- Submissions

Full Text
Gerontology & Geriatrics Studies
Evidence for Completion of Home Modifications for Decrease in Risk of Falls and Preservation of Autonomy
Hassan Izzeddin Sarsak
Department of Occupational Therapy, School of Rehabilitation Sciences, University of Jordan, Saudi Arabia
*Corresponding author: Hassan Izzeddin Sarsak, Department of Occupational Therapy, Batterjee Medical College, Jeddah, KSA, Saudi Arabia
Submission: October 10, 2018;Published: October 29, 2018

ISSN 2578-0093Volume4 Issue1
Abstract
Objectives: To review current literature on home modifications related to decreasing risk of falls and/or impact on autonomy to support best practice methods.
Results: Our review revealed three studies suggesting that for community dwelling older adults aged 65 years and older, a home modification intervention may decrease risk for falls and maintain autonomy.
Conclusion: Home modifications are effective and may reduce the risk of falling and maintain autonomy in older adults.
Keywords: Home modification; Risk of fall; Autonomy; Older adults; Activities of daily living; Occupational therapy; Randomized controlled trail
Introduction
Within the community dwelling population about 1/4-1/3 of persons aged 65-79 fall every year. Persons aged >80 years have about 1/2 fall every year Nikolaus & Bach [1]. More than 1/2 of the persons who have experienced a fall will have multiple episodes a year. Falls can result in loss of independence of activities of daily living (ADLs) Pardessus et al. [2]. Home modifications are utilized by occupational therapists (OTs) to provide environmental changes to remove hazards which can cause falls [3,4]. Effectiveness of home modifications has been debated. Risk for falls is an imbalance between the patient’s autonomy and environmental hazards [2-5]. The purpose of this study was to review current literature on home modifications related to decreasing risk of falls and/or impact on autonomy to support best practice methods. For the purpose of this study, we created a clinical/research PICO question (Population, Intervention, Comparison, and Outcome), a key to evidence-based decision [6]. The PICO formed for our study is as follows:
(P): For community dwelling older adults aged 65 years and older
(I): Does a home modification intervention
(C): No comparison
(O): Decrease risk for falls and/or impact autonomy?
Methods
Review of literature and search strategy
A research has been made in the following databases: Ovid, CINAHL, and PubMed. Keywords and Search items used to search articles for our study were home modification, risk of fall, autonomy, older adults, activities of daily living, occupational therapy, randomized controlled trail. By combining the search results, we found articles on home modifications for decrease in risk of falls and preservation of autonomy. Based on the format of PICO question, three most relevant articles were selected for our study. Studies cited in the reference of the three articles along with other articles were also used to collect important information. After all, the strongest evidence-based article was chosen based on level of evidence and significance level to highlight and confirm our results and conclusions.
Results
Table 1:A summary of Reviewed Articles in Relation to our PICO.

The three selected articles were related to the effectiveness of home modifications for decrease in risk of falls and preservation of autonomy. All articles were related to our PICO question. A summary of the three articles in relation to our PICO is presented (Table 1).
Discussion
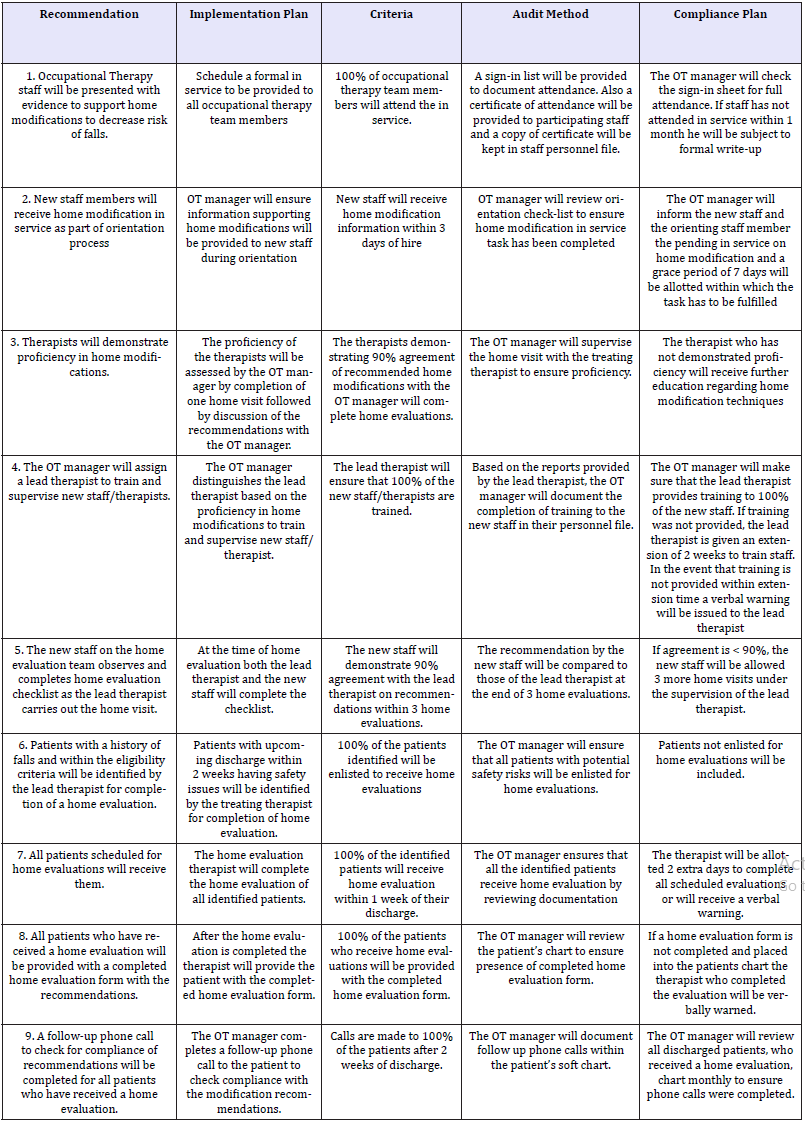
Cumming et al. [5] which examined the effectiveness of home modifications for decrease in risk of falls was selected as the strongest evidence-based article. Based on the hierarchy of levels of evidence in evidence-based practice, this study was a level II (Evidence obtained from at least one well designed RCT) [7]. They used a large sample size of 530 subjects. The intervention group (n=264) received home visits from an occupational therapist (OT), provided with a list of recommended home modifications, and further home visits were also provided if needed. Phone calls were made to encourage compliance with modifications, and a completion of monthly falls calendar was conducted. In the control group (n=266), no home visits were provided, and a completion of monthly falls calendar was conducted. In this study, the number of falls between intervention group (226) and control group (324) was not statistically significant. For subjects who experienced >1 fall in follow up period there was a reduction in risk of falling by 19% (p=.05). For subjects with a history of falls, there was a reduction in risk of falling in the intervention group by 36% (p=.001). For subjects with no history of falls the reduction in risk of falling was not significant. Evidence for decrease in risk of falls was supported by Cumming et al. [5]. In addition, evidence for preservation of autonomy was supported by Pardessus et al. [2]. Home modifications can be effective for decreasing the risk of falls and maintaining autonomy amongst community dwelling older adults. Thus, the following plan has been developed in our study and can be executed in clinics to ensure implementation of recommendations on home modifications for individuals with a history of falls who plan to return home (Table 2).
Table 2:A summary of recommendations, plan, and audit tool.
Conclusion
Our review suggested that home modifications are effective and may reduce the risk of falling and preserve autonomy in older adults. Thus, clinical guidelines, recommendations, a plan and audit tool have been created in our study to implement home modifications in clinics. The clinical guidelines for recommended intervention, the plan, and the audit tool recommend therapists to apply home modifications with older adults who are at risk of falls.
Funding details
No funding was required.
Acknowledgement
None.
Conflict of interest
Author declares that there is no conflict of interest.
References
- Nikolaus T, Bach M (2003) Preventing falls in community-dwelling frail older people using a Home Intervention Team (HIT): Results from the randomized falls-HIT trial. Journal of the American Geriatrics Society 51(3): 300-305.
- Pardessus V, Puisieux F, Di Pompeo C, Gaudefroy C, Thevenon A, et al. (2002) Benefits of home visits for fall and autonomy in the elderly: A randomized trial study. American Journal of Physical Medicine & Rehabilitation 81(4): 247-252.
- Rao SS (2005) Prevention of falls in older patients. American Family Physician 72(1): 81-88.
- Wyman JF, Croghan CF, Nachreiner NM, Gross CR, Stock HH, et al. (2007) Effectiveness of education and individualized counseling in reducing hazards in community-dwelling older women. Journal of the American Geriatrics Society 55(10): 1548-1556.
- Cumming RG, Thomas M, Szonyi G, Salkeld G, O’Neill E, et al. (1999) Home visits by an occupational therapist for assessment and modification of environmental hazards: A randomized trial of falls prevention. Journal of the American Geriatrics Society 47(12): 1397-1402.
- Richardson WS, Wilson MC, Nishikawa J, Hayward RS (1995) The wellbuilt clinical question: A key to evidence-based decision. ACP Journal Club 123(3): A12-A13.
- Hughes I (2006) Action research in healthcare: What is the evidence? ALAR Journal 11(1): 29-39.
© 2018Hassan Izzeddin Sarsak. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






