- Submissions

Full Text
Medical & Surgical Ophthalmology Research
Minor Surgery Program in a Health Centre
Antonio Masiá Alegre1* and Concepción Fernández-Pacheco2
1Medical specialist in Family and Community Medicine, Guillem de Castro Health Center, Spain
2Department of Nursing, Guillem de Castro Health Centre, Spain
*Corresponding author: Antonio Masiá Alegre, Medical specialist in Family and Community Medicine, Primary Care Team (EAP), Guillem de Castro Health Centre, Valencia, Spain; Email: amasiaalegre@gmail.com
Submission: December 21, 2017; Published: February 21, 2018

ISSN: 2578-0360 Volume1 Issue4
Introduction
Defined, agreed upon and even legislated in the field of primary care, why is minor surgery not a usual practice in the first level of health care? [1] We will talk about "rescuing” a family doctor's own practice and coordinating it with specialized attention to work as a team, without forgetting the important participation of nursing, looking for the quality of care and the improvement of work activity together with the satisfaction of both the user and of the professional.
Continuous training, adequate infrastructure and motivation of professionals are key. Finally, patient-medical motivation and satisfaction do not justify minor surgery on their own in primary care, but together with a precise surgical indication, safe and necessary practice, coordination with specialized care, plus scientific endorsement of what has been done and published. Until now, in addition to administrative support, they are real variables for its development and implementation [2]. Perhaps the medical super-specialization and the overloaded work schedule are two of the many reasons that have led to the practice of minor surgery in primary care reduced to simple sutures of injuries by nursing in most cases ... And It Is Not Like That
Our Experience
The EAP of the Guillem de Castro Health Centre is located in Valencia, belongs to the Department of Health 9 and has an assigned population of 27000 inhabitants. It has as reference centres the Integrated Sanitary Centre (C.S.I) of Juan Liorens at 1500 m and the General University Hospital of Valencia at about 1900 m. In 2008, the protocol of the minor surgery program in primary care was presented to the Medical Directorate of the Department of Health. Subsequently, a meeting was convened, both to the nursing staff and to the physicians of the centre, with the assistance of the Head of the Surgery Service of the reference hospital and a surgeon responsible for outpatient surgery, for the presentation of the program.
By having an operating theatre in the specialty centre, already used in morning and afternoon hours by different medical-surgical specialists, it was proposed to create a minor surgery agenda to start the activity in January 2009 by a family doctor and a nurse from the health centre and in the same operating room at the specialty centre. At the moment the operating room is available one afternoon a month. Currently a family doctor and a nurse of the health centre and an assistant of the centre of specialties, work in this program, circumscribing at the moment only to the patients belonging to the health centre. The collection of patients is carried out by the family doctors of the health centre, who refer to the agenda of the referring family doctor along with two forms: the preoperative assessment and the information-consent form for the patient to sign. Former.
Table 1:
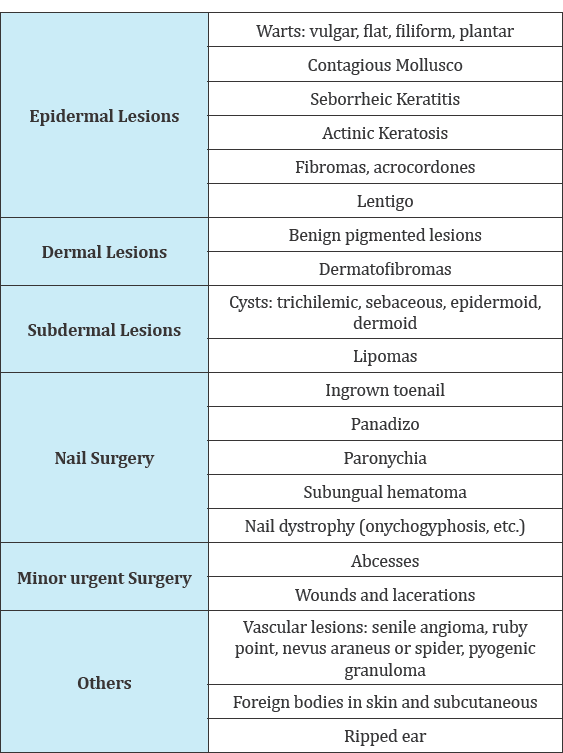
Table 2:

Table 3:
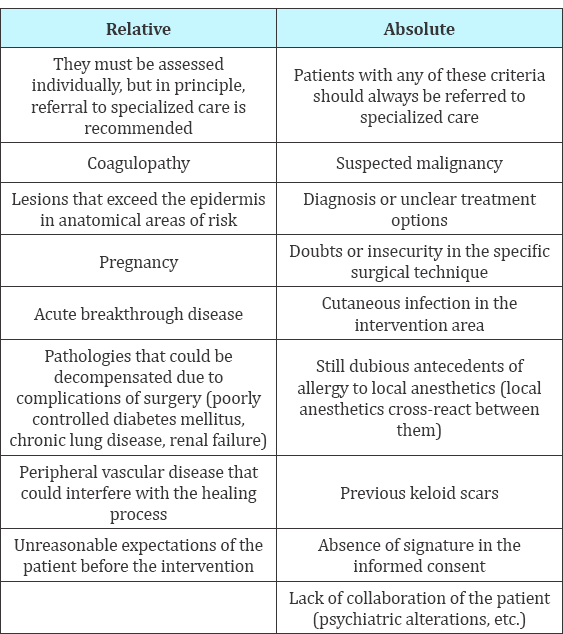
Specifies the pathologies included in the program and Table 2 [4] includes the inclusion criteria (Table 1)[3]. Regarding the exclusion criteria (Table 3) [4] it is important to take into account a series of fundamental premises before performing any surgical action in primary care:
a) Knowledge of the lesion to be treated and its natural history
b) Defined need for surgical treatment
c) Knowledge of the election procedure
d) Mastery of your surgical technique
e) Availability of an appropriate instrumental endowment
Absence of formal contra indications for minor surgery in primary care [5]. If the above requirements are not fulfilled or when the mere suspicion of malignant pathology is suspected, the patient should be referred to specialized assistance without delay. Once the patient is referred, the family doctor cites the patient in his / her diary, confirms the indication of inclusion to the program or refers to specialized care in his / her case, verifies the existence of documents and appointment for the intervention that will take place on the day indicated in him.
Operating Room of the Specialty Centre
Currently one afternoon is available per month of the operating room, by faxing, one week before the surgical appointment, to the head of the surgical program of the specialty centre the list of patients with the following information: name and surnames, System of Population Information (SIP) and diagnosis. The number of interventions per evening is 10-15. On the day of the surgery and before the surgery, the nurse and the doctor contact and explore the patient, clarifying any type of question and / or question.
After the intervention and referral ofthe samples to pathological anatomy and / or microbiology of the hospital, the patient is given an information and advice sheet, contact telephone number and appointment with the nurse in 48-72 h. Nursing follows up with regard to care and assessment of possible complications. A medical appointment is made at approximately 30 days for definitive discharge and delivery of pathological anatomy, whose computerized result is provided by the corresponding service of the reference hospital. The surgical techniques that are used are the following: [6]
1) Tangential excision (shaving and curettage)
2) Cylindrical excision (punch)
3) Fusiform excision of superficial lesions
4) Removal (exeresis) of dermal and sub dermal lesions
5) Cryosurgery
6) Electro surgery
7) Minor nail surgery
8) Incision-drainage of abscesses
Results
Since January 2009, the month in which we started the activity, we have operated on 600 patients, the most treated pathology being epidermal inclusion cysts, lipomas and abscesses. So far, as complications there have been only five seromas and two sutured wound infections. The preliminary results that we have at the moment show a high degree of patient satisfaction (Figure 1-3).
Figure 1

Figure 2
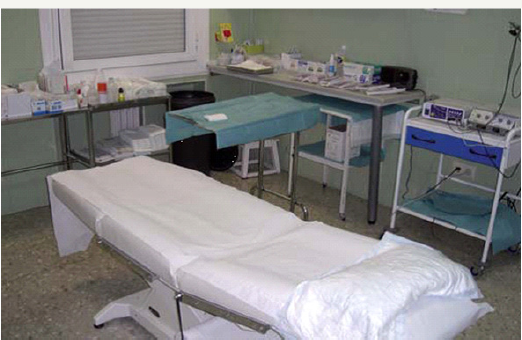
Figure 3

Discussion
We do not want to compare ourselves with surgeons, because we are not and because our daily activity is broader, but we can go back to the minor surgical plot that can be done in the field of family medicine, and should be part of the pre-graduated training and the residence. Without forgetting, of course, our fellow dermatologists with whom practical and real coordination is essential. We want to emphasize the idea of "teamwork”, and therefore highlight the important role of auxiliary and nursing in this activity, not only in the aspect of cleanliness, patient management in the waiting room, surgical assistantship, preparation of the field, cures, vaccination, etc. but also in the contact, follow-up and subsequent control of the patient.
We would miss the truth if only with enthusiasm we would like to develop the minor surgery, agreeing fully that it is fundamental, as in any other activity, a regulated and continuous training [7]. Family doctors and nurses, according to the inclusion and exclusion criteria defined, the type of injuries and procedures to be performed, and contraindications to know what to refer to specialized care, can and should undergo minor surgery. If you train and like this activity, we invite you to do it.
Conclusions
Minor surgery in primary care allows to decrease the waiting time, increasing patient satisfaction based on greater accessibility to the family doctor, without forgetting that we are not surgeons and therefore the program should achieve an improvement of the coordination with the medical-surgical specialties and propose a training system for primary care professionals.
Summary
Located the Minor Surgery (CM) in the field of Primary Care (PC) and with the accent placed on the concept of "teamwork”, we see how the most frequent pathologies performed since the beginning of the program have been:
a) Epidermal cysts
b) Lipomas
c) Fibromas
d) Nevus
e) Walking
f) Lear lobe ear
Regarding the most used surgical techniques we have:
l. Fifiform decision
2. Cylindrical selection (punch)
3. Tangential decision (shaving and curettage)
4. Exéresis
5. Sewer system
The correlation between the presurgical diagnosis and the antimopathological result was 68%, reducing the number of postoperative complications to 7 (5 seromas and 2 sutured wound infections). Thus, the CM is an activity of "added value" present in the portfolio of services of the PA, enhances the relationship of nursing and the family doctor to the patient, decreases the derivations to speciality, reduces costs and waiting lists, improving the access and the resolution capacity of the PA in these processes.
References
- Ministry of Health (2000) Portfolio of Primary Care services in the Valencian Community. Valencia, Spain.
- Royal Decree 63/95 on the adaptation of health benefits of the National Health System, London.
- Procedure guide in AP. Conselleria de Sanitat (Generalitat Valenciana), Spain.
- Arrivals JM, GdT (2003) Minor surgery and procedures in MF. Jarpyo editors, Madrid, Spain.
- Zurro AM, Pérez JFC (2003) Primary care Concepts, organization and clinical practice. Elsevier, Madrid, Netherlands.
- Márquez ARR, Temprano JMF, Hermoso IF, Guerrero JCV (2008) Manual of CM in AP. Ergon, Madrid, Australia.
- Training program in CM in AP (2002) Theoretical-practical workshop in person and distance. Teaching group Procedures and technologies in PA, USA.
© 2018 Antonio Masiá Alegre, et al. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






