- Submissions

Full Text
Experimental Techniques in Urology & Nephrology
Post Traumatic Urethral Stricture in a Girl: A Case Report
Lissoune Cissé, Mohamed Jalloh*, Medina Ndoye, Youssef Belamine, Abdourahmane Diallo, Mouhamadou M Mbodji, Oumar Gaye, Ayun Cassell, Ngor M Thiam, Issa Labou, Lamine Niang and Serigne Gueye
Hospital General Idrissa Pouye and Cheikh Anta Diop University of Dakar, Senegal
*Corresponding author: Mohamed Jalloh, Urology Department, Hospital General Idrissa Pouye BP: 3270, Dakar, Senegal
Submission: December 18, 2020;Published: February 12, 2021
ISSN 2578-0395Volume3 Issue3
Abstract
Introduction: Urethral trauma is rare in girls and its management is difficult and not classified. We report the case of a transection of the urethra.
Case: The authors report a case of a complete transection of the urethra in an 8-year-old girl following a road traffic accident, in which a complex pelvic fracture, a large thigh wound, vaginal and rectal lesion were noted. A suprapubic catheter was put in place because a urinary retention. The patient later presented with multiple urinary tract infections that were treated with antibiotics. The urethral injury was repaired 22 months after the accident. An anastomotic urethroplasty was performed. The outcome was satisfactory with a good urine stream and urinary continence.
Conclusion: Clinical assessment for a urethral lesion must be systematic for girls following pelvic trauma or vaginal injury. Cystoscopy can help diagnose urethral lesion. The best treatment is the anastomotic urethroplasty
Keywords: Cystoscopy;Girl;Pelvic fracture;Urethral trauma; Vaginal laceration
Introduction
Urethral trauma is rare in girls [1]. They often occur because of high energy trauma and frequently associated with pelvic trauma [2,3]. The urethral lesions may vary from contusion to a complete section of the urethra [4]. The treatment options are not well classified for girls [5]. The classic management for boys that entails leaving a suprapubic catheter in place followed by delay urethral repair, is not ideal for girls because it compromises the outcome of the urethral reconstruction later on [1]. Some authors suggest a management immediately after the urethral trauma in girls [1,3]. We report a case of an 8-year-old patient, who presented at our department for a previously poorly managed urethral stenosis from a urethral injury that occurred 2 years earlier during a road traffic accident.
Observation
An 8-year-old girl presented with a history of an auto-pedestrian road traffic accident
in June 2018 during which she was ran over by a truck. She presented a peri-rectal and
retroperitoneal hematoma, a left perineal hematoma, a complex pelvic fracture, anal and
vaginal wound, and a large wound on the external part of the thigh. She was hospitalized in an
urban hospital, and during that hospitalization she presented with an acute urinary retention
managed by a cystostomy 7 days after the accident. The pelvic fractures were managed by
functional treatment. The wound was treated with skin grafts. She presented recurrent
urinary tract infections managed by antibiotics according to antiprograms. She was referred
to our department 22 months after the accident.
Physical examination showed a patient in good health condition, a tenderness along
the left lumbar fossa and a suprapubic catheter in place draining clear urine. Voiding
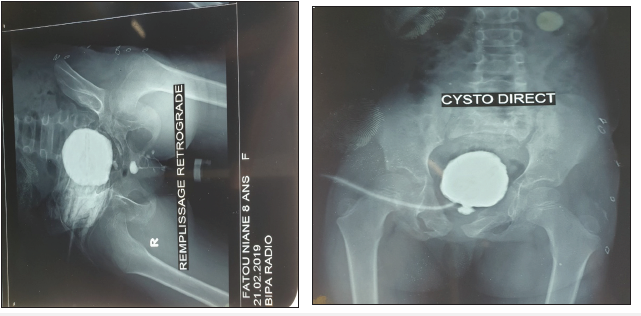
cystourethrogram showed a complete retro meatus urethral stricture associated with bladder
diverticula (Figure 1). The ultrasound showed a stage II left hydroureteronephrosis with thick
left bladder wall. A cystoscopy under general anesthesia was performed and showed a normal
meatus and distal urethra and an obliterated urethra 1cm from the meatus. A cystoscopy
through the suprapubic cystostomy orifice was then performed and showed bladder
trabeculations, dilation of the left ureteral meatus and normal bladder neck. The proximal
urethra was dilated for 0,5cm proximal the stenosis. Urethroplasty was then decided to repair
the stenosis.
Figure 1:Cystography images showing stenosis of the urethra.
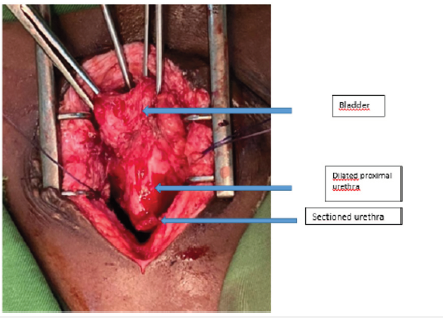
She was operated under general anesthesia; a midline incision was performed. The bladder was mobilized to expose the complete transection of the urethra and a dilation of the proximal part (Figure 2). A metallic guide wire was introduced through the meatus to identify the distal end of the urethra that was attached to the pubic bone. We mobilized and opened the 2 obliterated ends of the urethra and performed an anastomotic urethroplasty around a 10Fr Foley catheter. The post-operative period was complicated by a urinary tract infection due to Klebsiella Pneumoniae that was treated. The Foley catheter was removed 21 days after surgery. The outcome was satisfactory with good urine stream and urinary continence. Three months later the patient maintained a normal micturition with a good urinary continence.
Figure 2: Intraoperative image of the urethra section.
Discussion
Urethral traumas only occur in 3.4% of children who undergo trauma of the urinary tract [6]. They are more frequent in boys (7.4 to 13.5%) than girls (4 to 6%) [7]. That can be explained by the shortness of the female urethra, its mobility and the fact that it is protected by the pubic bone [1,6]. Urethral injury is more likely when there is a vaginal wound, diastasis of the symphysis pubis, multiple pubic fractures, or sacral injuries [5]. These injuries were present in our patient. However, the diagnosis of the urethral trauma is delayed in 40% of the cases [5] which was the case for the patient. This diagnostic delay can be responsible for severe perineal infection and a delay of treatment for the patient [5]. Thus, for every patient who has these lesions, it must be mandatory to search for urethral trauma. This search must be done through a voiding cystography alongside a cystoscopy which is the gold standard exam to localize and classify urethral lesions in girls [8]. The best management of the urethral trauma in girls is the immediate repair as soon as the patient is hemodynamically stable, right after the orthopedic repair, during the same general anesthesia [1,5,7]. The repair during the acute phase can decrease the risk of fibrosis. Moreover, there is a risk of a vaginal stenosis, urethrovaginal fistula and sphincter insufficiency in case of delayed repair [5,7]. Depending on the location of the urethral lesion and whether the vagina is wounded or not, the surgical approach can be retro-pubic, trans-pubic, trans-vesical, or trans-vaginal [7,8]. We opted for the retro-public approach due to the proximal location of the stenosis. The primary repair can be done by endoscopic realignment or anastomotic urethroplasty which has a better longterm outcome [5]. In the case of a delayed repair of the urethra, the technique depends on the location and type of the lesion [7,9]. In the case of a major wound, the repair can be done with a vesical, vaginal or oral mucosal graft. If the lesion is distal and the proximal urethra is intact, the best treatment is the creation of a new meatus [10]. In absence of a major wound, an anastomotic urethroplasty without tension of the urethra is the best choice, which was the case for our patient [7,9]. The complications of the reconstructions are predominately stenosis, vesico-vaginal fistula and urinary incontinence [9].
Conclusion
The search of urethral lesion in all girls who have a pubic or sacrum fracture, or vaginal laceration must be systematic. The diagnosis is confirmed by voiding cystography and cystoscopy. The management is urgent and must be done by specialized surgeon’s right after stabilizing the patient hemodynamically. Primary anastomotic urethroplasty is the best therapeutic choice.
Acknowledgment
The authors received no financial support for the research,
authorship, or publication of this article.
The authors declare no conflict of interest.
References
- Dorairajan LN, Gupta HH, Kumar S (2004) Pelvic fracture-associated urethral injuries in girls: experience with primary repair. BJU Int 94(1): 134-136.
- Delaney KM, Reddy SH, Dayama A, Stone ME, Meltzer JA, et al. (2016) Risk factors associated with bladder and urethral injuries in female children with pelvic fractures: an analysis of the national trauma data bank. J Trauma Acute Care Surg 80(3): 472-476.
- Hagedorn JC, Voelzke BB (2015) Pelvic fracture urethral injury in children. Arab J Urol 13(1): 37-42.
- Podesta ML, Jordan GH (2001) Pelvic fracture urethral injuries in girls. J Urol 165(5):1660-1665.
- Patel DN, Fok CS, Webster GD, Anger JT (2017) Female urethral injuries associated with pelvic fracture: a systematic review of the literature. BJU Int 120(6): 766-773.
- Tarman GJ, Kaplan GW, Lerman SL, Mcaleer IM, Losasso BE, et al. (2002) Lower genitourinary injury and pelvic fractures in pediatric patients. J Urol 59(1): 123-126
- Pilchler R, Fristch H, Skradski V, Horninger W, Schlenck B, et al. (2012) Diagnosis and Management of Pediatric Urethral Injuries. Urol Int 89(2): 136-142.
- Pineiro LM, Djakovik N, Plas E, Mor Y, Santucci RA, et al. (2010) Guidelines on Urethral Trauma. Eur Urol 57: 791-803.
- Ackerman AL, Blaivas J, Anger JT (2010) Female urethral reconstruction. Curr Bladder Dysfunct Rep 5(4): 225-232.
- Hemal AK, Dorairajan LN, Gupta NP (2000) Posttraumatic complete and partial loss of urethra with pelvic fracture in girls: an appraisal of management. J Urol 163 (1): 282-287.
© 2021 Mohamed Jalloh. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






