- Submissions

Full Text
Experiments in Rhinology & Otolaryngology
Correlations Between Computed Tomography and Nasal Endoscopic Findings in Patients of Chronic Rhinosinusitis
Abhishek K Ramadhin*
Otolaryngology - Head and Neck Surgery, Tufts University School of Medicine, USA
*Corresponding author: Abhishek K Ramadhin, MD, Rhinology fellow, St. Elizabeth’s Medical Center Clinical Associate, Otolaryngology - Head and Neck Surgery, Tufts University School of Medicine, Boston, USA
Submission: June 06, 2018;Published: September 20, 2018

ISSN 2637-7780 Volume2 Issue4
Abstract
Objectives: To correlate between computed tomography and nasal endoscopic findings in patients of chronic rhinosinusitis (as per RSTF symptom criteria). Study design: Cross-sectional study.
Materials and methods: All adult patients presenting for evaluation of Chronic Rhinosinusitis were studied with the use of the rhinosinusitis symptom inventory (RSI), nasal endoscopy, and sinus computed tomography (CT). We determined sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) between scores for symptoms, endoscopy, and CT.
Results: A total of 78 patients were studied with the use of the rhinosinusitis symptom inventory and then data were analysed. For endoscopy, after taking CT scan as gold standard, sensitivity, specificity, positive predictive value, and negative predictive value were calculated as 92.7, 91.3, 96.2, and 84 percent with likelihood ratio 55.59 (p=.000).
Conclusion: In CRS patients, for decision making, Endoscopy and CT scores correlate well with each other but not so well with the symptom score.
Keywords: Pott’s puffy tumour; Frontal osteomyelitis; Complication of sinusitis
Introduction
Chronic Rhino Sinusitis (CRS) is one of the commonest medical disease that has both boundless personal and economic impression. Given the importance of the disease, an acceptable uniform definition of sinusitis was needed for many years. But there was not a common consensus on it. To resolve this issue, first time in 1996, the American Academy of Otolaryngology-Head and Neck Surgery (AAO- HNS) convened a multidisciplinary RhinoSinusitis Task Force (RSTF) to challenge difficult issues associated to defining, staging, and research of rhino- sinusitis. The resulting article, “Adult Rhinosinusitis” published in 1997 [1]. In that article, first time officially Rhinosinusitis was explored and defined as “The condition manifested by an inflammatory response involving the following; the mucous membranes of nasal cavity and paranasal sinuses, fluids within these cavities, and / underlying bone”. Gradually various researchers found that factors contributing can be mucociliary impairment [2,3], infection bacterial, allergy, swelling of the mucosa for another reason, or physical obstructions caused by morphological/ anatomical distinctions in the nasal cavity or paranasal sinuses [4,5].
The multidisciplinary Rhino Sinusitis Task Force (RSTF) working definition of chronic rhinosinusitis is duration and symptom based and stated that any form of rhinosinusitis lasting for more than 12 weeks and having 2 or more major symptoms or 1 major and 2 minor symptoms, out of twelve major and minor symptoms. These symptom criteria had been useful in creating a standard in diagnosing rhinosinusitis. And nasal endoscopy has emerged as another mode of objective assessment of chronic rhinosinusitis used at all the centers worldwide to complement examinations to confirm diagnosis of the disease. It provides aids in assessing the integrity of the mucosa, as well as directly seeing mucosal changes, polyps, crusting, and/or discharge [6].
CT scan is another very important and popular investigation done since decades and got the value of gold standard test for CRS. It can delineate areas which is effective in demonstrating predisposing causes of chronic rhinosinusitis like anatomical distinction, variation, trauma and tumor. This can cause reduction of the ostiomeatal complex and sinus drainage channels. The association between symptom severity and CT scan findings has been a mat- ter of argument with studies providing conflicting reports [7-10]. Therefore, objective of the study is to correlate between computed tomography and nasal endoscopic findings in patients of chronic rhinosinusitis (as per RSTF symptom criteria)
Materials and Methods
The study was a cross-sectional study of 78 patients seen in the Department of Otorhinolaryngology and Head & Neck surgery in a tertiary care center. The sample comprised of adult patients presenting for assessment of CRS by using the RSTF symptom criteria’s, nasal endoscopy, and paranasal sinus computed tomography (CT). Patients were excluded from the study if they had a history of previous sinonasal surgeries, immune-compromised or autoimmune disorders, cystic fibrosis, recurrent acute rhinosinusitis, or if they were less than 18 years of age.
Method of Collection of Data
Rhinosinusitis symptom inventory (RSTF symptom criteria)
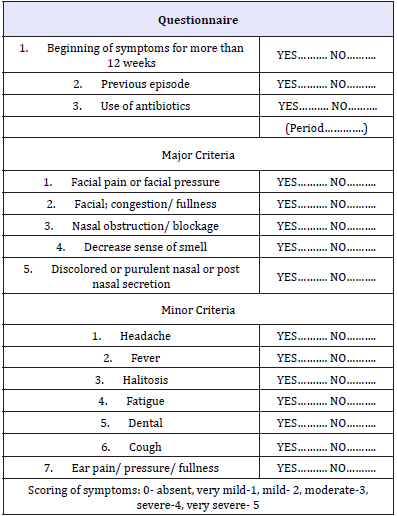
All patients completed the RSTF symptom criteria, which arranges the guideline symptoms of sinusitis on a six-point Likert scale going from zero (no symptoms) to five (maximal symptoms). As per the rule suggestion, the patient met symptom criteria for CRS if the subject had at least two major manifestations or one major and at least two minor symptoms that went on for over 12 weeks. A patient questionnaire was created to recognize the nearness of sinusitis manifestations as specified by the RSTF symptom criteria (Table 1).
Table 1:
A rigid sinonasal endoscope
Figure 1:
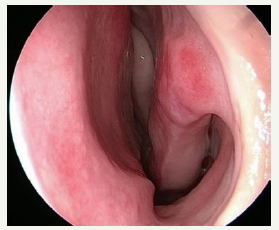
As per decorum, nasal endoscopy was done under topical anesthesia with a Zero degree or/and Thirty-degree rigid 4mm diameter endoscope and quantified using the Lund - Kennedy scoring system. According to this system, the endoscopic visualisation of the nose was quantified for the presence of polyps, discharge and edema. The scoring as shown in Table 2 & Figure 1 the diagnostic evidence of CRS was defined by a Lund-Kennedy endoscopic score greater than or equal to 2. The endoscopist was blinded to patient’s symptom scores.
Table 2:
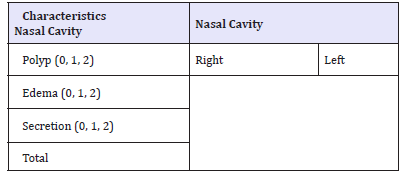
Note: polyp: 0- absent; 1-limited to the middle meatus; 2- extending to the nasal cavity Mucosa edema: 0- absent;
1-mild/moderate edema; 2- polypoid degeneration
Secretion:
0-absent
1-hyaline
2-thick and/or Mucopurulent
The CT scans
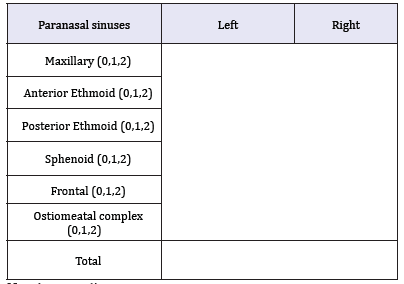
Another diagnostic evidence of CRS was defined and compared by the gold standard CT scan. Each patient CT scan of the paranasal sinuses was obtained and staged using the Lund Mackay CT scoring system. As shown in Table 3 & Figure 2. This system is based on the appearance of each paranasal sinus on the CT scan. The reviewer was blinded to the RSTF symptom criteria scores and endoscopic findings.
Figure 2:
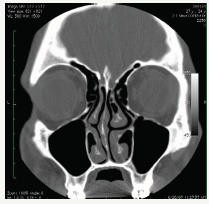
Table 3:
Statistical Analysis
Data for symptom criteria, endoscopic findings, and CT scores were tabularized in Excel data sheet and imported into SPSS software and then statistical analyses for specificity, sensitivity, negative predictive value (NPV), positive predictive value (PPV), likelihood ratio was performed to evaluate the symptom criteria for CRS and the diagnostic value of endoscopy and comparing it with gold standard CT scan. Analyses was performed with mild CT scan score i.e. LM score 1 and with moderate CT score i.e. LM score 4 and with endoscopy CRS diagnosis is taken as LK score 2.
Results
Total 78 eligible patients were chosen for analysis. The mean age of final study group was 37yrs and age group ranged from 18- 75 years. There were 61.5 % men and 38.5% women. As only those patients, who met RSTF symptoms criteria were included in the study. The top symptoms were headache, nasal obstruction, fatigue and facial pain pressure details are in Table 4. For alone major criteria of RSTF, the sensitivity, specificity, positive predictive value, and negative predictive value were 83.63, 30.43, 74.9, and 43.75 percent, respectively, for CRS (P=0.16).
Table 4:

Nasal endoscopy
mean Lund-Kennedy score was 4.1 with standard deviation 3.1 (Figure 3). Taking Lund-Kennedy score 2 for diagnosis of CRS and RSTF symptom criteria as gold standard, the sensitivity was 67.3%, and taking CT scan as gold standard with Lund MacKay score 1, the sensitivity, specificity, positive predictive value, and negative predictive value were 80.3, 100, 100, and 48. With chi square value 30.06 (p=.000) and likelihood ratio 32.357 (p=.000). and taking strict CT scoring with Lund Mackay score 4 the sensitivity, specificity, positive predictive value, and negative predictive value changes to 92.7, 91.3%, 96.2, and 84 percent, with likelihood ratio 55.59 (p=.000).
Figure 4:
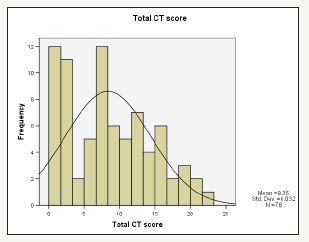
Figure 5:

CT scan
The mean Lund Mackay score was 8.35 with standard deviation 6. 03 (Figure 4) for CT scan alone taking Lund-Mackay score 1 and taking RSTF as gold standard, the sensitivity was 84.6%. but after taking only major symptom criteria as gold standard, the sensitivity was 85.5%, specificity was 18.8%, PPV was 80.3% and NPV was 25.0 %. With Pearson Chi-Square 0.175 and P=.676, with Lund Mackay 4 taking as diagnostic for CT scan alone taking RSI as gold standard, the sensitivity was 70.5%. And for major symptom criteria as gold standard, the sensitivity was 79.5%, specificity was 43. 8%, PPV- was 83.6% and NPV was 30.4%. With Pearson Chi-Square 1.969 and P=.161. likelihood ratio 1.87 (p=0.171).
Discussion
Chronic rhinosinusitis (CRS) is a common health problem that leads to regular visits to primary care GPs and to the otolaryngologist. A substantial advance in the diagnosis of CRS came with the American Academy of Otolaryngology’s Task Force on CRS, with the explanation of clinical criteria for the diagnosis of CRS [1]. Though the diagnosis of CRS as per the Task Force criteria is constructed on clinical grounds, the use of nasal endoscopy and CT scan helps in doing specific diagnosis and treatment [11,12].
Symptomatology
In our study we analyzed the symptomatology as of by 1997 Rhinosinusitis task force (RSTF) recommendations 12 criteria. Our evaluations were comparable to the study done by Francis [13]. The commonest symptoms were headache, nasal obstruction, fatigue, and facial pain pressure.
CT scan
In our study, we have taken (Lund-Mackay score of equal or more than 1 and 4 for diagnosis the CRS). As out of various CT scoring system only Lund-Mackay score is accepted by task force. For Lund MacKay score 1, sensitivity was 85.5%, specificity was 18.8 %, PPV was 80.3% and NPV was 25.5%. But with Lund MacKay score 4 it changed to sensitivity 79.5%, specificity 43. 8%, positive predictive value 83.6% and negative predictive value 30.4%. (P=.16). Therefore, it could be said that with lenient CT scoring (lund mackay score 1) the specificity reduces a lot.
Hwang et al. [14] had also shown in their study if RSTF symptoms are the gold standard diagnostic criteria, the positive predictive value (65%) and negative predictive value (10%) of CT scan findings were poor. Sensitivity (89%) was marginal, but specificity (2%) was very poor.
Diagnostic nasal endoscopy findings
For endoscopic evaluation we resorted to Lund- Kennedy DNE scoring system parameters, with a minimum score 2 or more than 2 for diagnosing the CRS. In our study, for endoscopy, taking RSTF symptom criteria as gold standard, the sensitivity was 67.3% and after taking CT (Lund MacKay score 4) as gold standard, the sensitivity, specificity, positive predictive value, and negative predictive values were 92.7, 91.3%, 96.2, and 84 percent.
Levine [15] study with nasal endoscopy revealed fifty-eight (38.7%) patients with nasal pathology who had not been seen with traditional anterior and posterior rhinoscopic examination. Kasapoglu et al. [16], found sensitivity of CT scan was 93% and overall correlation of diagnostic nasal endoscopy and CT findings were 87%. Stankiewicz [17], found out in their study that positive endoscopic results correlated well with CT, and negative endoscopic results correlated in 71% of patients with negative CT results.
Considering independently every one of the three assessments for the determination of Chronic rhinosinusitis, we watched that there was a statistically significant difference between them. In addition, considering the aftereffects of agreement and disagreement with respect to the illness, the investigation demonstrated that CT scan and nasal endoscopy displayed higher level of concurring outcomes, though CT scan and the questionnaire presented the highest proportion of disagreeing results.
Conclusion
In CRS patients, for decision making, Endoscopy and CT scores correlate well with each other but not so well with the symptom score. In patients who fulfil guideline symptom criteria for CRS, the addition of nasal endoscopy improves diagnostic precision for CRS.
References
- Lanza DC, Kennedy DW (1997) Adult rhinosinusitis defined. Otolaryngology and Head & Neck Surg 117(3): S1–S7.
- Sturgess JM, Chao J, Wong J, Aspin N, Turner JA (1979) Cilia with defective radial spokes: a cause of human respiratory disease. N Engl J Med 300(2): 53-56.
- Zacharek MA, Krouse JH (2003) The role of allergy in chronic rhinosinusitis. Otolaryngol Clin North Am 11(3): 196-200.
- Jones NS (2002) CT of the paranasal sinuses: a review of the correlation with clinical, surgical and histopathological findings. Clin Otolaryngol 27(1): 11-17.
- Jones NS, Strobl A, Holland I (1997) A study of the CT findings in 100 patients with rhinosinusitis and 100 controls. Clin Otolaryngol 22(1): 47-51.
- Meltzer EO, Hamilos DL, Hadley JA, Lanza DC, Marple BF, et al. (2004) Rhinosinusitis: establishing definitions for clinical research and patient care. J Allergy Clin. Immunol 114(6 Suppl): 155-212.
- Zinreich SJ, Kennedy DW, Rosenbaum AE (1987) Paranasal sinuses: CT imaging requirements for endoscopic surgery. Radiology 163(3): 769- 775.
- Bhattacharyya N (2006) Radiographic stage fails to predict symptom outcomes after endoscopic sinus surgery for chronic rhinosinusitis. Laryngoscope 116(1): 18-22.
- Wabnitz DA, Nair S, Wormald PJ (2005) Correlation between preoperative symptom scores, quality-of-life questionnaires, and staging with computed tomography in patients with chronic rhinosinusitis. Am J Rhinol 19(1): 91-96.
- Bradley DT, Kountakis SE (2005) Correlation between computed tomography scores and symptomatic improvement after endoscopic sinus surgery. Laryngoscope 115(3): 466-469.
- Lund VJ, Kennedy DW (1997) Staging for rhinosinusitis. Otolaryngol Head Neck Surg 117 (part 2): S35-S40.
- Buljcik Cupic MM, Savovic SN (2007) Endonasal endoscopy and computerized tomography in diagnosis of the middle nasal meatus pathology. Med Pregl 60: 327-332.
- Francis TK, Ling FT, Stilianos E, Kountakis SE (2007) Important clinical symptoms in patients undergoing functional endoscopic sinus surgery for chronic rhinosinusitis. Laryngoscope 117(6): 1090-1093.
- Hwang PH, Irwin SB, Griest SE, Caro JE, Nesbit GM (2003) Radiologic correlates of symptom-based diagnostic criteria for chronic rhinosinusitis. Otolaryngology and Head & Neck Surg 128: 489(4): 496.
- Levine HL (1990) The office diagnosis of nasal and sinus disorders using rigid nasal endoscopy. Otolaryngol Head Neck Surg 102(4): 370-373.
- Kasapoglu, Fikret, Onart, Selcuk B (2009) Preoperative evaluation of chronic rhinosinusitis patients by conventional radiographies, computed tomography and nasal endoscopy. Kulak Burun Bogaz Ihtisas Derg 19(4): 184-191.
- Stankiewicz JA, Chow JM (2002) Nasal endoscopy and the definition and diagnosis of chronic rhinosinusitis. Otolaryngol Head Neck Surg 126(6): 623-627.
© 2018 Abhishek K Ramadhin. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






