- Submissions

Full Text
Experiments in Rhinology & Otolaryngology
An Unusual Case of Secondary in Sphenoid Sinus from Carcinoma Prostate
George MV1* and Julit A Kannath2
1 Department of ENT, Jubilee Mission Medical College, India
2 Associate Professor in Radiodiagnosis department, Jubilee Mission Medical College Hospital and Research Institute, India
*Corresponding author: George MV, Department of ENT, Jubilee Mission Medical College, India
Submission: April 16, 2018; Published: May 11, 2018

ISSN 2637-7780 Volume1 Issue4
Abstract
This article is about a 69-year-old male patient, in whom there was a secondary metastasis in the Sphenoid sinus from a primary prostate carcinoma which was treated 10 years back from a reputed Medical College Hospital of South India. Prostatic cancer is commonly manifested by obstructive uropathy, regional lymphatic metastases, and hemato genous metastases to the axial skeleton. In the paranasal sinuses, metastatic carcinoma is far less common than primary carcinoma. While metastatic tumours to the nose and the paranasal sinuses overall are unusual, metastasis to the sphenoid sinus is exceedingly rare. The peculiarity of this patient was that, it presented with recurrent bleeding from nose and not the usual way of involvement of adjacent structures.
Introduction
Prostate cancer is the second most common cancer in men worldwide and the 8th leading cause of cancer death. The most dangerous stage of it is, bone metastasis [1]. Cancer prostate patients usually presents to the urologists with urinary obstruction They can present with regional lymph node metastasis also. Very rarely may present with bone metastasis also before other manifestations. As Sphenoid sinus metastasis was reported as the first manifestation in one case [2]. Metastasis of skull bone is usually seen in breast, lung and prostate carcinoma. Five syndromes have been described according to the metastatic site including orbital, para-sellar, middle fossa, jugular foramen and occipital condyle syndromes. MRI is the best in these cases. But CT with bone window and isotope scan also equally effective [3].
Case Report
Figure 1:
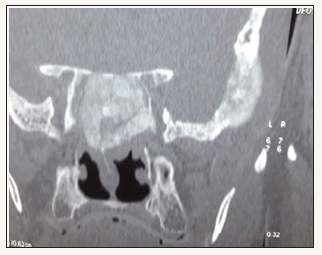
A 79-year-old male patient presented with history of recurrent bleeding from nose and naso pharynx. Diagnostic nasal endoscopy did not reveal any obvious lesions. There was no generalized bleeding tendency. Coagulation profile was normal. There was no hypertension. Renal and hepatic functions were normal. Treatment history for carcinoma prostate 10 years back from a premier medical college of South India was available. When he came to us serum PSA was 100mg/ml and acid phosphate was 63 units CT scan of the PNS showed an osteo blastic expansile lesion of the Sphenoid (Figure 1). A biopsy was not taken as it was very clear that he had secondaries in the Sphenoid from his prostate carcinoma he had, because of the following 3 reasons (Figure 2).
Figure 2:

a. Elevated PSA of 100mg/ml
b. Increased acid phosphate of 63 units
c. Osteoblastic expansive bones lesions; He was then referred to medical oncologist as advised by the urologist.
Discussion
Manifestations of metastatic of the skull bone are usually by the previously mentioned five syndromes producing cranial nerve involvement [3]. Lavasani et al. [4] described a case of a 67-yearoldman with adeno carcinoma of prostate who presented with gradual loss of vision. MRI in this case shown lesion of the orbital apex with extension to the ipsilateral Sphenoid. Barrs DM et al. [5] reported in a study of 8 patients with metastatic of Sphenoid that the symptoms resulted due to the involvement of adjacent strictures like the involvement of cranial nerves producing diplopia and decreased visual acuity. The primary sites were thyroid, kidney and breast. Prostate was the primary in only 2 cases. Viswanatha et al. [6] reported a case of secondary in the frontal and ethmoid sinus from prostate. Mikel et al. [7] reported that metastasis to PNS is rare and to the Sphenoid it is exceedingly rare. Symptoms included headache, facial pain, visual changes, and cranial nerve paralysis. Initial pathology, how long after primary therapy the PSA relapse occurs, how fast it is allaid in the distinction between local and distant failure [8]. In a study of 279 cases parasellar and sellar syndrome were seen in 29% cases. Middle fossa and jugular foramen syndrome in 6 and 3.5% cases. No specific syndrome in 33% [9].
Conclusion
It is rare to have secondaries of carcinoma prostate in Sphenoid sinus. This patient has presented in the unusual way. Moreover, he presented with the symptom of recurrent epistaxis instead of the usual way of involvement of adjacent strictures causing problems with vision or cranial nerve paralysis. Thus, this patient had an unusual complication of a common disease of skeletal secondary from prostate, in Sphenoid sinus.
References
- Burgess AW (2017) Bi specific protein targets prostate cancer. Oncotarget 8(22): 350-484.
- Matsumoto I, Furusato M, Inomata I, Wada T, Aizawa S (1986) Prostatic cancer presenting as metastatic adenocarcinoma of sphenoid sinus. Pathology International 36(11): 1753-1756.
- Laigle Donadey F, Taillibert S, Martin Duverneuil N (2005) Skull base metastases. J Neurooncol 75: 63
- Lavasani L, Zapanta PE, Tanna N, Sadeghi N (2006) Metastasis of prostatic adeno carcinoma to the sphenoid sinus. Ann Otol Rhinol Laryngol 115(9): 690-693.
- Barrs DM, Mc Donald TJ, Whisnant JP (1979) Metastatic tumors to the sphenoid sinus. The Laryngoscope 89(8): 1239-1243.
- Viswanatha B (2008) Prostatic carcinoma metastatic to the paranasal sinuses: a case report. Ear Nose Throat J 87(9): 519-522.
- Mickel RA, Zimmerman MC (1990) The sphenoid sinus-a site for metastasis. Otolaryngol Head Neck Surg 102(6): 709-716.
- Heidenreich A, Bastian PJ, Bellmunt J, Bolla M, Joniau S, et al. (2014) EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and local treatment with curative intent update 2013. Eur Urol 65(1): 124-137.
- Laigle Donadey F, Taillibert S (2005) Skull-base metastases. Journal of Neuro-Oncology 75(1): 63-69.
© 2018 George MV. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






