- Submissions

Full Text
Intervention in Obesity & Diabetes
The Weight Status of Children in Late Childhood within Southeast Wales (UK) and Predictions for their Future Health
Jarvis S*, Giles H, Jarvis P and New K
Faculty of Life Sciences and Education, University of South Wales, United Kingdom
*Corresponding author:Stuart Jarvis, Faculty of Life Sciences and Education, University of South Wales, Pontypridd, CF37-1DL, United Kingdom
Submission:July 21, 2021;Published: August 16, 2021

ISSN 2578-0263Volume5 Issue3
Abstract
Background: Current child measurements of weight status in Wales are determined at early childhood only. A further measurement at late childhood could identify adiposity levels prior to adolescence and young adulthood. The aim of this study therefore was to determine current adiposity levels in a cohort of children at late childhood and present a prediction of future levels upon entering young adulthood.
Methods: In total, 288 boys (M age=10.94 years, SD=0.58), and 257 girls (M age=10.78 years, SD=0.63) from Southeast Wales were measured for anthropometry and their BMI (kg/m2) determined. International Obesity Task Force (IOTF) data predicted their BMI at age 18 years.
Results: Approximately one quarter of boys and girls in late childhood were classified at an unhealthy weight. Predictive data showed that by age 18 years, this percentage had increased to approximately one third in both genders.
Conclusion: The overweight and obesity levels in our cohort were high and predicted that many could become obese adults. This study therefore supports the call for the current Wales child measurement programme to be extended to report weight status in late childhood and potentially target intervention with this generation of youth.
Keywords:Adiposity; Body composition; BMI; Primary school children
Introduction
It has been well established that obesity is associated with increased risk of developing major health conditions, including coronary heart disease, type 2 diabetes, some cancers, and a risk to people’s mental health [1]. The economic cost of obesity to a countries GDP is estimated at 5-14% of health expenditure for 2020-2050 [2] and in Wales, obesity associated illnesses are projected to cost the Welsh NHS in excess of £465 million per annum [3]. The impact of obesity on the lifecycle is suggested to originate in childhood [4]. Both the Avon Longitudinal Study of Parents and Children (ALSPAC) and the National Health and Nutrition Examination Survey (NHANES), amongst significant others have highlighted the importance of early detection of obesity and subsequent intervention during childhood. Most recently, in Wales, Beynon & Bailey [5] highlighted an increasing trend of severe obesity in children aged 4-5 years and suggested that both childhood obesity and severe childhood obesity needs an additional focus. At present, Wales utilizes the Child Measurement Programme (CMP) at 4-5 years only (i.e., early childhood) and there is no second measurement of children’s weight status in late childhood (i.e., 9-11 years old) as is typical in several other countries in the UK. Since devolution, Wales has had total spending and budgetary control over its health for the nation and its first Obesity Strategy for Wales was expected in the fall of 2019. This draft strategy was considering the introduction of a second measure of weight status of children in late childhood which could allow tracking of obesity and children’s category over time. Therefore, the primary aim of this study is to provide evidence of the weight status of children in late childhood (aged 9-11 years) in Wales which in turn, may support the call for inclusion of this second measurement point of children in Wales.
It has been suggested by Dietz [6] that the greater the severity of childhood obesity, the greater the degree of adult obesity. In addition, Chen et al. [7] suggests that being proactive in the prevention of weight gain at late childhood and adolescence prior to adulthood, might be more important than being reactive as achieving, and maintaining long term weight loss is difficult once obese. Therefore, to provide an insight with this population, a secondary aim of this study was to predict children’s BMI at age eighteen years via the use of a validated prediction equation. The use of this predictive equation [8] to predict future adiposity of children, has been previously investigated in several populations. For example, Janssen et al. [9] and Valerio et al. [10] who both reported a good strength of agreement in predicting obesity and CHD risk factors in young adults. Therefore, this exploratory prediction of weight status from children in late childhood could also provide justification to extend the Wales CMP beyond the early years.
Methods
Participants
Following ethical approval, children from eighteen primary schools in Southeast Wales participated in the study. In total, 545 children, aged between 10 and 11 years attended the test centre and compromised of 288 boys (M age=10.94 years, SD=0.58), and 257 girls (M age=10.78 years, SD=0.63). The participants were unintentionally exclusively Caucasian. All schools were from a single local authority in Wales and is classified as having 71.4% of its area in the most deprived 50% of Wales [11].
Measures and Procedures
Anthropometry
All data collection was undertaken by the first author, an experienced female anthropometric practitioner, using a designated private area with individual participants. Anthropometric data collected height, sitting height, Waist Circumference (WC) and body weight. A portable floor standing Seca Stadiometer (Seca Birmingham, UK) measured height (cm) in bare feet to the nearest 0.1cm. Sitting height was measured using the Seca Stadiometer to the nearest 0.1cm. Body weight (kg) was determined using the Tanita BC-418 MA device (Tanita, Middlesex, UK) to the nearest 0.1kg. WC (cm) was determined by manual girth measurement directly on bare skin, on standing participants using a Seca 201 tape measure (Seca Birmingham, UK) to the nearest 0.1cm. BMI was calculated from body weight (kg) divided by height (m2) [12]. Unlike adults, BMI in children varies significantly with age so a single definition cannot be used. BMI for children is categorized using variable thresholds that consider the child’s age and sex, with these thresholds being derived from a reference population, known as a child growth reference [13]. Therefore, this study uses a BMI classification which is in line with the UK90-WHO reference charts for BMI percentiles in children. BMI was also predicted for age 18 years using IOTF predictive BMI-for-age tables [14]. The authors acknowledge that whilst it is not recommended to use BMI values categorized from different organizations [13], it enabled data for this study to be utilized more comprehensively. To determine pubertal status, the previously validated models of Mirwald et al. [15] were adopted to predicting Peak Height Velocity (PHV) and Age to PHV (APHV).
Statistical analysis
Data were checked for normality using the Shapiro-Wilk test. The BMI data for girls (p=0.721) and boys (p=0.259) was parametric and the data for WC (cm) was non-parametric with p=0.001 for both sexes. All data was analysed using SPSS version 27.0 (SPSS Inc, Chicago, IL, USA).
Results
Descriptive data
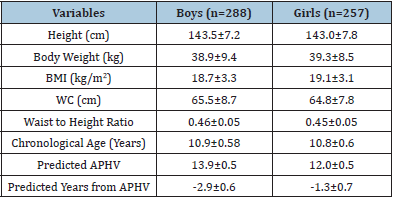
(Table 1) reports descriptive statistics for the sample. Overall, there were minimal differences between gender on height. Girls demonstrated slightly higher Body Weight (kg) and BMI (kg/m2) profiles than boys. The values, of WC (cm), Waist to Height Ratio and Chronological Age were all reported as being slightly higher in boys than girls. The prediction of PHV showed that girls were closer to the onset of puberty than boys.
Table 1: Means and standard deviations of physical characteristics for boys and girls. Note. BMI=Body Mass Index; WC=Waist Circumference; APHV=Age of Peak Height Velocity.
BMI percentiles
The data for UK90 WHO percentile scores across this cohort are shown in Table 2. Overall, it shows that just over 70% of both genders are classified at the normal weight range. Further scrutiny shows that approximately 27% of boys and girls are in the categories beyond this normal weight range with around 11% of these in both genders classified in the upper classifications of being very overweight or severely obese.
IOTF categorized BMI
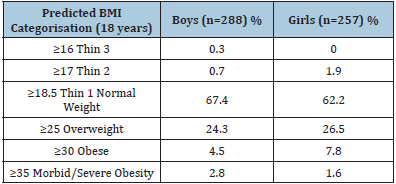
Looking at the IOTF predictions of BMI in this cohort at 18 years of age (Table 3) it estimated that approximately two thirds of both boys and girls are in the ≥18.5 thin 1/normal weight category. Of greater concern are approximately a third of both boys and girls predicted to be in classifications above this. Within these upper categories around 7% of boys and 8% of girls are predicted to be classified as either obese or morbid/severely obese.
Table 2: Body mass index percentiles based on UK90 WHO Categories. Note. BMI=Body Mass Index; UK90 WHO=United Kingdom 90 World Health Organisation.
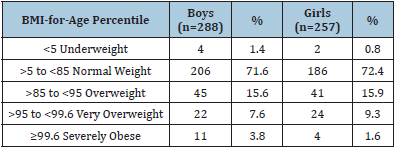
Table 3: International obesity task force predictions of BMI at age 18 years.
Discussion
Main findings of this study
The primary aim of this research was to provide novel data on the weight status of a cohort of 9-11 year old children in Wales. Our findings showed at this late childhood age, approximately one quarter of both boys and girls were already an unhealthy weight and just over 10% of these classified as being either very overweight or severely obese. A secondary aim of this study was to predict these children’s level of BMI at age 18 years. The findings from our cohort show by age 18 years, their predicted unhealthy weight status remained high with over one third of both the boys and girls being predicted to be at an unhealthy weight status entering young adulthood.
What is already known on this topic?
Similar prevalence studies in other parts of the UK identify that childhood obesity levels at late childhood are still increasing [16]. In England, the CMP identified that in children at age 10-11, 21.0% were obese and 14.1% overweight. In Scotland, the 2019 child measurement survey reported 30% of children aged 2-6 were obese, which fell to 25% of children aged 7-11, and rose again to 33% of children aged 12-15. Overall, boys were more likely than girls to be obese. Internationally, the OECD [2] reported, the majority of the childhood population in the OECD area were overweight or obese and amongst countries reporting measured data, the UK had the tenth highest rates of obesity. In 2016, the WHO reported over 340 million children and adolescents aged 5-19 were overweight or obese [17]. In Wales, although not directly comparable Beynon & Baily [5] have recently suggested that the prevalence of obesity and severe obesity in children is increasing, and an additional focus is required.
What this study adds
This study has presented a snapshot of the weight status of children in late childhood in Southeast Wales. To the authors knowledge there has been little analysis of weight status in children of late childhood in Wales and it therefore intends to add to the limited body of knowledge in this population. As previously iterated Wales currently only measures children at ages 4-5 years as part of its CMP and is proposing a secondary measurement of children in late childhood. Our study, although with only a small sample, on children in late childhood, shows that overweight and obesity is already a problem for approximately one third of the cohort across both genders. Therefore, it supports the calls to consider extending the current CMP to encompass a wider age range, enabling earlier identification and surveillance of overweight and obese children/adolescents in this population. In turn, as Beynon & Bailey [5] have previously advocated it would offer help to build a case for evidence-based interventions or monitor the success of interventions at a local authority or health board level. Further, our data for this cohort predicts by age 18 years, the overweight and obesity level will have risen to approximately one thirds of both boys and girls, further justifying closer tracking of obesity status throughout childhood and adolescence in Wales. Whilst the authors acknowledge this data is predictive, the impact of this approximate level of obesity for our future young Welsh adults is concerning, along with the potential associated health problems and the inevitable drain on limited health resources. The incidence of overweight/obesity in Wales is predicted to be higher than for England and Scotland at age 18 years [16].
Finally, late childhood presents an opportunity for assisting our young people to maintain a healthy weight as it is at this point in the life course that children are increasingly able to judge themselves differently according to the domain of their lives being addressed [18]. It has been suggested by Tonkin [19] that children at late childhood were potentially more responsive to interventions than during adolescence or young adulthood, when other interests become a priority. Whilst tracking and predicting alone will not reduce obesity, incorporating this approach to build upon other initiatives such as healthy eating programmes, nutritional guidelines, dietary and lifestyle education, could all aid in tackling obesity in Wales at this critical childhood age.
Limitations of this study
The limitations of this study were that reporting methods within the UK devolved governments differed slightly, as different age groups were reported on, making direct comparisons across the UK for child overweight and obesity less easy. Data from the IOTF [14] utilizing the child’s current age and BMI to predict potential BMI at age 18 years was predictive only. Further, international standards for BMI based classification of overweight and obesity in children and young people were difficult, making international comparisons difficult [20]. The Marmot review [21] suggested that social deprivation has an important influence on levels of obesity with children in lower socioeconomic groups more likely to be obese. This study can only present a general consensus of deprivation and therefore this needs to be taken into consideration when analyzing the study findings.
References
- (2019) Welsh Government, Welsh Government Healthy Weight: Healthy Wales 2020-2022 Delivery Plan, United Kingdom.
- OECD (2019) The heavy burden of obesity. The Economics of Prevention. Health Poverty Studies, Paris, France.
- (2016) Public Health Wales. Making a Difference.
- (2019) World Health Organisation. Global Strategy on Diet, Physical Activity and Health. Switzerland.
- Beynon C, Bailey L (2020) Prevalence of severe childhood obesity in Wales UK. J Public Health 42(4): 435-439.
- Dietz WH (1998) Health consequences of obesity in youth: childhood predictors of adult disease. Pediatrics 101: 518-525.
- Chen C, Ye Y, Zhang Y, Pan XF, Pan A (2019) Weight change across adulthood in relation to all cause and cause specific mortality: Prospective cohort study. BMJ 367: 15584.
- Cole TJ, Lobstein T (2012) Extended international (IOTF) body mass index cut-offs for thinness, overweight and obesity. Pediatr Obes 7(4): 284-294.
- Janssen I, Katzmarzyk PT, Srinivasan SR, Chen W, Malina RM, et al. (2005) Combined influence of body mass index and waist circumference on coronary artery disease risk factors among children and adolescents. Pediatrics 115(6): 1623-1630.
- Valerio G, Balsamo A, Baroni MG, Brufani C, Forziato C, et al. (2017) Childhood obesity classification systems and cardiometabolic risk factors: A comparison of the Italian, World Health Organisation and International Obesity Task Force references. Ital J Pediatr 43(1): 19.
- Welsh Index of Multiple Deprivation (2019) Welsh Government, Welsh Index of Multiple Deprivation, 2014. United Kingdom.
- World Health Organisation (2006) BMI-for-age (5-19 years).
- National Obesity Observatory (2011) A simple guide to classifying body mass index in children.
- World Obesity Federation (2015) Obesity classification.
- Mirwald RL, Baxter Jones ADG, Bailey DA, Beunen GP (2002) An assessment of maturity from anthropometric measurements. Med Sci Sports Exerc 34(4): 689-694.
- Baker C (2021) Obesity Statistics Jan 12. Briefing paper 3336.
- World Health Organisation. WHO Fact Sheet Obesity and overweight.
- Harter S (1985) Competence as a dimension of self-evaluation: Toward a comprehensive model of self-worth. In Leahy RL (Ed.), The Development of the Self. Academic Press, New York, USA, pp. 55-121.
- Tonkin RS (2001) Early intervention with an adolescent twist. Paediatr Child Health 6(7): 424-428.
- Cole TJ, Bellizzi MC, Flegal KM, Dietz WH (2020) Establishing a standard definition for child overweight and obesity worldwide: International survey. BMJ 320(7244): 1240-1243.
- Strategic Review of Health Inequalities in England post-2010 (2010) Fair society, healthier lives: The Marmot review.
© 2021 Jarvis S. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and build upon your work non-commercially.
 a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in
a Creative Commons Attribution 4.0 International License. Based on a work at www.crimsonpublishers.com.
Best viewed in 







.jpg)





























 Editorial Board Registrations
Editorial Board Registrations Submit your Article
Submit your Article Refer a Friend
Refer a Friend Advertise With Us
Advertise With Us
.jpg)






.jpg)













.bmp)
.jpg)
.png)
.jpg)














.png)

.png)



.png)






