- Submissions

Full Text
Modern Research in Dentistry
The Global Decline in the Use of Dental Amalgam Restorations
Omar El Mowafy1* and Nora El Mowafy2
1Professor in Restorative Dentistry, Canada
2Associate in Dentistry, Canada
*Corresponding author: Omar El Mowafy, BDS, PhD, FADM, Professor in Restorative Dentistry, Director of the International Dentist Advanced Placement Program, Faculty of Dentistry, University of Toronto, 124 Edward Street, Toronto, Ontario M5G 1G6, Canada
Submission: December 03, 2019;Published: December 10, 2019

ISSN:2637-7764Volume4 Issue4
Introduction
When posterior teeth, premolars and molars, develop significant carious lesions, they need to be treated through caries removal and placement of restorations. Currently, there are two widely used direct restorative materials, amalgam and resin composite, that are used by dentists globally for this purpose. However, over the last decade there has been a significant increase in the utilization of resin composite restorations on the expense of amalgam. A number of reasons led to this trend. While amalgam has been utilized by the profession as a long-lasting direct restorative material for over a century [1], however, recently there have been several concerns about its mercury content, color and restoration failures. While some amalgam restorations maintain their shiny silver appearance over the years (Figure 1), others undergo significant corrosion [2] with subsequent darkening of the restoration (Figure 2). Furthermore, the fact that there is a viable competitor, resin composite, that matches the natural color of the teeth, is a good reason for the shift. The majority of young adults of the current generation prefer to have their teeth restored with indistinguishable materials. Therefore, esthetics are a major driving force in this respect. Resin composite restorations can match the natural color of the teeth with a high level of accuracy (Figure 3). There use by dentists in North America has been constantly on the rise [3,4].
Figure 1: Large amalgam restorations on mandibular molars. These were polished well and retained their surface lustre over time
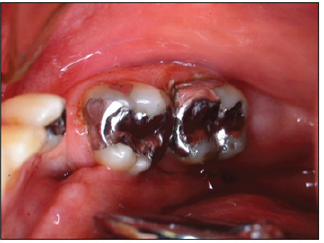
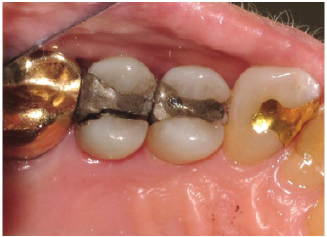
Figure 2: This maxillary molar has a mesio-occluso-lingual amalgam restoration that suffered from corrosion resulting in unsightly appearance. Perhaps the alloy from which this restoration was made is to blame for the outcome
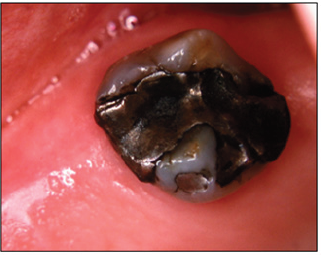
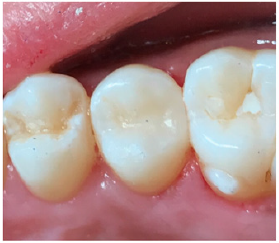
Figure 3: This maxillary second premolar has a disto-occlusal resin composite restoration that is indistinguishable due to optimal color matching
Amalgam and mercury
Dental amalgam restorations are made through mixing of an alloy powder primarily made of silver, copper and tin with liquid mercury at a ratio of 1:1 [5]. The resultant plastic mix is condensed into the prepared cavity before setting begins. Therefore, amalgam restorations have a 50% mercury content, however, in a reacted form. Mercury has been also used in several industries other than dentistry including paper mills, medical appliances as in thermometers, barometers, electrical equipment, dry batteries, semi-conductors and in paints. Recently, there has been global environmental concerns about the use of mercury in these industries. This led regulatory bodies in many parts of the world to require a number of industries to eliminate mercury, a heavy metal, from their products. This included the paints industry and manufacturers of dry batteries. In the dental profession, regulatory bodies in North America required all dental treatment facilities to have in place a special device, mercury separator, to collect elemental mercury from dental amalgam remnants as they pass through the wastewater lines. Furthermore, in 2008 in Norway, the use of amalgam restorations has been phased out [6,7]. A similar situation existed in Sweden and Denmark, while Germany has restricted the use of amalgam. In 2009, Health Canada has recommended that dentists should not place or remove amalgam restorations from the teeth of the pregnant women [8].
Amalgam failures
Amalgam restorations failures also played a role as a significant factor in the decline of their use [9]. Amalgam restorations may fail due to recurrent caries that occurs around the restoration margins (Figure 4). Another typical scenario for failure of Class 2 amalgam restorations is isthmus fracture (Figure 5). This can be caused by a variety of reasons that include: shallow cavity preparation, sharp internal lineangles and recurrent caries underneath. Furthermore, failure of amalgam restorations can be also manifested in the form of tooth fracture (Figure 6). This can be predisposed by preparing the amalgam cavities with sharp rather than rounded internal lineangles. Sharp internal lineagles tend to cause stress concentration during function with subsequent fatigue and ultimately fracture of a cusp on the long term. Special burrs with rounded corners that are pear-shaped can be useful in helping the dentist produce cavities with rounded internal lineangles. When severe, tooth fracture may render the tooth non-restorable (Figure 7). The risk of tooth fracture can be reduced when amalgam restorations are bonded to the tooth structure rather than being inserted as mere passive obturators.
Figure 4: A mesio-occlusal restoration on a mandibular first molar with evidence of recurrent caries at the gingival-buccal margin of the proximal area

Figure 5: Isthmus fracture of a mesio-occlusal amalgam restoration on a maxillary first molar.
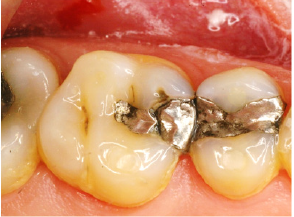
Figure 6: This maxillary second premolar had an mesio-occluso-distal amalgam restoration that resulted in fracture of the lingual cusp
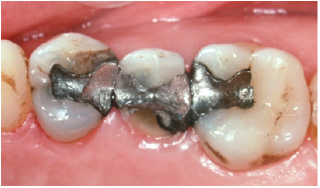
Figure 7: This maxillary second premolar had a mesio-occluso-distal amalgam restoration which caused the lingual cusp to fracture off. Because the fracture line extended subgingivally, the tooth was deemed as non-restorable and had to be extracted.
This shift in utilization of amalgam to resin composite is not surprising since change due to new technological advancements is inevitable in the dental profession. For example, over that last decade in North America, there has been a shift towards digital radiography and the archaic X-ray films with their developer and fixer solutions have quickly become obsolete. In the dental laboratory, there has been a shift towards the new technology of CAD-CAD designing and milling for fabrication of crowns, bridges and implant components. Simultaneously, the use of the aged lostwax technique is gradually declining. In a recent statistical report from the largest dental laboratory in the USA, 90% of all crowns that dentists in the USA prescribed were made out of non-metallic materials using the CAD-CAM technology, mainly glass-ceramic and zirconia. The remaining 10% were either cast gold or the traditional porcelain-fused -to-metal crowns.
Conclusion
In conclusion, it is not unexpected that the utilization of dental amalgam as a direct restorative material has dwindled and will continue to do so particularly when considering the fact that the dental profession has a mercury-free competitor, resin composite, that is capable of replacing dental amalgam with better tooth color matching abilities. In view of the global environmental concerns about mercury in dental amalgam, survival of amalgam as a direct restorative material is doomed.
References
- Black GV (1896) The physical properties of the silver-tin amalgams. Dental Cosmos 38: 965-992.
- Guthrom CE, Johnson LD, Lawless KR (1983) Corrosion of dental amalgam and its phases. J Dent Res46(6): 1372-1381.
- Leinfelder K (2004) The enigma of dental amalgam. J Esthet Restor Dent 16(1): 3-5.
- Christensen GJ (2010) Should resin-based composite dominate restorative dentistry today? J Am Dent Assoc 141(12): 1490-1493.
- (1895) Characters of filling materials. The Dental Cosmos 37: 553-561.
- Klif (2010a) Norwegian action plan for reducing mercury releases-TA 2731, Norwegian Climate and Pollution Agency, Oslo, Norway.
- (2012) Review of Norwegian experiences with the phase-out of dental amalgam use. Noregian Climate and Pollution Agency. TA 2946, Oslo, Norway.
- (2009) Government of Canada-medical devices. The safety of Dental Amalgam.
- Harris RK (1992) Dental amalgam: success or failure? Oper Dent 17(6): 243-252.
© 2019 Omar El Mowafy. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






