- Submissions

Full Text
Orthoplastic Surgery & Orthopedic Care International Journal
Osteoid Osteoma of the Metacarpal Head, A Case Report
Isaac Gammal* and Nader Paksima
Department of Orthopedic Surgery, NYU Langone Orthopedic Hospital, USA
*Corresponding author: Isaac Gammal, Department of Orthopedic Surgery, Division of Hand and Upper Extremity Surgery, NYU Langone Orthopedic Hospital, New York, USA
Submission: April 26, 2022;Published: May 26, 2022
ISSN 2578-0069Volume2 Issue4
Abstract
Keywords:Osteoid osteomas; Prostaglandins; Metacarpophalangeal; Tumor; Bone; Fluoroscopy; Radiofrequency; Misdiagnosis; Skeleton
Abbreviations:OO: Osteoid Osteomas; MP: Metacarpophalangeal; CT: Computed Tomography; MF: Middle Finger
Introduction
Osteoid Osteomas (OO) are small benign osteogenic tumors most commonly seen in the long bones of the lower extremity. They typically present in the first two decades of life. They are characterized by pain, often worse at night, which characteristically responds to aspirin and other nonsteroidal anti-inflammatory drugs, due to increased production of prostaglandins in these tumors. The tumor appears as an oval lytic nidus surrounded by fusiform cortical bone thickening. The nidus ranges between 5 and 20mm and is inconsistently visualized due to significant sclerosis. Between 19% and 31% of OO present in the upper extremity, and 5-15% of all lesions are seen in the hand and wrist, where it occurs most frequently in the phalanges [1]. The metacarpal bone is the least common site for OO [2].
Case Report
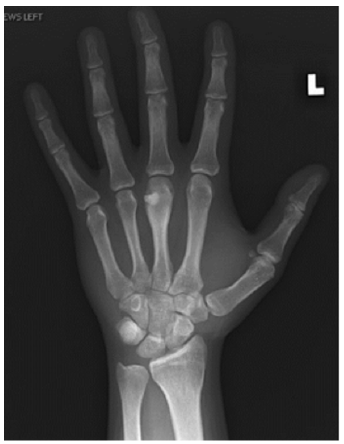
A 22-year-old right hand dominant male graduate student presented with 7 months of intermittent left-hand pain. He had seen an outside physician in the past and was diagnosed with a middle finger Metacarpophalangeal (MP) capsular sprain after radiographs were interpreted as negative. His past surgical history was significant for an ipsilateral both bone forearm fracture treated with intramedullary nailing when he was a child. Clinically, there was tenderness to palpation over the third metacarpal head and a mild prominence to palpation noted. Grip strength was significantly diminished on the affected side. His neurovascular status was intact. He had well-healed surgical scars from the previous forearm fracture and hardware removal and full elbow, forearm, wrist, and hand motion. Upon surgeon review of radiographs, there was a small lucent lesion in the ulnar aspect of the middle finger metacarpal head with areas of internal mineralization and adjacent cortical thickening (Figure 1). Computed Tomography (CT) imaging of the hand was performed for further evaluation, which showed a punctate central calcification with regular borders and surrounding reactive sclerosis (Figure 2), consistent with OO. The patient had failed a trial of nonoperative management and was indicated for excisional biopsy. A joint sparing approach was performed through a curvilinear incision over the ulnar aspect of the Middle Finger (MP) joint. A small incision was made in the proximal aspect of the sagittal fibers overlying the lesion, leaving the distal fibers intact. Caution was exercised to avoid violating the joint capsule. The junctura tendinum from the middle to ring extensor tendon was incised to aid in visualization. A 1.1mm Kirschner wire was used to mark the proposed cortical window and confirmed with fluoroscopy. An oval shaped cortical window was made with a small handheld burr (Figure 3). The lesion was then curetted, and the defect packed with calcium phosphate cement until adequate fill was confirmed with fluoroscopy (Figure 4). The extensor hood was repaired, as well as a locking horizontal mattress suture to repair the junctura. At 6-month follow up the patient was painfree and there was adequate cement filling the defect with no residual lucency (Figure 5).
Figure 1:Preoperative PA radiograph.
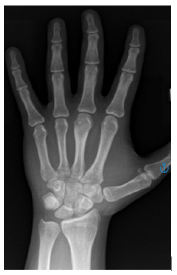
Figure 2:Coronal CT image.
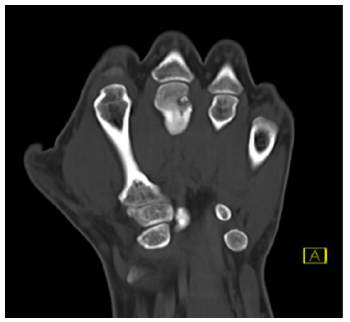
Figure 3:Intraoperative view of cortical window.
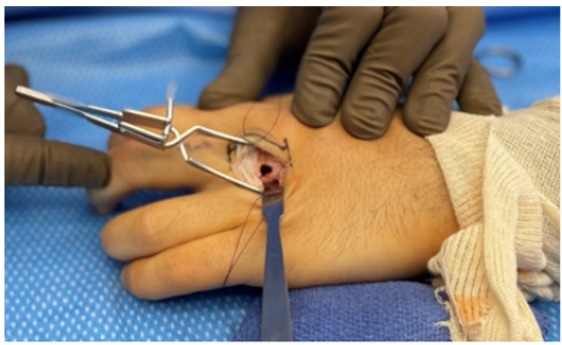
Figure 4:Fluoroscopic view post-curettage with calcium phosphate cement filling the defect.
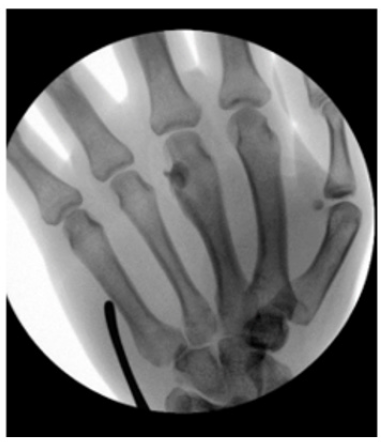
Figure 5:6-month follow up radiographs.
Discussion
Osteoid osteoma is a tumor of the developing skeleton and presents consistently with bone pain worse at night. By definition, OO do not exceed 1cm in diameter. Misdiagnosis of OO is common in atypical presentations resulting in a prolonged term of care. The atypical symptoms of OO and the presence of concurrent trauma or sports injuries may lead to misdiagnosis and delayed treatment, particularly during its early stage when symptoms are present, but no lesion is detected [3]. Treatment options for OO of the hand are limited, relative to treatment of lower
extremity diaphyseal OO. Percutaneous radiofrequency ablation demonstrates durable results in 90% of patients after 1-2 sessions [4]. However, its use is contraindicated for lesions in the hand due to the increased risk of soft tissue burns. To our knowledge, there is only one published report of a metacarpal head condylar lesion treated with en bloc excision. While the authors do not disclose their surgical technique rationale, the small lesion size and joint involvement render intraoperative visualization difficult, favoring en bloc excision. In our case we were able to accurately localize the lesion preoperatively with thin cut CT imaging and intraoperative fluoroscopy, enabling us to perform a complete surgical excision through a joint sparing approach. Several histological studies have been carried out with the specific aim of verifying the existence of nerve fibers within OO [5]. The histochemical procedures based on the affinity of nerves for silver stains have made it possible to demonstrate the presence of fine nerve fibers associated with these tumors [6]. Future advances in intraoperative staining may further aid in identification and complete excision of these lesions.
References
- Cohen JD, Harrington TM, Ginsberg WW (1983) Osteoid osteoma: 95 cases and a review of the literature. Semin Arthritis Rheum 12(3): 265-281.
- Chronopoulos E, Xypnitos FN, Nikolaou VS, Efstathopoulos N, Korres D (2008) Osteoid osteoma of a metacarpal bone: A case report and review of the literature. J Med Case Rep 2(1): 285.
- He H, Xu H, Lu H (2017) A misdiagnosed case of osteoid osteoma of the talus: A case report and literature review. BMC Musculoskelet Disord 18(1): 35.
- Barei DP, Moreau G, Scarborough MT, Neel MD (2000) Percutaneous radiofrequency ablation of osteoid osteoma. Clinical Orthopaedics and Related Research 373: 115-124.
- Fatayri B, Djebara AE, Fourdrain A, Bulaid Y, Sanguina M (2019) Resection of a rare metacarpal distal condyle osteoid osteoma. Case Rep Orthop 2019: 4542862.
- Greco F, Tamburrelli F, Laudati A, Cara LA, Trapani DG (1988) Nerve fibres in osteoid osteoma. Ital J Orthop Traumatol 14(1): 91-94.
© 2022 Isaac Gammal. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






