- Submissions

Full Text
Examines in Physical Medicine and Rehabilitation: Open Access
Rare Case Primary Report: Xia Gibb’s Syndrome
Rashij M* and Shabana CM
Physiotherapist, District Hospital, India
*Corresponding author: Rashij M, Physiotherapist, District Hospital, India
Submission: July 12, 2021; Published: July 29, 2021

ISSN 2637-7934 Volume3 Issue3
Abstract
Xia-Gibbs syndrome (Mental retardation, autosomal dominant 25; MRD25) (MIM 615829), first described in 2014, is a rare autosomal dominant disease characterized by mental retardation, developmental delay, speech delay, structural brain anomalies, hypotonicity, protuberant eyes, visual problems, laryngomalacia and low sleep quality. It occurs due to heterozygous mutations in the AT-hook DNA binding motif containing 1 (AHDC1) gene on chromosome 1p36. Research reports published in 2020 by Ping et al. [1], states that about 100 patients worldwide have been identified, all of them in the pediatric age or adulthood. To date, no fetal XGS has been reported [1-4]. Xia-Gibbs syndrome (XGS) is a recently described neurodevelopmental disorder due to heterozygous loss-of-function AHDC1 mutations. XGS is characterized by global developmental delay, intellectual disability, hypotonia, and sleep abnormalities. We are here to report our primary observations and findings of a diagnosed case of Xia Gibb’s Syndrome referred for Physiotherapy with signs of development delay, atonia, joint laxity and related features.
Keywords: Xia-Gibbs syndrome; XGS; Physiotherapy
Introduction
Eleven months old Ayesha Sajeer, a diagnosed case of “Xia Gibb’s Syndrome’’, (XGS) was
referred for Physiotherapy in the second week of April 2021 through the Physical Medicine
and Rehabilitation Department of Government District Hospital, Tirur, Kerala. She was sent
with signs of global development delay, dysmorphism and poor muscle tone. Baby Ayesha was
born as the 3rd child for a non-consanguineous couple without any significant prenatal and
perinatal events. She was born as NVD, cried immediately and the recorded birth weight was
2.650Kgs. No indications for immediate intensive care were noted on day one. However, on
the second day evaluation, the Pediatrician noticed a typical cardiac murmur which was later
confirmed as CHD - Atrial Septal Defect. This was managed conservatively from then.
Baby Ayesha was presented with general motor development delay, hypotonia, peripheral
joints laxity, high forehead, hypertelorism, bilateral hypo-pigmented iris, depressed nasal
bridge, upturned nares, low set ears, smooth philtrum, thin and tented upper lip, short
neck, transverse palmar crease, bilateral clinodactyly, oedematous limbs (specially feet), incurving
5th toes (bilateral) and mild hearing loss bilaterally. No symptoms of sleep apnea,
tracheomalacia, seizures, strabismus and orthopedic deformities were noted. Patient is too
young to evaluate autistic signs, intellectual disabilities, speech delays, sensory processing
disorders and behavioral issues. Brain MRI was not available to assess any structural brain
defects. Mother is 29 years old now, homemaker and father are 39 years, working abroad as
an unskilled labourer. Siblings are growing normal and are aged 9 and 4 years. No cases like
this were reported both on the maternal and paternal side. Baby Ayesha was the first case of
Xia Gibb’s Syndrome (XGS) attended by our department for Physiotherapy services. This is the
first case reported in this region. After the basic clinical evaluation on the day, the case was
asked to come on a later date to start with therapeutic interventions.
Meanwhile, we did refer to the available details on the web.
Since this was a newly identified genetic disorder, not many articles
were found on this. Only one article was found during our search
done between 13/04/2021 & 21/04/2021. This was published
from India by Goyal C, Naqvi W, Sahu A in 2020, at Cureus 12(8).
According to Goyal et al. [5] “NDT and SI approaches along with
the use of appropriate orthoses accelerated the achievement of
motor milestones in their case.” However, the case seen by them
was a 27 month boy with difficulty in sitting without support.
Based on our clinical experiences in Pediatric Physiotherapy and
the little information we have gathered from the literature, we have
taken this case for institution-based habilitation. We have enlisted
the following where Physiotherapy interventions are indicated.
(1) Global developmental delay (2) Hypotonia and joints laxity
(3) Spine care as precautionary (4) Orthotic supports as SOS. We
believe a regular therapist guided NDT program comprising weight
shifts, transitions, posturing and movement facilitation along with
accommodative chair, vestibular & reticular tracts stimulations,
weight bearing acts etc will help her progress.
Presently, we have scheduled 4/7 Physiotherapy visits for
her. Gradually, once I gain the confidence of the parents and vice
versa, the exercise regime can be progressed to home based with
periodic reviews. Speech therapy, Audiology and Occupational
therapy consultations will be scheduled as and when required. A
therapy diary to record the day-to-day events, medical and therapy
follow etc. and also comprising all exercises to be followed at home,
is issued to her. The status of her progress, outcome measures,
procedural images etc (Figure 1 & 2), will be reported after 8-12
months of interventions.
Figure 1: Features of dysmorphism.
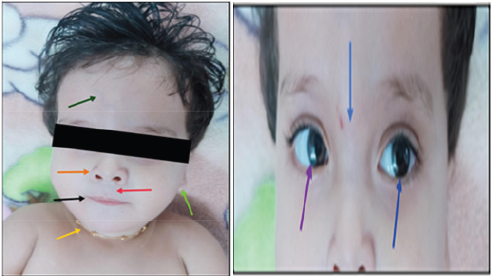
Figure 2: Transverse palmar crease.

Acknowledgement
Dr Javed Anees P, Junior Consultant-PM & R, District Hospital, Tirur, Malappuram, Kerala, India for referring the case and Ms Linshina T, Physiotherapist, Asten Physiotherapy Clinic, Othukkungal, Malappuram, Kerala, India for assisting in literature search.
References
- Ping He, Yu Yang, Zhen L, Li DZ (2020) Recurrent hypoplasia of corpus callosum as a prenatal phenotype of Xia-Gibbs syndrome caused by maternal germline mosaicism of an AHDC1 variant. European Journal of Obstetrics & Gynecology and Reproductive Biology 244: 208-210.
- Fan Xia, Bainbridge MN, Tan TY, Wangler MF, Scheuerle AE, et al. (2014) De novo truncating mutations in AHDC1 in individuals with syndromic expressive language delay, hypotonia, and sleep apnea. Am J Hum Genet 94(5): 784-789.
- Ritter AL, McDougall C, Skraban C, Medne L, Bedoukian EC, et al. (2018) Variable clinical manifestations of Xia Gibbs syndrome: Findings of consecutively identified cases at a single children's hospital. Am J Med Genet A 176(9): 1890-1896.
- Yang H, Douglas G, Monaghan KG, Retterer K, Cho MT, et al. (2015) De novo truncating variants in the AHDC1 gene encoding the AT-hook DNA-binding motif-containing protein 1 are associated with intellectual disability and developmental delay. Cold Spring Harb Mol Case Stud 1(1): 562.
- Goyal C, Naqvi W, Sahu A (2020) Xia-Gibbs syndrome: A rare case report of a male child and insight into physiotherapy management. Cureus 12(8): 9622.
© 2021 Rashij M. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






