Station, TX, USA). Measurement of micromotion and maximum principal stress were compared using paired t test between the implanted femora for the same cadaver. All continuous data were reported as means and standard deviation. Statistical significance was set at P<0.05 and power at 0.8.
Results
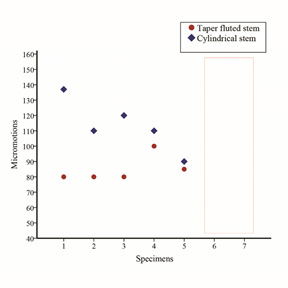
The average age of specimens was 73 y (65-80 y). This age group is a practical example for the real scenario since the revision cases are commonly found in old patients. Of the fourteen femurs conducted tests, two taper fluted stems were excluded due to the surgical error leading to massive femoral stem subsidence in early loading (8.06mm and 16.45mm), Figure 4. There was no significant difference for the prosthesis-bone micromotion between the tapered fluted stem and cylindrical stem group (85±10μm and 113±80μm respectively, p=0.59).
Figure 4: Bone-implant interfacial micromotions (m) between the taper fluted and cylindrical stem.
The strain measurements on the bony surfaces were transferred to the stresses acting on those regions. Table 1 shows no significant difference in the proximal and distal bone stresses could be observed between the taper fluted and the cylindrical femoral stems. The maximum principal stress at 1cm below the bone cut was 4.92±2.87MPa for the taper fluted stem and 2.56±0.77MPa for the cylindrical stem (p=0.47). In the meanwhile, the maximum principal bone stress at the tip of the stem (6cm distal to the bone cut) was no significant difference (2.14±1.43MPa and 5.23±0.77MPa for taper fluted and cylindrical stem, p=0.13).
Table 1: Micromotions and bone stress distribution between taper fluted and cylindrical femoral stems.
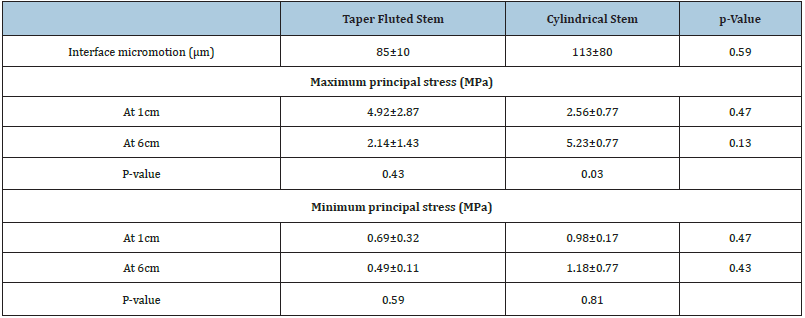
Bone stress distribution pattern was different between the taper fluted and the cylindrical femoral stems as shown in Figure 5. While the taper fluted stem attained the load distribution from the proximal to the distal portion of a periprosthetic bone (from 4.92±2.87MPa to 2.14±1.43MPa, p=0.43), the cylindrical stem type obviously showed the proximal bone stress shielding and the stem by-passed loads distally (from 2.56±0.76MPa to 5.23±0.77MPa, p=0.03).
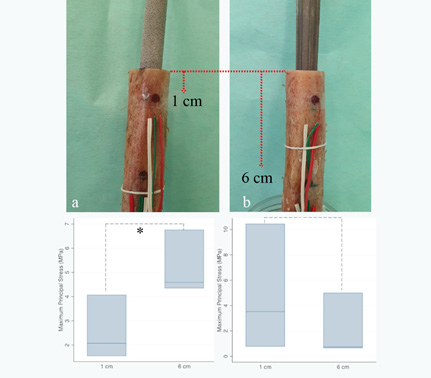
Figure 5: Bone stress analysis using rosette strain gauges at 1cm and 6cm from the osteotomy level between cylindrical stem (a) and taper fluted stem (b).
Discussion
The presence of proximal femur may obscure the distal motion between bone and implant and therefore would confound the comparison. Diaphyseal fixation is more critical in cases of an inadequate proximal bone stock, and our revision THA model represents the Paprosky type IIIB femurs by resecting the femur 12cm from the greater trochanter and allow only 6mm length of diaphyseal fit which is enough for minimum diaphyseal fixation [13]. Subsidence of the femoral stem usually manifests soon after weight-bearing, within 6-8 weeks of surgery, and typically, no later than 12 months postoperatively [14]. To achieve stable cementless revision stem fixation, initial prosthesis-bone micromotion should be restricted.
Initial stability from taper fluted and cylindrical femoral stem fixation in our in vitro study are comparable with minimal micromotions which are suitable for bony ingrowth in type IIIB femoral bone loss [15,16]. Both designs create enough initial stability with less than 150μm displacement (85±10μm and 113±80μm for taper fluted and cylindrical stem, respectively, p=0.59). It seems that the axial stability for taper fluted stem is greater than the cylindrical shape stem, although the statistical difference could not be observed. Similar to the previous study, the greater axial and rotational stability for taper fluted stem (13.33μm and 9.81μm) was noted compared to the cylindrical stem (18.37μm and 13.40μm) [10]. Taper fluted stem has superior initial fixation stability to fully porous-coated cylindrical stems as reported in a saw bone experimental study (1574N vs 500N) [17].
The difference in elastic modulus between taper fluted and cylindrical femoral stem is also a crucial concern. Ti has a lower modulus of elasticity compared to CoCr, leading to a lower stiffness for an equivalent stem diameter [17]. Clinical study also reported an incidence of bone resorption in the proximal femur around the cylindrical stem of 60-67% since 3 to 10 years after implantations [6]. Our study clearly demonstrated the proximal bone stress shielding around the cylindrical fully coated stem (2.56±0.76MPa and 5.23±0.77MPa, p=0.03). The factors that enhance proximal femoral bone resorption are women, patients with low cortical index, and large-diameter femoral stem especially for a diameter >18mm [9,15]. The high-stress concentration at the tip of the cylindrical stem relates to thigh pain, with a clinical incidence of 15.6% for an average of 12 years after implantations [6]. On the other hand, taper design shows better bone hoop stress and load distribution from the proximal-distal direction (4.92±2.87MPa to 2.14±1.43MPa).
The 15-y survivorship with revision of the extensive porouscoated cylindrical stem was 99.3%, whereas the 10-y survivorship with revision of the taper fluted stem was 93.5% [18]. Although the component longevity between taper fluted and cylindrical femoral stem is both excellent, the taper fluted stem shows advantages not only in biomechanics study but also in the clinical outcomes. The incidence of periprosthetic fracture after cylindrical femoral stem is higher than the taper fluted stem [9]. The tapered design allows for safer insertion since taper fluted stems are prepared in line-toline reaming. On the other hand, the cylindrical stems are prepared oversized relative to the ream size for adequate press-fit and engage early, which increases the potential risk of fracture. Despite the lower periprosthetic fracture rate observed in taper fluted stems, massive subsidence has been a major concern in this stem type [5,19]. There is 14% failure after tapered fluted stem implantations due to early massive subsidence (>5mm) in our study.
The design of taper fluted stem is susceptible to early subsidence with the prevalence of up to 35% of patients [5,19]. Inadequate stem diameter and the small 2 taper angle would be the cause of subsidence in this design [20]. A larger taper angle in a more temporary tapered fluted design showed less subsidence and promising results [21]. However, the surgical technique is matter for the taper stem insertion. Hand reaming with a precise depth can prevent over-reaming of the femoral canal and subsidence. Adequate diaphyseal fit for the taper stem design could be noticed when surgeons feel endosteal scratching and concomitant leg moving along with hand reaming. In general, a line-to-line stem size is recommended; however, the final stem size should be rechecked whether the depth of femoral stem penetration as determined in the preoperative planning is no longer move using moderate strikes of the mallet or the sound of the hammering changes. Prophylactic cerclage wiring is recommended before seating the stem trial to prevent the fracture. If the trail penetrates somewhat deeper beyond into the medullary canal, one size larger is recommended to avoid an early subsidence. In case of a femoral bow, distal femoral cortical perforation should be cautioned especially for a long taper fluted stem.
There were some limitations in this study. First, we acknowledge different bone qualities might result in selection bias; however, this limitation was restricted by comparing different stem types within the same cadaver. Second, the axial stability investigated in this study was unable to replicate the implant stability during complex motions of the hip joint. However, the micromotion and subsidence mainly resulted from walking or standing which considered as a compression force as conducted in this study.
Conclusion
Both taper fluted and cylindrical femoral stems provided adequate initial stability with a proper micromotion range for boneimplant osteointegration for type IIIB Praprosky femoral bone loss. Although only initial stability was investigated, it is one of the main factors responsible for desirable long-term clinical outcome. Regardless of aforementioned advantages and disadvantages of each design, both cylindrical and tapered fluted stem show excellent survivorship. Taper fluted stem has a biomechanical advantage in revision hip arthroplasty surgery with proximal femoral defect in term of better stress distribution without stress shielding effect and stability. Early subsidence for the taper fluted stem could be prevented by implant oversized relative to the ream size if the trail penetrates deeper beyond the desired depth for adequate press-fit and engage early.
Acknowledgement
The authors would like to express their sincere thanks to Zimmer Biomet Thailand for prostheses donation in this experiment. Aside from the donation, Zimmer Biomet Thailand was not involved in study design, data analysis and interpretation, or manuscript writing and submittal decision. The authors would like to thank the Cadaveric Surgical Training Center, Faculty of Medicine, Chiang Mai University for providing the cadavers used in this study.
Conflict of Interest
The authors have no relevant financial or non-financial interests to disclose.
References
- Kurtz S, Ong K, Lau E, Mowat F, Halpern M (2007) Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 89(4): 780-785.
- Sakellariou VI, Babis GC (2014) Management bone loss of the proximal femur in revision hip arthroplasty: Update on reconstructive options. World J Orthop 5(5): 614-622.
- Paprosky WG, Aribindi R (2000) Hip replacement: treatment of femoral bone loss using distal bypass fixation. Instr Course Lect 49: 119-130.
- Kwong LM, Miller AJ, Lubinus P (2003) A modular distal fixation option for proximal bone loss in revision total hip arthroplasty: a 2- to 6-year follow-up study. The Journal of arthroplasty 18(3 Suppl 1): 94-97.
- Palumbo BT, Morrison KL, Baumgarten AS, Stein MI, Haidukewych GJ, et al. (2013) Results of revision total hip arthroplasty with modular, titanium-tapered femoral stems in severe proximal metaphyseal and diaphyseal bone loss. J Arthroplasty 28(4): 690-694.
- Kang JS, Moon KH, Park SR, Choi SW (2010) Long-term results of total hip arthroplasty with an extensively porous coated stem in patients younger than 45 years old. Yonsei Med J 51(1): 100-103.
- Abdelsamie KR, Elhawary I, Ali H, Ali M, El-Shafie M, et al. (2020) Outcomes of modular femoral revision implants and the effect of component design on subsidence. Bone Joint J 102-b(6): 709-715.
- Kosmopoulos V, Russell RD, Rodrigues DC, Bucci G, Huo MH (2020) Tapered stem geometry provides superior initial fixation stability to cylindrical stem geometry in the setting of severe bone loss: A finite element analysis. Engineering Reports 2(8): e12218.
- Zhang Y, Zhang Y, Sun JN, Hua ZJ, Chen XY, et al. (2020) Comparison of cylindrical and tapered stem designs for femoral revision hip arthroplasty. BMC Musculoskeletal Disorders 21.
- Kirk K, Potter B, Lehman R, Xenos J (2007) Effect of distal stem geometry on interface motion in uncemented revision total hip prostheses. American journal of orthopedics (Belle Mead NJ) 36(10): 545-549.
- Russell RD, Pierce W, Huo MH (2016) Tapered vs cylindrical stem fixation in a model of femoral bone deficiency in revision total hip arthroplasty. J Arthroplasty 31(6): 1352-1355.
- Sporer SM, Paprosky WG (2003) Revision total hip arthroplasty: the limits of fully coated stems. Clin Orthop Relat Res (417): 203-209.
- Ellenrieder M, Souffrant R, Schulze C, Mittelmeier W, Bader R (2020) Micromotion and subsidence of a cementless conical fluted stem depending on femoral defect size - A human cadaveric study. Clin Biomech (Bristol, Avon) 80: 105202.
- Al-Najjim M, Khattak U, Sim J, Chambers I (2016) Differences in subsidence rate between alternative designs of a commonly used uncemented femoral stem. Journal of Orthopaedics 13(4): 322-326.
- Engh CA, O'Connor D, Jasty M, McGovern TF, Bobyn JD, et al. (1992) Quantification of implant micromotion, strain shielding, and bone resorption with porous-coated anatomic medullary locking femoral prostheses. Clin Orthop Relat Res (285): 13-29.
- Pilliar RM, Lee JM, Maniatopoulos C (1986) Observations on the effect of movement on bone ingrowth into porous-surfaced implants. Clin Orthop Relat Res (208): 108-113.
- Richards CJ, Duncan CP, Masri BA, Garbuz DS (2010) Femoral revision hip arthroplasty: a comparison of two stem designs. Clinical Orthopaedics and Related Research 468(2): 491-496.
- Picado CHF, Savarese A, Cardamoni VDS, Sugo AT, Garcia FL (2020) Clinical, radiographic, and survivorship analysis of a modular fluted tapered stem in revision hip arthroplasty. J Orthop Surg (Hong Kong) 28(1): 2309499019891638.
- (2013) A comparison of modular tapered versus modular cylindrical stems for complex femoral revisions. J Arthroplasty 28(8 Suppl): 71-73.
- Isacson J, Stark A, Wallensten R (2000) The wagner revision prosthesis consistently restores femoral bone structure. Int Orthop 24(3): 139-142.
- Ngu AWT, Rowan FE, Carli AV, Haddad FS (2019) Single 3° tapered fluted femoral stems demonstrate low subsidence at mid-term follow-up in severe bony deficiency. Annals of Translational Medicine 7(23): 725-725.
© 2022 Sakkadech Limmahakhun. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






