- Submissions

Full Text
Open Access Biostatistics & Bioinformatics
Managing Pandemic Disasters: A Resource-Based Analysis
Boaz Ronen1, Moshe Leshno1, Zvi Lieber1, Alex Coman2, Joseph S Pliskin3* and Shimeon Pass4
1Tel Aviv University, Coller School of Management, Israel
2The Academic College of Tel Aviv-Yaffo, Israel
3Ben Gurion University of the Negev, Department of Industrial Engineering and Management, Israel
4SH. Pass and Associates, Kiryat Ono, Israel
*Corresponding author:Joseph S Pliskin, Ben Gurion University of the Negev, Department of Industrial Engineering and Management, Department of Health Policy and Management, Harvard T.H. Chan School of Public Health, Israel
Submission: February 02, 2024;Published: February 13, 2024

ISSN: 2578-0247 Volume3 Issue4
Opinion
Healthcare crises are well-known phenomena that occur and are highly disruptive. Consider, for example, Covid19 and other pandemics, wars, multi-casualty natural disasters, industrial disasters, etc. Healthcare systems in Brazil, Spain, Italy, and more around the world collapsed due to the lack of a clear methodology for handling such crises. Following a largescale value creation project with a large medical center we developed a resource-based methodology to cope with three healthcare crisis scenarios: “Peace”, “War” and “Tsunami”.
We identified three load/capacity scenarios for hospitals: “Peace”, “War” and “Tsunami”. The Peacetime scenario is the normal overload situation in a hospital. Figure 1 during “Peace” times, hospitals are usually 10%-20% short in resources. To overcome bottlenecks, managers apply evolutionary methods such as constraint management [1], the complete kit concept, etc. This is the normal condition in hospitals where there are fluctuations in supply and demand. Bottlenecks in this situation are typically medical crews: senior physicians and experienced nurses.
Figure 1:We identified three load/capacity scenarios for hospitals: “Peace”, “War” and “Tsunami”. The Peacetime scenario is the normal overload situation in a hospital.
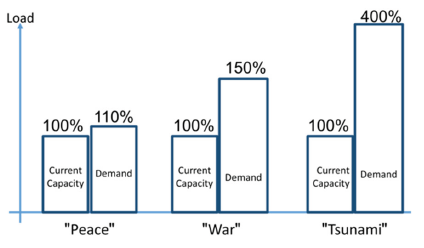
During “War” times, such as during the COVID-19 pandemic, the need for resources exceeds capacity by over 50%. To overcome this shortage, managers use the above-mentioned evolutionary methods but must also apply revolutionary methods. Here too, system bottlenecks are typically the medical crews. The first step is to create a protective capacity by rapid deployment of auxiliary hospitals. Converting internal medicine wards to COVID-19 wards, postponing elective surgeries, etc. Medical crews work significantly harder and effort must be made to offload them through nurses, paramedics, physician assistants, etc. War scenarios require a hybrid application of evolutionary and revolutionary actions. During “Tsunami” times, thousands of patient’s storm hospital emergency departments. In this scenario, revolutionary methods must be applied. Since the bottlenecks are still medical crews, the policy should be to hospitalize a minimum number of patients and send the majority back to their communities.
Evolutionary steps are a waste of managerial energy during the Tsunami scenario as they focus on double-digit improvement rather than on an “order-of-magnitude” increase. For Peace and War scenarios, the Theory of Constraints (TOC) can serve as an effective tool to increase capacity. During “peace” times, evolutionary strategies handle excess demand peaks. During “war” times, a hybrid evolutionary/disruptive (revolutionary) strategy should be applied. During “Tsunami” times, a disruptive (revolutionary) strategy should be applied exclusively.
This paper deals with healthcare crisis management during pandemic times. The leader must diagnose the condition the organization is in and act accordingly. The concept is applicable in other “code brown” crisis management scenarios such as chemical or nuclear massive accidents, natural disasters, etc. Many leaders respond intuitively to such crises. By establishing a resource management methodology, we strive to facilitate the dialogue within the team and also among teams that have not worked together in the past.
References
© 2024 Joseph S Pliskin. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






