- Submissions

Full Text
COJ Nursing & Healthcare
The Nursing Diagnosis Development of Internet Addiction: Content Validation with Nursing Experts
Ester Gilart Cantizano, María Dueñas and Anna Bocchino*
Nursing Faculty, Clínica Salus Infirmorum, University of Cádiz, Spain
*Corresponding author: Anna Bocchino, Nursing Faculty, Clínica Salus Infirmorum, University of Cádiz, Cádiz, Spain
Submission: July 01, 2019;Published: December 17, 2019

ISSN: 2577-2007Volume5 Issue5
Abstract
Purpose: This study aimed to validate the definition and define the characteristics and related factors of Internet Addiction, a proposed nursing diagnosis.
Methods: Using Fehring’s diagnostic content validity model, Spanish experts were asked to assess the adequacy of the label, defining its characteristics and other related factors.
Findings: The content validity index was 0.79. A total of 19 defining characteristics were validated by the experts.
Conclusion: The present study supports the proposed development of a nursing diagnosis for Internet Addiction.
Practice implications: The results suggest that the inclusion in the NANDA-I taxonomy of the validated nursing diagnostic version of “Internet Addiction” would allow nursing professionals to identify the disorder and its causes and manifestations, and therefore provide the information needed to plan relevant interventions and results.
Objective: Validation of the definition, defining characteristics and related factors on internet addiction, a proposal for a nursing diagnosis.
Methodology: Using Fehring's content validation model, the denomination of the label, the defining characteristics and other related factors were agreed by Spanish experts.
Result: The global content validity index was 0.79. A total of 19 defining characteristics were validated by the experts. Conclusion: This study supports the proposal to develop a nursing diagnosis for Internet Addiction.
Practical implications: The results obtained suggest that the inclusion in the NANDA-I taxonomy of the diagnosis "Internet addiction" would allow nursing professionals to identify the problem, its causes and manifestations, and therefore provide the necessary information to plan interventions and most relevant results.
Keywords: Nursing diagnosis; Validation; Internet addiction
Purpose and Objectives
Pathological Internet Use (PIU) and Internet Addiction (IA) are the most recent terms used to describe the excessive and inappropriate use of certain applications, such as the internet and social networks, etc., with significant implications for an individual’s physical, cognitive, emotional and social health [1-4].
The concept of IA is conceptualised as an impulse-control disorder and regarded as a taxonomy of behavioral addiction [5-7]. Much of the recent literature in this realm has shown that excessive use of the internet can cause a pattern of behavior similar to substance addictions [8-11]. Indeed, in the new edition of the International Classification of Diseases (ICD-11), the WHO task force is considering the integration of behavioral addictions with a new diagnostic category, of which computer and IA is a subcategory [12].
However, there is still debate and controversy surrounding this concept within the academic community, in which researchers acknowledge much conceptual disparity and the need for further work to fully understand IA and its constituent disorders [13].
Even without the official recognition of IA and the associated disagreement over its diagnostic criteria, it is considered to be a behavioral addiction, the prevalence of which seems to be increasing [14-17]. Social and behavioral scholars generally concur that there is an IA phenomenon that causes unhealthy [18-20]. In this respect, several authors [21,22] have reported a significant co-morbidity of IA with neurological complications, psychological distress, social problems and health problems, especially in teenagers and young adults [23,24].
Researchers agree on the need to have valid and reliable measurement instruments and solid theoretical models that make it possible to understand the characteristics, correlations and consequences of this problem [25]. For this, it is necessary to have an integral knowledge of the problem in terms of not only its descriptive variables, but also its explanatory ones, which initially passes through the identification of the variables associated with the problematic use of the internet.
Several cross-sectional studies have indicated notable associations between the excessive use of the internet and anxiety [26-30], cravings [31], hostility [32], insomnia [33-36], distress [26,34], low self-esteem [13,37,38], irritability and nervousness [8,39]. Scientific evidence shows that the negative repercussions of the excessive use of the internet are likely to cause other serious psychological effects in the individual, such as aggressive behavior, a loss of control and impulsivity [12,28,40].
According to numerous studies, IA negatively affects the overall school performance of adolescents [18], considerably interferes with everyday occupational activities and thus dramatically and negatively affects relationships and interactions with family and friends [14,18,28,30,33,39,41-44].
Furthermore, it is worth highlighting the correlation between pathological and maladaptive internet and endocrine conditions (psychomotor agitation and pulse acceleration) [26,28,30].
All proposed studies have drawn attention to noteworthy aspects, which in part explain the negative effects that arise as a result of IA. In this regard, for there to be an addiction, several factors must come together, including depression [45-47], social isolation [20], social phobia [41], risk of suicide [33], negative effects on diet and physical activity [46,48] and unhealthy behaviors (alcohol and/or other substances) [33,49,50].
Nonetheless, despite the numerous studies on the topic (or perhaps because of them), to date, a generally accepted definition and diagnosis have not yet been determined. In addition, despite the presence of problems of both a conceptual and methodological nature which make it difficult to arrive at definitive conclusions, numerous studies have determined the risks and negative consequences in respect of an individual’s biopsychosocial health as a result of an addiction to the internet. In this regard, it is fitting to question the role that nursing professionals assume in this context because the implementation of preventative actions for the care and treatment of both individuals, and their respective families, who suffer from addiction’s negative consequences becomes fundamental.
To provide quality care, nurses should be able to safely utilize their clinical skillset to recognize and diagnose the patient’s actual or potential response to a condition. The systematic use of the NANDA-I taxonomy would provide the information needed to plan more relevant nursing interventions to successfully realize nursing responsibilities [51]. Nonetheless, in practice, conditions arise that are very difficult to distinguish due to the interactions of different variables and perhaps even variables disguised as other types of physical or psychological illnesses.
Thus, it becomes necessary to create a new diagnostic label related to Internet Addiction because the use of standardized scientific language may be the catalyst that enables the approach from theory to practice and, therefore, the necessary feedback to provide systematic high-quality care based on evidence. The nurse taxonomy that has been used is the North American Nursing Diagnosis Association-International [52] version, organized by concepts according to the domains of Taxonomy II, which have been considered Domain 9 (coping-tolerance to stress) and Class 2 (coping responses). To date, in the NANDA-I taxonomy or in the International Classification for Nursing Practice (ICNP), there is no diagnostic label that refers to the Internet Addiction person’s biopsychosocial condition.
Moreover, a tour of the evaluation/measurement methods of the defining characteristics (DCs), the related factors (RFs) and the condition’s impact on individuals and families shows the existence of tools focused on the evaluation/measurement of each characteristic/factor but not the existence of a specific evaluation tool for diagnosis in this group.
Currently, the taxonomy contains 244 diagnoses that must undergo a continuous process of review and improvement to be adapted to daily practice by nurses around the world and to increase its level of scientific evidence. For this work to be possible, it is necessary for diagnoses to demonstrate their adaptation to practice, meaning that they are validated in different contexts, situations and theoretical models determined through research. Despite this necessity and the references by both multiple authors [53-56] and the NANDA-I itself, to consider the validation of diagnoses as a priority issue to achieve an improvement in care and greater professional development, these types of studies are clearly insufficient at an international level [57] and almost non-existent at the national level. Therefore, validation requires an evidence-based response agreed upon by the scientific community, enabling us to offer high-quality, comprehensive and systematized care [58-60]. Within this context, the aim of the present paper is the content validation of a new diagnostic label for use in clinical and healthcare practice.
The specific objectives are as follows:
- The content validation of a new diagnostic label whose definition is as follows: a pathological mental and physical state characterized by habits of unhealthy behaviors related to the uncontrolled use of the Internet.
- To determine the degree of representativeness of each of the DCs of the proposed label.
- To determine the degree of representativeness of the other factors related to the proposed label to evaluate the need for inclusion of the diagnosis in the NANDA-I classification.
Methodology
To validate the nursing diagnosis of the NANDA-I, the diagnostic label should be agreed upon based on its definition and the content of its DCs; additionally, RFs should be confirmed as representative by a group of experts. This study is a two-part study that includes concept analysis, based on the method proposed by Walker & Avant [61], followed by diagnostic content validation, adapted from the method proposed by Fehring [62].
Phase 1: Name of the diagnostic label based on the definition
Design: An exploratory, descriptive and diagnostic content validation study in which the diagnostic label was agreed upon by a panel of experts and the Delphi technique based on the following definition: “pathological, mental and physical state characterized by habits of unhealthy behaviors related to [the] uncontrolled use of Internet”.
Phase 2: Validation of diagnostic content
Design: Once the label was defined, an exploratory, descriptive and diagnostic content validation study was conducted, following the model proposed by Fehring [62,63], in which the DCs and RFs that were proposed for the diagnosis, according to the literature, were confirmed as representative by a group of experts, thus obtaining the degree to which each DC and RF are indicative of the given diagnosis.
Population and sample: A convenience sample of expert nurses in the area of the most prevalent diagnosis, community, family and psychosocial nursing was selected.
Inclusion, exclusion, and eligibility criteria: The following inclusion criteria were established:
- Possessing a degree of nursing in community, family or psychosocial nursing;
- A minimum of 2 years of professional experience in these areas; and
- A minimum of 2 years of professional experience in university teaching in an area of community or psychosocial nursing. Refusal to participate in the study was considered an exclusion criterion.
The eligibility criteria were to meet at least one of the inclusion criteria and not to meet the exclusion criterion. Origin and recruitment of the sample: The sample was recruited through e-mail communication with nurses related to the area of community, family and psychosocial nursing; and with collaborators of the research group, whose cooperation to recruit professionals was requested. Instruments and variables: Two questionnaires were created for data collection. First, to agree on the diagnostic label of the proposed definition, the instrument for information collection was a structured survey that was divided into the following sections: sociodemographic variables and the definition of a diagnostic label that the panel experts should name. In the first round, the diagnostic label was selected from the definition by a consensus of experts; in the second phase, a new survey, in which the lists of DCs and RFs were included to identify those that were most representative, was sent to the experts again. The questionnaires were produced on paper and online through the Survey Monkey tool, whose link to the questionnaire was sent through e-mail.
The collected variables are described below:
Sociodemographic variables: Sex (male, female), age, academic degree (nurse, nurse practitioner, university expert/unofficial master’s, official master’s, doctoral programmed, doctorate), position at the institution where he/she works (nurse, nurse case manager, coordinator, teacher) and length of time in the position (years and months).
DCs of the diagnosis agreed upon by experts as “IA”: The following list of 19 identified DCs was presented as the most important identified in the literature: low self-esteem, pulse acceleration, psychomotor agitation, insomnia, cravings, distress, hostility, deterioration of social relations, deterioration of family relations, deterioration of occupational activities, deterioration of academic performance, nervousness, anxiety, irritability, impulsivity, loss of control, aggressive behavior, lack of attention and decrease in concentration. Participants were required to identify those that, according to their experience and/or professional opinion, were most representative or characteristic of those that occur in people to whom the diagnosis could be applied. To that end, they were instructed to indicate the option that they considered most appropriate for each of the DCs from among the following: not at all representative, a slightly representative, moderately representative, substantially representative and totally representative.
RFs of the proposed diagnosis: The following list of six identified RFs was also presented as the most important identified in the literature: depression, social isolation, social phobia, risk of suicide, negative effects on diet and physical activity and unhealthy behaviors (alcohol and/or other substances). As with the DCs, the participants were required to rate their representativeness by indicating the option that they considered to be most appropriate for each of them.
Data Analysis
The data were analyzed using the Statistical Package for the Social Sciences 21.0 (SPSS, Chicago, IL). First, a descriptive analysis of the sociodemographic variables was performed, expressing the quantitative variables in terms of frequency and percentage and the qualitative variables in terms of mean and standard deviation. For phase 1, regarding choosing the diagnostic label for the proposed definition, a consensus was reached through the categorization of proposed labels by the experts based on the definition, and the “units of context” (which are the smallest pieces of information) were analyzed; the information from the experts was systematized, choosing the most frequently proposed information as the final label.
For phase 2, the method proposed by Fehring was followed to calculate the weights for each DC, thus yielding the diagnostic content validity (DCV). To determine the level of representativeness of each DC, a weight was assigned to each of the expert’s values such that “not at all representative” equaled 0, “a slightly representative” equaled 0.25; “moderately representative” equaled 0.50; “substantially representative” equaled 0.75; and “totally representative” equaled 1. The weighted average of the scores attributed to each of the DCs was calculated and represents the DCV index, achieving values from 0 to 1. If the score was greater than or equal to 0.8, the DC was considered to be highly representative of the diagnosis and catalogued as “major”. DCs with ratios of less than 0.80 but greater than 0.50 were considered to be low representatives and labelled as “minor”. DCs obtaining values less than or equal to 0.5 were considered not representative and were therefore discarded. The proposed RFs were analyzed in a manner analogous to the described procedure.
Once the weights corresponding to each of the DCs were assigned, the degree of representativeness of the full diagnostic content for IA was assessed by calculating the overall DCV index. This index indicates how confident a practitioner should be when using the diagnosis for a particular patient. The higher the score, the more confident practitioners were in a diagnosis. When a NANDA diagnosis has more than seven DCs, it is recommended that they follow the amendments proposed by Sparks and Lien-Gieschen [64] to the original method by Fehring [62,63]. Because this is the case in the diagnosis of IA, these authors’ premises were used for this study. They proposed calculating the overall DCV index by counting the scores of the major DCs twice and the minor DCs once and then determining the arithmetic mean of each to avoid any artificial decreases. If the result is lower than 0.6, the diagnosis should be considered not representative in cases of IA, whereas if it is greater than 0.8, the diagnosis should be considered representative. In the case of obtaining a final value between 0.6 and 0.79, the degree of representativeness of the diagnosis cannot be determined, requiring further study to obtain decisive results.
Findings
Characteristics of the sample
The final sample was composed of a total of 148 experts, with the majority being female (75%) and having a mean age of 44.68 years (SD=10.98). The mean length of experience in the position was 16.74 years (SD=11.70). With respect to educational background, 78.38% possessed a nursing degree, 8.11% were nurse practitioners and 13.51% had some type of graduate education (university expert, master’s, doctoral programmed or doctorate). Regarding the position in the institution, 86.49% were nurses, 1.35% were case managers, 4.05% were coordinators and 8.11% were teachers.
Phase 1: Diagnostic label based on the definition
The names proposed by experts for the diagnostic label underwent categorization through an analysis of the “units of context”; the results showed that the proposed categories were the Inappropriate Use of the Internet, Internet Addiction, New Technological Stress and the Abuse of the Internet.
Of the four options provided, the label that was least preferred by experts was “Abuse of the Internet”, which was proposed by only 8.11%, followed by “New Technological Stress” (9.46%); 20.95% proposed “Inappropriate Use of the Internet”. The experts expressed a greater preference (61.49 %) for the label “Internet Addiction”, which was assigned to the proposed definition.
Phase 2: Validation of the DCs
With regard to the DCs, of the 19 proposed DCs for the diagnosis, all were validated by the experts, obtaining scores greater than 0.5. Nine were significant DCs, of which higher scores were obtained for the following DCs: deterioration of social relations (0.8615), deterioration of family relations (0.8514) and lack of attention (0.8429). With respect to the minor characteristics, the low self-esteem DC scored the lowest, achieving only 0.6267. The overall content validity index for the diagnostic label was 0.79. The DCV index achieved by each DC is presented in Table 1.
Table 1: Diagnostic content validity score for the defining characteristics.
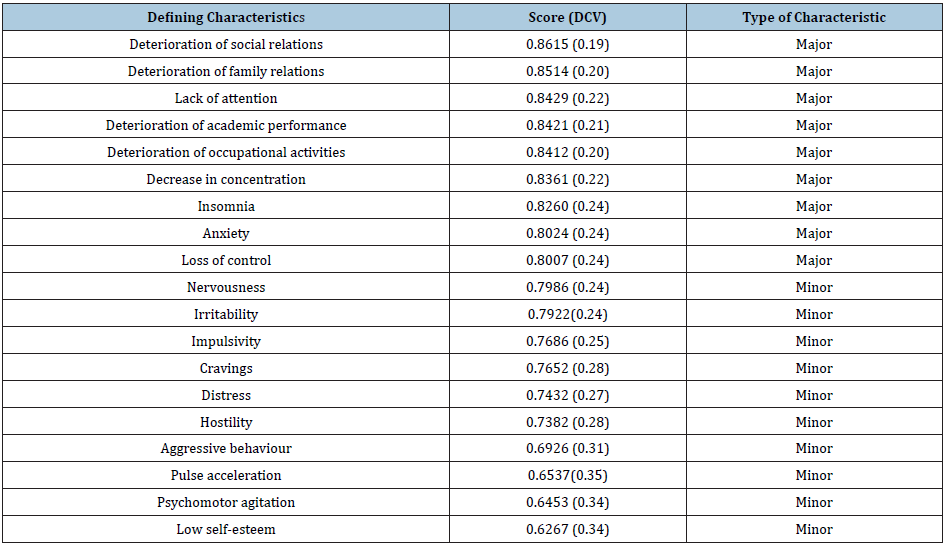
With regard to the RFs, five of the six RFs proposed were considered validated, with social isolation obtaining the highest score (0.85), followed by social phobia (0.80), negative effects on diet and physical activity (0.74), depression (0.70) and unhealthy behaviors (alcohol and/or other substances) (0.64). Table 2 details the obtained results.
Table 2: Content validity score for the related factors.
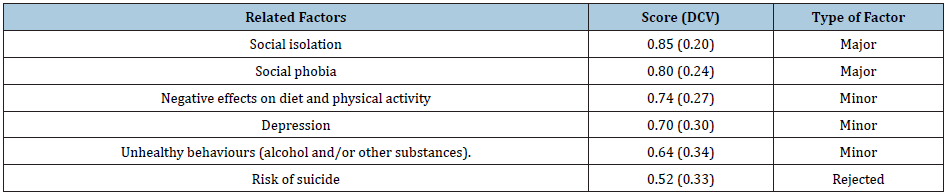
Discussion
The main objective of this study was the proposal and content validation of a new diagnostic label for the NANDA-I “Internet Addiction” (61.49%), under the modality of content validity evidence. The overall content validity index obtained for the DCs was 0.79 (0.20); according to the model adopted by Sparks and Lien-Gieschen [64], the diagnostic label is therefore considered valid for content representatives to accept the diagnosis as validated.
Referring to the representativeness of the DCs considered by the experts as indicative for the diagnosis, of the 19 proposed DCs, all were validated and satisfactorily covered the spectrum of validated and evaluated diagnostic content. This result confirmed what had already been highlighted in literature: it would be possible to affirm that there are clinical manifestations that are characterized as the addiction to Internet diagnosis.
In this regard, deserve reflection the manifestations considered by the experts as major or greater frequency in individuals displaying this addictive behavior. When examining, for example, the high occurrence of the “deterioration of social relations” (0.8615), “deterioration of family relations” (0.8514), “deterioration of academic performance” (0.8421) and “deterioration of occupational activities (0.8412) DCs; these results are not surprising, considering the numerous studies [18,33,41,44] that show the clear and related presence of these characteristics in individuals that have this type of addiction.
These people have unhealthy behaviors across different environments and situations, such as the family home, for example, when individuals refuse to leave their bedroom or cooperate in family activities; in the school environment through low academic performance; and in the work environment, using work activities and as a result shown in the same low performance.
These manifestations, in turn, are related and sharpen the characteristics of "lack of attention" (0.8429) and "decrease in concentration" (0.8361), which are also greatly valued by experts. The DCs “insomnia” (0.8260), “anxiety” (0.8024) and “loss of control” (0.8007) were also considered critical by the experts. The selection by the experts of a large number of DCs representative of IA shows the great impact of the biopsychosocial model on people who experience it, which is reflected in three macro categories in the symptoms exhibited as physical, psychological and social manifestations [28,33]. In this model, the negative impacts that affect an individual addicted to the internet is manifested at both the physiological and psychological levels. In this regard, one of the physiological consequences that should be considered at the time of the evaluation of addiction is that the sleep-wake rhythm is unbalanced since individuals that have these types of addictive behaviors forego sleep to remain connected to the internet. In addition, the most common psychological consequences should be noted, such as anxiety, loss of control and/or an inability to reduce their excessive and inappropriate use of these technologies.
On the other hand, the DCs, “pulse acceleration” (0.6537), “psychomotor agitation” (0.6453), “aggressive behavior” (0.6926), “cravings” (0.7692), “irritability” (0.7922) and “nervousness” (0.7986) were considered to be minor to the “IA” diagnostic label. A questionable fact considered that many of these manifestations are supported by other studies that put of manifest the existing relationship between this addiction and the proposed characteristics [26,28,30,39].
In relation to the analysis of corroborated etiological or RFs, according to the referenced literature [33,41,46], five of the six proposed RFs were considered validated, "risk of suicide" (0.52) being dismissed by the lack of consensus. This result could be explained by the fact that the experts have not considered it to be specific or exclusive to this nursing diagnosis, given that it can be even more representative of other diagnostic labels. Although it is true that this characteristic does not have a directly proportional relationship with the proposed label, it was included because there was empirical evidence of its relationship with the addiction.
In addition, it should be noted that the factor that scored highest was "social isolation" (0.85), likely because it was considered by experts as the most relevant given its existing relationship with the "deterioration of social relations" characteristic. Despite the results, the collected data are limited by inherent deficits in the validation model used, the origin and the system of their selection, and in some no conformity was detected in the translation of the taxonomy. The DCV only indicates what a group of experts thinks; it does not have the assurance that their judgments agree with the phenomenon, and no direct information is collected in real time with the patients [65]. After the DCV, it becomes necessary to conduct clinical validation studies and construct validity studies [66-70].
Conclusion
As indicated above, IA generates various health problems in the individual [2,4]. The interest that the issue has raised in the past few decades has generated numerous studies [5] that have attempted to measure the true extent of the problem and to assess whether IA could or could not be a type of public health problem. In this context, in the present project it was possible to validate the content of the new diagnostic label “IA” not present in the diagnostic taxonomy of the NANDA-I, as well as the identification of the majority of its defining characteristics and factors related to the literature.
Implications for Nursing Knowledge
The results suggest that the inclusion of the NANDA-I taxonomy of the validated nursing diagnostic version of “IA” would provide nursing professionals with the ability to name a health problem that they observe and attend to in a standard manner in their clinical practice. This ability would warrant the planning of more effective care because nursing diagnoses are tools that help identify a problem, its causes and its manifestations and, therefore, would provide the information needed to plan the most specific interventions in both clinical and evidence-based practice.
References
- Fernández MJ, Peñalva A, Irazabal I (2015) Habits of use and risk behaviors on the Internet in preadolescence. Communicate 22(44):
- Lam LT (2014) Internet gaming addiction, problematic use of the Internet, and sleep problems: A systematic review. Curr Psychiatry Rep 16(4): 444.
- Marín Díaz V, Requena SB, González MJM (2015) Are university students addicted to social networks? Complutense Journal of Education 26: 233-251.
- Surià R (2015) Disability in young people, the risk of excessive Internet use? Health and Addictions 15(1): 15-24.
- Carbonell X, Fúster H, Chamarro AY, Oberst U (2012) Internet and mobile addiction: A Review of Spanish empirical studies. Roles of the Psychologist 33(2): 82-89.
- García del Castillo JA (2013) Technological addictions: The rise of social networks. Health and Addictions 13(1): 5-14.
- Roberts JA, Pirog SF (2013) A preliminary investigation of materialism and impulsiveness as predictors of technological addictions among young adults. J Behav Addict 2(1): 56-62.
- Echeburúa E, Corral P (2010) Addiction to new technologies and social networks in young people: a new challenge. Addictions 22(2): 91-95.
- Grant JE, Potenza MN, Weinstein A, Gorelick DA (2010) Introduction to behavioural addictions. The American Journal of Drug and Alcohol Abuse 36(5): 233-241.
- Han DH, Bolo N, Daniels MA, Arenella L, Lyoo IK, et al. (2011) Brain activity and desire for Internet video gameplay. Comprehensive Psychiatry 52(1): 88-95.
- Spada MM (2014) An overview of problematic Internet use. Addict Behav 39(1): 3-6.
- Mann K, Fauth Bühler M, Seiferth N, Heinz A (2013) The concept of behavioural addiction and limits of the term addiction. Nervenarzt 84(5): 548-556.
- Griffiths MD, Kuss DJ, Demetrovics Z (2014) Social networking addiction: An overview of preliminary findings. In: Rosenberg K, Feder L (Eds.), Behavioural Addictions, New York, USA, pp. 119-141.
- Derbyshire KL, Lust KA, Schreiber LRN, Odlaug BL, Christenson GA, et al. (2013) Problematic Internet use and associated risks in a college sample. Compr Psychiatry 54(4): 415-422.
- Jelenchick LA, Becker T, Moreno MA (2012) Assessing the psychometric properties of the Internet addiction test (IAT) in US college students. Psychiatry Res 196(2-3): 296-301.
- Li W, Garland EL, Howard MO (2014) Family factors in Internet addiction among Chinese youth: A review of English- and Chinese-language studies. Comput Human Behav 31: 393-411.
- Weinstein A, Lejoyeux M (2010) Internet addiction or excessive internet use. Am J Drug Alcohol Abuse 36(5): 277-283.
- Stavropoulos V, Alexandraki K, Motti F (2013) Recognising internet addiction: prevalence and relationship to academic achievement in adolescents enrolled in urban and rural Greek high schools. J Adolesc 36(3): 565-576.
- Petry NM, Rehbein F, Gentile DA, Lemmens JS, Rumpf HJ, et al. (2014) An international consensus for assessing internet gaming disorder using the new DSM‐5 approach. Addiction 109(9): 1399-1406.
- Yao MZ, Zhong ZJ (2014) Loneliness, social contacts and Internet addiction: A cross-lagged panel study. Computers in Human Behaviour 30: 164-170.
- Pontes HM, Kuss DJ, Griffiths MD (2015) Clinical psychology of Internet addiction: a review of its conceptualisation, prevalence, neuronal processes, and implications for treatment. Neuroscience & Neuroeconomics 4: 11-23.
- Uddin MS, Mamun AA, Iqbal MA, Nasrullah M, Asaduzzaman M, et al. (2016) Internet addiction disorder and its pathogenicity to psychological distress and depression among university students: A cross-sectional pilot study in Bangladesh. Psychology 7(8): 1126-1137.
- Kuss DJ, Griffiths MD, Binder JF (2013) Internet addiction in students: Prevalence and risk factors. Computers in Human Behaviour 29(3): 959-966.
- Kuss DJ, Rooij VAJ, Shorter GW, Griffiths MD, van de Mheen D (2013) Internet addiction in adolescents: Prevalence and risk factors. Computers in Human Behaviour 29(5): 1987-1996.
- Tao R, Huang X, Wang J, Zhang H, Zhang Y, et al. (2010) Proposed diagnostic criteria for internet addiction. Addiction 105: 556-564.
- Berner JE, Santander J (2012) Internet abuse and dependence: the epidemic and its controversy. Journal of Neuro Psychiatry 50(3): 181-190.
- Echeburúa E, Labrador F, Becoña E (2010) Addiction to new technologies. Pirámide, Madrid, Spain.
- Escurra MM, Salas BE (2014) Construction and validation of the social network addiction questionnaire (ARS). Liberabit 20(1): 73-91.
- Lee BW, Stapinski LA (2012) Seeking safety on the internet: Relationship between social anxiety and problematic internet use. J Anxiety Disord 26(1): 197-205.
- Vilca LW, Gonzales G (2011) Construction of the social network addiction risk questionnaire (CrARS). In: Lima: General Directorate of Research, I National Research Congress, Union Peruvian University, Peru.
- Becoña IE, Cortés TM (2016) Addictions manual for psychologists’ specialists in clinical psychology in training.
- Adalıer A, Balkan E (2012) The relationship between internet addiction and psychological symptoms. International Journal of Global Education 1(2): 42-49.
- Heo J, Oh J, Subramanian SV, Kim Y, Kawachi I (2014) Addictive internet use among Korean adolescents: a national survey. PloSone 9(2): e87819.
- Thomée S, Härenstam A, Hagberg M (2011) Mobile phone use and stress, sleep disturbances, and symptoms of depression among young adults - a prospective cohort study. BMC Public Health 11(1): 66.
- Kormas G, Critselis E, Janikian M, Kafetzis D, Tsitsika A (2011) Risk factors and psychosocial characteristics of potential problematic and problematic internet use among adolescents: a cross-sectional study. BMC Public Health 11(1): 595.
- Xu J, Shen L, Yan C, Hu H, Yang F, et al. (2012) Personal characteristics related to the risk of adolescent Internet addiction: a survey in Shanghai, China. BMC Public Health 12: 1106.
- Casas JA, Ruiz-Olivares R, Ortega RR (2013) Validation of the internet and social networking experiences questionnaire in Spanish adolescents. International Journal of Clinical and Health Psychology 13(1): 40-48.
- Herrera HMF, Pacheco MMP, Palomar LJ, Zavala AD (2010) Facebook addiction related to low self-esteem, depression and lack of social skills. Psicología Iberoamericana 18(1): 1-18.
- Echeburúa EY, Requesens A (2012) Addiction to social networks and new technologies in youth and adolescents. Guide for educators. Pyramid, Madrid, Spain.
- Lee HW, Choi JS, Shin YC, Lee JY, Jung HY, et al. (2012) Impulsivity in Internet addiction: A comparison with pathological gambling. Cyberpsychology Behav Soc Netw 15(7): 373-377.
- De Leo JA, Wulfert E (2013) Problematic Internet use and other risky behaviours in college students: An application of problem-behaviour theory. Psychol Addict Behav 27(1): 133-141.
- Gámez GM, Orue I, Calvete E (2013) Evaluation of the cognitive-behavioural model of generalized and problematic Internet use in Spanish adolescents. Psicothema 25(3):
- Leung L, Lee PS (2012) Impact of internet literacy, internet addiction symptoms, and internet activities on academic performance. Social Science Computer Review 30(4): 403-418.
- Liu QX, Fang XY, Zhou ZK, Zhang JT, Deng LY (2013) Perceived parent-adolescent relationship, perceived parental online behaviours and pathological internet use among adolescents: Gender-specific differences. PloS One 8(9): e75642.
- Andreou E, Svoli H (2013) The association between internet user characteristics and dimensions of internet addiction among Greek adolescents. International Journal of Mental Health and Addiction 11(2): 139-148.
- Bener A, Bhugra D (2013) Lifestyle and depressive risk factors associated with problematic Internet use in adolescents in an Arabian Gulf culture. Journal of Addiction Medicine 7: 236-242.
- Yang CY, Sato T, Yamawaki N, Miyata M (2013) Prevalence and risk factors of problematic Internet use: A cross-national comparison of Japanese and Chinese university students. Transcultural Psychiatry 50(2): 263-279.
- Santaliestra-Pasías AM, Mouratidou TM, Verbestel V, Huybrechets I, Gottrand F, et al. (2012) Food consumption and screen-based sedentary behaviours in European adolescents: the HELENA study. Arch Pediatr Adolesc Med 166(11): 1010-1020.
- Lee YS, Han DH, Kim SM, Renshaw PF (2013) Substance abuse precedes internet addiction. Addict Behav 38(4): 2022-2025.
- Sun P, Johnson CA, Palmer P, Arpawong TE, Unger JB, et al. (2012) Concurrent and predictive relationships between compulsive Internet use and substance use: Findings from vocational high school students in China and the USA. Int J Environ Res Public Health 9(3): 660-673.
- Herdman TH, Kamisuru S (2014) In: Bulechek G, Butcher H, Dochterman J, Wagner C (Eds.), NANDA International nursing diagnoses: Definitions and classification, Wiley-Blackwell, Oxford, USA.
- Herdman TH (2012) NANDA International nursing diagnosis: Definition & classification, Wiley- Blackwell, Oxford, USA.
- Ackley B, Ladwig G (2013) Nursing diagnosis handbook: An Evidence based guide to planning care. Elsevier Health Sciences, St. Louis, Missouri, USA.
- Arcas P (1990) Research in nursing. Priorities and strategies. Nursing Role 148: 55-60.
- Luis M (2008a) Diagnostic Nurses: Critical Review and Practical Guidance. 8th (edn), Elsevier España.
- Luis M (2008b) Diagnostic Nurses: Critical Review and Practical Guidance. Masson, Spain.
- Lunney M (2011) Critical Reasoning for Achieving Healthcare Results: Case Studies and Nursing Analysis. Elsevier, Barcelona, Spain.
- Moreno CT, Gallego FC, María GE, Gil de Miguel A (2010) Barriers to the utilization of research. A descriptive study of clinical nurses and nurses with experience as researchers. Enfermería Clínica 20(3): 153-164.
- Pearson A, Field J, Jordan Z (2007) Evidence-based clinical practice in nursing and health care. McGraw-Hill, Madrid, Spain.
- Wallin L (2009) Knowledge translation and implementation research in nursing. Int J Nurs Stud 46(4): 576-587.
- Walker LO, Avant KC (2005) Concept analysis. In: Walter LO, Avant KC (Eds.), Strategies for theory construction in nursing, 3rd (edn), Appleton-Century-Crofts, New York, USA, pp. 35-78.
- Fehring RJ (1994) The Fehring model. In: Carroll Johnson RM, Paquette M (Eds.), Classification of nursing diagnosis: Proceedings of the tenth conference. JB Lippincott, Philadelphia, USA, pp. 55-57.
- Fehring RJ (1987) Methods to validate nursing diagnoses. Heart & Lung 16(6): 625-629.
- Sparks S, Lien-Gieschen T (1994) Modification of the diagnostic content validity model. Nurs Diagn 5(1): 31-35.
- Fehring RJ, Fadden T, Wake MM (1991) Multinational validation of anxiety, hopelessness, and ineffective airway clearance. International Journal of Nursing Terminologies and Classifications 2(2): 57-65.
- Parker I (1999) (Eds) Deconstructing psychotherapy. Sage, London.
- Boubeta RA, Ferreiro GS, Salgado GP, Couto BC (2015) Variables associated with problematic internet use among adolescents. Salud y drogas 15(1): 25-38.
- Şaşmaz T, Öner S, Kurt AÖ, Yapıcı G, Yazıcı AE, et al. (2014) Prevalence and risk factors of Internet addiction in high school students. European Journal of Public Health 24(1): 15-20.
- Scroggins L (2012) The process for development of an approved NANDA International nursing diagnosis. In: Herman TH (Eds), NANDA International nursing diagnoses: Definitions & classification, Wiley-Blackwell, Oxford, UK, pp. 499-507.
- Young KS, Yue XD, Ying L (2011) Prevalence estimates and etiologic models of Internet addiction. Internet addiction: A handbook and guide to evaluation and treatment pp. 3-17.
© 2019 Anna Bocchino. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






