- Submissions

Full Text
Associative Journal of Health Sciences
A Diagnostic Dilemma: Tuberculosis of the Gallbladder
Rohit Kumar Singh1, Soumya Khanna2, Tiwary SK3, Puneet3 and Ajay K Khanna3*
1Fellow in Surgical Gastroenterology, Departments of General Surgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi, Uttar Pradesh, India
2Associate Professor, Department of Anatomy, Institute of Medical Sciences, Banaras, Hindu University, India
3Professor, Departments of General Surgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi, Uttar Pradesh, India
*Corresponding author: Ajay K Khanna, Professor, Departments of General Surgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi, Uttar Pradesh, India
Submission: March 03, 2023;Published: May 12, 2023

ISSN:2690-9707 Volume2 Issue4
Abstract
Tuberculosis affecting the gallbladder is a very uncommon occurrence and is usually detected alongside calculous or acalculous cholecystitis. It is often challenging to diagnose tuberculosis of the gallbladder before surgery. Research indicates that most cases are not diagnosed until after the gallbladder has been removed, except in cases where there is strong suspicion of tuberculosis. Even then, confirmation of the diagnosis can only be achieved through histopathological examination of the gallbladder. We are reporting a case of gallbladder tuberculosis in an 18-year-old male who visited the surgical outpatient department with symptoms of chronic cholecystitis resulting from the presence of gallstones. Abdominal ultrasound detected a single gallbladder stone situated in the fundal region. After, undergoing laparoscopic cholecystectomy and receiving anti-tubercular drugs, the patient demonstrated a positive result in terms of the patient’s health and improvement visible on medical imaging.
Keywords:Cholecystectomy; Gallstones; Tuberculosis
Introduction
The first documented case of tuberculosis affecting the gallbladder was observed by Gaucher in 1870. The primary factors believed to contribute to the onset of gallbladder tuberculosis are cholelithiasis and obstruction of the cystic duct [1].
Patients who experience right upper quadrant abdominal pain are frequently diagnosed with gallstones and associated inflammation of the gallbladder (GB) [2,3]. The occurrence of isolated tuberculosis (TB) in the gallbladder prior to surgery is extremely uncommon and is often overlooked unless there is a strong suspicion of the disease. Ultrasound examination of the gallbladder can produce indistinct findings, making the diagnosis of gallbladder tuberculosis challenging, particularly in cases of calculus cholecystitis. We are presenting a case of a patient who was diagnosed with gallbladder tuberculosis through histopathological evaluation following cholecystectomy, despite having been initially diagnosed with symptomatic cholelithiasis. The diagnosis of gallbladder tuberculosis continues to be a challenging task. Distinguishing between gallbladder tuberculosis and other gallbladder disorders remains a difficult task. It is challenging to identify gallbladder tuberculosis prior to surgery, and symptoms that persist after surgery because of tuberculosis can intermittently be misdiagnosed as the “post-cholecystectomy syndrome.” Hepatobiliary tuberculosis has increased prevalent in males, with males affected twice that of females. No particular age is specified by this disease, although one study suggests that the majority of patients fall between the ages more than 10 and less than 50 years [4,5].
Case Report
A male patient, aged 18 years, reported a history of right upper abdominal pain lasting for 18 months. The patient did not report experiencing fever, jaundice, weight loss, or loss of appetite. Physical examination did not reveal any abnormalities except for mild tenderness in the right hypochondrium. Standard tests, such as CBC, LFT (blood investigations) and chest X-ray, yielded normal results without any anomalies detected. An abdominal ultrasound identified the presence of several gallstones in the gallbladder, with the largest measuring 19mm in diameter. The patient received an elective cholecystectomy through laparoscopic surgery. During the surgery, the gallbladder was found to be enlarged and containing numerous calculi. The cystic duct appeared dilated and short, and there were thick adhesions present among the gallbladder wall and the duodenum (Figure 1). The liver, CBD, and other parts of the intestine appeared normal upon examination.
Figure 1:Thick adhesions present among the gallbladder wall and the duodenum.
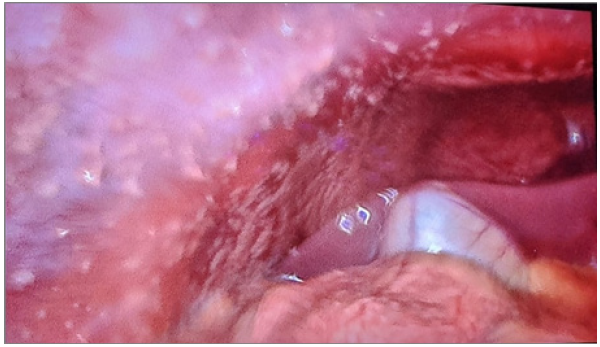
Figure 2:Detected tuberculosis bacteria was negative.
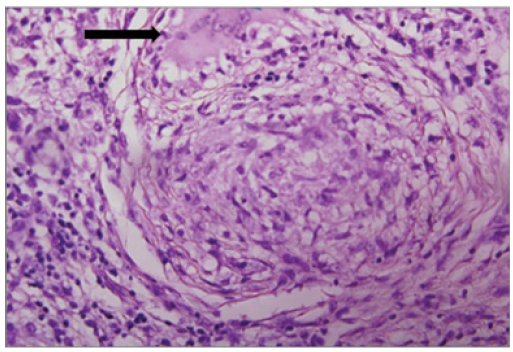
The specimen that was removed during the surgery was sent for a histopathological examination. The examination of the gallbladder tissue under a microscope showed specific ulcers and persistent, heavy inflammation within the layer beneath the epithelium, with some scattered granulomas composed of epithelioid cells and giant cells. However, the acid-fast stain used to detect tuberculosis bacteria was negative (Figure 2).
Discussion
Gaucher initially reported tuberculosis affecting the gallbladder in 1870, and this is considered a rare site for tuberculosis to occur. Until now, there have been fewer than 100 cases reported documented in the medical studies. Tuberculosis infection has a low likelihood of affecting the mucosal lining of the gallbladder which could be due to the presence of bile acids that are highly concentrated and the alkaline environment of the gallbladder lumen that inhibits the growth of tuberculosis. As the tuberculosis bacilli travel up the biliary system, they can serve as a source of formation for the stones. If tubercles are present in the serosal layer of the gallbladder, it suggests that the infection has spread through the peritoneal cavity [6,7]. The most prominent risk factors for the progress of gallbladder tuberculosis include the presence of gallbladder stones and obstruction of the cystic duct. Gallbladder tuberculosis is primarily disseminated through the hematogenous route and can involve adjacent lymph nodes or peritoneal tubercles. Patients commonly present with symptoms of right-sided upper abdominal pain, weight loss, nausea, vomiting, and gastrointestinal diarrhea. However, jaundice and a palpable abdominal mass are not frequently observed. It is important to note that most of these symptoms are linked to the presence of gallstones. Leukocytosis is a common finding in a few patients [8]. Diagnosing tuberculosis of the gallbladder can be challenging prior to surgery, especially when it coexists with calculus cholecystitis. Typically, the assessment is confirmed by microscopic evaluation of the sample gallbladder specimen post-cholecystectomy. The complete course of antitubercular medication is the recommended treatment for tuberculosis affecting the gallbladder [9,10].
Conclusion
Identifying the rare occurrences of tuberculosis in atypical locations is crucial in eradicating tuberculosis from regions where it is endemic. The frequency of abdominal tuberculosis is on the rise, and recognizing its clinical features can reduce the time to diagnosis and improve its treatment. Since tuberculous cholecystitis is challenging to diagnose, and often only detected after cholecystectomy or post-mortem examination, it is recommended that all cholecystectomy specimens undergo histopathological examination to identify any evidence of tuberculosis. The preferred initial treatment for tuberculosis affecting the gallbladder is the standard TB treatment. In general, the outlook for this condition is positive. Administering the appropriate antitubercular treatment can lead to lower rates of illness and death, as well as improved long-term results, and may even prevent the need for surgery in cases where the disease is medically treatable.
References
- Bendre M, Rane N, Narwade N (2014) Isolated tuberculosis of gallbladder: A case report. Indian Journal of Applied Research. 4(4): 439-440.
- Kapoor S, Sewkani A, Naik S, Sharma S, Jain A, et al. (2006) Myriad presentations of gall bladder tuberculosis. Indian J Gastroenterol 25(2): 103-104.
- Kumar K, Ayub M, Kumar M, Keswani NK, Shukla HS (2000) Tuberculosis of the gallbladder. HPB Surg 11(6): 401-404.
- Xu XF, Yu RS, Qiu LL, Shen J, Dong F, et al. (2011) Gallbladder tuberculosis: CT findings with histopathologic correlation. Korean J Radiol 12(2): 196-202.
- Abu Zidan FM, Zayat I (1999) Gallbladder tuberculosis (case report and review of the literature). Hepatogastroenterology 46(29): 2804-2806.
- Rejab H, Guirat A, Ellouze S, Trigui A, Mizouni A, et al. (2013) Primitive gallbladder tuberculosis: A case report with review of the literature. Ann Ital Chir 84(ePub): 1-3.
- El Malki HO, Benkabbou A, Mohsine R, Ifrine L, Belkouchi A, et al. (2006) Gallbladder tuberculosis. Can J Surg 49(2): 135-136.
- (2015) Djajakusuma, Timbol, Ong. Clinicopathologic Features of Hepatobiliary Tuberculosis: A Ten-Year Retrospective Autopsy Series. Philipp Soc Gastroenterol.
- (2019) Ministry of Health of the Republic of Indonesia. National Guidelines for Management of Medical Services Tuberculosis, pp: 1-139.
- Akhtar K, Zaheer S, Ahmad SS, Mansoor T (2009) Gall bladder tuberculosis. Ann Trop Med Public Health 2: 61-62.
© 2023 Ajay K Khanna. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)































 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






