- Submissions

Full Text
Innovation in Tissue Engineering & Regenerative Medicine
Neuronal Regeneration Potential of Facial Nerve for Compound Wound in an Elderly Patient
S Cox1, R Hossain2, SGJ Ng2, M Mani1 and EK Tan1*
1Department of Plastic Surgery, New Zealand
2Department of Ophthalmology, New Zealand
*Corresponding author:EK Tan, Department of Plastic Surgery, New Zealand
Submission: January 12, 2021;Published: January 28, 2021

Volume1 Issue4January, 2021
Introduction
The capacity of axonal regeneration and reinnervation in peripheral nerves are maintained
throughout life but tends to be delayed and less effective with aging [1]. In complex and
compound facial wounds, specifically where significant contamination and soft tissue loss is
ensued, it can be a dilemma to decide between performing staged reconstruction of an injured
facial nerve against primary repair especially in cases of heavily contused and/or divided
facial nerve at multiple levels. We wish to share our experience of performing primary repair
of facial nerve’s branches in a compound facial wound with underlying fracture in a 70-yearold
male patient. A significant recovery of all 5 branches of his facial nerve was observed 21
weeks after surgery.
We would advocate primary repair of a severely injured facial nerve in an older patient
with a complex compound facial as a preferred option whenever deemed clinically possible
as it can potentially yield good clinical outcomes and remove the need for further staged
revisional surgery.
Background
A 70-year-old man presented to the Emergency Department (ED) within two hours of
sustaining an equine related facial wound. He remembered being kicked in the right side of
his face and developed a complex compound facial wound. The wound extended from his
right nasolabial superiorly to his right outer canthus. His Glasgow Coma Score (GCS) was
15/15. His past medical history included significant ischaemic heart disease with an ejection
fraction of 52% after an angioplasty nine years previously. A pan Computed Tomography (CT)
revealed a right zygomatic body, infraorbital rim and parasymphisis fractures of the mandible
but no other concomitant injury beyond his head. His right eye visual acuity was limited
to counting fingers. His right pupil was fixed and dilated, and the intraocular pressure was
measured at 50mmHg. He underwent an emergency canthotomy & cantholysis to decompress
the orbit, which improved the intraocular pressure to 25mmHg.
He was attended by Maxillofacial team for emergency wound exploration, washout and
internal fixation of his facial fractures. All his facial nerve branches were identified as divided
within the wound and the on-call Plastic Surgery team was contacted. On upon further
exploration, there was segmental loss of the zygomatic branch of facial nerve including the
distal end. Branches to orbicularis oculi, risorius and main trunk of buccal branch were 100%
divided; however, both proximal and distal ends were identified, albeit heavily contused.
The zygomatic branch was placed within zygomaticus major muscle substance and
primary repair of other branches with 8’0 and 9’0 Ethilon were performed with minimal
tension across repair sites where possible. A single drain was inserted into wound bed and
overlying skin was closed with 5’0 Prolene. The drain was removed five days post-surgery and
skin sutures removed seven days later. On week 21 post surgery, he was reviewed in Plastic
Surgery Outpatients and observed to have adequate dynamic upper eyelid closure of his right
eye and function of the buccal branch of the facial nerve. There was a mild ectropion of his
right lower eyelid and he was listed for revisional lateral tarsorraphy.
Patient expressed satisfaction with his facial symmetry both at rest and on animation
(Figure 1-4).
Figure 1:Pre-operative 3D CT of facial injury (left) and post fixation (right).

Figure 2:5 months post-surgery.

Figure 3: Eye opening (left) and ability for full closure (right) 5 months post-surgery showing functional orbicularis oculi.
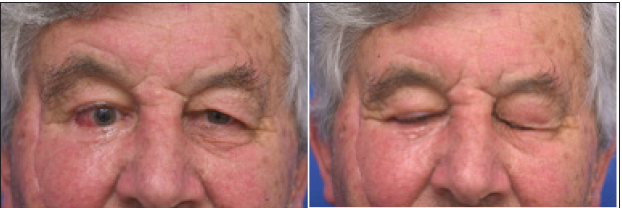
Figure 4: Cheeks at resting (left) and puffing out (right) 5 months post-surgery showing functional buccal branch of facial nerve.

Discussion
Peripheral nerve regeneration growth is around 1mm/day
and is affected by a variety of different variables [2]. In order to
reconstruct a peripheral nerve, there needs to be a stable skeletal
framework, coverage of soft tissue over the nerve, an end organ
to innervate as well as no infection [3,4]. Poor prognosis of nerve
regeneration is associated with advancing age, more proximal
injuries, delayed repair, scarring, smoking, nerve repair under
tension, crush injuries with associated bony and soft tissue injury,
and medical comorbidities such as diabetes, hypothyroidism
and peripheral vascular disease [4,5]. Direct end to end repair of
traumatically injured nerves has been found to be associated with
better functional outcomes than other surgical techniques such
as end to side, conduit or grafting options.4 Despite attempts to
improve functional outcomes of peripheral nerve repairs, there has
been little improvement over the last 50 years; in part due to relates
to difficulties conducting RCT’s and also lack of understanding basic
human biology of nerve regeneration [6,7].
Advancing age is correlated with poorer outcomes of nerve
regeneration, much of this is thought to be associated with reduced
“robust regenerative response” but largely poorly understood
[4,5]. The term advancing age defined as 65 years and older based
on chronological age and socioeconomic constructs is not in itself
a homogenous group due to difference in genetics, lifestyle and
health. In this case, there was significant contamination of the
wound bed from the traumatic nature of the injury and the options
considered with regards to his facial nerve injury at the time of
surgery were:
1. Immediate direct repair of all nerve branches with burying
of the proximal end of nerve that has distal segmental loss
directly into muscle.
2. Delayed primary repair of the nerve within 72 hours following
further wound irrigation.
3. Staged reanimation of his facial nerve after patient has
recovered from the acute injury.
There are distinct advantages and disadvantages with all of
these options. For example, the first option is associated with
highest chance of nerve regeneration potential with reduced need
to return to theatre for surgery of the facial nerve, but high risk
of inherent wound infection associated with presence of suture
materials. A review of literature revealed no obvious universally
accepted gold standard in the situation of the current case. Many
centers managing such injuries have caseloads of two per year,
making long term follow-up and statistically analysis challenging.
Repair within 24 hours and 72 hours were advocated in separate
centers [8-10]. Two centers reported no difference in technical
methods used for nerve repair but one included nerve injury in
oncological setting instead of acute trauma [7,8].
Conclusion
The management of facial nerve injury in a compound facial wound can be challenging in an elderly patient and there is limited evidence to support different approaches. Our experience suggests that whenever possible, repair/reconstruction of the facial nerve in elderly patients is a worthwhile consideration that can produce a clinical good outcomes in protection of the eye and restoration of facial symmetry.
References
- Verdu E, Ceballow D, Vilches J, Navarro X (2000) Influence of aging on peripheral nerve function and regeneration. J Peri Ner Sys 5(4): 191-208.
- Gordon T (2016) Nerve regeneration: Understanding biology and its influence on return of function after nerve transfers. Hand Clinics 32(2): 103-117.
- Geissler J, Stevanovic M (2019) Management of large peripheral nerve defects with autografting. Injury 50(5): S64-S67.
- Palispis WA, Gupta R (2017) Surgical repair in humans after traumatic nerve injury provides limited functional neural regeneration in adults. Experimental neurology 290: 106-114.
- Socolovsky M, Rasulic L, Midha R (2017) Manual of peripheral nerve surgery: From the basics to complex procedures. Thieme.
- Brown S, Isaacson B, Kutz W, Barnett S, Rozen SM (2019) Facial nerve trauma: Clinical evaluation and management strategies. Plastic and reconstructive surgery 143(5): 1498-1512.
- Sánchez OM, Gavilán J, Penarrocha J, González OT, Moraleda S, et al. (2019) Facial nerve repair: The impact of technical variations on the final outcome. European Archives of Otorhinolaryngology 276(12): 3301-3308.
- Frijters E, Hofer SO, Mureau MA (2008) Long-term subjective and objective outcome after primary repair of traumatic facial nerve injuries. Annals of plastic surgery 61(2): 181-187.
- Matsuda K, Kakibuchi M, Sotsuka Y, Kubo T, Shibata M, et al. (2015) End-to-side “loop” graft for total facial nerve reconstruction: Over 10 years’ experience. Journal of Plastic Reconstructive & Aesthetic Surgery 68(8): 1054-1063.
- Hu M, Xiao H, Niu Y, Liu H, Zhang L (2016) Long-term follow-up of the repair of the multiple-branch facial nerve defect using acellular nerve allograft. Journal of Oral and Maxillofacial Surgery 74(1): e1-e11.
© 2021 EK Tan. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






