- Submissions

Full Text
Advancements in Case Studies
Timeline and Outcome of Anosmia and Ageusia Associated with Covid-19 Infection: A Case Report
Viviane Flumignan Z1*, Cristina Scavasine V1, Ghizoni Teive HA1, Branco Germiniani FM1, Azevedo VF2, Paulo Roberto Z3 and Camargo Rogenski CAM4
1Neurology division, Brazil
2Rheumatology division, Brazil
3Occupational medicine division, Brazil
4Othorrinolaringology division, Brazil
*Corresponding author: Viviane Flumignan Z, Department of vascular neurology, Brazil
Submission: April 28, 2020;Published: May 12, 2020

ISSN 2639-0531Volume2 Issue4
Abstract
Background: Viral respiratory diseases can present with ageusia (hypogeusia) and anosmia (hyposmia) due to viral neurotropism, usually manifest together with other symptoms in the acute phase and have in most instances both a good and short recovery. During the epidemic period of COVID-19, doctors should consider SARS-CoV-2 infection as a differential diagnosis. Recent series reporting these neurologic manifestations do not provide information about neither the timeline, nor the outcome of these symptoms in this scenario.
Patient’s concerns: A 54-year-old female physician with well-controlled diabetes, hypertension and arrhythmia who presented with an acute respiratory syndrome with influenza symptoms, with sudden onset of fever, followed by dry cough on the second day, and on the 4th day the patient noticed a sudden and total loss of smell and taste sensations. After 20 days, she noticed a mild return of flavor perception, mainly for spicy foods, but still complained of hyposmia and dysgeusia until the end of this report (30 days after the onset of neuropathic symptoms).
Diagnoses: COVID 19 associated with anosmia and ageusia induced by viral respiratory disease inflammation.
Intervention: cyanocobalamin supplementation to 9,000 micrograms per day.
Outcomes: A mild return of flavor began after the 20th day for specific seasoned foods, but olfaction didn’t improve. After 30 days of symptoms she performed a Sniffin Sticks Test, whose result was compatible with hyposmia. A longer follow-up should be warranted to better assess the final outcome.
Lessons learned: Anosmia and ageusia have been described as either an isolated manifestation or together within the clinical spectrum of SARS-CoV-2 (COVID-19). However, the definitive prognosis is still unclear - although she had total improvement of the COVID-19 respiratory manifestations, sensory symptoms remained. We present the timeline and the outcome of the sensory symptoms over 30 days.
Keywords: Olfaction disorders; Anosmia; Taste disorders; Ageusia; SARS-CoV-2 infection; Coronavirus; COVID-19
Abbreviations: ABR: Brazilian Academy of Rhinology; ABORL-CCF: Brazilian Association of Otorhinolaryngology and Cervico-Facial Surgery; ACE: Angiotensin-Converting Enzyme; BID: two times a day; COVID-19: Coronavirus disease 2019; CT: Computed tomography; MERS: Middle East Respiratory Syndrome; RNA: ribonucleic acid; SARS: Severe acute respiratory syndrome; SARS-CoV-2: Severe acute respiratory syndrome coronavirus 2; SpO2: Peripheral oxygen saturation; WHO: World Health Organization
Introduction
Smell and taste can be compromised in some viral respiratory infections and had been reported previously with the first studies of coronavirus during the SARS and MERS epidemic periods over the last decades. As the SARS-CoV-2 pandemic progressed over the last six months, varying degrees these sensory disturbances have been reported and ultimately led to the incorporation of both ageusia and anosmia as characteristic symptoms, if not obligatory [1]. The transduction mechanism of smell and taste is a complex sequence of processes, with biochemical mediators induced by the presence of particulated stimuli. Anatomical particularities make these neurons more vulnerable to injury; nevertheless, these olfactory and taste receptor neurons are able to be replaced in days. In spite of that, nutritional state, certain drugs, radiation and viral infections could impair this turn-over mechanism [2,3].
Nervous system involvement in COVID-19 seems to be less affected than other human organs, but ACE2 receptors are also expressed on glial cells and neurons, as well as skeletal muscle, which makes them a potential target for COVID-19. The invasion of the nervous system can be either direct or indirect - the protective role of the blood-brain barrier in containing the virus needs to be further explored, but the invasion of the brain via the nose epithelium through the unmyelinated neurons of the olfactory nerve and bulb has been shown to cause neuronal death in mice models of SARS-CoV [1,4]. Recently in a hospital series with 214 patients, 78 (36.4%) patients had some neurologic manifestations [5]. The combination of anosmia and ageusia can significantly impact quality of life in surviving patients and should be taken as a red-flag for the differential diagnosis of acute respiratory syndromes, suggestive of SARS-CoV-2. Nonetheless, the natural history of these specific symptoms, with resolution (if any), remains unclear, and more specific information gathered can be of help in envisioning a standard, prototypical timeline.
Case Presentation
A 54 y/o Caucasian, female physician, with a previous history of controlled type I Diabetes, hypertension and taquiarritmia, taking glargine /lispro insulin, losartan 100 mg BID (recently changed for amlodipine as a self-made decision 1 week before the onset of symptoms) and fempromamona 300mg BID. She gave a lecture at the Stroke International meeting that took place in Rio de Janeiro, Brazil, from March 10th to March 14th. Symptoms began four days after the meeting, first with fever, followed by headache. In the first 24 hours, fever rapidly increased up to 38ᵒ Celsius. Body temperature would temporarily abate with paracetamol for about 5-6 hours, and then raise again. On the second day, fatigue, myalgia and discreet dry cough appeared. On March 19th, with 621 confirmed cases of coronavirus, Brazil was still not considered a country with national community transmission; this was only declared by the local authorities on March 22nd, following 1,128 confirmed cases.
On the 3rd day of disease, with persistent fever, the patient went back to the ER. Peripheral oxygen saturation (SpO2) was 92%, but physical examination remained unremarkable. Coronavirus was confirmed by a positive real-time reverse transcriptase polymerase chain reaction (RT-PCR) assay test from a throat swab specimen after 4 days of the initial symptoms. An unenhanced chest computed tomography (CT) performed on the 3rd day after onset, showed minimal thickening of the bronchial walls, findings that were not suggestive of COVID-19 (Figure 1). On the 4th day ageusia and anosmia started abruptly, even without any previous rhinorrhea or nasal obstruction while both fever and cough resolved. No specific protocol of treatment was instituted. Hidroxicloroquine was considered, but later discarded due to a relative cardiotoxicity contraindication. Olsetamivir was not available and azithromycin was not prescribed. Neither anti-inflammatory drugs nor oral antihistamines were recommended for this acute period. She started to take vitamin B12 BID (5000mcg). She went back to work after a 14 days-hiatus, following a positive IgM and IgG serology. Ageusia and anosmia remained remarkably unimproved until the 20th day from the initial symptoms, when the perception of distinctive flavor, such as spices, started to come back. At that time IgM and IgG serologic tests were positive. Until the end of this report, 30 days from the onset of neuropathy she remained with dysgeusia and hyposmia, even though the serologic profile evolved to that of a chronic phase/resolution with only a positive IgG fraction. As ancillary evaluation, a Sniffin Sticks Test was performed and documented the persistent symptoms (Figure 2).
Figure 1: Unenhanced chest CT of a 54-year-old woman (slice at the level of the base of the lower lobes of the lungs) showed minimal thickening of the bronchial walls.
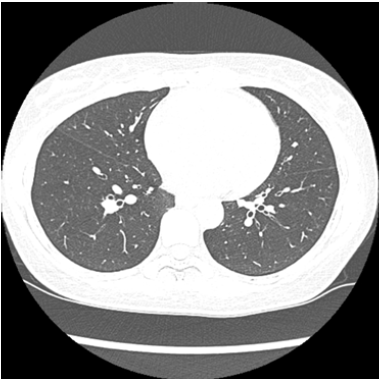
Figure 2: Timeline of ageusia/anosmia.

Discussion
Coronaviruses are enveloped single-stranded RNA viruses that are zoonotic in nature. The main symptoms are like those of the common cold to a more severe respiratory infection, whether with or without enteric, hepatic, and neurological symptoms. In 2019, the SARS-CoV-2 (severe acute respiratory syndrome) was officially named COVID-19 by WHO [2]. Coronavirus has previously caused two large-scale pandemics in the last two decades - SARS and MERS. Studies reported that COVID-19 S-protein has a strong interaction with human ACE2 (angiotensin converting enzyme 2) the same receptor of SARS-CoV that caused an epidemic of smaller proportions [6]. The spectrum of COVID-19 manifestation seems to be large, ranging from mild to severe cases, with asymptomatic patients and deaths being reported. The most common are fever, cough, myalgia or fatigue, pneumonia, and complicated dyspnea, whereas less common reported symptoms include headache, diarrhea, hemoptysis, runny nose, and phlegm-producing cough [2,4]. New symptoms are still being reported.
One retrospective study showed 36.4% of neurological symptoms, being 19 (8.9%) related to the peripheral system including hypogeusia, hyposmia, hypopsia and neuralgia. The most common peripheric complaints were dysgeusia in 12 (5.6%) and hyposmia in 11 (5.1%). The more frequent symptoms in the central nervous system compromise were dizziness and headache (16.8% and 13.1% respectively). All neurologic symptoms were significantly more common in severe cases as compared with non-severe cases, but these numbers were all seen in hospitalized patients which can be a bias in clinical observation. These patients also had a high D-dimer level and a lower lymphocyte counts, which were both implied as playing a potential role in the pathophysiology of stroke in COVID-19 patients, and as a mechanism of possible immunosuppression [5].
Additionally, the mechanism underlying CNS manifestation should include the role of the ACE2 receptor, which has already been identified as the functional receptor for SARS-CoV-2, as mentioned above. Like other respiratory viruses, SARS-COV-2 may enter the nervous system through either a hematogenous or retrograde neuronal route. The presence of hyposmia can support the latter [7]. Anosmia, the inability or decreased ability to perceive smell, is estimated to afflict 3–20% of the whole population. Risk of olfactory dysfunction increases with old age and may also result from chronic sinonasal diseases, severe head trauma, and upper respiratory infections, or neurodegenerative diseases. Ageusia or taste impairment, can present either along with anosmia or not, but is rarely mentioned. As olfactory and taste testing are not part of general health exams, clinicians need to rely on patients’ self-reports. Therefore, statistics analysis of these symptoms are likely to be underestimated. Nevertheless, self-report measurements are both sensitive (correct recognition of olfactory dysfunction) and specific (correct recognition of normal) in comparison with gold standard tests [8-10]. The underlying mechanism of anosmia in any scenario is debatable and seems to be poorly understood.
The lack of inflammation in SARS-CoV-infected brains in the past posed the possibility that neurons died by apoptosis; a form of cell death associated with minimal cellular infiltration combined with an impairment of astrocytes function. It means that there is no replacement of the basal cell resulting in a loss of smell-taste, a turnover process well known in olfactory system [11]. However, in COVID-19 a different theory proposes that excessive levels of proinflammatory cytokines/chemokines in the brain result in a “cytokine storm” phenomenon. To a certain extent, this might also explain the systemic symptoms of the disease as a whole [12]. As for dysgeusia, taste perception is mediated by three cranial nerves -VII, IX and X - with a more complex physiology. Salts and acids come from a molecular interaction with ionic channels in the membrane of receptor cells, whereas sweet and bitter tastes are the result of interaction with specific receptors in the cell membrane. Indeed the tongue has four types of papillae and the five taste qualities can be perceived on all loci where there are taste buds are found, making the perception of taste much more complex and without distinct ‘taste-specific’ areas, as was previously believed [13]. It’s remarkable how rare taste loss is reported in any condition - even when the taste system is structurally damaged, there are few complaints of taste loss. That's because taste nerves inhibit one another, which may explain why patients fail to notice changes in everyday taste experience [14].
Taste and olfaction are often confused in the minds of patients because “taste” is used as a synonym for “flavor” in ordinary conversation. Taste refers to sensations arising from the taste buds embedded in the tissues of the tongue, palate, and throat. Olfactory qualities are much more numerous than those of taste. Flavor brings the idea of the taste-olfaction mix. The majority of papers referred to anosmia without disgeusia information [14]. All of these should be kept in mind when the timeline and recovery process of anosmia and ageusia are reporting together. Viral infections of the upper airways are the second leading cause of anosmia, with spontaneous recovery in most cases. It usually starts with all respiratory manifestation and release in 4-5 days. A recent Chinese study [5] reported only 5.1% of hyposmia in patients with COVID-19. However, anecdotal evidence of anosmia in 30% of patients in Daegu, South Korea, and 2/3 of COVID-19 patients in Heinsberg, Germany was reported by the Brazilian Academy of Rhinology (ABR) and the Brazilian Association of Otorhinolaryngology and Cervico-Facial Surgery (ABORL-CCF), alerting doctors to the possibility of these findings being an alarm symptom for COVID-19. Although there is no robust evidence, ABR advises that the presence of sudden anosmia (with or without ageusia and without concomitant nasal obstruction) may suggest COVID-19 in this pandemic scenario with sustained transmission of the SARS-CoV-2 virus. Patients in these presentations should be advised to stay in for more than 14 days and wait for the resolution of anosmia, which appears to be temporary in most cases.
To date, no specific antiviral treatment has been confirmed to be effective against COVID-19 nor for anosmia and ageusia in any scenario. Therefore, patients infected with COVID-19 should receive appropriate symptomatic treatment and supportive care. Corticosteroids are not indicated in acute phase but there is no consensus about their use later [15]. We did not find consistent information about the outcome or timeline of the ageusia and anosmia. Our case still had not fully recovered until the 20th day after the initial symptoms when she experienced a subjective improvement, despite still having an abnormal Sniffin Sticks Test result on the 30th day, compatible with hyposmia. The reasons for that are unclear but might be related to the specific microstructure of neurons in the I, VII, IX and X cranial nerves. We hope that further cases, series or surveys (including a Brazilian one which is already under way) will focus on prognostic information about those symptoms and their value for the development of disease specific biomarkers in the future.
References
- Netland J, Meyerholz DK, Moore S, Cassell M, Perlman S (2008) Severe acute respiratory syndrome coronavirus infection causes neuronal death in the absence of encephalitis in mice transgenic for human ACE2. J Virol 82(15): 7264-7275.
- Huang C, Wang Y, Li X, Ren L, Zhao J, et al. (2020) Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 395(10223): 497-506.
- Li Y, Bai W, Hashikawa T (2020) The neuroinvasive potential of SARS‐CoV2 may play a role in the respiratory failure of COVID‐19 patients. J Med Virol 92(6): 552-555.
- Wu Y, Xu X, Chen Z, Duan J, Hashimoto K, et al. (2020) Nervous system involvement after infection with COVID-19 and other coronaviruses. Brain Behav Immun.
- Mao L, Jin H, Wang M, Hu Y, Chen S, et al. (2020) Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China. JAMA Neurology.
- Chen Y, Liu Q, Guo D (2020) Emerging coronaviruses: Genome structure, replication, and pathogenesis. J Med Virol 92(4): 418-423.
- Marc D, Dominique JF, Élodie B, Jessica D, Mathieu MP, et al. (2013) Human coronavirus: respiratory pathogens revisited as infectious neuro-invasive, neurotropic, and neurovirulent agents. In: Sunit KS, Daniel R (Eds.), Neuroviral Infections: RNA Viruses and Retroviruses (1st edn), CRC press, Boca Raton, Florida, USA, pp. 93-122.
- Durrant DM, Ghosh S, Klein RS (2016) The olfactory bulb: An immuno-sensory effector organ during neurotropic viral infections. ACS Chem Neurosci 7(4): 464-469.
- Schöpf V, Kollndorfer K (2015) Clinical assessment of olfactory performance-why patient interviews are not enough: a report on lessons learned in planning studies with anosmic patients. HNO 63(7): 511-515.
- Ribeiro JC, Simões J, Silva F, Silva ED, Hummel C, et al. (2016) Cultural adaptation of the Portuguese version of the “Sniffin’ Sticks” smell test: Reliability, validity, and normative data. PLOS ONE 11(2): e0148937.
- Arabi YM, Balkhy HH, Hayden FG, Bouchama A, Luke T, et al. (2017) Middle east respiratory syndrome. N Engl J Med 376(6): 584-594.
- Ye Q, Wang B, Mao J (2020) The pathogenesis and treatment of the `Cytokine Storm’ in COVID-19. J Infect.
- Kinnamon SC, Margolskee RF (1996) Mechanisms of taste transduction. Curr Opin Neurobiol 6(4): 506-513.
- Krajewska J, Krajewski W, Zub K, Zatoński T (2020) COVID-19 in otolaryngologist practice: a review of current knowledge. Eur Arch Otorhinolaryngol.
- Tobaiqy M, Qashqary M, Al-Dahery S, Mujallad A, Hershan AA, et al (2020) Therapeutic management of COVID-19 patients: A systematic review. Infection Prevention in Practice.
© 2020 Viviane Flumignan Z. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)






























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)














.bmp)
.jpg)
.png)
.jpg)










.jpg)






.png)

.png)



.png)






