- Submissions

Full Text
Medical & Surgical Ophthalmology Research
Ocular Biometry and its Relation to Amplitude of Accommodation in Normal Subjects
Masoumeh Ahadi1, Afsaneh Ebrahimi2 and Shahrokh Ramin3*
1PhD candidate in Optometry and vision science, Shahid Beheshti University of Medical Sciences, Iran
2Ophthalmologist, Eye clinic in Omid Hospital, Iran
3Ophthalmologist, Shahid Beheshti University of Medical Sciences, Iran
*Corresponding author: Shahrokh Ramin,Student Research Committee, Shahid Beheshti University of Medical Sciences, Tehran, Iran
Submission: October 2, 2020;Published: November 11, 2020

ISSN 2578-0360 Volume3 Issue1
Abstract
Purpose: To assess age-related ocular biometric findings and relation with amplitude of accommodation in normal subjects.
Methods: This study was conducted on 295 normal subjects. In all participants slit lamp biomicroscopy, funduscopy, and measurement of visual acuity and refraction, and biometry were performed. Amplitude of accommodation was measured by the push up test. In this study, right eyes of subjects were selected to statistical analysis.
Results: The mean spherical equivalent was 0.13±0.27D and the mean keratometric power was 44.03±1.51D. There was a significant relationship between age and the mean keratometric power (r=0.164, P=0.006). The mean axial length of eyes was 22.91±0.76mm and was correlated with both the keratometric power (r=-0.727, P<0.001) and the axial length (r=-0.165,P=0.019). The mean amplitude of accommodation was 4.75±1.96D. Our results showed a significant relationship between age and amplitude of accommodation (r=-0.734, P<0.001). The mean anterior chamber depth was 3.19±0.33mm. The anterior chamber depth was also found to correlate with both age (r=-0.368, P<0.001) and amplitude of accommodation (r=0.399, P<0.001).
Conclusion: Aging effects on ocular parameters (keratometric power, axial length, and anterior chamber depth). Subjects with deep anterior chamber depth have slightly higher amplitude of accommodation.
Keywords: Presbyopia;Amplitude of accommodation;Biometric findings
Background
Accommodation of the eye defined as changes in the dioptric power of the eye to focus sharply on objects at a range of distances. The maximum potential increase in optical power of eye is known as the amplitude of accommodation [1]. Presbyopia is a progressive loss of the accommodative ability of the eye that occurs with aging [2]. It is one of the most visual impairment of later life in the world and there was approximately 1.8 billion people globally with presbyopia in 2015 [3]. It starts around age 40 and causes difficulties in reading and near work [4]. Uncorrected presbyopia has negative impacts on near vision‐related quality of life [5]. The most significant risk factor for presbyopia is age. Other factors are female sex, certain medical conditions (cardiovascular disease, anemia, diabetes, autoimmune disease, and eye trauma) and some drugs (antihistamines and antidepressants) [6]. People who have hypermetropia typically tend to experience the onset of presbyopia earlier than their emmetropic persons [7,8]. Also, there are large inter-individual differences in the accommodation ability for subjects of the same age [9]. We designed this study to assess aging changes of optical components including keratometric power, axial length, and anterior chamber depth (ACD) and possible effects of them on amplitude of accommodation.
Materials and Methods
Ethics statement
Our study was conducted by Student Research Committee, Shahid Beheshti University of Medical Sciences after approval by the Human Ethics Committee (number IR.SBMU.RETECH. REC.1398.676). Under the principles of Helsinki declaration and detailed explanation of the research, the consent form was received from all participants.
Patient selection
In present study, 295 persons aged between 33-52 years old from those coming to the eye clinic in Abhar, Iran were participated. They were healthy and without systemic and ophthalmic diseases. Exclusion criteria consisted of ocular diseases such as refractive errors, amblyopia, accommodative insufficiency, accommodative spasm, strabismus, pterygium, cataract, ptosis, glaucoma, and retinal and optic nerve disorders, and history of trauma to ocular surfaces and ocular surgery and systemic drug using.
Subjects examinations
In all participants slit lamp biomicroscopy, funduscopy, and measurement of visual acuity with ETDRS chart and axial length of the globe (ultrasound biomicroscopy with Alcon Ocuscan) performed. Objective refraction was performed by autorefractometer (Topcon Medical Systems, KR800) and refined by retinoscopy (Beta 200 Heine, Germany). Subjective refraction was performed by an experienced optometrist. Spherical equivalent (the numerical sum of the sphere power with half of the cylinder power) was considered as refractive errors of subjects. According to spherical equivalent (SE), all subjects were emmetropic refraction (SE between −0.50 to +0.5D). We measured amplitude of accommodation with the push up method. Push up method is the most common and simple test for routine measurement of amplitude of accommodation. Under standard illumination, each test was performed monocularly with optically corrected for distance vision. We explained the procedure to our subjects and asked them to view a 20/20 row of letters on a handheld reduced Snellen chart approaching the eye and states when there is ‘the first blur’. For each eye, it was assessed 2-3 times and average of findings was recorded as the final measurement. The measurement is converted to its reciprocal to provide the amplitude of accommodation in diopters [10].
Statistical analysis
In this study, right eyes of subjects were selected to statistical analysis. Our data was analyzed by SPSS software version 18 using one-way ANOVA, Kruskal-Wallis, and spearman’s correlation.
Results
This study performed on 295 persons (188 males and 107 females) with the mean age of 42.68±4.75 years with a range of 33 to 52 years. Best corrected visual acuity was 20/20 or better in all participants and there were no amblyopic patients. The mean spherical equivalent was 0.13±0.27D (from −0.50D to +0.50D) and did not correlate with age (r=0.095, P=0.104). The mean keratometric power was 44.03±1.51D (range of 40.0 to 48.0D). The mean keratometric power was 43.79±1.46D in men and it was 44.45±1.52D in women, and this difference was significant (P<0.001). There was a significant relationship between age and the mean keratometric power (r=0.164, P=0.006). The mean keratometric power showed an increase trend with aging. The mean axial length of eyes was 22.91±0.76mm (range of 21.10-24.91mm). The mean axial length was 23.06±0.74D in men and it was 22.70±0.74D in women, and this difference was a significant (P<0.001). The mean axial length was correlated with keratometric power (r=-0.727, P<0.001). Also, the mean axial length of eyes decreased with aging and there was a significant relationship between age and axial length (r=-0.165, P=0.019). The mean amplitude of accommodation was 4.75±1.96 D (range of 1.50-11.00D). The mean amplitude of accommodation was 5.05±2.05 D in men and 4.21±1.68 D in women, and it differed between them significantly (P=0.001). The amplitude of accommodation decreased with aging. Our findings showed a significant relationship between age and amplitude of accommodation (r=-0.734, P<0.001). Amplitude of accommodation had no correlation with both the keratometric power (r=-0.052, P=0.378) and the axial length (r=-0.073, P=0.309). Amplitude of accommodation showed a significant correlation with spherical equivalent (r=-0.111, P=0.049). According to age of subjects, we divided our subjects in five age groups: 32-36 years, 36-40 years, 40-44 years, 44-48 years, and 48-52 years. The mean amplitude of accommodation, keratometric power, axial length, and anterior chamber depth are presented in the (Table1).
Table 1:Optical parameters (mean±SD) of subjects in different age groups.
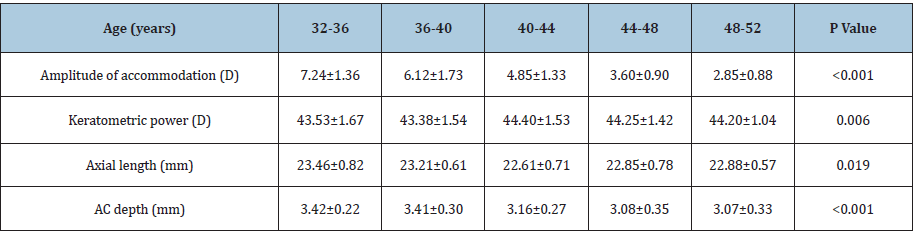
The mean anterior chamber depth was 3.19±0.33mm (range of 2.34-4.10mm). The mean anterior chamber depth was 3.25±0.32D in men and it was 3.10±0.34D in women, and there was a significant difference between them (P=0.002). The anterior chamber depth was also found to correlate inversely with patient age (r=-0.368, P<0.001). Moreover, there was a significant relationship between anterior chamber depth and amplitude of accommodation (r=0.399, P<0.001). When we divided each group into 5 groups according to anterior chamber depth 2.20-2.60, 2.60-3.00, 3.00-3.40, 3.40-3.80, and 3.80-4.20mm), the amplitude of accommodation was found to be directly related to subjects anterior chamber depth (Figures 1& 2).
Figure 1:Correlation plot of the amplitude of accommodation and different factors including: A: age, B: AC depth, C: axial length, and D: refraction.
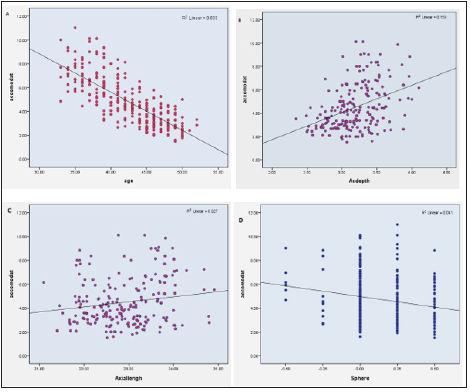
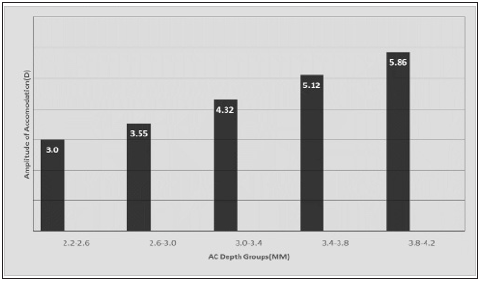
Figure 2:Amplitude of accommodation (mean±SD) in different anterior chamber depth groups.
Discussion
Presbyopia affects everyone, but sometimes it involves people younger than age 40 and conversely there are some older than age 45 without difficulty to focus on close objects [1-4]. In present study, we assessed aging changes of biometric parameters and effects of them on amplitude of accommodation in emmetropic subjects. Our results showed several changes in optical components of eyes with aging. While the corneal curvature was on the process of steepening but both of axial length and anterior chamber depth decreased with aging. These changes of refractive components prevent change of total refraction and develop a stable processes in emmetropia. Also, in subjects with elongated eye, cornea was flatter and in those with shorter eye, cornea was steeper. In agreement with our findings, several population-based studies showed similar results (increased keratometric power, and decreased axial length and anterior chamber depth, with aging) [11-15]. In our study, amplitude of accommodation showed significant correlation with age and anterior chamber depth. However, other ocular parameters including keratometric power and axial length had no correlation with amplitude of accommodation. Age-related changes in the lens and ciliary muscle dysfunction leads to decreased amplitude of accommodation [16]. Interestingly, anterior chamber depth had direct correlation with amplitude of accommodation. People with shallow anterior chamber depth showed lower amplitude of accommodation when compared with age-matched controls. In each age group, subjects with deep anterior chamber depth had more amplitude of accommodation. Amplitude of accommodation affected anterior chamber depth and should be considered when prescribing near glasses. Previous studies have shown myopic patients have deeper anterior chamber and presbyopic symptoms in myopia develop much later than emmetropia and hypermetropia [17-19].
The accommodative function result from a larger forward movement of the anterior lens surface and a small posterior movement of the posterior lens surface [20]. During accommodation, the lens becomes thicker and the anterior chamber do shallower along the polar axis [21]. In our idea, in eyes with deep anterior chamber, there are more distance between the cornea and crystalline lens. So crystalline lens has more space to forward movement of the lens and increased ability of accommodation. However, other studies showed no significant correlation between amplitude of accommodation and anterior chamber depth, axial length, and lens thickness [22,23]. Also, amplitude of accommodation of women was slightly lower than men. It might be correlated to anatomical differences between them (steeper keratometric power, shorter axial length, and shallower anterior chamber depth in women). In several population-based studies, similar results have reported [7,19,24,25]. We suggest further studies with more patients, especially assessment of other parameters like thickness and autofluorescence of the crystalline lens thickness and effects on accommodation.
Conclusion
Our study demonstrated age related changes in biometric parameters in normal eyes. With aging, axial length and anterior chamber depth decreased and the corneal curvature became steeper. In Our subjects, there were statistically significant correlation between amplitude of accommodation with age and anterior chamber depth. Subjects with deep anterior chamber depth have slightly higher amplitude of accommodation.
Acknowledgement
This study is related to the project NO 1398.255 from Student Research Committee, Shahid Beheshti University of Medical Sciences, Tehran, Iran. We also appreciate the “Student Research Committee” and “Research & Technology Chancellor” in Shahid Beheshti University of Medical Sciences for their financial support of this study.
References
- Sergienko NM, Nikonenko DP (2015) Measurement of amplitude of accommodation in young persons. Clin Exp Optom 98(4): 359-361.
- (2010) Care of the patient with presbyopia. St. Louis (MO): American Optometric Association, USA.
- Fricke TR, Tahhan N, Resnikoff S, Papas E, Burnett A, et al. (2018) Global prevalence of presbyopia and vision impairment from uncorrected presbyopia: Systematic review, meta-analysis, and modelling. Ophthalmology 125(10):1492-1499.
- Goertz AD, Stewart WC, Burns WR, Stewart JA, Nelson LA (2014) Review of the impact of presbyopia on quality of life in the developing and developed world. Acta Ophthalmol 92(6): 497-500.
- Patel I, West SK (2007) Presbyopia: prevalence, impact, and interventions. Community Eye Health 20(63): 40-41.
- http://www.mayoclinic.org/diseases-conditions/presbyopia/basics/causes/con-20032261.
- Nirmalan PK, Krishnaiah S, Shamanna BR, Rao GN, Thomas R (2006) A population-based assessment of presbyopia in the state of Andhra Pradesh, South India: The Andhra Pradesh Eye Disease Study. Invest Ophthalmol Vis Sci 47(6): 2324-2328.
- McBrien NA, Millodot M (1986) Amplitude of accommodation and refractive error. Invest Ophthalmol Vis Sci 27(7): 1187-1190.
- López Alcón D, Marín Franch I, Fernández Sánchez V, López Gil N (2017) Optical factors influencing the amplitude of accommodation. Vision Res 141: 16-22.
- Burns DH, Evans BJW, Allen PM (2014) Clinical measurement of amplitude of accommodation: A review. Optometry in Practice 15(3): 75-86.
- Hashemi H, Asgari S, Emamian MH, Mehravaran S, Fotouhi A (2015) Age-related changes in corneal curvature and shape: The shahroud eye cohort study. Cornea 34(11): 1456-1458.
- Fledelius HC, Stubgaard M (1986) Changes in refraction and corneal curvature during growth and adult life. A cross-sectional study. Acta Ophthalmol (Copenh) 64(5): 487-491.
- Cheon MH, Sung KR, Choi EH, Kang SY, Cho JW, et al. (2010) Effect of age on anterior chamber angle configuration in Asians determined by anterior segment optical coherence tomography; clinic-based study. Acta Ophthalmol 88(6): e205-e210.
- Bhardwaj V, Rajeshbhai GP (2013) Axial length, anterior chamber depth-a study in different age groups and refractive errors. J Clin Diagn Res 7(10): 2211-2212.
- Chen H, Lin H, Lin Z, Chen J, Chen W (2016) Distribution of axial length, anterior chamber depth, and corneal curvature in an aged population in South China. BMC Ophthalmol 16(47):1-7.
- Glasser A, Campbell MC (1998) Presbyopia and the optical changes in the human crystalline lens with age. Vision Res 38(2): 209-229.
- Abraham LM, Kuriakose T, Sivanandam V, Venkatesan N, Thomas R, et al. (2005) Amplitude of accommodation and its relation to refractive errors. Indian J Ophthalmol 53(2): 105-108.
- Hosny M, Alio JL, Claramonte P, Attia WH, Perez Santonja JJ (2000) Relationship between anterior chamber depth, refractive state, corneal diameter, and axial length. J Refract Surg 16(3): 336-340.
- Kato K, Kondo M, Takeuchi M, Hirano k (2019) Refractive error and biometrics of anterior segment of eyes of healthy young university students in Japan. Sci Rep 9: 1-7.
- Charman WN (2008) The eye in focus: Accommodation and presbyopia. Clin Exp Optom 91(3): 207-25.
- Koretz JF, Cook CA, Kaufman PL (1997) Accommodation and presbyopia in the human eye. Changes in the anterior segment and crystalline lens with focus. Invest Ophthalmol Vis Sci 38(3): 569-578.
- Faramarzi A, Bagheri A, Karimian F, Shaianfar H, Razzaghi MR, et al. (2015) Correlation between ocular biometry and amplitude of accommodation in early presbyopia. Eur J Ophthalmol 25(4): 298-301.
- Abraham LM, Kuriakose T, Sivanandam V, Venkatesan N, Thomas R, et al. (2010) Correlation between ocular parameters and amplitude of accommodation. Indian J Ophthalmol 58(6): 483-485.
- Sng CC, Foo LL, Cheng CY, Allen JC, He M, et al. (2012) Determinants of anterior chamber depth: The Singapore Chinese Eye Study. Ophthalmology 119(6): 1143-1150.
- Zocher MT, Rozema JJ, Oertel N, Dawczynski J, Wiedemann P, et al. (2016) Biometry and visual function of a healthy cohort in Leipzig, Germany. BMC Ophthalmol 16(79): 1-20.
© 2020 Shahrokh Ramin. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






