- Submissions

Full Text
Determinations in Nanomedicine & Nanotechnology
“Lean Management”-A Method of Improving Change Management in Healthcare Organizations
Joanna Jasińska*
Department of Social, Computer & Medicine Science, Poland
*Corresponding author: Joanna Jasińska, Department of Social, Computer & Medicine Science, Poland
Submission: January 6, 2020;Published: January 22, 2020

ISSN: 2832-4439 Volume1 Issue5
Abstract
The aim of this article is to present selected ways of developing the management in medical institutions in Poland with the help of Lean Management. The author concentrates on processes of changes in clinical hospitals which include dealing with special tasks in healthcare system, diversity of tasks, medical technology, diversity of relationships with the surrounding, financing from few different sources, limits of resources (especially public ones). The article leads to a conclusion that Lean Management should be a way of thinking.
Introduction
The production management system developed and implemented at the Toyota
concern in the period after World War II was recognized as a kind of miracle in the area of
management systems, enabling the improvement of productivity, quality and efficiency of
enterprises. For years, it was introduced to production systems, as well as in health care and
many entities operating in various sectors of the economy under the name Lean Management,
Lean Production or simply Lean. Lean in management means eliminating losses and any
factors not adding value to a product or service. The key ingredient of Lean is continuous
improvement (kaizen). Niedziółka & Piasek [1]. According to Graban, Lean is a set of tools,
management system and philosophy, whose introduction can change the way of organization
and management of medicinal entities. “A lean system is a method that allows hospitals to
improve the quality of patient care by reducing the number of errors and reducing waiting
times” Graban [2]. Permanent pursuit of perfection in the management of manufacturing
processes is not without a negative impact on the satisfaction of healthcare system employees.
It is often not connected with raising salaries, improving work safety or improving working
conditions.
The purpose of this article is to indicate selected directions for improving change
management in healthcare entities in Poland using the Lean Management concept. Changes in
management were presented in the aspect of restructuring activities undertaken in healthcare
entities. Particular attention will be focused on change processes in multi-specialized
hospitals, which have the following features:
A. Performing specialized tasks in the field of health protection.
B. Multi-tasking.
C. Using highly advanced medical technologies.
D. The multiplicity and diversity of relationships with the environment.
E. Financing from several sources.
Specialist hospitals, due to their organizational complexity, are subject to change
processes, which results not only from legally imposed obligations [Act of 15 April 2011
on medical activities: Dz. Of Laws 2011 No. 112, item 654], but also from the decisions of managers managing entities. These institutions are implementing
changes in the financial and organizational area. The effectiveness
of actions resulting from centrally made systemic decisions aimed
at restoring the financial balance of public health care facilities
in Poland has been undertaken since the 1990s and is now being
continued. As part of the so-called Plan B in the years 2009-2016
[Resolution No. 58/2009 of the Council of Ministers of 27 April
2009 on establishing a multiannual program called ‘Support
for local government units in actions stabilizing the health care
system’]. The restructuring changes program at that time covered
80 independent public health care facilities Rydzewska 2017, p.
179-187.
Despite a number of initiatives at the level of the Ministry of
Health and at the level of management by public local governments
of public health care facilities, their debt not only has not stabilized,
but-as the latest data shows-it increases in the scale of the health
system (Table 1). In view of such facts, it is justified to seek and
implement solutions that are good practices enabling rational and
effective/lean resources of medical organizations while reconciling
the interests of recipients of medical services.
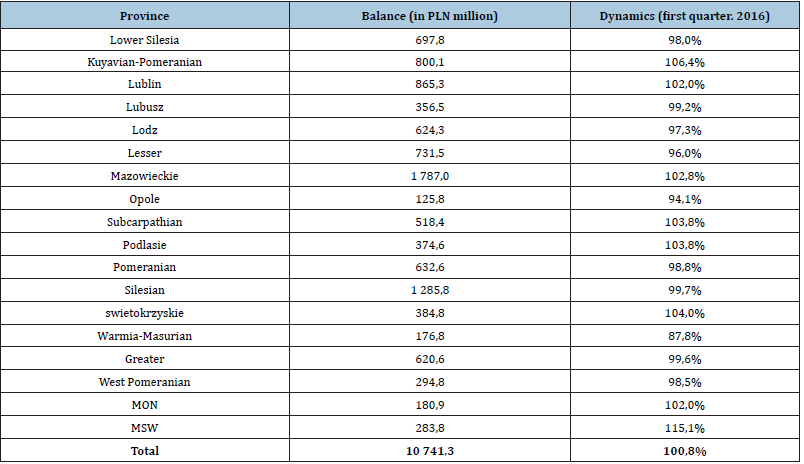
Table 1: The debt of public healthcare institutions in Poland (first quarter 2016).
Source: Dynamics of total SPZOZ liabilities, broken down by voivodships. MZ information based on survey data obtained
from voivodship offices, the Ministry of the Interior, the Ministry of National Defense, medical universities and
SPZOZ supervised by the Ministry of Health, http://www.mz.gov.pl/
Lean Management Concept-Main Assumptions
A number of Lean Management terms have been presented in
the literature. This concept is presented as business management,
which assumes adapting it to market management conditions
based on continuous organization rationalization processes
and its relations with the environment. These processes should
concern the introduction of changes in the organization in terms of
operations, property structure, management, shaping the attitudes
of employees focused on “slimming” the organization Lichtarski
[3]. In another term, the emphasis is on ways of reducing the
cost of generating added value for the customer by rationalizing
employment, infrastructure, expenditure on current and investment
activities, and working time Jones & Womack [4]. The main principle
of Lean Management is primarily the elimination of waste to reduce
the costs of the entity’s operations while ensuring adequate added
value for the client Czerska [5]. In a different approach, Lean
Management is combined with the organization management
method, especially in the process of implemented changes Martínez
& Moyano [6]. It emphasizes rationalization by restructuring the
organization’s resources and the way they are used, taking into
account the conditions arising from its environment. In the term
Lean Management, the role of “slimming” the organization in order
to improve the productivity and quality of products is emphasized
Martínez & Moyano [6].
As it results from the quoted terms, the Lean concept refers to
both the internal elements of the subject and his relationship with the environment in which he operates. It covers activities improving
the quality of products, restructuring the scope of manufactured
products, related to the flattening of organizational structures,
with changes in human resource management and ensuring the
competitiveness of manufactured products. The key concept of
Lean Management is the added value of the product or service for
the recipient, while generating profit for their producer. Obtaining
it requires meeting at least the following conditions:
A. The customer (in the case of health protection, individual
patient or institutional payer-public or private) is willing to pay for
the product,
B. The product (health service) has the value desired by the
customer (it is not defective, has utility value, corresponds to the
health need),
C. The manufacturer (medical entity) rationalizes the use
of production factors (labor input, expenditure on manufacturing
instrumentation, expenditure on infrastructure, proper inventory
rotation).
Understanding the Lean Management principle is a condition
to avoid misunderstanding its essence. Correct interpretation
is associated with its identification with activities aimed at
eliminating waste (from Japanese Muda), and not with austerity
measures consisting in limiting expenditures while providing value
not fully desired for the patient (e.g. limiting the employment of
persons in the positions of medical secretaries assisting the work
of doctors or people working in the registration of medical entities,
resulting in longer queues and patient waiting times, as well as
employee dissatisfaction due to excessive workload). Cholewicka
[7]. The term Muda is combined, among others with: production
of defective products, production of products with low utility and
low efficiency for the recipient, production of often unnecessary
products, inefficient organization of employees’ work resulting
in so-called apparent actions (not having a real purpose), lack
of synchronization in time and space of activities of individual
employees or groups of employees (downtime related to time not
worked effectively, resulting from non-delivery of products by the
previous product manufacturing links).
To sum up, it should be emphasized that the concept of
lean management, especially in the management of healthcare
organizations, should be clearly understood. Elimination of waste
(time, equipment and apparatus, money) should be distinguished
from economical and limiting resources of medical organizations
that cause disruptions in the course of medical processes, extending
patient waiting time, offering defective health services and
dissatisfaction of employees with work overload. Lean Management
as a concept supporting the implementation of changes is not a way
to generate profit at all costs, but is a way to reconcile the demand
side with the supply side through the transformation of assets, the
way of management, organization, relations with the environment
understood not only as a market of health services, but much more
widely ( legislation, competition, outsourcing, general economic
factors).
Principles and Tools of Lean Management in the Aspect of Application in Healthcare Organizations
Creating patient value should be based on several principles of
Lean Management. The rules are as follows:
A. The products are free of defects (benefits having value
for the recipient; benefits not disputed by payers-in accordance
with technological standards, requirements set by payers as to
the qualifications of personnel, medical equipment and apparatus,
infrastructure conditions; benefits corresponding to satisfying a
given health need; no loss of time and material; safe in terms of
health, technology and hygiene for all stakeholders).
B. Solving problems at the place of origin (employees’
readiness to redefine activities and redesign work).
C. Compliance of the performed health service with the
standard way of its performance (if it was developed), objectives,
conditions of implementation.
D. Transparency of relations between producers and
recipients of health services thanks to a properly designed and
constantly improved process of manufacturing and supplying
products; designing roles enabling the production of services
without defects Jimmerson et al. [8].
Techniques leading to the elimination of losses and adapting
business results to external expectations should also be adapted
to the specifics of healthcare organization entities. Selected
techniques include, but are not limited to, techniques that may
prove particularly valuable from the perspective of the effectiveness
of implementing changes in healthcare organizations. These are
among others:
A. Just in Time or production on time-the use of this tool
allows you to eliminate the unjustified expectations of patients,
employees from the same or another organizational unit, recipients,
suppliers, and as a consequence prevents the loss of contracts and
income.
B. Kanban-is a system of signals used in undertaking
individual actions at various stages of product creation (at what
point in time the next health service for the patient is needed,
in which organizational part of the entity, which personal and
material resources are to be used). The condition of introducing
the signal system is to create an undisturbed system of relations
between individual groups of employees or organizational units
of the therapeutic entity leading to the development of principles
of close cooperation and a system of communication between
them. A particularly desirable approach to patient management is
treating the patient care path as an inseparable whole (successive
phases of value creation), which is a condition for determining
the cumulative value (final health effect) of individual services
(medical procedures) performed for the patient. The condition is
cooperation between individual organizational parts of the entity
and a departure from treating services performed by individual
organizational units as final or detached from the final effect for
the patient.
C. Elimination of waste-areas of waste can be: production
of health services that do not correspond to the reported demand,
breaks/downtime between the individual stages of the process of
creating value (the final health effect) for the recipient, unjustified
movement between the stages of creating value (transport of the
patient between parts of the hospital or between hospitals), the
appearance of defects in the manufacturing process or product
(making an incorrect diagnosis based on a faulty performance of
a diagnostic test), unjustified generation of inventory, unnecessary
movement of employees, equipment and apparatus, documentation
and an unfriendly way of delivering products to recipients (failure
to comply with the dates and hours of health service). For exampleobtaining
incorrect results of a patient’s diagnostic examination
requires correction or repetition, i.e. the consumption of additional
material resources and workload, as well as additional control.
This, in turn, can cause “downtime” in other parts of the medical
organization.
D. 5 S (selection, systematics, cleaning, standardization,
self-discipline)-the use of this tool becomes possible to reduce
in-hospital infections, which may also result from irregularities
in waste storage, non-compliance with occupational hygiene,
movement between hospital departments without adequate
protection against exposure to infection biological agents.
E. Creating a value stream map (VSM)-the essence of VSM is
to analyze how to produce and deliver the product to the customer
and identify those activities that add value. The activity that creates
the value of a patient’s medical service is to conduct an interview
with the patient by a nurse, as opposed to providing no interview
with a patient waiting for direct contact with a doctor who only
after entering the office orders or conducts the interview himself.
F. Jidoka-is a way for employees to respond in the event
of problems during the product manufacturing process. Prevents
the penetration of the defective product or its parts into the
next stages of manufacture and subsequent positions, e.g. in the
event of incorrect preparation of the patient for a diagnostic test
or surgery, the employee should break the chain of subsequent
medical activities that may have a defective “effect” of the medical
procedure.
G. To sum up, it should be emphasized that the selection of
tools under the Lean Management concept and the way they are
used must take into account the specifics of a given activity, as well
as adapting them to a given type of therapeutic entity Kubis [9].
Using the Principles Of “Lean” Management in Restructured Healthcare Organizations-Lean Healthcare
The principles of Lean management in health care were adopted to be called Lean Healthcare. They have been introduced in many healthcare organizations in numerous countries De Souza [10]. However, experience shows that only part of the Lean Management tools and methods have been used to improve selected areas of activity of health care entities, especially hospitals. Given the specifics of the healthcare sector and operations, Lean Healthcare has a specific interpretation: a medical entity is an entity that produces specific products-most often they are health services; health service is a manufacturing process; the patient, together with the services provided to him which bring specific health effects, is a product. The applications of Lean Healthcare in healthcare organizations presented in the literature show that it is most often focused on improving the quality of health care (increasing the value of the product for the patient), improving access to health services, improving organizational processes and rationalizing costs. Improving access to healthcare understood as shortening the waiting time for health services, streamlining internal processes related to providing patients with services are the factors that allow rationalization of the costs of medical procedures. By increasing work efficiency, both in terms of health services and support activities (patient registration, referring patients to appropriate organizational units in the hospital)-there is the possibility of shortening expectations for services and improving the economic efficiency of entities. With the high effectiveness of implementing changes, patient waiting times can be reduced by up to 42% [Bernatek 2015, pp. 67-87]. Reducing patients’ waiting time for medical procedures is not the only attribute of high-quality healthcare. It also depends on the method of providing health services, especially in those entities (mainly hospitals) that provide comprehensive care for a package of medical services. Often, due to the nature of the disease, the group of patients requires various activities not only within one ward/hospital department. An example would be elderly patients with chronic diseases. The experience of hospitals indicates that ensuring higher quality of care may depend on the implementation of so-called complex comanaged care depending on the patient’s condition and medical procedures that he needs. This creates a situation in which patients are not exposed to frequent movement between different parts of the hospital (avoiding unnecessary transport) and frequent changes of the staff who care for them. This undoubtedly increases the sense of patient safety Greco et al. [11].
The problem of many healthcare organizations in most health systems is the strong bureaucracy of organizational structures. This is associated with the loss of working time of medical workers, and from the point of view of patients with prolonged paths and time from the moment of issuing the diagnostic test order to its execution and obtaining the test result. Often, the extension of the “path” is associated either with errors in completing order cards or with errors in the performance of the study itself. According to Canadian experience, by optimizing the time spent on organizational processes or activities related to medical diagnostics, hospitals can intensify both human and apparatus work, and thus at the same time provide more health services, which can translate into increased accessibility them (Figure 1); [2].
An additional advantage is the implementation of the same activity with the same measures Villeneuve [12]. The changes inspired by the Lean Healthcare concept, which resulted in a reduction of patients waiting time by 19-24%, were associated with the creation of clear, understandable mechanisms of cooperation between individual employees by defining their roles in the chain of creating value for the patient, creating new principles of employee communication, defining patterns procedures and work schedules, scope of duties and ways of solving current problems. Adaptation of Lean Healthcare in Swedish hospitals has resulted in improved management due to the introduction of work standardization, organizational connections of positions/people working in mutual logical relationships, elimination of unnecessary and disruptive medical procedures, introduction of employee motivation to independently identify problems and overcome them Mazzocato et al. [13] Implementing Lean in Swedish Municipalities and Hospitals.
Figure 1: Impact of lean management on the organization of healthcare [2].
The effectiveness of Lean Healthcare adaptation in
strengthening employee roles in the value creation chain may be
conditioned by transferring greater responsibility for the way the
work is performed and its effects to individual employees who
perceive it as an increased motivation to work Glossmann et al.
[14]. Given the specifics of the tasks performed, the manner of
management in healthcare organizations, and strong restrictions
on their functioning, caused by limited access to public funds, an
approach that can bring good results from the implementation
of Lean principles is the evolutionary approach [Nielsen,
Improving Healthcare through Lean Management: Experiences
from the Danish healthcare system]. In view of the international
experience and conclusions resulting from the implementation
of Lean Healthcare in healthcare entities and the conditions for
the functioning of healthcare organizations in Poland, an attempt
can be made to indicate directions for improving management in
healthcare entities. Particular attention will be focused on specialist
hospitals. The starting point for determining the areas of the
entity’s operations that should become subject to improvement/
restructuring is the diagnosis of the entity’s activities, including:
A. Analysis of the economic situation (basic economic values
and indicators as well as financial statements); in the conditions of
growing financial debt of hospitals in Poland, the scope of analysis
should include: financial efficiency ratios-receivables turnover,
liabilities turnover, inventory turnover; debt ratios-total debt ratio,
equity to liabilities ratio; productivity indicators);
B. Analysis of the causes of the entity’s existing financial
situation (impact of system changes on the entity’s position).
C. Analysis of internal causes of organization and
management irregularities (scope and structure of resources,
degree of their adaptation to conducted activity, allocation of
resources in the entity, organization of work processes, mutual
relations between medical activities).
The conclusions made as a result of the diagnosis should
become the starting point for indicating the directions of improving
the management of the entity. However, creating a uniform list
of directions, or “path of change” for all hospitals is not justified
because existing profile, technological, organizational and financial
differences that generate other problems. Potentially they may
include:
A. Setting priority and other tasks in individual areas of
conducted activity (medical, scientific, didactic) and medical
specialties as well as individual activities constituting their
implementation.
B. Organizational changes, e.g. laboratory diagnostics
combined with a change in the location of diagnostic cells to
reduce costs; allocation of archived documents in one “place” in the
hospital building, which will allow faster access to information and
adaptation of vacant rooms for other purposes.
C. Functional changes-restructuring of hospital beds in
order to adjust the financing bed base (monitoring indicators of
average period of stay of patients, waiting time for admission to a
ward or clinic, the degree of bed use).
D. Resource changes: a combination of clinical units enabling
consistent policy to intensify the use of medical equipment and
apparatus; providing access to the departments’ facilities providing
health services as part of caring for the local population (eliminating
duplication of purchases of the same equipment and apparatus
as well as dispersion of equipment increasing operating costs);
centralization of the distribution of diagnostic base elements.
E. Changes in personal resources in the aspect of assigning
employees to diagnostic, hospitalization and outpatient tasks;
formal assignment of employees to consulting tasks not only within one branch, but also for other organizational units.
F. Eliminating (by pooling) duplication of the same medical
procedures by several hospital organizational units to improve
resource management and eliminate unnecessary manufacturing
factors.
G. Determining the centers of responsibility for the
management of medical equipment and apparatus (taking over
supervision over the management of diagnostic equipment by a
separate department, plant, clinic or clinic).
H. Implementation of new medical technologies enabling
more efficient diagnosis of disease entities, which is associated with
shortening the waiting time for results and the time from diagnosis
to intervention.
I. Implementation of an integrated IT system facilitating
and accelerating the flow of information in the hospital (integrated
management of drugs, medical equipment, centralization of
material management).
J. Implementation of integrated management of medical
materials, medical consumables and medicines.
K. Establishment of cost responsibility centers to strengthen
supervision and eliminate waste.
L. Developing the principles of communication between
the management and employees in order to explain and motivate,
which allows reducing stress and social unrest associated with the
economic uncertainty of the entity.
M. Compliance with the precise implementation of contracts
with payers in order to eliminate any financial sanctions, including
the termination of contracts; particular attention should be focused
on the so-called over-limit benefits.
N. Property restructuring (e.g. when the hospital operates
in several different buildings/rooms distant from each other or
the infrastructure is not used due to poor technical condition) to
eliminate unnecessary usable space and unnecessary transport, to
rationalize maintenance costs and depreciation costs.
O. Outsourcing of non-medical services.
Summary
The effective functioning of medical entities depends not only on the course of internal management processes, but also on the flexible adjustment of their activities to the changing environment. The emergence of new health technologies, changing health exposures not yet occurring or occurring to a limited extent, demographic and epidemiological changes in combination with systemic factors force changes in which the use of “lean management” may be particularly useful. The main directions of improving the functioning of healthcare organizations should be: reducing the time of access to health services by designing an efficient from the point of view of direct recipients of the implementation of activities preceding the performance of health services; this is associated with a smooth transfer of information, e.g. about available places in hospital wards; maximum focus on patients’ expectations, while in the case of financing services from public funds-focus on the implementation of obligations towards public payers (National Health Fund, ministries, local governments), which are related to the implementation of the principles of contracts concluded (comprehensiveness and continuity of care, accuracy of diagnoses , reliability of the use of diagnostic, therapeutic and prophylactic methods, ensuring declared personnel, equipment and infrastructure conditions, maintaining the assumed level of costs and financial result). Ensuring good communication between patients and the medical entity in the scope of providing information at every stage of medical treatment with the patient. Conducting constant analysis of work positions, activities of individual organizational parts of the medical entity in order to formulate current recommendations for employees assuming equal treatment of medical employees and those indirectly involved in the provision of medical services. In addition, care for proper technological preparation, which allows to avoid discouragement of employees and patients as well as the increase of costs and losses, which result, e.g. from poor-quality diagnostic tests results requiring repetition, downtime, cancellations of medical services. It is also important to increase the quality of tasks implemented, which contributes to strengthening the relationship between hospitals and recipients of their products (patients, payers, other medical entities) Sobczak et al. [15].
Even precise determination of directions of changes in health care organizations may not prevent management staff from implementing them incorrectly. The main risks associated with the distortion of the Lean being are most often: identifying the Lean concept with the economic or financial rationalization of the medical entity’s economy, reducing financial liquidity, reducing the quality of services and bypassing legal provisions imposing specific obligations on entities contracting benefits with payers, increasing the level of employee stress and decrease in motivation to work, rationalizing employment by simply limiting it, neglecting the problems of employees with lower qualifications Robbins [16]. According to prof. Zimniewicz [17], the need arises to consolidate the Lean concept as a way of thinking [18-31].
References
- Niedziółka M, Piasek A (2014) Kaizen Costing by the modern method of cost management. Scientific Notebooks of the Podlasie Academy in Siedlce, Series: Administration and Management 81: 79-87.
- Graban M (2014) Lean hospitals: Improving quality, Patient safety, and Employee engagement. (3rd edn), CRC Press, USA, pp. 330-363.
- Lichtarski J (1997) Fundamentals of enterprise science. WAE, Wrocław, Poland, p. 224.
- Jones DT, Womack JP (2014) Slimming companies. CIM, Warsaw.
- Czerska J (2016) More than slimming, i.e. the essence of the Lean management concept. Staff.
- Martínez PJJ, Moyano JF (2014) Lean management, supply chain management and sustainability: A Literature Review. Journal of Cleaner Production 85: 134-150.
- Cholewicka GK (2014) LEAN method-process and product improvement. Quality Problems 1: 21.
- Jimmerson C, Weber D, Sobek DK (2005) Reducing waste and errors: Piloting lean principles at intermountain healthcare. Jt Comm J Qual Patient Saf 31(5): 249-257.
- Kubis N (2015) Lean management tools. Technical and Economic Issues 50(2-3): 291-303.
- De Souza LB (2009) Trends and approaches in lean healthcare. Leadership in Health Services 22(2): 121-139.
- Greco A, Cascavilla L, Paris F, Addante F, Miscio L, et al. (2012) The nephro-geriatric unit in a lean-oriented in-hospital model of care. J Nephrol 25(19): S16-S19.
- Villeneuve C (2014) Fujitsu’s lean solution group-lean healthcare in Canada. Fujitsu Sci Tech 47(1): 41-48.
- Mazzocato P, Holden RJ, Brommels M, Aronsson H, Bäckman U, et al. (2012) How does lean work in emergency care? A case study of a lean-inspired intervention at the Astrid Lindgren Children's hospital, Stockholm, Sweden. BMC Health Serv Res 12: 28.
- Glossmann JP, Schliebusch O, Diehl V, Walshe R (2000) Lean management in hospitals: Potentials and limitations. Med Klin 95(8): 470-473.
- Sobczak A, Rydlewska LI (2012) Occupational health service management-The concept and application of lean management. Med Pr 63(5): 599-606.
- Robbins A (2016) Lean Management and outsourcing. The road to success is to take massive, determined actions. Change management. POU Newsletter, pp. 34-45.
- Zimniewicz K (1999) Contemporary concepts and management methods. Foundations of Management 3(2): 55-64.
- http://www.leancenter.pl/error/nopage
- https://www.diva-portal.org/smash/get/diva2:460019/FULLTEXT01.pdf
- Der-Shin Ke Overwork (2012) Stroke, and Karoshi-death from Overwork. Acta Neurol Taiwan 21: 54-59.
- https://mfiles.pl/pl/index.php/Lean_management
- http://jmf.wzr.pl/pim/2012_1_1_22.pdf
- Izabela RL (2013) Lean management-improving management. Entrepreneurship and Management 14: 275-290.
- Inoue K, Matsumoto M (2000) Karo jisatsu (suicide from overwork): A spreading occupational threat. Occup Environ Med 57(4): 284-285.
- Iwasaki K, Takahashi M, Nakata A (2006) Health problems due to long working hours in Japan: Working hours, workers' compensation (Karoshi), and preventive measures. Ind Health 44(4): 537-540.
- Kawanishi Y (2016) On Karo-Jisatsu (suicide by overwork): Why do Japanese workers work themselves to death? International Journal of Mental Health 37(1): 61-74.
- Nogalski B, Walentynowicz P (2016) Modern management concepts in production companies of the Pomeranian region-an attempt to evaluate. Scientific Notebooks of E. Kwiatkowski University of Business and Administration in Gdynia 7: 14-32.
- Nielsen AP, Improving healthcare through lean management: Experiences from the Danish healthcare system. 5th Nordic Conference on Health Organization and Management, pp. 1-25.
- Uchiyama S, Kurasawa T, Sekizawa T, Nakatsuka HJ (2005) Job strain and risk of cardiovascular events in treated hypertensive Japanese workers: Hypertension follow-up group study. J Occup Health 47(2): 102-111.
- (2011) Medical activities. Journal of Laws No. 112, item 654, Poland.
- Weathers C, North S (2010) Overtime activists take on corporate titans: Toyota, McDonald’s and Japan’s work hour controversy. Pacific Affairs 82(4): 615-636.
© 2020 Joanna Jasińska. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






