- Submissions

Full Text
Orthopedic Research Online Journal
Coracoid Deformity in Obstetric Brachial Plexus Palsy
Yussef Ali Abdouni*
Department of Orthopedics, Santa Casa Medical School, Brazil
*Corresponding author: Yussef Ali Abdouni, Department of Orthopedics, Assistant Professor of the Orthopedic Departament of Santa Casa, Member of the Brazilian Society of Hand Surgery, International Member of the American Society for Surgery of the Hand (ASSH), Santa Casa Medical School, Rua Cesário Mota, São Paulo-01221-020, Brazil
Submission: May 01, 2018;Published: May 30, 2018

ISSN: 2576-8875
Volume3 Issue1
Abstract
Secondary shoulder deformities are frequently observed in patients with obstetric brachial plexus palsy. Muscular imbalance promotes internal rotation, retroversion of the glenoid cavity and, at least, posterior displacement of the humeral head. This dislocation, in addition to the action of the muscle insertions on the coracoid process, causes a elongation of this structure. The coracoid follows the migratory humeral head, overlaping the plane of the glenoid. The reduction of the humeral head may be prevented by the deformity of the coracoid.
Keywords: Brachial plexus; Obstetric paralysis; Scapula
Introduction
Patients with partial recovery of obstetric brachial plexus injuries may develop shoulder deformities secondary to the imbalance between the active internal rotator muscles and the insufficient external rotators. Changes in the glenohumeral joint gradually occur, with retroversion of the glenoid cavity and an accentuation of the internal rotation, culminating with the posterior displacement of the humeral head [1,2]. In addition, by the action of the biceps brachii, coraco-brachialis, and pectoralis minor muscles, there is an elongation of the coracoid process, which protrudes further towards the scapular line and the humeral head (Figure 1). Nath et al concluded, through tomographic measurements, that there are statistically significant differences in the size of the coracoid and its distance to the humeral head between the normal sides and affected by obstetric paralysis [3]. This alteration in the coracoid process can limit the elevation of the limb by the impact of this elongated structure against the humeral head, besides interfering in the surgical treatment, in those cases in which there is a need to relocate the humeral head.
Figure 1: Computed tomography with 3D reconstruction of the shoulder of a 9-year-old patient with sequela of obstetric palsy. The elongated coracoid process is observed and projected onto the humeral head, which is posterior displaced.

Decreased coraco-scapular angle and coraco-humeral distance can be attributed to the stresses applied on the coracoid process caused by the medial rotation contracture and/or posterior subluxation of the humeral head [4]. Movements of the humeral head (internal and external rotation and abduction) influence the growth and direction of the coracoid. In obstetric paralysis, these movements are reduced and posterior subluxation of the humeral head occurs [5]. The coracoid tends to follow the displaced head maintaining more or less the same proportion of coracohumeral distance and the size of the scapula. With the progression of glenohumeral deformity, the coracoid process protrudes more caudally and follows the subluxation of the humeral head. In fact, the coracohumeral distance narrows secondary to the presence of posterior subluxation of the humeral head on the affected shoulders [3].
The coracohumeral distance becomes especially minor when the shoulder is rotated internally. The coracoid overlap is greater in patients with glenohumeral deformities for reasons similar to those mentioned above. The medial rotation contracture causes posterior humeral head subluxation and glenoid retroversion [4,5]. These factors influence the growth and direction of the coracoid, since it follows the migratory humeral head, carried by the muscular insertions in it. As a result, the coracoid intercepts and overlaps the plane of the glenoid. Surgical intervention is usually required for these patients to correct their glenohumeral deformities by repositioning the posteriorly subluxated humeral head anteriorly to properly articulate with the glenoid. However, the abnormal spatial orientation of the coracoid process may potentially interfere with the success of this procedure [6]. The resection of the coracoid process in these situations, besides allowing adequate reduction of the humeral head, eliminates the mechanical barrier to the elevation of the upper limb.
In Waters stages III and IV, where it is still possible to reduce the humeral head and some degree of remodeling of the glenoid surface [7], by redistributing the pressure of the humeral head on this surface, as in congenital hip dysplasia, this procedure is indicated. The approach can be obtained by a small deltopectoral access and the osteotomy must be sufficiently done to no longer present the impingement (Figure 2). It is usually necessary to remove the pectoralis minor, short head of the biceps and the coraco-brachialis insertions. Release of the elbow flexors in this procedure is another advantage as there is often an imbalance of forces leading to a flexion contracture [8].
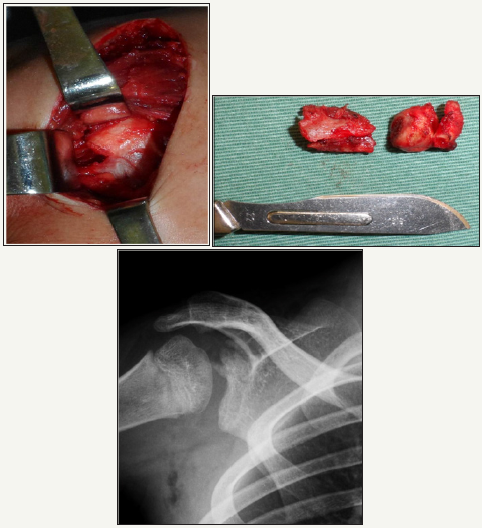
Figure 2:
Right: Surgical approach;
Left: The resected coracoid process;
Below: Reduction of the humeral head obtained after resection.
In the same surgical time it is possible and advisable to release the internal rotators, either by the arthroscopic approach, as described by Pearl et al. [9], or by the conventional anterior access. In the postoperative period the child remains immobilized for 6 weeks with the shoulder in neutral rotation.
References
- Birch R (2001) Late sequelae at the shoulder in obstetrical palsy in children. Surgical techniques in orthopaedics and traumatology: Shoulder. In: Randelli M, Karlsson J (Ed.), Surgical Techniques in Orthopaedics and Traumatology. Elsevier, Paris, France 3: 55-200-E-210.
- Waters PM, Smith GR, Jaramillo D (1998) Glenohumeral deformity secondary to brachial plexus birth palsy. J Bone Joint Surg (Am) 80(5): 668-677.
- Nath RK, Paizi M (2007) Scapular deformity in obstetric brachial plexus palsy: a new finding. Surg Radiol Anat 29(2): 133-140.
- Soldado F, Kozin SH (2005) The relationship between the coracoid and glenoid after brachial plexus birth palsy. J Pediatr Orthop 25(5): 666- 670.
- Kozin SH (2004) Correlation between external rotation of the glenohumeral joint and deformity after brachial plexus birth palsy. J Pediatr Orthop 24(2): 189-193.
- Nath RK, Karicherla P, Mahmooduddin F (2010) Shoulder function and anatomy in complete obstetric brachial plexus palsy: Long-term improvement after triangle tilt surgery. Childs Nerv Syst 26(8): 1009- 1019.
- Waters PM, Bae DS (2005) Effect of tendon transfers and extra-articular soft tissue balancing on glenohumeral development in brachial plexus birth palsy. J Bone Joint Surg Am 87(2): 320-325.
- Nath RK, Melcher SE, Lyons AB, Paizi M (2007) Surgical correction of the medial rotation contracture in obstetric brachial plexus palsy. J Bone Joint Surg Br 89: 1638-1644.
- Pearl ML, Edgerton BW, Kazimiroff PA, Burchette RJ, Wong K (2006) Arthroscopic release and latissimus dorsi transfer for shoulder internal rotation contractures and glenoumeral deformity secondary to braquial plexus birth palsy. J Bone Joint Surg(Am) 88(3): 564-574.
© 2018 Yussef Ali Abdouni. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






