- Submissions
Full Text
Developments in Anaesthetics & Pain Management
Emerging Role of Bedside Ocular Ultrasound in Emergency Department and Intensive Care Unit
Surjya Prasad Upadhyay1*, Piyush N Mallick2, Waleed Elmatite3, Vasu Kumar4 and Amit Jain4
1Department Specialist Anaesthesiologist, NMC Hospital, UAE
2Department Consultant Anaesthesiologist, Al Zahra Hospital Sharjah, UAE
3Department Paediatric Anaesthesia, women and child hospital Buffalo, USA
4Specialist Ophthalmology, NMC Hospital, UAE
*Corresponding author: Surjya Prasad Upadhyay, Specialist Anaesthesiologist, NMC Hospital, DIP; Dubai, UAE
Submission: September 10, 2017; Published: January 08, 2018

ISSN 2640-9399 Volume1 Issue1
Abstract
Ultrasonography (US) is being increasingly used outside the radiology suites into various areas like operative room (OR), intensive care (ICU) and emergency department (ED) both as diagnostic tool as well to guide interventions. The popularity and application of US for vascular catheterization, thoracic and abdominal assessment in ED and ICU has increased dramatically over the last decade. The orbital US is one the simple, quick and potential imaging tool to assess not only ocular pathology, but also act as window for intracranial pathology which provide bedside, real time information. Ultrasound has become integral part of ED and ICU and can be applied as bed side point of care in variety of traumatic or non-traumatic ocular condition. This review provides updated information on the emerging application of orbital US in ED and ICU for various ocular and intracranial pathology.
Keywords: Ocular ultrasonography; Ocular trauma; Retinal detachment; Intracranial pressure
Introduction
Ocular Ultrasound is another relatively new application for both emergency and intensive care unit and has been very popular since last decade [1]. This simple procedure not only useful for diagnosing ocular trauma but as window to intracranial pathology [2,3]. Similar to other ultrasonography technique, its non-invasive, bedside, provide real time information and often, the first imaging modality used orbital assessment. Since eye is a fluid filled structure, fluid is a very good conductor of ultrasound waves, therefore ultrasound is an ideal non-invasive tool to scan and assess the entire globe, and it can be used for both traumatic and non- traumatic eye disorder. Orbital ultrasound can be used over a wide range of disease or condition where direct clinical assessment is of little value [4]. Common uses of ultrasound as bedside tool in varieties of clinical condition (Table 1).
Table 1:
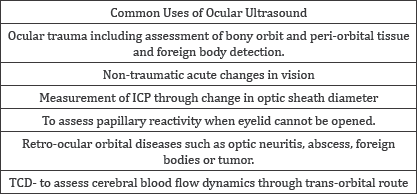
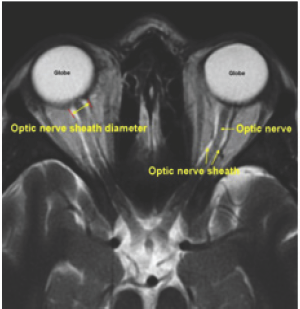
However, ocular ultrasound applications are somewhat unique and not standardized at this time, in order to utilize the full advantage of all possible ocular application of ultrasound, knowledge of examination techniques and sono-anatomy of eye and orbit is required. This article is designed is to provide the information on sono-anatomy, principles, techniques and indications of ocular ultrasound assessment in emergency, intensive care unit and peri-operative uses [5] (Figure 1).
Figure 1: MRI anatomy of the optic nerve and sheath.
Examination Technique
Any modern ultrasound system capable of imaging superficial structure can be used for orbital scanning; however there are dedicated ophthalmic use ultrasound scanners that allow detailed ophthalmic measurement. The detail description of general ophthalmic ultrasound is beyond the scope of this chapter. We will focus mainly on emergency and intensive care unit ultrasound. Because of the relatively shallow depths, small volume of the region of interest and the very low attenuation in ocular media, transducer with higher frequencies are used, most commonly, an 8-14-MHz linear array transducer. Higher frequencies offer better resolution. Newer point of care ultrasound system is acceptable for eye/orbit imaging if equipped with an appropriate transducer. To abide by the current safety standards, a machine should be chosen that displays the safety-related settings: mechanical index (MI) and thermal index (TI) on the screen. In ocular ultrasound sound needs lowest possible TI & MI [6].
Scanning Technique
Patient lie supine with head slightly rotated to the other side to prevent gel pouring. Scanning is done using linear (more than 7.5 MHz) probe after sterile gel over the closed eyelids, a transparent adhesive (tegaderm) can be apply over the closed eye to prevent gel getting inside in case patient open the yes unintentionally. Very gentle pressure application especially in case of trauma to avoid chances of further injury; contraindicated in suspected globe rupture. Transverse and sagittal scans through closed eye eyelid are obtained. Step wise examination Eye lids, Cornea, Anterior chamber, Lens, Posterior chamber, foreign bodies, Vitreous pathology & Retinal detachment, Optic nerve sheath and its diameter. The examination should be performed first in B-mode, with appropriate focus, depth and gain. Focus and depth to be adjusted depending on the depth of segment to be examined. Reducing gain often help to visualize the wall of the globe, foreign bodies, retinal detachment and optic nerve sheath perfectly, while increasing the gain enable visualization of content of vitreou body, masses, tumor etc. [7-9].
The entire globe can be examined in just maneuvers, four dynamic quadrant views and one static slice through the macula and optic disc, known as longitudinal macula (LMAC). The quadrant views are designated as per clock face superimposed on the yes, T12, T3, T6, and T9.
Normal Eye Sono-Anat
Normal Anatomy of eye Figure 2 consist of anterior and posterior chamber, anterior chamber consist of cornea, anterior chamber, iris, ciliary body and lens. The lens is attached to the ciliary bodies at lateral ends. The posterior chamber consists of vitreous, retina, optic disc and posterior ocular wall. Retina anchors posteriorly at the optic disc (Figure 2). On Ultrasound (US) examination, the cornea is seen as most superficial structure as very thin line, below which the anterior chamber is seen as an anechoic structure. The lens is seen as another anechoic structure with very thin anterior and posterior echogenic capsules, the ciliary body can be seen on either side of the lens as hypoehoic structure. Posterior to the lens, the vitreous is seen as large anechoic area. The posterior wall which is comprises odd retinal; choroid and sclera (RCS complex) appear as bright echogenic line that is interrupted by the optic disc or papilla. The optic nerve sheath is can be seen as tubular structure extending posteriorly from the optic disc (Figure 3). Centre retinal artery and vein can be seen on color doppler is helpful in cases of suspected vascular abnormalities like central retinal vessel occlusion, inflammatory diseases and tumors [9] (Figure 3).
Figure 2: Diagram illustrating ocular anatomy; cornea (1), iris (2), ciliary body (3), vitreous chamber (4) posterior ocular wall (5) and optic disc (6).
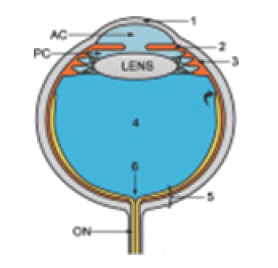
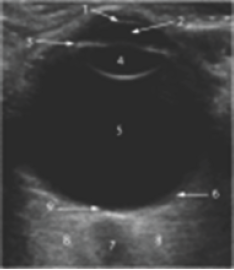
Figure 3: Sonographic appearance of the structures of the normal eye.
The cornea(1), anterior chamber (2), iris (3), lens (4), vitreous chamber (5) The RCS complex (6), optic nerve (ON; 7), retrobulbar fat (8), the optic disc or papilla (9).
Ocular Ultrasonography in Trauma
Orbital ultrasound can be used as point of care bed side tool in emergency and intensive care unit in trauma patients. Many of these patients with orbital trauma will have swollen and edematous lids and often difficult for direct clinical examination. The ability of US to evaluate orbit even in close eye quickly and non-invasively without the need for pupil dilatation makes it a great tool in emergency room and ICU to evaluate several emergent conditions like globe perforation, retro bulbar hematoma, retinal detachment, subluxation of lens, vitrous haemorrhage, foreign body; apart from orbital pathology, it can be used to assess the papiloedema and increasing in intracranial pressure (ICP) [10-15]. Some of the common bedside uses of orbital ultrasound in emergency/ ICU set up are as given below
Papillary Light Reflex
Reviewing of pupilary light reflex (PRL) has great diagnostic and prognostic implication in head trauma [16,17] When direct clinical examination is hindered or not possible due to lid edema, Ultrasound examination in coronal provide the capability of viewing and recording real-time grayscale image of iris and thereby pupilary size and its changes in response to light, which can be recorded also using the M-mode (Figure 4,5).
Figure 4: Probe placement in coronal plane, and US image at Irish lvel showing the pupillary opening.
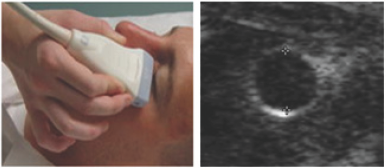
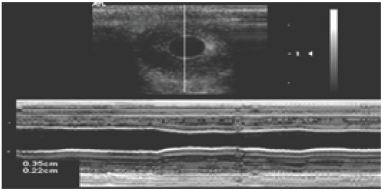
Figure 5: B-mode and M-mode displays of papillary light reflex.
Globe Rupture
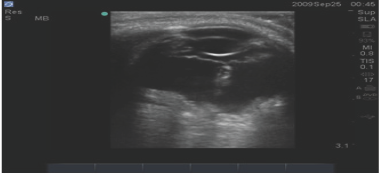
Traumatic rupture of ophthalmic globe is a real emergency as delay in surgical intervention may lead to permanent loss of vision. Bedside ultrasound can be helpful to diagnose globe rupture, especially when abnormalities like corneal edema, hyphema, vitreous hemorrhage or cataract make direct visualization of orbital content difficult. US finding f globe rupture include reduced globe size, collapse of anterior chamber and buckling of sclera. When globe rupture is suspected, the transducer should be placed very gently, rather than applying any pressure on globe, a copious amount of gel can be applied so that the US probe does not actually have to make contact with the eyelid (Figure 6).
Figure 6: Globe rupture: decrease globe size, collapse anterior chamber and buckling of sclera.
Retinal Detachment
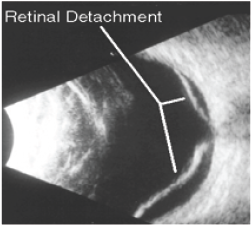
Retinal detachment can be difficult to diagnose clinically when the detachment is small. Retinal tears are often accompanied by vitreous hemorrhage. US finding in retinal detachment include a hyperechoic undulating membrane in the posterior-lateral globe to folded surface attaches to the ora serrata anteriorly and the optic nerve posteriorly (Figure 7).
Figure 7: USG showing Retinal Detachment.
Vitreous Hemorrhage
Vitreous hemorrhage can interfere with vision; even can cause blindness if it is large. The echogenic appearance of vitreous hemorrhage depends on its duration and severity. Fresh small bleed appear as small dots or flakes of low reflective mobile opacities in vitreous chamber. More severe and older hemorrhage, blood organizes and forms like a thick membrane and may settled inferiorly due to gravitational force (Figure 8).
Figure 8: USG image showing small fresh and large organize vitreous hematoma.

Intracranial Pressure and Optic Nerve Sheath Measurement
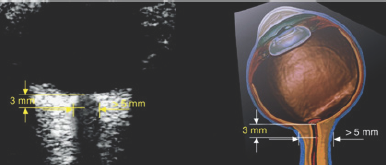
Ocular US can be used to evaluate intracranial pressure (ICP) by measuring the optic nerve sheath diameter (ONSD) even before development of papilloedema which takes several hours to develop. US can be used as point of care for rapid, bedside, non- invasive means of detecting elevated ICP. Optic nerve is attached to the eye ball posteriorly and is covered by optic nerve sheath which is contiguous with the dura mater and has trabeculated arachnoid space through which cerebrospinal fluid (CSF) slowly percolates. The relationship between ONSD and elevated ICP has been well established [13-15]. Normal ONSD measured up to 5 mm in diameter. Adult optic nerve sheath diameter of more than 5.8mm consider positive for intracranial hypertension. The outer border of the arachnoid must be identifiable for actual ONSD measurement; clear, well-focused images must thus allow confident measurement of the inner diameter of the dural sheath [15,18]. As a standard optic nerve sheath diameter is measured at 3 mm away from the optic nerve origin. A position of 3 mm behind the optic disc is recommended because the ultrasound contrast is greatest and the results are more reproducible. At least two measurements are taken and then averaged. Enlarged ONSD is highly coo related with direct measurement of ICP with high specificity and sensitivity of more than 90% [19,20]. A recent study has documented the changes in ONSD measurement reliably and rapidly with changes in ICP [21]. So it can be used as a bedside monitoring for changes in ICP (Figure 9).
Figure 9: Sono-image Optic nerve Sheath Diameter measurement.
Orbital Transcranial Doppler
It is done through the close eye lid by placing low frequency (1-2 MHz) phase array US probe to insonate the ophthalmic artery and carotid siphon [22].
Limitation
Main limitation of ocular US is that it is a technical procedure and require some amount of technical expertise and interpretation are highly operator dependent. US should not be used when there is evidence of globe rupture or impending rupture as pressure over the globe may be detrimental.
Conclusion
Ultrasound has become integral part of emergency and ICU and can be applied as bed side point of care in variety of traumatic or non-traumatic ocular condition.
References
- American College of Emergency Physicians (2009) Emergency ultrasound guidelines. Ann Emerg Med 53(4): 550-570.
- Blaivas M, Theodoro D, Sierzenski PR (2002) A study of bedside ocular ultrasonography in the emergency department. Acad Emerg Med 9(8): 791-799.
- Kilker BA, Holst JM, Hoffmann B (2014) Bedside ocular ultrasound in the emergency department. Eur J Emerg Med 21(4):246-253.
- Dudea SM (2011) Ultrasonography of the eye and orbit. Medical Ultrasonography 13(2): 171-174.
- Kendall CJ, Prager TC, Cheng H, Gombos D, Tang RA, et al. (2015) Diagnostic Ophthalmic Ultrasound for Radiologists. Neuroimaging Clin N Am 25(3): 327-365.
- Fowlkes JB (2008) American Institute of Ultrasound in Medicine Consensus Report on Potential Bio-effects of Diagnostic Ultrasound. J Ultrasound Med 27(4): 503-515.
- De La Hoz Polo M, Torramilans LA, Pozuelo SO, Anguera BA, Esmerado AC, et al. (2016) Ocular ultrasonography focused on the posterior eye segment: what radiologists should know. Insights Imaging 7(3): 351364.
- Berges O, Koskas P, Lafitte F, Piekarski JD (2006) Sonography of the eye and orbit with a multipurpose ultrasound unit. J Radiol 87(4 Pt 1): 345353.
- Belden CJ, Abbitt PL, Beadles KA (1995) Color Doppler US of the orbit. Radio graphics 15(3): 589-608.
- Sargsyan AE, Dulchavsky AG, Adams J, Melton S, Hamilton DR, et al. (2008) Ultrasound detection of simulated intra-ocular foreign bodies by minimally trained personnel. Aviat Space Environ Med 79(1): 58-61.
- Chiao L, Sharipov S, Sargsyan AE, Melton S, Hamilton DR, et al. (2005) Ocular examination for trauma; clinical ultrasound aboard the International Space Station. J Trauma. 58(5): 885-889.
- Blaivas M (2000) Bedside emergency department ultrasonography in the evaluation of ocular pathology. Acad Emerg Med 7: 947-950.
- BlaivasM, TheodoroD, SierzenskiPR (2003) Elevated intracranial pressure detected by bedside emergency ultrasonography of the optic nerve sheath. Acad Emerg Med 10(4): 376-381.
- DubourgJ, JavouheyE, GeeraertsT, Messerer M, Kassai B (2011) Ultrasonography of optic nerve sheath diameter for detection of raised intracranial pressure.a systematic review and meta-analysis. Intensive Care Med 37(7): 1059-1068.
- Amini A, Kariman H, Arhami Dolatabadi A, Hatamabadi HR, Derakhshanfar H, et al. (2013) Use of the sonographic diameter of optic nerve sheath to estimate intracranial pressure. Am J Emerg Med 31(1): 236-239.
- Schreiber MA, Aoki N, Scott BG, Beck JR (2002) Determinants of mortality in patients with severe blunt head injury. Arch Surg 137(3): 285-290.
- The Brain Trauma Foundation (2000) The American Association of Neurological Surgeons. The Joint Section on Neurotrauma and Critical Care. Papillary diameter and light reflex. J Neurotrauma 17: 583-559.
- Tayal VS, Neulander M, Norton HJ, Foster T, Saunders T, et al. (2007) Emergency department sono-graphic measurement of optic nerve sheath diameter to detect findings of increased intracranial pressure in adult head injury patients. Ann Emerg Med 49(4): 508-514.
- Soldatos T, Karakitsos D, Chatzimichail K, Papathanasiou M, Gouliamos A, et al. (2008) Optic nerve sonography in the diagnostic evaluation of adult brain injury. Crit Care 12(3): R67.
- Kimberly HH, Shah S, Marill K, Noble V (2008) Correlation of optic nerve sheath diameter with direct measurement of intracranial pressure. Acad Emerg Med 15(2): 201-204.
- Singleton J, Dagan A, Edlow JA, Hoffmann B (2015) Real-time optic nerve sheath diameter reduction measured with bedside ultrasound after therapeutic lumbar puncture in a patient with idiopathic intracranial hypertension. Am J Emerg Med 33(6): 860.e5-7.
- Soldatos T, Karakitsos D, Wachtel M, Boletis J, Chatzimichail K, et al. (2010) The Value of Transcranial Doppler Sono-graphy With a Transorbital Approach in the Confirmation of Cerebral Circulatory Arrest. Transplant Proc 42(5): 1502-1506.
© 2018 Surjya Prasad Upadhyay, et al. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






