- Submissions

Full Text
Determinations in Nanomedicine & Nanotechnology
Nanoparticles from Tulsi (Ocimum Sanctum) in Immune Enhancement against COVID-19 Situation
Dharita Desai and Thulasi G Pillai*
K J Somaiya Institute of Engineering and Information Technology, Affiliated to Mumbai University, Mumbai, India
*Corresponding author: Thulasi G Pillai, K J Somaiya Institute of Engineering and Information Technology, Affiliated to Mumbai University, Mumbai, India
Submission: December 8, 2021;Published: February 14, 2022

ISSN: 2832-4439 Volume2 Issue3
Abstract
The world is witnessing the outbreak of COVID-19, a disease caused by a novel corona virus, SARSCoV- 2. It has largely affected people throughout the world and has weakened their immune systems to a great extent. To get rid of suffering and curing ailments and to enhance our immune system humans have been using plants from prehistoric times. Nanoparticles in plants are referred to as building blocks of nanotechnology. Plants produce stable nanoparticles and also the rate of synthesis is faster than that of the microorganisms. Ocimum sanctum commonly known as tulsi is considered as “The Queen of Herbs”. It has a significant role to play in traditional medicine. Several scientific studies have been conducted to reveal the efficient use of the whole plant or its parts for the treatment of different diseases. Nanoparticles in Tulsi can help to fight against various diseases and improves the immune system. Using leaf broth of medicinal herb Ocimum sanctum (Tulsi), the synthesis of antibacterial silver nanoparticles (AgNPs) is reported. Silver nanoparticles (AgNPs) are microbicidal agents. It could be potentially used as an alternative to antivirals to treat human infectious diseases generally where the other antivirals have generally proven unsuccessful, especially in the case of influenza virus infections [1-5]. It has been reported as one type of potent therapeutic nanoparticles which boost the immune system to a greater extent especially in the COVID-19 situation.
Keywords:Nanotechnology; Nanoparticles; Ocimum sanctum; Immune system; Silver nanoparticles; Corona virus; COVID-19
Abbreviations: CoV: Coronaviruses; MERS: Middle East Respiratory Syndrome; SARS-CoV-2: Severe Acute Respiratory Syndrome Coronavirus-2
Introduction
The outbreak of COVID-19 caused a huge effect on people and greatly affected their immune systems. The immune system of our body fights against various viruses, bacteria, and infectious diseases [6,7]. Anti-viral, anti-bacterial, and anti-oxidant properties of plants act as an immune booster especially during the time of COVID-19 situation. Nanoparticles are the building blocks for nanotechnology and the nanoparticles from plants are known for stability and faster rate of synthesis. Ocimum sanctum has also known as Tulsi is reported as the best herb with various properties to fight against infectious diseases. Nanoparticles in tulsi help fight against diseases and improve the immune system [8].
Corona virus
Coronaviruses (CoV) is a family of viruses that can cause illnesses ranging from the common cold to more severe diseases like severe pneumonia, acute respiratory distress syndrome, sepsis, and septic shock occur, all potentially leading to death [9-11]. Alpha, beta, gamma, and delta are four subtypes of coronavirus used by scientists to categorize the various species. Among all the types of coronaviruses, seven have affected humans out of which four most common are 229E, NL63, OC43, and HKU1. They cause mild illnesses in the upper and lower airways, nose, sinuses, throat, and lungs while the remaining three i.e., SARS-CoV, MERS-CoV, SARS-CoV-2 can cause more severe illness. SARS-CoV virus causes severe acute respiratory syndrome or SARS, and its symptoms include fever, tiredness, chills, muscle aches, cough, difficulty breathing, diarrhea [12]. In severe cases, SARS can cause a lack of oxygen in the blood, leading to death in 10% of people. While MERS-CoV is a type of coronavirus that causes Middle East Respiratory Syndrome, or MERS causing fever, cough, shortness of breath. Severe Acute Respiratory Syndrome Coronavirus-2 (SARS-CoV-2), the virus responsible for the COVID-19 pandemic [13]. It was first identified in Wuhan, China, in December 2019 and has since spread globally that is mainly transmitted through droplets generated when an infected person coughs, sneezes, or exhales.
Effects of Covid-19
COVID-19 has caused respiratory and intestinal infections in humans as well as animals. It can cause fever, dry cough, tiredness aches and pains, sore throat, diarrhea, conjunctivitis, headache, loss of taste or smell and a rash on the skin, or discoloration of fingers or toes [14-20]. The symptoms differ in severity, some people who have no symptoms up to those with fever, cough, sore throat, general weakness, and fatigue, and muscular pain while in very serious cases, severe pneumonia, acute respiratory distress syndrome, sepsis, and septic shock occur, potentially leading to death. Thus, it has largely affected the human immune system and reduced resistance against viruses and bacteria’s [21].
Immune enhancement in covid-19
Immune system is the fighter that protects our body against viruses and diseases and produces antibodies to kill pathogens [22,23]. They play a very significant role in fighting against infectious diseases and keep us healthy. It is important to enhance our immune system to fight against viruses like covid-19. Nanoparticles in plants that contain various properties and applications act as the best agents in fighting against various diseases and enhancing our immune system. Nutritional compounds like vitamin C, antioxidants, and zinc do work with your immune system while Vitamin C, Zinc, anti-viral and anti-bacterial properties of plants act as an immune booster thus keeping infection at bay [24].
Tulsi & its Nanoparticles
Tulsi scientifically known as Ocimum Scantum is considered as Queen of Herbs and described as a sacred and medicinal plant in ancient literature. It is derived from ‘Sanskrit’, which means “the incomparable one”. Tulsi in ayurvedic medicine is being used in various clinical conditions like anxiety, chronic cough, bronchitis, fever, snake, and scorpion bites [25]. It has various properties like Anti-stress, Antioxidant, Hepatoprotective,Immunomodulating, Anti-inflammatory, Anti-bacterial, Antiviral, anti-fungal, Antipyretic, Antidiuretic, Antidiabetic, Hypoglycemic, Hypolipidemic, Antimalarial, etc. Synthesis of antibacterial silver nanoparticles (AgNPs) is reported using leaf broth of medicinal herb Ocimum sanctum (Tulsi) [26,27].
Nanoparticles in Tulsi
Nanoparticles in plants are widely used due to their stability and faster synthesis and play a significant role in traditional medicine [28]. Tulsi nanoparticles (AgNPs) have great potential in a broad range of applications as antimicrobial agents, biomedical device coatings, drug-delivery carriers, imaging probes, and diagnostic and optoelectronic platforms biochemical functionality tailored by diverse size- and shape-controlled AgNPs [29]. They are considered as one of the most significant nanoparticles due to their exceptional broad-spectrum bactericidal properties, relatively low cost of manufacturing AgNPs, unique properties, and ability to form diverse nanostructures. Silver nanoparticles (AgNPs) are one of the most fascinating nanomaterials among several metallic nanoparticles as they are involved in biomedical applications. AgNPs have a significant role in nanoscience and nanotechnology, particularly in nanomedicine.
AgNPs biological and biomedical applications are antibacterial, antifungal, antiviral, anti-inflammatory, anti-cancer, anti-angiogenic, Bio-sensing, drug carrier, anti-tumor, anti-oxidative, imaging, and human health care [30,31]. Silver nanoparticles (AgNPs) are found in various shapes like spherical shape AgNPs, oval shape AgNPs, rod shape AgNPs, Flower shape AgNPs, and Precursors. AgNPs are microbicidal agents which could be potentially used as an alternative to antivirals to treat human infectious diseases, especially influenza virus infections where antivirals have generally proven unsuccessful. Its antibacterial effects of silver nanoparticles have been used to control bacterial growth also produce reactive oxygen species and free radicals which cause apoptosis leading to cell death preventing their replication. It is reported as one type of potent therapeutic nanoparticle which boosts the immune system to a greater extent especially in the COVID-19 situation [32,33].
Synthesis of AgNPs
Silver nanoparticles (AgNPs) have proved to be most effective because of its good antimicrobial efficacy against bacteria and viruses [34,35]. They are undoubtedly the most widely used nanomaterials among all and it has been reported through the studies about the successful biosynthesis of silver nanoparticles by plants such like ocimum scantum. They can be potentially used as an alternative to antivirals to treat human infectious diseases. There are three main categories for silver nanoparticle (AgNPs) mainly known as physical method, chemical method, biological method [36] (Figure 1).
Figure 1: Synthesis of AgNPs.
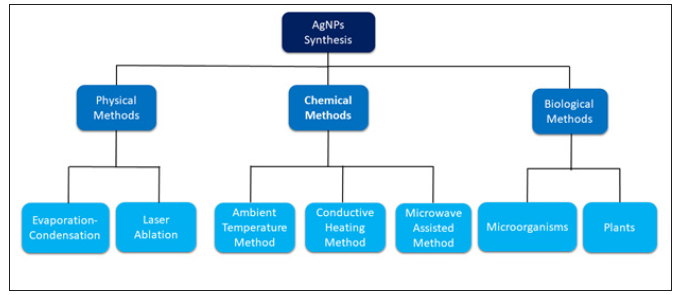
Physical methods: The two approaches of physical methods are evaporation-condensation and laser ablation. Physical synthesis methods using evaporation-condensation have an advantage over chemical methods due to the absence of solvent contamination in the prepared thin films and the uniformity of NPs distribution [37]. The evaporation-condensation method is very useful since nanoparticle generator for long-term experiments for inhalation toxicity studies. Silver nanoparticles (AgNPs) can also be synthesized using the laser ablation method of metallic bulk materials in solution. The absence of chemical reagents in solutions is the main advantage of the laser ablation technique for the production of metal colloids.
Chemical methods: The chemical method has three approaches i.e., ambient temperature methods, conductive heating methods, and microwave-assisted methods. Synthesis of silver nanoparticles (AgNPs) can also be done using chemical reduction by organic and inorganic reducing agents. Silver nanoparticles can be prepared by mixing the corresponding metal ions with reduced polyoxometalates which serve as reducing and stabilizing agents at room temperature. They can also be synthesized using microemulsion techniques as they are uniform and size controllable. The presence of citrate, polyvinylpyrrolidone, poly (acrylic acid), and collagen synthesis of silver nanoparticles (AgNPs) has been reported using UV-initiated photoreduction which is a simple and effective method. Synthesis of AgNPs using the photochemical method is also a clean process that has a high spatial resolution, convenience of use, and great versatility. The most promising one is the microwave-assisted method since microwave heating has shorter reaction times, reduced energy consumption, and better product yields. Thus, preventing the agglomeration of the particles formed. In order for consistently yielding nanostructures with smaller sizes, narrower size distributions, and a higher degree of crystallization microwave heating is better than a conventional oil bath. It was reported that by employing carboxymethyl cellulose sodium as a reducing and stabilizing agent synthesis of silver nanoparticles (AgNPs) can be done using the microwave-assisted method. Synthesis of AgNPs can also be done using the simple tollens method with controlled size [38].
Biological methods: The biological method has two effective approaches i.e., using microorganisms and plants. It has been reported that the synthesis of nanoparticles by chemical approaches is not eco-friendly and expensive. Thus, there is a need for developing eco-friendly processes that do not use toxic chemicals in the synthesis. During the research, it was observed that the potential of organisms in nanoparticle synthesis ranges from simple prokaryotic bacterial cells to eukaryotic fungi, and plants [39].
Biological methods can be used for the synthesis of highly stable and well-characterized nanoparticles. Synthesis of silver nanoparticles can be done by bioreduction of aqueous silver ions with culture supernatant of nonpathogenic bacterium, bacillus licheniformis. Using fusarium oxysporum silver nanoparticles AgNPs (5-50nm) could be synthesized extracellularly with no evidence of flocculation of the particles even a month after the reaction. The bioreduction of the silver ions occurred on the surface of the cells and proteins can have a critical role in the formation and stabilization of the synthesized silver nanoparticles (AgNPs). Chaetoceros Calcitrans, Chlorella Salina, Isochrysis Galbana, and Tetraselmis Gracilis are some of the marine algae that can be used for the reduction of silver ions and thereby the synthesis of silver nanoparticles (AgNPs). Synthesis of nanoparticles (NPs) using plants is a very cost-effective, economic, and valuable alternative, thus can be used for the large-scale production of NPs. Biosynthesis of silver nanoparticles (AgNPs) can be done using the extract of Camellia sinensis (green tea) as it acts as a reducing and stabilizing agent. In silver nanoparticle (AgNPs) synthesis plant extracts from alfalfa (Medicago Sativa), lemongrass (Cymbopogon Flexuosus), and geranium (Pelargonium Graveolens) have served as green reactants. For green synthesizing of silver nanoparticles (AgNPs), the capsicum annuum can also be used. It was observed and reported that Ocimum Sanctum (Tulsi) leaf extract can reduce silver ions into crystalline silver NPs (4-30nm) within 8 min of reaction time and were stable due to the presence of proteins which may act as capping agents. Tulsi leaves contain ascorbic acid which may play a significant role in the reduction of silver ions into metallic silver nanoparticles (AgNPs).
AgNPs in immune enhancement against Covid-19
Silver nanoparticles (AgNPs) have gained considerable interest due to their unique properties like antimicrobial, antiviral, antiinflammatory, etc. Covid-19 has adversely affected human health and reduced immune system to a great extent. Silver nanoparticles being microbicidal agents, reducing agent, stabilizer, flexibility, and other medicinal properties have significant inhibitory effects against microbial pathogens, and are widely used as antimicrobial in a diverse range of products. Antibacterial effects of silver nanoparticles have been used to control bacterial growth during covid-19 situation and helped improve human immune system. It also produces reactive oxygen species and free radicals which cause apoptosis leading to cell death preventing their replication. Thus, AgNPs acts as the best agents in fighting against various diseases and enhancing our immune system [40].
Application of AgNPs
Nanoparticles in tulsi have tremendous prospects for the improvement of the diagnosis and treatment of human diseases. They have gained considerable interest because of their medicinal as well as other properties and proven applicability in diverse areas. Their flexibility and incorporation into various media have encouraged researchers to further study the mechanistic aspects of antimicrobial, antiviral, and anti-inflammatory effects. AgNPs produce reactive oxygen species and free radicals and being one type of potent therapeutic nanoparticles, it is used to boost the immune system to a greater extent especially in the COVID-19 situation. Thus, they have huge applications in medicine and helps in the potential improvement of the immune system.
Conclusion
Tulsi nanoparticles being microbicidal agents and their incredible properties, have become significant in many fields in recent years such as health care, environment, agriculture, etc. Tulsi and its nanoparticles have highly medicinal applications and are used to improve the immune system, especially during the covid-19 situation. Viruses like covid-19 have highly affected human health and due to the medicinal effects of nanoparticles, they have served as an alternative to antivirals to treat human infectious diseases, control bacterial growth, and are proven as the best agents in fighting against various diseases and enhancing our immune system.
References
- Colvin VL, Schlamp MC, Alivisatos A (1994) Light emitting diodes made from cadmium selenide nanocrystals and a semiconducting polymer. Nature 370: 354-357.
- Wang Y, Herron N (1991) Nanometer-sized semiconductor clusters: Materials synthesis, quantum size effects, and photophysical properties. J Phys Chem 95(2): 525-532.
- Schmid G (1992) Large clusters and colloids. Metals in the embryonic state. Chem Rev 92(8): 1709-1727.
- Senapati S (2005) Biosynthesis and immobilization of nanoparticles and their applications. Ph.D. Thesis, University of Pune, India, pp. 1-57.
- Sastry M, Ahmad A, Khan MI, Kumar R (2003) Biosynthesis of metal nanoparticles using fungi and actinomycete. Curr Sci 85(2): 162-170.
- Mafune F, Kohno J, Takeda Y, Kondow T, Sawabe H (2000) Structure and stability of silver nanoparticles in aqueous solution produced by laser ablation. J Phys Chem B 104(35): 8333-8337.
- Mafune F, Kohno J, Takeda Y, Kondow T, Sawabe H (2001) Formation of gold nanoparticles by laser ablation in aqueous solution of surfactant. J Phys Chem B 105(22): 5114-5120.
- Tarasenko N, Butsen A, Nevar E, Savastenko N (2006) Synthesis of nanosized particles during laser ablation of gold in water. Appl Surf Sci 252(13): 4439-4444.
- Tsuji T, Iryo K, Watanabe N, Tsuji M (2002) Preparation of silver nanoparticles by laser ablation in solution: Influence of laser wavelength on particle size. Appl Surf Sci 202(1-2): 80-85.
- Tsuji T, Kakita T, Tsuji M (2003) Preparation of nano-size particle of silver with femtosecond laser ablation in water. Applied Surface Science 206(1-4): 314-320.
- Tien DC, Tseng KH, Liao CY, Huang JC, Tsung TT (2008) Discovery of ionic silver in silver nanoparticle suspension fabricated by arc discharge method. Journal of Alloys and Compounds 463(1-2): 408-411.
- Wiley B, Sun Y, Mayers B, Xi Y (2005) Shape-controlled synthesis of metal nanostructures: The case of silver. Chem Eur J 11(2): 454-463.
- Merga G, Wilson R, Lynn G, Milosavljevic B, Meisel D (2007) Redox catalysis on “naked” silver nanoparticles. J Phys Chem C 111(33): 12220-12206.
- Zhang Y, Peng H, Huang W, Zhou Y, Yan D (2008) Facile preparation and characterization of highly antimicrobial colloid Ag or Au nanoparticles. J Colloid Interface Sci 325(2): 371-376.
- Chen M, Feng YG, Wang X, Li TC, Zhang JY, et al. (2007) Silver nanoparticles capped by oleylamine: Formation, growth, and self-organization. Langmuir 23(10): 5296-5304.
- Ghosh SK, Kundu S, Mandal M, Nath S, Pal T (2003) Studies on the evolution of silver nanoparticles in micelle by UV-photoactivation. J Nanopart Res 5: 577-587.
- Abid JP, Wark AW, Brevet PF, Girault HH (2002) Preparation of silver nanoparticles in solution from a silver salt by laser irradiation. Chem Commun (Camb) 7: 792-793.
- Eutis S, Krylova G, Eremenko A, Smirnova N, Schill AW, et al. (2005) Growth and fragmentation of silver nanoparticles in their synthesis with a fs laser and CW light by photo-sensitization with benzophenone. Photochem Photobiol Sci 4: 154-159.
- Zhou P, Yang XL, Wang XG, Hu B, Zhang L, et al. (2020) A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 579: 270-273.
- Prakash P, Gupta N (2005) Therapeutic uses of Ocimum Sanctum Linn (Tulsi) with a note on eugenol and its pharmacological actions: A short review. Indian J Physiol Pharmacol 49(2): 125-131.
- Skaltsa M, Couladi M, Philianos S, Singh M (1987) Phytochemical studies of the leaves of ocimum sanctum. Fitotdepia 58(4): 286.
- Mondal S, Mirdha BR, Mahapatra SC (2009) The science behind sacredness of tulsi (Ocimum sanctum ). Ind J Physiol Pharmacol 53(4): 292-309.
- Singh N, Verma P, Pandey BR, Bhalla M (2012) Therapeutic potential of ocimum sanctum in prevention and treatment of cancer and exposure to radiation: An overview. Int J Pharm Sci & Drug Res 4(2): 97-104.
- Das SK, Vasudevan DM (2006) Tulsi: The Indian holy power plant. Nat Pdt Rad 5(4): 279-283.
- Chattopadhyay RR (1993) Hypoglycemic effect of Ocimum sanctum leaf extract in normal and streptozotocin diabetic rats. Indian J Exp Biol 31(11): 891-893.
- Guan WJ, Ni Z, Hu Y, Liang W, Chun-Quan O, et al. (2020) Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med 382:1708-1720.
- WHO (2020) Coronavirus disease 2019 (COVID-19) situation report 72. Geneva, pp. 1-13.
- Yip MS, Leung HL, Li PH, Cheung CY, Dutry I, et al. (2016) Antibody-dependent enhancement of SARS coronavirus infection and its role in the pathogenesis of SARS. Hong Kong Med J 22(3): 25-31.
- Robinson WE, Montefiori DC, Mitchell WM (1988) Antibody-dependent enhancement of human immunodeficiency virus type 1 infection. Lancet 1(8589): 790-794.
- Robinson WE, Montefiori DC, Mitchell WM, Prince AM, Alter HJ, et al. (1989) Antibody-dependent enhancement of human immunodeficiency virus type 1 (HIV-1) infection in vitro by serum from HIV-1-infected and passively immunized chimpanzees. Proc Natl Acad Sci USA 86(12): 4710-4714.
- Ochiai H, Kurokawa M, Matsui S, Yamamoto T, Kuroki Y, et al. (1992) Infection enhancement of influenza a NWS virus in primary murine macrophages by anti-hemagglutinin monoclonal antibody. J Med Virol 36(3): 217-221.
- Ho MS, Chen WJ, Chen HY, Szu-Fong L, Min-Chin W, et al. (2005) Neutralizing antibody response and SARS severity. Emerg Infect Dis 11(11): 1730-1737.
- Hoffmann M, Kleine-Weber H, Schroeder S, Krüger N, Herrler T, et al. (2020) SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell 181(2): 271-280.
- Xu Z, Shi L, Wang Y, Zhang J, Huang L, et al. (2020) Pathological findings of COVID-19 associated with acute respiratory distress syndrome. Lancet Respir Med 8(4): 420-422.
- Du L, Zhao G, He Y, Guo Y, Zheng B, et al. (2007) Receptor-binding domain of SARS-CoV spike protein induces long-term protective immunity in an animal model. Vaccine 25(15): 2832-2838.
- Tseng CT, Sbrana E, Iwata-Yoshikawa N, Newman PC, Garron T, et al. (2012) Immunization with SARS coronavirus vaccines leads to pulmonary immunopathology on challenge with the SARS virus. PLoS One 7(4): e35421.
- Satyavati GV, Gupta AK, Bhati N (1987) Ocimum Linn. (La-miaceae; Labiateae), in Medicinal Plants of India. Indian Council of Medical Research 2: 354.
- Rai V, Iyer U, Mani UV (1997) Effect of Tulasi (Ocimlllll sanctum) leaf powder supplementation on blood sugar levels, serum lipids and tissue lipids in diabetic rats. Plant Foods Hum Nutr 50(1): 9-16.
- Gupta SK, Prakash J, Srivastava S (2002) Validation of traditional claim of Tulsi, Ocimum sanctum Linn. as a medicinal plant. Indian J Experimental Biology 40(7): 765-773.
- Batta SK, Santhakumari G (1971) The antifertility effect of Ocimum sanctum and Hibiscus Rosa Sinensis. Indian J Medical Research 59(5): 777-781.
© 2022 Thulasi G Pillai. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






