- Submissions

Full Text
COJ Biomedical Science & Research
Diagnosing and Treatment of Osteoarthritis in a Parkinson’s Disease Patient
Talukdar D*
Department of Medical Research, Dominica
*Corresponding author: Talukdar D, Department of Medical Research, Dominica
Submission: November 18, 2020; Published: March 11, 2021

Volume1 Issue5March 2021
Abstract
A 46-year-old woman with a past medical history of Parkinson’s Disease reports pain in her left knee while walking at home. It involved a gradual onset over the past couple of months due to limitations in her movement. She requires assistance to perform her day-to-day activities. She wears a postural support belt to straighten her spine and walks in a hunched back position. She complains about stiffness in joints and pain in her left knee while walking. She takes Vitamin D3 with Calcium tablets to strengthen her bones. She is not obese but complains of a past knee injury wherein she fell and slipped accidentally 10 years ago. She has no prior history of knee surgery. The patient also complains about a grating sensation while walking using the affected knee joint. How should the patient be diagnosed and treated for her left knee pain which is limiting her movements?
Background
Osteoarthritis (OA) of the knee is a chronic disease that can lead to pain due to degeneration of the cartilage between the joints. Joint stiffness is noticeable along with tenderness when pressure is applied in the affected region. As per World Health Organization (WHO) Global Burden Study Report, the overall disability-adjusted life years (DALY’s) due to the burden of the disability is 6.8% globally. It also states that the overall prevalence of the disease is higher among women than men. It is also estimated that 10-15% of all adults suffer from osteoarthritis aged over 60 years [1]. OA can cause stiffness in all structures in a joint. It commonly affects the knees, hip joints, shoulder, hands, and feet. It is related to the aging process along with certain modifiable risk factors like obesity, lack of exercise, occupation, etc., and non-modifiable risk factors like a traumatic injury to the joint, gender, genetic predisposition, etc. Patients suffering from OA can experience loss of flexibility with limitations in a full range of motion, bone spurs which can form around the affected region [2].
Diagnosing OA
OA can lead to wearing and tearing of cartilage which cushions the bones from rubbing
against each other. It can lead to friction and deterioration of the cartilage. It can eventually
lead to changes in the bone affecting the joint overall. The lining of the knee joint can also
get inflamed due to loss of connective tissue, reduced joint compartment space, and joint
spurs which can cause friction [3]. During the examination of the patient, reduced flexibility
with increased tenderness was noted. Prolonged morning stiffness can also be observed
with patients suffering from OA with difficulty climbing stairs, walking, and getting up from
a seated position. OA is a degenerative disease that can cause difficulty in performing daily
tasks. Patients experience pain sensation with repeated stress on the affected joint. It can lead
to inflammation with added stress to weight-bearing joints [4].
X-rays are considered a preferred imaging test that is readily available and affordable by
patients worldwide. In certain complex cases, MRI can offer detailed information in terms of
bones and soft tissues. But it is not used commonly for diagnosing OA [5]. X-rays can show
bone spurs around the affected joint, but it cannot show the loss of cartilage around bone
joints. But it does reveal the osteophytes and narrowing of joint spaces as indicated in this case
wherein various joint compartment spaces like lateral tibiofemoral, and patellofemoral were
reduced (Figure 1 & 2) [6]. The location of the tenderness along the medial or lateral lines is
also crucial for the initial diagnosis. Tears such as meniscal and anterior cruciate ligament are
also quite common. Clinical correlation is also quite necessary. There is no routine blood work for OA. No infection was indicated in synovial fluid which can lead
to other diagnoses such as gout or pseudogout.
Figure 1:OA left knee lateral side.
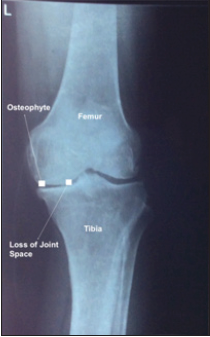
Figure 2:OA loss of joint space.
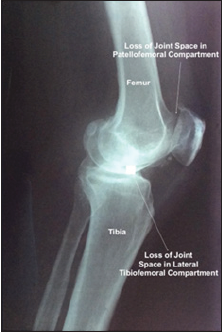
OA loss of joint space.
Drugs like Acetaminophen and Non-steroidal anti-inflammatory drugs (NSAIDs) like Advil, Motrin IB, etc. can provide relief from OA pain but chronic use can lead to liver and kidney damage, bleeding issues, cardiovascular, digestion issues, etc. Physical therapy is recommended as it increases flexibility, balances extra stress on affected joints, and reduces pain [7]. For immediate pain relief in OA, cortisone, and lubrication injections of hyaluronic acid can be considered as well. Other NSAIDs like Meloxicam, Diclofenac, and topical non-steroidal anti-inflammatory Voltaren Gel and COX-2 inhibitors like Celebrex can be used to treat OA. Other movement therapies like yoga and tai chi are also effective in reducing OA pain and improves the flexibility of the joints. Various assistive devices and braces can relieve stress from the affected joint and balance the weight proportionally. Transcutaneous electrical nerve stimulation (TENS) is also efficient in relieving OA pain for a short-term basis [8].
Recommendations
As mentioned in the above clinical vignette, the Parkinson’s Disease patient suffering from knee pain should be assessed with physical examinations including anterior draw test, Lachman test, etc. It is crucial to find the cause for joint pain, tenderness, and stiffness. Radiography specifically X-Ray shows the narrowing of space between joint compartments. Clinical correlation shows joint pain not related to rheumatoid arthritis and no infection was found in the synovial fluid. The patient was diagnosed with osteoarthritis (OA) of the left knee. Acetaminophen, NSAIDs, capsaicin cream, and NSAID Ibuprofen gel with low impact exercises, yoga, and nutritional supplements like glucosamine and chondroitin are recommended as treatment plans.
References
- Wittenauer R, Smith L, Aden K (2013) Background paper 6.12 osteoarthritis. World Health Organisation, Switzerland.
- Felson DT (2006) Osteoarthritis of the knee. New England Journal of Medicine 354(8): 841-848.
- Spector TD, Hart DJ (1992) How serious is knee osteoarthritis? Annals of the Rheumatic Diseases 51(10): 1105-1106.
- Amin S, Luepongsak N, McGibbon CA, LaValley MP, Krebs DE, et al. (2004) Knee adduction moment and development of chronic knee pain in elders. Arthritis Care & Research 51(3): 371-376.
- Wenham CY, Grainger AJ, Conaghan PG (2014) The role of imaging modalities in the diagnosis, differential diagnosis and clinical assessment of peripheral joint osteoarthritis. Osteoarthritis and Cartilage 22(10): 1692-1702.
- Cibere J (2006) Do we need radiographs to diagnose osteoarthritis? Best Practice & Research Clinical Rheumatology 20(1): 27-38.
- Altman RD (2010) Early management of osteoarthritis. Am J Manag Care 16: S41-S47.
- Ringdahl EN, Pandit S (2011) Treatment of knee osteoarthritis. American Family Physician 83(11): 1287-1292.
© 2021 Talukdar D. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






